Abstract
The role that Toll-like receptor (TLR) signaling may have in stimulating macrophages to become tumor promoting is not yet clearly defined. However, given the role macrophages play in restoring tissue homeostasis such as in the tissue repair response, it is likely that tumor-induced TLR signaling provides macrophages with signals of persistent injury. In this chapter, we review the molecular determinants of TLR signaling, the role TLR signaling plays in infection, wound healing, and tumorigenesis and discuss how TLR signaling in tumor-associated macrophages may result in tumor progression.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
- Avian Influenza
- Endogenous Ligand
- Lewis Lung Carcinoma
- Severe Acute Respiratory Syndrome
- Transitional Cell Bladder Carcinoma
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Introduction
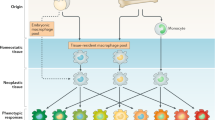
Macrophages are bone marrow-derived cells that initially circulate as monocytes and subsequently undergo differentiation into tissue resident macrophages. Macrophages support tissues by remodeling, secreting growth and angiogenic factors, and phagocytosing apoptotic cells. Virchow first described the presence of leukocytes in human tumours in 1863 and suggested that cancer originates in sites of chronic inflammation (Balkwill and Mantovani 2001). Wounding of normal tissues results in the production of numerous growth factors, cytokines, and chemokines, all of which recruit and differentiate circulating monocytes to tissues. Tumour cells have been found to produce similar growth factors and cytokines that recruit macrophages to tumours (Condeelis and Pollard 2006). Further, there is an emerging characterization of macrophage activation by tumour-derived ligands of Toll-like receptors (TLRs), a family of transmembrane proteins initially characterized as sensors of infection.
Whereas the role of these tumour-associated macrophages (TAMs) has yet to be clearly characterized, a majority (>80%) of clinical studies correlate an increased number of TAMs with a worse prognosis (Pollard 2004). Several in vivo studies have supported these clinical observations: mice deficient in CSF-1 and thus deficient in macrophages (Wiktor-Jedrzejczak et al. 1990), when crossed with mice prone to develop metastatic breast cancer, develop the same numbers of breast tumours but nearly no metastases (Lin et al. 2001). The role that TLR signaling may have in stimulating macrophages to become tumour promoting is not clearly defined. However, given the role that macrophages play in restoring tissue homeostasis such as in the tissue repair response, it is likely that tumour-induced TLR signaling will provide macrophages with signals of persistent injury in need of repair. In this chapter, we review the molecular determinants of TLR signaling, the role TLR signaling plays in infection, wound healing, and tumourigenesis and discuss how TLR signaling in TAMs may result in tumour progression.
Toll-Like Receptors
The TLR family of transmembrane proteins is best characterized as pattern recognition receptors (PRR) for sensing conserved pathogen-associated molecular patterns (PAMPs) (Medzhitov et al. 1997). PAMPs are conserved molecular patterns that are universal to all microorganisms within a defined class. Further, PAMPs are present within microorganisms regardless of their pathogenicity. In addition to microbial products, TLRs can also recognize endogenous, host-derived ligands (Jiang et al. 2007; Sims et al. 2010). Ten TLRs have been identified in humans and 12 TLRs in mice (Takeuchi and Akira 2010).
TLRs can be divided into two general groups based on the types of ligands they recognize and their subcellular localization. TLR1, TLR2, TLR4, TLR5, TLR6, and TLR11 are expressed on the plasma membrane and can recognize lipids, lipoproteins, and proteins from exogenous and endogenous sources. In contrast, TLR3, TLR7, TLR8, and TLR9 localize to intracellular compartments including the endoplasmic reticulum, endosomes, lysosomes, and endolysosomes, and they recognize nucleic acids (Kawai and Akira 2010).
TLRs are type I single spanning transmembrane proteins. Their molecular structure is defined by an extracellular or endolysosomal N-terminal leucine-rich repeat (LRR) domain followed by a transmembrane domain and then by a C-terminal cytoplasmic Toll/IL-1 receptor (TIR) domain. Below is a concise description of the known TLRs and their ligands.
TLR2 recognizes PAMPs from a variety of microorganisms including bacteria, fungi, Mycoplasma, and viruses by forming heterodimers with TLR1 and TLR6. The TLR1/TLR2 heterodimer recognizes triacyl lipoproteins, whereas the TLR6/TLR2 heterodimer recognizes diacyl lipoproteins.
TLR4 recognizes lipopolysaccharide (LPS), a component of the outer membranes of Gram-negative bacteria, by forming a homodimeric complex with LPS and myeloid differentiation factor-2 (MD2). In addition to bacterial products, TLR4 can recognize components of viral envelopes. TLR4 also recognizes endogenous ligands such as oxidized phospholipids produced during acute lung injury caused by avian influenza (Imai et al. 2008).
TLR5 recognizes flagellin, a component of the bacterial flagellum. In the lamina propria of the small intestine, flagellin stimulates lamina propria dendritic cells (DCs) to induce T cells to differentiate into Th17 cells and Th1 cells and B cells to differentiate into immunoglobulin A-producing plasma cells (Uematsu et al. 2008). TLR11, which is found in mice but not in humans, is closely related to TLR5. It is thought to recognize uropathogenic bacterial components (Zhang et al. 2004). In addition, it can recognize a profilin-like molecule from Toxoplasma gondii.
Nucleic acids are recognized by TLR3, TLR7, TLR8, and TLR9. TLR3 recognizes double-stranded RNA (dsRNA) from viruses (Alexopoulou et al. 2001) that are presented within endolysosomes. An analog of dsRNA, polyinosinic:polycytidylic acid (poly I:C), is also recognized by TLR3 and is commonly used to simulate viral infections. Activation of TLR3, as all TLRs that recognize nucleic acids, leads to the production of type I interferons as well as other pro-inflammatory cytokines.
