Abstract
Background
Recently, several randomized trials have noted improved outcomes with staged percutaneous coronary intervention (PCI) of nonculprit vessels in patients with ST-segment elevation myocardial infarction (STEMI) and multivessel disease. However, it remains unclear whether diabetes status affects the outcomes after different revascularization strategies. This study thus compared the impact of diabetes status on long-term outcomes after staged complete revascularization with that after culprit-only PCI.
Methods
From January 2006 to December 2015, 371 diabetic patients (staged PCI: 164, culprit-only PCI: 207) and 834 nondiabetic patients (staged PCI: 412, culprit-only PCI: 422) with STEMI and multivessel disease were enrolled. The primary endpoint was 5-year major adverse cardiac and cerebrovascular event (MACCE), defined as a composite of all-cause death, myocardial infarction (MI), stroke or unplanned revascularization.
Results
The rate of the 5-year composite primary endpoint for diabetic patients was close to that for nondiabetic patients (34.5% vs. 33.7%; adjusted hazard ratio [HR] 1.012, 95% confidence interval [CI] 0.815–1.255). In nondiabetic patients, the 5-year risks of MACCE (31.8% vs. 35.5%; adjusted HR 0.638, 95% CI 0.500–0.816), MI (4.6% vs. 9.2%; adjusted HR 0.358, 95% CI 0.200–0.641), unplanned revascularization (19.9% vs. 24.9%; adjusted HR 0.532, 95% CI 0.393–0.720), and the composite of cardiac death, MI or stroke (11.4% vs. 15.2%; adjusted HR 0.621, 95% CI 0.419–0.921) were significantly lower after staged PCI than after culprit-only PCI. In contrast, no significant difference was found between the two groups with respect to MACCE, MI, unplanned revascularization, and the composite of cardiac death, MI or stroke in diabetic patients. Significant interactions were found between diabetes status and revascularization assignment for the composite of cardiac death, MI or stroke (Pinteraction = 0.013), MI (Pinteraction = 0.005), and unplanned revascularization (Pinteraction = 0.013) at 5 years. In addition, the interaction tended to be significant for the primary endpoint of MACCE (Pinteraction = 0.053). Moreover, the results of propensity score-matching analysis were concordant with the overall analysis in both diabetic and nondiabetic population.
Conclusions
In patients with STEMI and multivessel disease, diabetes is not an independent predictor of adverse cardiovascular events at 5 years. In nondiabetic patients, an approach of staged complete revascularization is superior to culprit-only PCI, whereas the advantage of staged PCI is attenuated in diabetic patients.
Trial registration This study was not registered in an open access database
Similar content being viewed by others
Background
Primary percutaneous coronary intervention (PCI) is currently the standard care for patients with ST-segment elevation myocardial infarction (STEMI). Approximately 50% of these patients have multivessel disease and present worse clinical outcomes compared with those having single-vessel disease [1, 2]. Although several previous small-scale randomized controlled trials (RCTs) and registries [3,4,5,6,7,8] supported a conservative approach for nonculprit diseases, recent landmark RCTs have improved outcomes with immediate or staged complete revascularization [9,10,11,12]. Accordingly, the latest European Society of Cardiology guideline upgraded the recommendation for nonculprit lesions revascularization during primary PCI or as a staged procedure over culprit-only PCI [13].
Diabetes is a strong independent predictor of adverse cardiovascular events in patients with coronary artery disease (CAD) [14,15,16,17,18]. Over recent decades, the prevalence of diabetes mellitus is dramatically increased from 108 million in 1980 to 451 million in 2017 [19, 20]. Generally, diabetic patients are prone to a diffuse and rapidly progressive form of atherosclerosis. This increases the risk of unfavorable clinical outcomes after revascularization [21, 22]. In this setting, diabetes might be an important consideration when choosing a revascularization strategy, i.e., staged complete revascularization or culprit-only PCI in patients with STEMI and multivessel disease.
Nevertheless, the relation between the effect of diabetes and different strategies remains underdetermined. These high-risk patients are generally underrepresented by RCTs, with a small proportion of diabetic patients enrolled [9,10,11,12]. In a study conducted by Hamza et al. [23], diabetic patients underwent complete revascularization with STEMI and multivessel disease were significantly associated with lower risk of adverse cardiovascular events than that in culprit-only PCI group. However, the limitations of their study were the small sample size and a short follow-up period of only 6 months. We therefore performed this study to compare the impact of diabetes status on long-term outcomes of patients with STEMI and multivessel disease after staged complete revascularization with that after culprit-only PCI.
Methods
Study design and population
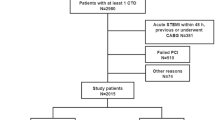
The present report is a single-center, retrospective, observational study. The study design has been previously described [24]. Briefly, a total of 1205 patients with STEMI and multivessel disease who underwent primary PCI within 12 h from symptom onset underwent staged complete revascularization or culprit-only PCI between January 2006 and December 2015 in our center. The local ethical committee approved the study, and the written informed consent was waived because of the retrospective enrollment. In addition, patient records were anonymized and deidentified before database merging and analysis.
Diabetes mellitus was diagnosed based on previous medical records as well as therapeutic status of glucose-lowering therapy, i.e., insulin, oral hypoglycemic agents, diet and exercise. Multivessel disease was defined as the presence of ≥ 70% angiographic stenosis in ≥ 1 nonculprit major coronary arteries (with diameter ≥ 2.5 mm). Exclusion criteria were single-vessel disease (n = 1390), left main disease (n = 40), concomitant chronic total occlusion (n = 307), rescue PCI (n = 116), immediate complete revascularization (n = 81), undergoing coronary artery bypass graft surgery (n = 97), receiving medical therapy only (n = 34), or being dead during hospitalization (n = 16).
Study procedures
All patients received loading doses of aspirin (300 mg), clopidogrel (600 mg) or ticagrelor (180 mg) before primary PCI. The culprit vessel was ascertained by evaluation of electrocardiographic changes, echocardiographic and angiographic findings. Primary PCI as well as the use of heparin, thrombus aspiration, and glycoprotein IIb/IIIa inhibitor were in compliance with the current guidelines and the operators’ routine practice [13, 25]. After the procedure, aspirin (100 mg/day) and clopidogrel (75 mg/day) or ticagrelor (180 mg/day) were prescribed at the same time every day. Culprit-only PCI was defined as the treatment of the culprit vessel only at the time of primary PCI without revascularization of nonculprit vessels during the following 30 days after primary PCI. In the staged PCI group, revascularization of significant nonculprit lesions was performed within 30 days after the procedure, which was determined by the physicians and/or patients. Contrast-induced acute kidney injury was defined as an increase in serum creatinine of ≥ 25% compared with baseline values or as an absolute increase in serum creatinine of ≥ 0.5 mg/dL (44.2 mmol/L) within 72 h after PCI [26, 27].
Follow-up and endpoints
Demographics, cardiovascular risk factors, clinical characteristics, laboratory data, angiographic and procedural details were collected from hospital databases and recorded in a computerized database. Follow-up information was obtained from the review of hospital charts, clinical visits or telephone interviews, which were conducted by trained reviewers. In order to record at least 2-year follow-up information about all patients, we extended the follow-up period to May 31, 2018.
The primary endpoint was major adverse cardiac and cerebrovascular event (MACCE), defined as a composite of all-cause death, myocardial infarction (MI), stroke, or unplanned revascularization. Secondary outcomes included the individual components of the primary endpoint as well as cardiac death, and the composite of cardiac death, MI or stroke. All deaths were considered to be cardiac-related unless a non-cardiac origin was documented. Diagnosis of MI was made according to fourth universal definition of MI [28]. Stroke was defined as a new focal neurological deficit lasting > 24 h, which was confirmed by neurologists based on both clinical and radiographic criteria [29]. Unplanned revascularization was repeat PCI or coronary artery bypass grafting of any vessels excluding staged PCI. In addition, all the endpoints were verified and adjudicated by an independent clinical events committee (XTS, HL and SZL).
Statistical analysis
Continuous variables were expressed as mean ± standard deviation or median (interquartile range), and were compared using the Student’s t test and Mann–Whitney U test according to different distributions. Categorical variables were expressed as number (percentage), and were compared using the Chi-square test or Fisher’s exact test. The Kaplan–Meier method was used to plot time-to-event curves, and differences were assessed using log-rank test. To find predictors of clinical events, Cox proportional hazard model analysis was conducted to provide adjusted hazard ratios (HRs) with 95% confidence intervals (CIs). Variables in Table 1 (without laboratory data) with P ≤ 0.1 at the univariate analysis were entered into multivariate Cox regression analysis. In particular, formal interaction testing was performed between diabetes status and revascularization treatment on all clinical outcomes.
To adjust for potential confounders from the real world, a double 1:1 propensity score-matching analysis (staged PCI vs. culprit-only PCI groups) without replacement, on the basis of the nearest neighbor in terms of Mahalanobis distance with a caliper of 0.02, was performed in each subgroup of patients, i.e., nondiabetic and diabetic patients. To estimate the propensity score, a logistic regression model was used including variables of age, gender, current smoking, hypertension, previous MI, previous PCI, peripheral vascular disease, chronic kidney disease, time from symptom onset to PCI, heart rate, access site of PCI, Killip class III/IV, number of diseased vessels, culprit vessel of left anterior descending coronary artery, nonculprit vessel of left anterior descending coronary artery, thrombus aspiration, intra-aortic balloon pump, stent length, use of angiotensin-converting enzyme inhibitors or angiotensin receptor blockers and use of β-blockers. In addition, to assess the robustness of the results, long-term outcomes of patients undergoing staged PCI within 10 days were compared with those in culprit-only PCI group not undergoing revascularization of nonculprit vessels during the following 10 days after primary PCI in both nondiabetic and diabetic population.
Statistical analyses were conducted using SPSS 23.0 (SPSS Inc., Chicago, Illinois, USA) and STATA 12.0 (StataCorp, College Station, Texas, USA). A two-sided P value of < 0.05 was considered to indicate statistical significance.