TLR7 and TLR8 recognize single-stranded RNA (ssRNA) as well as the imidazoquinoline analogs of ssRNA within endolysosomes. TLR7 can also detect RNA from bacteria, also within the context of the endolysosome (Mancuso et al. 2009). Unmethylated DNA with CpG oligodeoxynucleotides (cytosine–guanosine repeats), commonly found in bacteria and viruses, is recognized by TLR9. In addition to DNA, TLR9 may recognize the crystalline metabolite of malaria, hemozoin (Coban et al. 2005). However, there is some evidence that hemozoin binds to the malaria DNA which can be recognized by TLR9 in the endolysosome (Parroche et al. 2007).
Although the ligand for human TLR10 has not yet been identified, it shares sequence homology with TLR1 and TLR6. In mice, the gene for TLR10 is disrupted by a retrovirus.
TLR Signaling Pathways
Upon recognition of their ligands, TLRs signal for the transcription of genes that allow the stimulated cell to appropriately respond to the stimulus. Specificity of this response is, in part, determined by the combination of adaptor molecules that associate with the C-terminal cytoplasmic domains of TLRs. These adaptors have in common a TIR domain. The five known TIR domain-containing adaptors of TLRs are MyD88 (myeloid differentiation factor 88), TRIF (TIR domain-containing adaptor inducing interferon beta; also known as TICAM-1), TIRAP (also known as MAL), TRAM (TRIF-related adaptor molecule), and SARM (Sterile-alpha and Armadillo motif-containing protein) (O’Neill and Bowie 2007). TLR signaling can be divided into two signaling pathways depending on whether they use either MyD88 or TRIF as adaptor molecules. The downstream targets vary in that MyD88 induces inflammatory cytokines, whereas TRIF induces type I interferons and inflammatory cytokines. TRAM and TIRAP are bridging adaptors that help to recruit and bind TRIF to TLR4 and MyD88 to TLR2, respectively (Takeuchi and Akira 2010). SARM functions as a negative regulator of NF-kB and IRF activation by blocking TRIF-dependent transcription factor activation (Carty et al. 2006).
MyD88 Signaling
MyD88 was the first characterized TLR adaptor and can signal downstream of all TLRs except TLR3. MyD88 binds to IRAK4 (IL-1 receptor-associated kinase), which can activate IRAK1 and IRAK2. The IRAKs then associate with the E3 ubiquitin ligase TRAF6 (TNFR-associated factor 6), which with E2-ubiquitin conjugating enzyme complex forms a polyubiquitin chain on TRAF6 (Xia et al. 2009). This polyubiquitin chain can activate kinases such as TAK1 (TGF-β-activating kinase-1) that phosphorylate and thus inactivate the inhibitor of NF-kB, IkBa. Free of its inhibitor, NF-kB can induce the expression of a cascade of pro-inflammatory genes upon translocation to the nucleus. MAPKs (mitogen-activated protein kinases) can also be activated through MyD88 signaling, leading to the induction of pro-inflammatory cytokines.
TRIF Signaling
TLR3 and TLR4 can both signal through the adaptor TRIF. Whereas TLR3 can bind directly to TRIF for signaling, TLR4 requires the adaptor TRAM to signal through TRIF. The TRIF-dependent pathway results in the activation of NF-kB and IRF3. Upon activation, TRIF binds to TRAF6, TRAF3 as well as RIP1 (C-terminal receptor-interacting protein-1) and RIP3. The TRAFs then associate with TRADD (TNFR-associated death domain protein) which, in combination with FADD (FAS-associated death domain-containing protein), can result in the ubiquitination of RIP1 and then the activation of NF-kB (Ermolaeva et al. 2008; Pobezinskaya et al. 2008).
TLRs in Host Defense
An evolutionarily conserved role for TLRs is in the host defense against pathogens. The first barriers encountered by most pathogens are surface epithelial cells that line the skin, lungs, gastrointestinal tract, and genitourinary tract. Signaling of TLRs in these tissues can lead to the production and secretion of antimicrobial factors such as α- and β-defensins, cathelicidin, phospholipase A2, and lysozyme. Moreover, release of these effectors can further enhance the immune response to signal through TLRs. Further, TLR signaling on immune cells such as macrophages and neutrophils leads to the release of the microbicidal compounds, reactive oxygen species, and reactive nitrogen intermediates.
Beyond inducing an acute innate immune response, signaling through TLRs is critical to establishing an adaptive immune response. Antigen uptake with concomitant TLR activation on DCs allows for the discrimination between self and non-self. One way in which appropriate antigens can be targeted by the adaptive immune system is by their proximity to the TLR ligand (Blander and Medzhitov 2004, 2006a, b). This has been demonstrated through cooccurrence of antigens and TLR ligands in DCs, allowing for efficient presentation of antigen on MHC Class II or through the ligation of an antigen to a TLR ligand enabling an efficient production of antibodies (Palm and Medzhitov 2009). Further, the appropriate immune response is determined by the general class of pathogen as determined by the detected TLR ligands. For instance, TLR4 recognizes LPS from Gram-negative bacteria, while TLR2 recognizes peptidoglycan from Gram-positive bacteria.
The adaptive immune response can be controlled by TLRs at multiple levels including the control of antigen uptake (West et al. 2004) and presentation (Blander and Medzhitov 2006b) by DCs, the maturation of DCs, cytokine production by antigen-presenting cells, and control of survival of activated T cells. Signaling through TLRs on B cells is crucial for activation, proliferation, immunoglobulin isotype class switching, and maturation during infection as well as immunization (Gerondakis et al. 2007). Further, TLRs can induce antibody production by memory B cells (Bernasconi et al. 2002).
Endogenous Ligands of TLRs
Exogenous, non-self molecules were the first identified and characterized TLR ligands. However, more recently, an increasing number of endogenous, self ligands have been identified and characterized (Karin et al. 2006; Kawai and Akira 2010). These endogenous ligands have in common their association with either infection or tissue destruction and cell death. Therefore, the ligands are more accurately described as altered self rather than self. Most of these endogenous ligands are released during tissue damage, such as that observed in tumour progression. The emerging list of endogenous ligands is complicated by the potential contamination of reagents with exogenous, pathogen-associated products. Therefore, biochemical analysis demonstrating direct interaction between endogenous ligands and TLRs will be required to address the skepticism that presently exists. Identification and characterization of endogenous ligands may be especially relevant to TAMs, as many tumours exist in a sterile environment. Therefore, for many tumour types, the TLR ligands that activate TAMs will likely be derived from an endogenous source.