Results
Baseline patient, angiographic and procedural characteristics
Among the 1205 patients with STEMI and multivessel disease who received staged complete revascularization (n = 576) or culprit-only PCI (n = 629), 371 (30.8%) had diabetes mellitus, of which 164 (44.2%) received staged PCI and 207 (55.8%) underwent culprit-only PCI. Among the remaining 834 nondiabetic patients, 412 (49.4%) received staged PCI and 422 (50.6%) underwent culprit-only PCI. Staged PCI was performed after a median time of 6 days in both nondiabetic and diabetic cohorts. The staged procedures were performed within 10 days after primary PCI in 89.0% (n = 146) of the diabetic patients and 90.3% (n = 372) of the nondiabetic patients. The mean follow-up period was 5.01 years.
Compared with nondiabetic patients, diabetic patients were less likely to be male (P = 0.031) and current smokers (P = 0.032) and to receive thrombus aspiration (P = 0.021), but were more likely to receive β-blockers (P = 0.006) with longer time from symptom to intervention (P = 0.009) (Table 1). In diabetic patients, those who underwent staged PCI were more likely to be male (P = 0.006), had less culprit vessels of left anterior descending coronary artery (P = 0.003), and were less frequently to receive transradial PCI (P < 0.001) and defibrillator (P = 0.016) than those who received culprit-only PCI. In nondiabetic patients, those who underwent staged PCI were younger (P = 0.001), had lower prevalence rates of chronic kidney disease (P = 0.013) and Killip class III/IV (P = 0.010), had more three-vessel disease (P < 0.001), nonculprit vessels of left anterior descending coronary artery (P = 0.003), were more frequently to use intra-aortic balloon pump (P = 0.006), angiotensin converting enzyme inhibitor/angiotensin receptor blocker (P < 0.001) during hospitalization, and less likely to receive transradial PCI (P < 0.001) and temporary pacemaker (P = 0.027). Besides, patients who underwent staged PCI had lower heart rates (P = 0.010), shorter time from symptom to intervention (P = 0.004), and shorter total stent length (P = 0.010) than those who underwent culprit-only PCI (Table 2).
Comparison of 5-year outcomes between diabetic and nondiabetic patients
Clinical outcomes according to diabetes status are shown in Table 3 and Fig. 1. The 5-year incidences of MACCE (34.5% vs. 33.7%; HR 1.075, 95% CI 0.872 to 1.325) and a composite of cardiac death, MI or stroke (12.4% vs. 13.3%; HR 0.976, 95% CI 0.692 to 1.377) were similar in diabetic patients and nondiabetic patients. In addition, the risks of all-cause death, cardiac death, MI, stroke, and unplanned revascularization were not significantly different between those two groups.
After adjusting potential confounders, diabetes was not independently associated with the primary endpoint of MACCE (Adjusted HR 1.012, 95% CI 0.815 to 1.255), and the composite of cardiac death, MI or stroke (Adjusted HR 0.869, 95% CI 0.608 to 1.242) at 5 years. Notably, the strategy of culprit-only PCI (P = 0.010), previous stroke (P = 0.012), chronic kidney disease (P = 0.016), and high systolic blood pressure (P = 0.021) were independently associated with the higher incidence of MACCE at 5 years (Table 4).
Comparison of 5-year outcomes between staged complete revascularization and culprit-only PCI
Among nondiabetic patients, patients who received staged PCI presented lower risks of MACCE (31.8% vs. 35.5%; HR 0.643, 95% CI 0.507 to 0.815), MI (4.6% vs. 9.2%; HR 0.346, 95% CI 0.199 to 0.601), unplanned revascularization (19.9% vs. 24.9%; HR 0.625, 95% CI 0.466 to 0.837), and the composite of cardiac death, MI or stroke (11.4% vs. 15.2%; HR 0.529, 95% CI 0.362 to 0.774) than those who underwent culprit-only PCI (Table 5 and Fig. 2). No significant difference was found between the two revascularization strategies with respect to all-cause mortality, cardiac mortality, and stroke. After the potential confounders were adjusted, staged PCI was associated with a decrease in the risk of the primary endpoint of MACCE (Adjusted HR 0.638, 95% CI 0.500 to 0.816), MI (Adjusted HR 0.358, 95% CI 0.200 to 0.641), unplanned revascularization (Adjusted HR 0.532, 95% CI 0.393 to 0.720), and the composite of cardiac death, MI or stroke (Adjusted HR 0.621, 95% CI 0.419 to 0.921) in nondiabetic patients.
In diabetic patients, the incidences of the primary endpoint of MACCE (37.8% vs. 31.9%; HR 0.939, 95% CI 0.662 to 1.331) and the secondary outcomes were comparable between the two revascularization therapies (Table 5 and Fig. 3). After the potential confounders were adjusted, staged PCI was not independently associated with MACCE (Adjusted HR 0.986, 95% CI 0.683 to 1.422) and the secondary endpoints of the composite of cardiac death, MI or stroke (Adjusted HR 1.593, 95% CI 0.846 to 3.000), all-cause death (Adjusted HR 0.876, 95% CI 0.404 to 1.898), cardiac death (Adjusted HR 0.840, 95% CI 0.304 to 2.316), MI (Adjusted HR 1.599, 95% CI 0.663 to 3.858), stroke (Adjusted HR 0.857, 95% CI 0.248 to 2.964) and unplanned revascularization (Adjusted HR 1.038, 95% CI 0.672 to 1.605) at 5 years.
By formal interaction testing, significant interactions were found between diabetes status and revascularization assignment for the composite of cardiac death, MI or stroke (Pinteraction = 0.013), MI (Pinteraction = 0.005), and unplanned revascularization (Pinteraction = 0.013) at 5 years. In addition, the interaction tended to be significant for the primary endpoint of MACCE (Pinteraction = 0.053). However, there were no significant interactions between diabetes status and treatment for all-cause mortality, cardiac mortality and stroke (Table 5).
Propensity score-matching analysis
After propensity score-matching, 127 matched pairs for diabetic patients with STEMI and multivessel disease and 280 matched pairs for nondiabetic patients with STEMI and multivessel disease were generated. All the matched variables were well balanced for both diabetic and nondiabetic cohorts, with postmatching absolute standardized differences < 10% (Additional file 1: Figure S1). No significant differences for main baseline patient, angiographic and procedural characteristics were present between the staged PCI and culprit-only PCI groups in both diabetic and nondiabetic cohorts (Additional file 1: Table S1). Diabetic patients undergoing staged PCI were less likely to receive defibrillator compared with those in culprit-only group (P = 0.010). In nondiabetic population, compared with those in culprit-only group, patients in the staged PCI group were less likely to receive temporary pacemaker (P = 0.020) and associated with higher risk of acute kidney injury after PCI (P = 0.049).
Among nondiabetic patients, patients undergoing staged PCI were associated with lower risks of MACCE (HR 0.583, 95% CI 0.432 to 0.787), MI (HR 0.275, 95% CI 0.134 to 0.563), unplanned revascularization (HR 0.546, 95% CI 0.380 to 0.783), and the composite of cardiac death, MI or stroke (HR 0.498, 95% CI 0.311 to 0.798) compared with those undergoing culprit-only PCI (Additional file 1: Table S2 and Figure S2A). In diabetic patients, the risks of the primary endpoint of MACCE (HR 1.271, 95% CI 0.820 to 1.971) and all the secondary outcomes were comparable between the two strategies (Additional file 1: Table S2 and Figure S2B). Furthermore, there were significant interactions between diabetes status and revascularization assignment for MACCE (Pinteraction = 0.004), MI (Pinteraction = 0.004), unplanned revascularization (Pinteraction = 0.005), and the composite of cardiac death, MI or stroke (Pinteraction = 0.007).
Sensitivity analysis
Sensitivity analysis comparing patients undergoing staged complete revascularization within 10 days after primary PCI versus those undergoing culprit-only PCI was concordant with the overall analysis in both diabetic and nondiabetic population. However, diabetic patients undergoing staged PCI was associated with higher risk of MI than those undergoing culprit-only PCI (Adjusted HR 2.617, 95% CI 1.057 to 6.481) (Additional file 1: Tables S3, S4 and Figure S3).
Discussion
During the 10-year study, diabetes was present in 30.8% of the patients with STEMI and multivessel disease who underwent primary PCI in our center. Multivariate analysis showed that diabetes mellitus was not independently associated with the primary endpoint of MACCE or the secondary outcomes at 5 years. Compared with culprit-only PCI, staged complete revascularization was associated with lower risks of MACCE, MI, unplanned revascularization and the composite of cardiac death, MI or stroke in nondiabetic patients. However, no significant difference was found between the two revascularization strategies in terms of all the outcomes in diabetic patients. Besides, significant interactions between diabetes status and treatment for MI, unplanned revascularization and the composite of cardiac death, MI or stroke at 5 years were found. Furthermore, these findings were demonstrated by propensity score-matching analysis.
Patients with STEMI and multivessel disease were associated with worse outcomes than those with single-vessel disease [1, 2]. However, the management of nonculprit lesions has been fiercely debated for two decades until the recent publication of the landmark RCTs [9,10,11,12]. The Preventative Angioplasty in Myocardial Infarction trial showed that preventive PCI of nonculprit lesions significantly reduced the risk of a composite endpoint of cardiac death, MI, and refractory angina at 23 months [9]. The Complete Versus culprit-Lesion only PRimary PCI trial indicated that patients who received in-hospital complete revascularization had lower composite risk of all-cause death, recurrent MI, heart failure, and ischemia-driven revascularization at 1 year [10]. In addition, the Third DANish Study of Optimal Acute Treatment of Patients with STEMI-PRImary PCI in MULTIvessel Disease and the Compare-Acute trials indicated significant benefit of immediate or complete revascularization regarding adverse cardiac events compared with culprit-only PCI [11, 12]. Furthermore, the studies conducted by Cui et al. and Toyota et al. with 5-year information confirmed and extended the results of previous studies with short- or medium-term follow-up period [24, 30].