Intracellular-Derived Ligands
Intracellular-derived endogenous ligands include nuclear proteins and heat shock proteins. HMGB1 (high-mobility group box 1) is a nuclear protein that can bind chromatin that is released during cell necrosis or inflammation (Scaffidi et al. 2002; Wang et al. 1999). HMGB1 has been reported to be recognized by a variety of TLRs including TLR2, TLR4, and TLR9 (Sims et al. 2010). In models of ischemia–reperfusion and septic shock, HMGB1 is proinflammatory. Neutralizing antibodies against HMGB1 in the TLR4−/− background are both protective in the ischemia–reperfusion model, suggesting that endogenous, non-pathogen-derived proinflammatory signaling is mediated through TLR4 (Tsung et al. 2005b). Further, other HMGB proteins – namely HMGB1, HMGB2, and HMGB3 have been found to function as universal sentinels for nucleic acids that can activate a variety of PRRs including TLRs, NLRs (NOD-like receptors), and RLRs (RIG-I-like receptors) (Yanai et al. 2009). As a DNA-binding protein, HMGB1 can bind both host- and pathogen-derived DNA. When the HMGB1–nucleic acid complex binds the RAGE (receptor for advanced glycation end products) receptor, it is endocytosed and presented to TLR9, where it leads to the activation of DCs and B cells (Tian et al. 2007). How the release of HMGB1 is regulated, whether through a non-classical secretory lysosomal pathway or during necrosis, has not yet been determined. However, the release of HMGB1 was found to be dependent on the cytosolic NLR, NLRP3, and its adaptor ASC (apoptotic speck-like protein containing a caspase recruitment domain) but independent of caspase-1 in a lung infection model (Willingham et al. 2009). Whether there is a physiologic correlate to controlled HMGB1 release has yet to be determined. However, HMGB1 is highly expressed in a variety of solid tumours including colon cancer, breast cancer, melanoma, prostate cancer, and pancreatic cancer. Further, this elevated expression of HMGB1 is associated with tumour progression and metastasis (Ellerman et al. 2007). One consequence of TLR signaling in TAMs by endogenous ligands was suggested in a report of the induction of apoptosis in activated T cells by TAMs that were stimulated by unidentified tumour-derived TLR4 ligands (Liu et al. 2010).
Heat-shock proteins including Hsp60, Hsp70, Hsp90, and gp96 have been reported to activate macrophages and DCs through TLR2 and TLR4. However, heat-shock proteins have also been shown to bind exogenous ligands for TLRs such as LPS and lipoproteins. Therefore, it is unclear whether the effects of these molecular chaperones is direct or through contamination (Tsan and Gao 2009).
TLR Ligands Induced by TLR Signaling
TLR signaling by PAMPs leads to the production of antimicrobial products. In a possible feed-forward mechanism of signal amplification, two of these products have been reported to signal through TLRs. β-Defensin-2 is a pore-forming antimicrobial protein secreted by mucosal epithelium in response to TLR signaling. However, it was also suggested to directly activate immature DCs to express costimulatory molecules and undergo maturation through TLR4, leading to an adaptive immune response (Biragyn et al. 2002). Cathelicidin (LL37) is an antimicrobial peptide that is secreted by keratinocytes and neutrophils upon TLR stimulation. In addition to its antimicrobial properties, LL37 can bind with host DNA or RNA released from necrotic cells and, upon phagocytosis of this aggregate, signal through TLR9 and TLR7, respectively (Ganguly et al. 2009; Lande et al. 2007).
A cellular byproduct of infection by the H5N1 avian influenza virus and from aspiration of acidic solutions that leads to TLR signaling is oxidized phospholipid. In a murine model of lung infection, both TLR4−/− and TRIF−/− mice were protected from the acute lung injury resulting from the avian flu infection, suggesting that this pathway is critical in the detection of this form of oxidative damage (Imai et al. 2008). Of note, all forms of acute lung injury examined including SARS (severe acute respiratory syndrome), pulmonary anthrax, monkey pox, and Yersinia pestis infection resulted in significantly elevated levels of oxidized phospholipids.
Extracellular Matrix Ligands
Altered extracellular matrix glycoproteins are another class of endogenous ligands of TLRs. Biglycan is a proteoglycan that binds collagen and is expressed in the extracellular matrix. Biglycan was found to induce pro-inflammatory cytokines in a TLR2- and TLR4-dependent manner (Schaefer et al. 2005). Further, biglycan-deficient mice were more resilient to shock induced by LPS or zymosan, and this was associated with lower levels of circulating TNFα. These findings suggest that release of biglycan from the extracellular matrix through stresses such as inflammation may result in a pro-inflammatory feed-forward mechanism.
Similar to biglycan, hyaluronan, a glycosaminoglycan, is a major constituent of the extracellular matrix. Hyaluronan is also a cell wall component of the bacteria Streptococcus groups A and C as well as Pasturella multocida (Jiang et al. 2007). Upon tissue damage or inflammation, small fragments of hyaluronan can be recognized by TLR2 and TLR4 to produce pro-inflammatory cytokines. Signaling through these TLRs may be important in tissue repair as TLR2- and TLR4-deficient mice challenged with bleomycin-induced sterile lung injury had greater lung pathology and a higher mortality rate than wild-type mice. The converse corollary experiment in which lung-specific overexpression of hyaluronan is protective of sterile injury supports the hypothesis that TLR signaling via hyaluronan is protective of the lung epithelium (Jiang et al. 2005). These findings suggest that the physiologic correlate of these systems may be that with small deviations from homeostasis, signaling by endogenous ligands through TLRs may be used to restore tissue integrity, whereas in a more severe infection with increased tissue damage, this mechanism may lead to immunopathology.