Diabetes mellitus is both an important risk factor for the development of CAD [20, 31] and a major determinant of poor clinical outcomes in patients with CAD [14,15,16,17,18]. Patients with diabetes mellitus often have a high incidence of complex disease with smaller vessel size, longer lesion length, and higher plaque burden [32]. The Improving Care for Cardiovascular Disease in China-Acute Coronary Syndrome Project which included 63,450 patients from 150 tertiary hospitals revealed that the prevalence of diabetes/possible diabetes was 36.8% in STEMI patients, which was a little higher than the finding of our study. In addition, diabetic/possible diabetic patients had 2.4-fold increased risk of in-hospital mortality and a twofold increased risk of a combination of cardiac death, recurrent MI, stent thrombosis or stroke compared with nondiabetic patients [14]. Jung et al. [15] reported that people with diabetes had a two- to sixfold higher risk of major adverse cardiac events than people without diabetes in South Korea. A report from Spain showed that patients with MI and diabetes had a significantly 15% higher in-hospital mortality than nondiabetic patients [16]. A systematic review and meta-analysis with a total of 1,225,174 patients revealed an increased risk of early mortality (odds ratio 1.66, 95% CI 1.59 to 1.74) and 6–12-month mortality (odds ratio 1.86, 95% CI 1.75 to 1.97) in diabetic patients with acute coronary syndrome [17]. Besides, Klempfner et al. [18] enrolled 11, 472 patients with acute coronary syndrome found that diabetes was independently associated with a significantly increased mortality risk (39%) at 1 year compared with nondiabetic patients. Moreover, the incidence of ischemic events was consistently higher in diabetic patients after PCI or coronary artery bypass graft surgery [21, 22]. The latest guideline has classified STEMI patients with diabetes as a special population and presented specific sections for the management of these patients in consideration of their extremely high risk [13]. Therefore, diabetes status might be a major factor in the choice of revascularization strategy in patients with STEMI and multivessel disease.
Unfortunately, it remains undetermined whether diabetes has an effect on the outcomes of these patients who received staged complete revascularization or culprit-only PCI. Only a small number of patients with diabetes were included in previous RCTs and this high-risk group of patients were underrepresented [9,10,11,12]. Hamza et al. enrolled 100 diabetic patients with STMEI and multivessel disease to randomly receive staged complete revascularization (n = 50) or culprit-only PCI (n = 50). After 6-month follow-up, they found that staged complete revascularization was significantly associated with a reduction in major adverse cardiac events (6% vs. 24%, P = 0.01), primarily due to reduction in ischemia-driven revascularization in the complete PCI group (2% vs. 12%; P = 0.047). However, their sample size was relatively small and the follow-up period was relatively short [23]. Therefore, it is necessary to determine whether the effect of diabetes on clinical outcomes differs according to different revascularization strategies.
In this study, STEMI patients with and without diabetes mellitus showed similar risks of ischemic events. Furthermore, diabetes was not a predictor of the primary endpoint of MACCE or the secondary outcomes at 5 years in multivariate analysis, while the strategy of culprit-only PCI was an independent predictor of the less favorable outcomes in these patients. Patients with STEMI and multivessel disease was a higher-risk population in STEMI patients, thus the impact of revascularization strategy on prognosis is more important than the impact of diabetes status on prognosis in our study. Although with increased risk of perioperative events, early revascularization of nonculprit lesions can reduce ischemic burden, stabilize vulnerable plaque, and reduce the long-term incidence of ischemic events [33]. Nonetheless, the comparable results between the diabetic and nondiabetic groups here could be partially explained, since data on the length of illness and details of antidiabetic therapy was not available in our study, which might have an effect on prognosis in diabetic patients. Actually, inappropriate antidiabetic therapy can significantly increase the risk of mortality [34].
The most important finding of the present study might be that the interactions between diabetes status and revascularization assignment tended to be significant for the outcomes of MACCE, MI, unplanned revascularization, and the composite of cardiac death, MI or stroke at 5 years, which were confirmed by propensity score-matching analysis. In nondiabetic patients, the 5-year risks of MACCE, MI, unplanned revascularization, and the composite of cardiac death, MI or stroke were significantly lower in staged PCI group than those in culprit-only PCI group, whereas the incidences of all the outcomes were similar between the two revascularization strategies in diabetic patients. In other words, the strategy of staged complete revascularization lost its advantage in patients with diabetes and multivessel disease, which was contrary to the results of study conducted by Hamza et al. In clinical scenarios, the diffuse and rapidly progressive forms of CAD in diabetic patients may lead to more stent implantation characterized by longer length and smaller diameter, which is associated with worse outcomes. Although the new-generation drug-eluting stent has been widely used in clinical practice, the morbidity and mortality are still high in diabetic patients undergoing PCI and diabetes mellitus remains a risk factor for restenosis and stent thrombosis [32, 35]. Considering the staged PCI of nonculprit vessels brings no additional benefits to diabetic patients with multivessel disease as compared with culprit-only PCI, it becomes even more important to choose an optimal hypoglycemic regimen in this population. Recently, several studies have found that the new antidiabetic drugs, i.e., sodium-glucose cotransporter 2 inhibitors and glucagon-like peptide 1 agonists can lower blood glucose levels and mortality risks [36,37,38,39]. Henceforward, these new types of drugs should be given a full consideration in the treatment of diabetic patients with STEMI and multivessel disease.