Versican, a proteoglycan of the extracellular matrix, was identified as the active component of media conditioned by Lewis lung carcinoma that led to the induction of pro-inflammatory cytokines by macrophages (Kim et al. 2009). The induction of these cytokines was determined to be through TLR2/TLR6 signaling. Further, mice deficient in TLR2 or its adaptor, MyD88, had a higher rate of survival and fewer metastases than the wild-type mice. In this study, direct binding of versican to TLR2 but not TLR4 was demonstrated. Whether the versican produced by Lewis lung carcinoma is altered in a way to make it detectable by TLRs is not known.
TLRs and Tissue Repair
TLR signaling has been found to have significant roles in tissue regeneration and repair (Kluwe et al. 2009; Rakoff-Nahoum and Medzhitov 2009). The process of tissue repair requires the clearance of damaged tissues, repopulation of lost cell types, reestablishment of the tissue vasculature and innervation, and remodeling of the overall tissue architecture.
TLR ligands can be categorized into exogenous and endogenous categories, based on from where they are derived. As such, upon damage of tissue, signaling through TLRs can be mediated by exogenous and endogenous ligands. Damage of epithelial surfaces, including the skin and intestine, compromise the integrity of these barriers, allowing for exposure to TLR ligands from microorganisms whether commensals or pathogens. In contrast, damage to internal organs that do not have surfaces colonized by mircroorganisms results in the release of stress signals, which can relay the nature and degree of tissue damage through TLRs.
Various models have demonstrated that TLR signaling can either prevent or promote tissue injury. In models of sterile lung injury using bleomycin, signaling through TLR2 and TLR4 was found to be protective of the lung epithelium. The endogenous ligand in this model was determined to be the extracellular matrix proteoglycan hyaluronan. When TLR signaling induced by hyaluronan was blocked with inhibitory peptides, the increased lung pathology was similar to that seen in the TLR2/TLR4 deficient mice (Jiang et al. 2005). In an analogous system, mice sterilized of their gut flora demonstrated increased intestinal injury after treatment with dextran sulfate sodium (DSS) compared with wild-type mice. Further, this increased DSS-induced intestinal damage was similar to that seen in MyD88 deficient mice, indicating that signals from the commensal bacteria is important in tissue preservation (Rakoff-Nahoum et al. 2004). One mechanism by which TLR signaling may result in tissue protection is the delivery of anti-apoptotic signals to cells, preventing cell loss. This may allow TLR signaling to establish the threshold of tolerable injury and cell death. Downstream products of TLR signaling such as cyclooxygenase-2 provide a signal for progenitor cells to proliferate, restoring the damaged tissue.
In other models of tissue injury, signaling through TLRs has been associated with increased tissue pathology. Ischemia followed by reperfusion results in inflammation and oxidative stress of the affected tissue. In various models of ischemia–reperfusion including liver, kidney, heart, and brain, TLR4-deficient mice are relatively protected (Oyama et al. 2004; Tang et al. 2007; Tsung et al. 2005b; Wu et al. 2007). The cells in which TLR signaling is critical for this pathology vary. For instance, in the liver, the abrogation of TLR4 signaling in hematopoietic cells is protective (Tsung et al. 2005a), whereas in the kidney, the abrogation of TLR4 signaling in parenchymal cells is protective (Zhang et al. 2008). HMGB1 is an endogenous TLR ligand that is upregulated in both liver and kidney after ischemia–reperfusion. Antibodies that bind and deplete HMGB1 after liver ischemia–reperfusion are protective of subsequent tissue damage. Further, the depletion of HMGB1 in mice deficient in both TLR2 and TLR4 does not confer any additional protection from tissue pathology (Tsung et al. 2005b). This suggests that the protection conferred in the TLR2 and TLR4 deficient mouse model is due to the loss of signaling downstream of TLR ligand HMGB1. Two extracellular matrix proteins known to be endogenous TLR ligands, biglycan and hyaluronan, are induced by ischemia–reperfusion (Wu et al. 2007), but their role in mediating tissue injury has yet to be determined.
TLR signaling also promotes tissue regeneration in several models. After resection of part of the liver, MyD88-deficient mice exhibit delayed regeneration of the liver (Seki et al. 2005). Although the ligands for TLRs leading to this regenerative effect of MyD88 signaling are not known, it is thought they may be from intestinal commensal bacteria as mice grown in germ-free conditions have similarly impaired liver regeneration after resection. Models of skin wound healing have also demonstrated that MyD88 deficient mice heal at a slower rate with less granulation tissue and fewer vessels within granulation tissue of the wound (Macedo et al. 2007).
TLRs in Cancer and Tumour-Associated Macrophages
Correlations between inflammation and cancer have been made over the past several hundred years. In some instances, it has been observed that infections correlate with the remission of tumours. Deidier observed that tumours resolved after patients developed venereal infections in the eighteenth century (Rakoff-Nahoum and Medzhitov 2009). In contrast, Virchow suggested in the nineteenth century that sites of chronic inflammation are the origin of some cancers (Balkwill and Mantovani 2001). Experimental models have demonstrated evidence supporting both of these observations, with TLR signaling leading to either the regression or the promotion of various tumour types. Further, genetic association studies have linked polymorphisms within various TLR loci (TLR1, TLR2, TLR3, TLR4, TLR6, and TLR10) to an increased risk of prostate, breast, colorectal, and nasopharyngeal cancers (El-Omar et al. 2008; Rakoff-Nahoum and Medzhitov 2009). Whether these TLR variants display a gain or loss of function remains to be determined. Although the cell types in which TLR signaling is relevant to disease outcomes have not firmly been established in all model cases, there is increasing evidence that TLR signaling in macrophages has a profound impact on tumour progression.
TLR Signaling Causes Tumour Regression
In the late nineteenth century, William Coley read and observed that postoperative infections after resection of tumours often lead to a better clinical outcome. To determine whether this was due to live microorganisms or their products, Coley generated a combination of killed Gram-positive and Gram-negative bacteria, which included Streptococcus pyogenes and Serratia marcescens, respectively (Hennessy et al. 2010). Intratumoural injection of these “toxins” was observed to have antitumour responses (Hallam et al. 2009). In the mid-twentieth century, Shear and Turner determined that LPS was the active antitumour component in Coley’s toxins (Rakoff-Nahoum and Medzhitov 2009). Therefore, TLR signaling likely mediated these original observations of antitumour response to TLR ligand injections.
Proof for the antitumour efficacy of TLR ligands comes in the form of two agents approved by the US Food and Drug Administration for the treatment of cancers. First, the Bacillus Calmette-Guerin (BCG) vaccine, a live attenuated strain of Mycobacterium bovis, is approved for the treatment of primary and relapsed superficial transitional cell bladder carcinoma. The use of this agent is mucosal via intravesicular administration into the bladder. The effect of the BCG vaccine may be through TLR2 and TLR4 signaling as abrogation of signaling through these TLRs either by knockout or by blocking antibodies inhibited the maturation of and proinflammatory cytokine production by myeloid DCs in model systems (Uehori et al. 2003).
Second, imiquimod is an imidazoquinoline analog of ssRNA that signals through TLR7. Imiquimod is approved by the US Food and Drug Administration for the treatment of superficial basal cell carcinomas and actinic keratoses (intraepidermal neoplasm of dysplastic keratinocytes). Imiquimod induces maturation and proinflammatory cytokine production in DCs and leads to a Th1 antitumour lymphocyte response (Clark et al. 2008; Schon and Schon 2008). TLR7 is also expressed on macrophages and keratinocytes. The critical responsive cell(s) by which this TLR7 ligand acts has yet to be characterized.
TLR signaling from endogenous ligands has recently been determined to have a profound impact on the clinical response to chemotherapy and radiation therapy (Apetoh et al. 2007). Treatment of solid tumours often includes chemotherapy and/or radiation therapy. The efficacy of these therapies has been attributed to their direct elimination of tumour cells. However, an adaptive immune response stemming from these destructive therapies was determined to affect clinical outcome. In mice and humans, dying tumour cells treated with chemotherapy or radiotherapy release the nuclear protein HMGB1, which activates the TLR4–MyD88 pathway in DCs leading to tumour antigen-specific T-cell immunity. The activation of TLR4 by HMGB1 is essential for efficient cross-presentation of tumour antigens and effective antitumour response. Further, a cohort of breast cancer patients carrying a sequence polymorphism of TLR4, which is hypo-responsive to LPS, was found to relapse more quickly after chemotherapy or radiation therapy than the wild-type allele (Apetoh et al. 2007).
Various TLR ligands are in clinical trials for the treatment of cancer, infections, and autoimmune diseases. Currently, CpG-based oligonucleotides that target TLR9 are in clinical trials for the treatment of non-small cell lung cancer (Krieg 2008). Other TLR9 ligands are in clinical trials for the treatment of non-Hodgkin’s lymphoma as well as prostate and colorectal cancer (Hennessy et al. 2010). Specific to the effect of TLR signaling in TAMs, injection of M13 bacteriophage into an ectopic tumour model of melanoma resulted in a MyD88-dependent shift from the alternatively activated M2 phenotype to the classically activated M1 phenotype. This shift to the M1 phenotype correlated with an increase production of proinflammatory cytokines and an influx of neutrophils into the tumour (Eriksson et al. 2009).
TLR Signaling Promotes Tumourigenesis
In contrast to the relatively protective effects resulting from TLR signaling described above, numerous studies have revealed that TLR signaling can conversely lead to tumour progression and metastasis. In a murine model of breast cancer metastasis, 4T1 mammary adenocarcinoma cells injected intravenously resulted in increased angiogenesis, vascular permeability, and tumour cell invasion in the group receiving intraperitoneal LPS compared with the control groups (Harmey et al. 2002). Analogously, in a murine model of colon carcinoma metastasis, CT26 colon adenocarcinoma cells injected intravenously developed an increased number of tumour nodules and lung weights in the group receiving intraperitoneal LPS than the control mice. In this case, TLR-signaling was dependent on a supportive cell type such as a TAM. This is likely because NF-kB signaling within the tumour cells which was found critical to the anti-apoptotic effects was observed in the wild-type but not the TLR4 mutant mice (Luo et al. 2004).
Whereas the initial studies on the tumour-promoting effects of TLR signaling used isolated TLR ligands, more recent studies have studied the effect of bacterial infection on tumourigenesis. The clearest example of how bacterial infection can promote tumourigenesis is the association of chronic infection with Helicobacter pylori and the development of gastric cancer. To study the role of infection on tumour progression, Listeria moncytogenes, a Gram-positive facultative intracellular bacterium, was injected into ectopically implanted H22 hepatocellular carcinoma cells. The Listeria survived in larger but not smaller tumours. Further, Listeria increased growth of these tumours, which could be abrogated with silencing of TLR2 but not TLR4 expression (Huang et al. 2007).
MyD88 signaling is crucial for tumour progression in both spontaneous Apcmin/+ model and the azoxymethane chemical carcinogenesis model of intestinal tumourigenesis. In the first model, Apcmin/+ mice lack one copy of the adenomatous polyposis coli (APC) tumour suppressor gene. Therefore, upon loss of the working copy of the gene, development of a focus of atypical epithelia begins. Apcmin/+ MyD88−/− mice had fewer and smaller polyps than Apcmin/+ mice; however, the number of microadenomas was not different between the Apcmin/+ MyD88−/− mice and the Apcmin/+ mice. Similarly, in azoxymethane-induced carcinogenesis, the incidence of tumour formation was decreased in the MyD88−/− mice. Therefore, MyD88 signaling is essential for tumour progression but not initiation (Rakoff-Nahoum and Medzhitov 2007).
TAMs are associated with a worse clinical outcome in a majority of tumour types. Yet, few tumour-derived TLR ligands that activate TAMs to promote tumour progression and metastasis have been identified and characterized. One clear example was the product of a biochemical screen of macrophage-activating factors secreted by tumours. The extracellular matrix protein versican produced by Lewis lung carcinoma cells induced the secretion of IL-6 and TNFα by macrophages through TLR2/TLR6 signaling. Further, direct binding of TLR2 to versican was demonstrated. Abrogation of signaling through TLR2/TLR6 and MyD88 resulted in increased survival and fewer metastases in a murine model of metastatic lung cancer (Kim et al. 2009).