Limitations
There are several limitations of our study. First, as a single-center, nonrandomized study, our research is limited by unbalanced baseline characteristics and selection bias. Although we performed rigorous multivariable-adjusted analysis and propensity score-matching analysis, there might still be some unmeasured confounders. Second, our results were mainly derived from subgroup analysis of a cohort study, thus we might have inadequate statistical power to detect differences in clinical events in diabetic patients and the results should be interpreted as hypothesis generating. Moreover, the number of subjects with diabetes was modest (371), and possibly not all confounders were identified. Therefore, further larger-scale investigation in dedicated trials of diabetic patients is warranted. Third, the data on length of illness and details of antidiabetic therapy were not collected in the study. Finally, the significance of nonculprit lesions was routinely assessed on angiography other than ischemia testing, for example, fractional flow reserve or noninvasive physiological stress test for most patients.
Conclusions
In patients with STEMI and multivessel disease, diabetes mellitus is not an independent predictor of adverse cardiovascular events at 5 years. In nondiabetic patients, an approach of staged complete revascularization is superior to culprit-only PCI, whereas the advantage of staged PCI is attenuated in diabetic patients. Further studies are needed to evaluate the prognostic impact of diabetes on outcomes in patients with STEMI and multivessel disease requiring revascularization procedures.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- PCI:
-
percutaneous coronary intervention
- STEMI:
-
ST-segment elevation myocardial infarction
- RCT:
-
randomized controlled trial
- CAD:
-
coronary artery disease
- MACCE:
-
major adverse cardiac and cerebrovascular event
- MI:
-
myocardial infarction
- HR:
-
hazard ratio
- CI:
-
confidence interval
References
Sorajja P, Gersh BJ, Cox DA, McLaughlin MG, Zimetbaum P, Costantini C, Stuckey T, Tcheng JE, Mehran R, Lansky AJ, et al. Impact of multivessel disease on reperfusion success and clinical outcomes in patients undergoing primary percutaneous coronary intervention for acute myocardial infarction. Eur Heart J. 2007;28(14):1709–16.
Park DW, Clare RM, Schulte PJ, Pieper KS, Shaw LK, Califf RM, Ohman EM, Van de Werf F, Hirji S, Harrington RA, et al. Extent, location, and clinical significance of non-infarct-related coronary artery disease among patients with ST-elevation myocardial infarction. JAMA. 2014;312(19):2019–27.
Dambrink JH, Debrauwere JP, van ‘t Hof AW, Ottervanger JP, Gosselink AT, Hoorntje JC, de Boer MJ, Suryapranata H. Non-culprit lesions detected during primary PCI: treat invasively or follow the guidelines? EuroIntervention. 2010;5(8):968–75.
Ghani A, Dambrink JH, van ‘t Hof AW, Ottervanger JP, Gosselink AT, Hoorntje JC. Treatment of non-culprit lesions detected during primary PCI: long-term follow-up of a randomised clinical trial. Neth Heart J. 2012;20(9):347–53.
Cavender MA, Milford-Beland S, Roe MT, Peterson ED, Weintraub WS, Rao SV. Prevalence, predictors, and in-hospital outcomes of non-infarct artery intervention during primary percutaneous coronary intervention for ST-segment elevation myocardial infarction (from the National Cardiovascular Data Registry). Am J Cardiol. 2009;104(4):507–13.
Dziewierz A, Siudak Z, Rakowski T, Zasada W, Dubiel JS, Dudek D. Impact of multivessel coronary artery disease and noninfarct-related artery revascularization on outcome of patients with ST-elevation myocardial infarction transferred for primary percutaneous coronary intervention (from the EUROTRANSFER Registry). Am J Cardiol. 2010;106(3):342–7.
Hannan EL, Samadashvili Z, Walford G, Holmes DR Jr, Jacobs AK, Stamato NJ, Venditti FJ, Sharma S, King SB 3rd. Culprit vessel percutaneous coronary intervention versus multivessel and staged percutaneous coronary intervention for ST-segment elevation myocardial infarction patients with multivessel disease. JACC Cardiovasc Interv. 2010;3(1):22–31.
Kornowski R, Mehran R, Dangas G, Nikolsky E, Assali A, Claessen BE, Gersh BJ, Wong SC, Witzenbichler B, Guagliumi G, et al. Prognostic impact of staged versus “one-time” multivessel percutaneous intervention in acute myocardial infarction: analysis from the HORIZONS-AMI (harmonizing outcomes with revascularization and stents in acute myocardial infarction) trial. J Am Coll Cardiol. 2011;58(7):704–11.
Wald DS, Morris JK, Wald NJ, Chase AJ, Edwards RJ, Hughes LO, Berry C, Oldroyd KG, Investigators P. Randomized trial of preventive angioplasty in myocardial infarction. N Engl J Med. 2013;369(12):1115–23.
Gershlick AH, Khan JN, Kelly DJ, Greenwood JP, Sasikaran T, Curzen N, Blackman DJ, Dalby M, Fairbrother KL, Banya W, et al. Randomized trial of complete versus lesion-only revascularization in patients undergoing primary percutaneous coronary intervention for STEMI and multivessel disease: the CvLPRIT trial. J Am Coll Cardiol. 2015;65(10):963–72.
Engstrom T, Kelbaek H, Helqvist S, Hofsten DE, Klovgaard L, Holmvang L, Jorgensen E, Pedersen F, Saunamaki K, Clemmensen P, et al. Complete revascularisation versus treatment of the culprit lesion only in patients with ST-segment elevation myocardial infarction and multivessel disease (DANAMI-3-PRIMULTI): an open-label, randomised controlled trial. Lancet. 2015;386(9994):665–71.