Conclusions
Tumour progression has long been associated with inflammation. In particular, increased macrophage density in solid tumours as well as lymphomas has been associated with a poorer prognosis. Inherent to cancer is the loss of normal tissue architecture, which may provide signals or perpetual tissue stress and damage. Cancers have been compared with wounds that do not heal (Dvorak 1986) and they both have significant overlap in their gene expression signatures (Chang et al. 2004). Among the signals for tissue damage are endogenous TLR ligands. As macrophages have the physiologic role of restoring tissue integrity and homeostasis after tissue damage, cancers exploit them as a rich source of growth factors and angiogenic factors (Pollard 2009). Future therapeutic opportunities to modulate the progression of cancer will come from understanding the signals produced by tumours, and the pathways they educate macrophages into trophic TAMs. In addition, early studies suggest that TLR signaling may enable the production of an acquired immune response and, therefore, a more durable remission after treatment. Dissecting and modulating both the trophic and acquired immune responses from TLR signaling will be challenging but will have great therapeutic promise.
References
Alexopoulou L, Holt AC, Medzhitov R, Flavell RA (2001) Recognition of double-stranded RNA and activation of NF-kappaB by Toll-like receptor 3. Nature 413:732–738
Apetoh L, Ghiringhelli F, Tesniere A, Obeid M, Ortiz C, Criollo A, Mignot G, Maiuri MC, Ullrich E, Saulnier P et al (2007) Toll-like receptor 4-dependent contribution of the immune system to anticancer chemotherapy and radiotherapy. Nat Med 13:1050–1059
Balkwill F, Mantovani A (2001) Inflammation and cancer: back to Virchow? Lancet 357:539–545
Bernasconi NL, Traggiai E, Lanzavecchia A (2002) Maintenance of serological memory by polyclonal activation of human memory B cells. Science 298:2199–2202
Biragyn A, Ruffini PA, Leifer CA, Klyushnenkova E, Shakhov A, Chertov O, Shirakawa AK, Farber JM, Segal DM, Oppenheim JJ et al (2002) Toll-like receptor 4-dependent activation of dendritic cells by beta-defensin 2. Science 298:1025–1029
Blander JM, Medzhitov R (2004) Regulation of phagosome maturation by signals from toll-like receptors. Science 304:1014–1018
Blander JM, Medzhitov R (2006a) On regulation of phagosome maturation and antigen presentation. Nat Immunol 7:1029–1035
Blander JM, Medzhitov R (2006b) Toll-dependent selection of microbial antigens for presentation by dendritic cells. Nature 440:808–812
Carty M, Goodbody R, Schroder M, Stack J, Moynagh PN, Bowie AG (2006) The human adaptor SARM negatively regulates adaptor protein TRIF-dependent Toll-like receptor signaling. Nat Immunol 7:1074–1081
Chang HY, Sneddon JB, Alizadeh AA, Sood R, West RB, Montgomery K, Chi JT, van de Rijn M, Botstein D, Brown PO (2004) Gene expression signature of fibroblast serum response predicts human cancer progression: similarities between tumors and wounds. PLoS Biol 2:E7
Clark RA, Huang SJ, Murphy GF, Mollet IG, Hijnen D, Muthukuru M, Schanbacher CF, Edwards V, Miller DM, Kim JE et al (2008) Human squamous cell carcinomas evade the immune response by down-regulation of vascular E-selectin and recruitment of regulatory T cells. J Exp Med 205:2221–2234
Coban C, Ishii KJ, Kawai T, Hemmi H, Sato S, Uematsu S, Yamamoto M, Takeuchi O, Itagaki S, Kumar N et al (2005) Toll-like receptor 9 mediates innate immune activation by the malaria pigment hemozoin. J Exp Med 201:19–25
Condeelis J, Pollard JW (2006) Macrophages: obligate partners for tumor cell migration, invasion, and metastasis. Cell 124:263–266
Dvorak HF (1986) Tumors: wounds that do not heal. Similarities between tumor stroma generation and wound healing. N Engl J Med 315:1650–1659
Ellerman JE, Brown CK, de Vera M, Zeh HJ, Billiar T, Rubartelli A, Lotze MT (2007) Masquerader: high mobility group box-1 and cancer. Clin Cancer Res 13:2836–2848
El-Omar EM, Ng MT, Hold GL (2008) Polymorphisms in Toll-like receptor genes and risk of cancer. Oncogene 27:244–252
Eriksson F, Tsagozis P, Lundberg K, Parsa R, Mangsbo SM, Persson MA, Harris RA, Pisa P (2009) Tumor-specific bacteriophages induce tumor destruction through activation of tumor-associated macrophages. J Immunol 182:3105–3111
Ermolaeva MA, Michallet MC, Papadopoulou N, Utermohlen O, Kranidioti K, Kollias G, Tschopp J, Pasparakis M (2008) Function of TRADD in tumor necrosis factor receptor 1 signaling and in TRIF-dependent inflammatory responses. Nat Immunol 9:1037–1046
Ganguly D, Chamilos G, Lande R, Gregorio J, Meller S, Facchinetti V, Homey B, Barrat FJ, Zal T, Gilliet M (2009) Self-RNA-antimicrobial peptide complexes activate human dendritic cells through TLR7 and TLR8. J Exp Med 206:1983–1994
Gerondakis S, Grumont RJ, Banerjee A (2007) Regulating B-cell activation and survival in response to TLR signals. Immunol Cell Biol 85:471–475