Smits PC, Abdel-Wahab M, Neumann FJ, Boxma-de Klerk BM, Lunde K, Schotborgh CE, Piroth Z, Horak D, Wlodarczak A, Ong PJ, et al. Fractional flow reserve-guided multivessel angioplasty in myocardial infarction. N Engl J Med. 2017;376(13):1234–44.
Ibanez B, James S, Agewall S, Antunes MJ, Bucciarelli-Ducci C, Bueno H, Caforio ALP, Crea F, Goudevenos JA, Halvorsen S, et al. 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation: the Task Force for the management of acute myocardial infarction in patients presenting with ST-segment elevation of the European Society of Cardiology (ESC). Eur Heart J. 2018;39(2):119–77.
Zhou M, Liu J, Hao Y, Liu J, Huo Y, Smith SC Jr, Ge J, Ma C, Han Y, Fonarow GC, et al. Prevalence and in-hospital outcomes of diabetes among patients with acute coronary syndrome in China: findings from the Improving Care for Cardiovascular Disease in China-Acute Coronary Syndrome Project. Cardiovasc Diabetol. 2018;17(1):147.
Jung CH, Chung JO, Han K, Ko SH, Ko KS, Park JY, Taskforce Team of Diabetes Fact Sheet of the Korean Diabetes. Improved trends in cardiovascular complications among subjects with type 2 diabetes in Korea: a nationwide study (2006–2013). Cardiovasc Diabetol. 2017;16(1):1.
de Miguel-Yanes JM, Jimenez-Garcia R, Hernandez-Barrera V, Mendez-Bailon M, de Miguel-Diez J, Lopez-de-Andres A. Impact of type 2 diabetes mellitus on in-hospital-mortality after major cardiovascular events in Spain (2002–2014). Cardiovasc Diabetol. 2017;16(1):126.
Bauters C, Lemesle G, de Groote P, Lamblin N. A systematic review and meta-regression of temporal trends in the excess mortality associated with diabetes mellitus after myocardial infarction. Int J Cardiol. 2016;217:109–21.
Klempfner R, Elis A, Matezky S, Keren G, Roth A, Finkelstein A, Banai S, Goldenberg I, Fisman EZ, Tenenbaum A, et al. Temporal trends in management and outcome of diabetic and non-diabetic patients with acute coronary syndrome (ACS): residual risk of long-term mortality persists: insights from the ACS Israeli Survey (ACSIS) 2000–2010. Int J Cardiol. 2015;179:546–51.
Cho NH, Shaw JE, Karuranga S, Huang Y, da Rocha Fernandes JD, Ohlrogge AW, Malanda B. IDF Diabetes Atlas: Global estimates of diabetes prevalence for 2017 and projections for 2045. Diabetes Res Clin Pract. 2018;138:271–81.
Einarson TR, Acs A, Ludwig C, Panton UH. Prevalence of cardiovascular disease in type 2 diabetes: a systematic literature review of scientific evidence from across the world in 2007–2017. Cardiovasc Diabetol. 2018;17(1):83.
Elezi S, Kastrati A, Pache J, Wehinger A, Hadamitzky M, Dirschinger J, Neumann FJ, Schomig A. Diabetes mellitus and the clinical and angiographic outcome after coronary stent placement. J Am Coll Cardiol. 1998;32(7):1866–73.
Kogan A, Ram E, Levin S, Fisman EZ, Tenenbaum A, Raanani E, Sternik L. Impact of type 2 diabetes mellitus on short- and long-term mortality after coronary artery bypass surgery. Cardiovasc Diabetol. 2018;17(1):151.
Hamza M, Mahmoud N, Elgendy IY. A randomized trial of complete versus culprit-only revascularization during primary percutaneous coronary intervention in diabetic patients with acute ST elevation myocardial infarction and multi vessel disease. J Interv Cardiol. 2016;29(3):241–7.
Cui K, Lyu S, Song X, Liu H, Yuan F, Xu F, Zhang M, Wang W, Zhang M, Zhang D, et al. Long-term safety and efficacy of staged percutaneous coronary intervention for patients with ST-segment elevation myocardial infarction and multivessel coronary disease. Am J Cardiol. 2019;124(3):334–42.
Levine GN, Bates ER, Blankenship JC, Bailey SR, Bittl JA, Cercek B, Chambers CE, Ellis SG, Guyton RA, Hollenberg SM, et al. 2015 ACC/AHA/SCAI focused update on primary percutaneous coronary intervention for patients with ST-elevation myocardial infarction: an update of the 2011 ACCF/AHA/SCAI guideline for percutaneous coronary intervention and the 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction. J Am Coll Cardiol. 2016;67(10):1235–50.
Murphy SW, Barrett BJ, Parfrey PS. Contrast nephropathy. J Am Soc Nephrol. 2000;11(1):177–82.
Mehran R, Nikolsky E. Contrast-induced nephropathy: definition, epidemiology, and patients at risk. Kidney Int Suppl. 2006;100:S11–5.
Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, White HD, Group ESCSD. Fourth universal definition of myocardial infarction (2018). Eur Heart J. 2019;40(3):237–69.