Hallam S, Escorcio-Correia M, Soper R, Schultheiss A, Hagemann T (2009) Activated macrophages in the tumour microenvironment-dancing to the tune of TLR and NF-kappaB. J Pathol 219:143–152
Harmey JH, Bucana CD, Lu W, Byrne AM, McDonnell S, Lynch C, Bouchier-Hayes D, Dong Z (2002) Lipopolysaccharide-induced metastatic growth is associated with increased angiogenesis, vascular permeability and tumor cell invasion. Int J Cancer 101:415–422
Hennessy EJ, Parker AE, O’Neill LA (2010) Targeting Toll-like receptors: emerging therapeutics? Nat Rev Drug Discov 9:293–307
Huang B, Zhao J, Shen S, Li H, He KL, Shen GX, Mayer L, Unkeless J, Li D, Yuan Y et al (2007) Listeria monocytogenes promotes tumor growth via tumor cell toll-like receptor 2 signaling. Cancer Res 67:4346–4352
Imai Y, Kuba K, Neely GG, Yaghubian-Malhami R, Perkmann T, van Loo G, Ermolaeva M, Veldhuizen R, Leung YH, Wang H et al (2008) Identification of oxidative stress and Toll-like receptor 4 signaling as a key pathway of acute lung injury. Cell 133:235–249
Jiang D, Liang J, Fan J, Yu S, Chen S, Luo Y, Prestwich GD, Mascarenhas MM, Garg HG, Quinn DA et al (2005) Regulation of lung injury and repair by Toll-like receptors and hyaluronan. Nat Med 11:1173–1179
Jiang D, Liang J, Noble PW (2007) Hyaluronan in tissue injury and repair. Annu Rev Cell Dev Biol 23:435–461
Karin M, Lawrence T, Nizet V (2006) Innate immunity gone awry: linking microbial infections to chronic inflammation and cancer. Cell 124:823–835
Kawai T, Akira S (2010) The role of pattern-recognition receptors in innate immunity: update on Toll-like receptors. Nat Immunol 11:373–384
Kim S, Takahashi H, Lin WW, Descargues P, Grivennikov S, Kim Y, Luo JL, Karin M (2009) Carcinoma-produced factors activate myeloid cells through TLR2 to stimulate metastasis. Nature 457:102–106
Kluwe J, Mencin A, Schwabe RF (2009) Toll-like receptors, wound healing, and carcinogenesis. J Mol Med 87:125–138
Krieg AM (2008) Toll-like receptor 9 (TLR9) agonists in the treatment of cancer. Oncogene 27:161–167
Lande R, Gregorio J, Facchinetti V, Chatterjee B, Wang YH, Homey B, Cao W, Su B, Nestle FO, Zal T et al (2007) Plasmacytoid dendritic cells sense self-DNA coupled with antimicrobial peptide. Nature 449:564–569
Lin EY, Nguyen AV, Russell RG, Pollard JW (2001) Colony-stimulating factor 1 promotes progression of mammary tumors to malignancy. J Exp Med 193:727–740
Liu YY, Sun LC, Wei JJ, Li D, Yuan Y, Yan B, Liang ZH, Zhu HF, Xu Y, Li B et al (2010) Tumor cell-released TLR4 ligands stimulate Gr-1+ CD11b+ F4/80+ cells to induce apoptosis of activated T cells. J Immunol 185:2773–2782
Luo JL, Maeda S, Hsu LC, Yagita H, Karin M (2004) Inhibition of NF-kappaB in cancer cells converts inflammation-induced tumor growth mediated by TNFalpha to TRAIL-mediated tumor regression. Cancer Cell 6:297–305
Macedo L, Pinhal-Enfield G, Alshits V, Elson G, Cronstein BN, Leibovich SJ (2007) Wound healing is impaired in MyD88-deficient mice: a role for MyD88 in the regulation of wound healing by adenosine A2A receptors. Am J Pathol 171:1774–1788
Mancuso G, Gambuzza M, Midiri A, Biondo C, Papasergi S, Akira S, Teti G, Beninati C (2009) Bacterial recognition by TLR7 in the lysosomes of conventional dendritic cells. Nat Immunol 10:587–594
Medzhitov R, Preston-Hurlburt P, Janeway CA Jr (1997) A human homologue of the Drosophila Toll protein signals activation of adaptive immunity. Nature 388:394–397
O’Neill LA, Bowie AG (2007) The family of five: TIR-domain-containing adaptors in Toll-like receptor signalling. Nat Rev Immunol 7:353–364
Oyama J, Blais C Jr, Liu X, Pu M, Kobzik L, Kelly RA, Bourcier T (2004) Reduced myocardial ischemia-reperfusion injury in toll-like receptor 4-deficient mice. Circulation 109:784–789
Palm NW, Medzhitov R (2009) Pattern recognition receptors and control of adaptive immunity. Immunol Rev 227:221–233
Parroche P, Lauw FN, Goutagny N, Latz E, Monks BG, Visintin A, Halmen KA, Lamphier M, Olivier M, Bartholomeu DC et al (2007) Malaria hemozoin is immunologically inert but radically enhances innate responses by presenting malaria DNA to Toll-like receptor 9. Proc Natl Acad Sci USA 104:1919–1924
Pobezinskaya YL, Kim YS, Choksi S, Morgan MJ, Li T, Liu C, Liu Z (2008) The function of TRADD in signaling through tumor necrosis factor receptor 1 and TRIF-dependent Toll-like receptors. Nat Immunol 9:1047–1054
Pollard JW (2004) Tumour-educated macrophages promote tumour progression and metastasis. Nat Rev Cancer 4:71–78
Pollard JW (2009) Trophic macrophages in development and disease. Nat Rev Immunol 9:259–270
Rakoff-Nahoum S, Medzhitov R (2007) Regulation of spontaneous intestinal tumorigenesis through the adaptor protein MyD88. Science 317:124–127
Rakoff-Nahoum S, Medzhitov R (2009) Toll-like receptors and cancer. Nat Rev Cancer 9:57–63
Rakoff-Nahoum S, Paglino J, Eslami-Varzaneh F, Edberg S, Medzhitov R (2004) Recognition of commensal microflora by toll-like receptors is required for intestinal homeostasis. Cell 118:229–241