Barber M, Stott DJ, Langhorne P. An internationally agreed definition of progressing stroke. Cerebrovasc Dis. 2004;18(3):255–6 (author reply 256–7).
Toyota T, Shiomi H, Taniguchi T, Morimoto T, Furukawa Y, Nakagawa Y, Horie M, Kimura T, Investigators CR-KAR. Culprit vessel-only vs. staged multivessel percutaneous coronary intervention strategies in patients with multivessel coronary artery disease undergoing primary percutaneous coronary intervention for ST-segment elevation myocardial infarction. Circ J. 2016;80(2):371–8.
Kengne AP, Turnbull F, MacMahon S. The Framingham Study, diabetes mellitus and cardiovascular disease: turning back the clock. Prog Cardiovasc Dis. 2010;53(1):45–51.
West NE, Ruygrok PN, Disco CM, Webster MW, Lindeboom WK, O’Neill WW, Mercado NF, Serruys PW. Clinical and angiographic predictors of restenosis after stent deployment in diabetic patients. Circulation. 2004;109(7):867–73.
Lu DY, Zhong M, Feldman DN. Complete versus culprit-only revascularization in STEMI: a contemporary review. Curr Treat Options Cardiovasc Med. 2018;20(5):41.
Deedwania P, Kosiborod M, Barrett E, Ceriello A, Isley W, Mazzone T, Raskin P, American Heart Association Diabetes Committee of the Council on Nutrition PA, Metabolism. Hyperglycemia and acute coronary syndrome: a scientific statement from the American Heart Association Diabetes Committee of the Council on Nutrition, Physical Activity, and Metabolism. Circulation. 2008;117(12):1610–9.
Alfonso F, Rivero F. Coronary revascularization in diabetic patients with chronic kidney disease. Eur Heart J. 2016;37(46):3448–51.
Zheng SL, Roddick AJ, Aghar-Jaffar R, Shun-Shin MJ, Francis D, Oliver N, Meeran K. Association between use of sodium-glucose cotransporter 2 inhibitors, glucagon-like peptide 1 agonists, and dipeptidyl peptidase 4 inhibitors with all-cause mortality in patients with type 2 diabetes: a systematic review and meta-analysis. JAMA. 2018;319(15):1580–91.
Zhuang XD, He X, Yang DY, Guo Y, He JG, Xiao HP, Liao XX. Comparative cardiovascular outcomes in the era of novel anti-diabetic agents: a comprehensive network meta-analysis of 166,371 participants from 170 randomized controlled trials. Cardiovasc Diabetol. 2018;17(1):79.
Zelniker TA, Wiviott SD, Raz I, Im K, Goodrich EL, Furtado RHM, Bonaca MP, Mosenzon O, Kato ET, Cahn A, et al. Comparison of the effects of glucagon-like peptide receptor agonists and sodium-glucose cotransporter 2 inhibitors for prevention of major adverse cardiovascular and renal outcomes in type 2 diabetes mellitus. Circulation. 2019;139(17):2022–31.
Tanaka A, Node K. Clinical application of glucagon-like peptide-1 receptor agonists in cardiovascular disease: lessons from recent clinical cardiovascular outcomes trials. Cardiovasc Diabetol. 2018;17(1):85.
Acknowledgements
Not applicable.
Funding
The study was funded by the Ministry of Science and Technology of the People’s Republic of China, State Science and Technology Support Program (No. 2011BAI11B05) and Beijing Lab for Cardiovascular Precision Medicine, Beijing, China (PXM2019_014226_000023).
Author information
Authors and Affiliations
Contributions
The original idea came from KYC, XTS, HL and SZL. KYC, FY, FX, MZ, WW, MDZ, DFZ and JFT performed the acquisition, analysis, and interpretation of the data. XTS, HL and SZL made contribution to endpoints adjudication. KYC, JFT and SZL wrote the manuscript. All authors critically revised the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics of approval and consent to participate
The present study was approved by the Clinical Research Ethics Committee of Beijing Anzhen Hospital, Capital Medical University (No.: 2012001). Informed consent was exempt by the committee.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1. Table S1.
Baseline patient, angiographic and procedural characteristics according to diabetes status and revascularization assignment in propensity-matched population. Table S2. Five-year outcomes according to diabetes status and revascularization assignment in propensity-matched population. Table S3. Baseline patient, angiographic and procedural characteristics according to diabetes status and revascularization assignment in sensitivity analysis. Table S4. Five-year outcomes according to diabetes status and revascularization assignment in sensitivity analysis. Figure S1. Absolute standard difference before and after propensity score-matching in (A) nondiabetic population and (B) diabetic population. Figure S2. Kaplan–Meier curves of clinical outcomes for (A) nondiabetic patients and (B) diabetic patients in propensity-matched population. Figure S3. Kaplan–Meier curves of clinical outcomes for (A) nondiabetic patients and (B) diabetic patients in sensitivity analysis.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Cui, K., Lyu, S., Liu, H. et al. Staged complete revascularization or culprit-only percutaneous coronary intervention for multivessel coronary artery disease in patients with ST-segment elevation myocardial infarction and diabetes. Cardiovasc Diabetol 18, 119 (2019). https://doi.org/10.1186/s12933-019-0923-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12933-019-0923-0