Scaffidi P, Misteli T, Bianchi ME (2002) Release of chromatin protein HMGB1 by necrotic cells triggers inflammation. Nature 418:191–195
Schaefer L, Babelova A, Kiss E, Hausser HJ, Baliova M, Krzyzankova M, Marsche G, Young MF, Mihalik D, Gotte M et al (2005) The matrix component biglycan is proinflammatory and signals through Toll-like receptors 4 and 2 in macrophages. J Clin Invest 115:2223–2233
Schon MP, Schon M (2008) TLR7 and TLR8 as targets in cancer therapy. Oncogene 27:190–199
Seki E, Tsutsui H, Iimuro Y, Naka T, Son G, Akira S, Kishimoto T, Nakanishi K, Fujimoto J (2005) Contribution of Toll-like receptor/myeloid differentiation factor 88 signaling to murine liver regeneration. Hepatology 41:443–450
Sims GP, Rowe DC, Rietdijk ST, Herbst R, Coyle AJ (2010) HMGB1 and RAGE in inflammation and cancer. Annu Rev Immunol 28:367–388
Takeuchi O, Akira S (2010) Pattern recognition receptors and inflammation. Cell 140:805–820
Tang SC, Arumugam TV, Xu X, Cheng A, Mughal MR, Jo DG, Lathia JD, Siler DA, Chigurupati S, Ouyang X et al (2007) Pivotal role for neuronal Toll-like receptors in ischemic brain injury and functional deficits. Proc Natl Acad Sci USA 104:13798–13803
Tian J, Avalos AM, Mao SY, Chen B, Senthil K, Wu H, Parroche P, Drabic S, Golenbock D, Sirois C et al (2007) Toll-like receptor 9-dependent activation by DNA-containing immune complexes is mediated by HMGB1 and RAGE. Nat Immunol 8:487–496
Tsan MF, Gao B (2009) Heat shock proteins and immune system. J Leukoc Biol 85:905–910
Tsung A, Hoffman RA, Izuishi K, Critchlow ND, Nakao A, Chan MH, Lotze MT, Geller DA, Billiar TR (2005a) Hepatic ischemia/reperfusion injury involves functional TLR4 signaling in nonparenchymal cells. J Immunol 175:7661–7668
Tsung A, Sahai R, Tanaka H, Nakao A, Fink MP, Lotze MT, Yang H, Li J, Tracey KJ, Geller DA et al (2005b) The nuclear factor HMGB1 mediates hepatic injury after murine liver ischemia-reperfusion. J Exp Med 201:1135–1143
Uehori J, Matsumoto M, Tsuji S, Akazawa T, Takeuchi O, Akira S, Kawata T, Azuma I, Toyoshima K, Seya T (2003) Simultaneous blocking of human Toll-like receptors 2 and 4 suppresses myeloid dendritic cell activation induced by Mycobacterium bovis bacillus Calmette-Guerin peptidoglycan. Infect Immun 71:4238–4249
Uematsu S, Fujimoto K, Jang MH, Yang BG, Jung YJ, Nishiyama M, Sato S, Tsujimura T, Yamamoto M, Yokota Y et al (2008) Regulation of humoral and cellular gut immunity by lamina propria dendritic cells expressing Toll-like receptor 5. Nat Immunol 9:769–776
Wang H, Bloom O, Zhang M, Vishnubhakat JM, Ombrellino M, Che J, Frazier A, Yang H, Ivanova S, Borovikova L et al (1999) HMG-1 as a late mediator of endotoxin lethality in mice. Science 285:248–251
West MA, Wallin RP, Matthews SP, Svensson HG, Zaru R, Ljunggren HG, Prescott AR, Watts C (2004) Enhanced dendritic cell antigen capture via toll-like receptor-induced actin remodeling. Science 305:1153–1157
Wiktor-Jedrzejczak W, Bartocci A, Ferrante AW Jr, Ahmed-Ansari A, Sell KW, Pollard JW, Stanley ER (1990) Total absence of colony-stimulating factor 1 in the macrophage-deficient osteopetrotic (op/op) mouse. Proc Natl Acad Sci USA 87:4828–4832
Willingham SB, Allen IC, Bergstralh DT, Brickey WJ, Huang MT, Taxman DJ, Duncan JA, Ting JP (2009) NLRP3 (NALP3, Cryopyrin) facilitates in vivo caspase-1 activation, necrosis, and HMGB1 release via inflammasome-dependent and -independent pathways. J Immunol 183:2008–2015
Wu H, Chen G, Wyburn KR, Yin J, Bertolino P, Eris JM, Alexander SI, Sharland AF, Chadban SJ (2007) TLR4 activation mediates kidney ischemia/reperfusion injury. J Clin Invest 117:2847–2859
Xia ZP, Sun L, Chen X, Pineda G, Jiang X, Adhikari A, Zeng W, Chen ZJ (2009) Direct activation of protein kinases by unanchored polyubiquitin chains. Nature 461:114–119
Yanai H, Ban T, Wang Z, Choi MK, Kawamura T, Negishi H, Nakasato M, Lu Y, Hangai S, Koshiba R et al (2009) HMGB proteins function as universal sentinels for nucleic-acid-mediated innate immune responses. Nature 462:99–103
Zhang D, Zhang G, Hayden MS, Greenblatt MB, Bussey C, Flavell RA, Ghosh S (2004) A Toll-like receptor that prevents infection by uropathogenic bacteria. Science 303:1522–1526
Zhang B, Ramesh G, Uematsu S, Akira S, Reeves WB (2008) TLR4 signaling mediates inflammation and tissue injury in nephrotoxicity. J Am Soc Nephrol 19:923–932
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2011 Springer Science+Business Media, LLC
About this chapter
Cite this chapter
Colegio, O.R., Medzhitov, R. (2011). TLR Signaling and Tumour-Associated Macrophages. In: Lawrence, T., Hagemann, T. (eds) Tumour-Associated Macrophages. Springer, New York, NY. https://doi.org/10.1007/978-1-4614-0662-4_9
Download citation
DOI: https://doi.org/10.1007/978-1-4614-0662-4_9
Published:
Publisher Name: Springer, New York, NY
Print ISBN: 978-1-4614-0661-7
Online ISBN: 978-1-4614-0662-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)