Abstract
Background
Every year in Italy, influenza affects about 4 million people. Almost 5% of them are hospitalised. During peak illness, enormous pressure is placed on healthcare and economic systems. This study aims to quantify the clinical and economic burden of severe influenza during 5 epidemic seasons (2014–2019) from administrative claims data.
Methods
Patients hospitalized with a diagnosis of influenza between October 2014, and April 2019, were analyzed. Clinical characteristics and administrative information were retrieved from health-related Administrative Databases (ADs) of 4 Italian Local Health Units (LHUs). The date of first admission was set as the Index Date (ID). A follow-up period of six months after ID was considered to account for complications and re-hospitalizations, while a lookback period (2 years before ID) was set to assess the prevalence of underlying comorbidities.
Results
Out of 2,333 patients with severe influenza, 44.1% were adults ≥ 65, and 25.6% young individuals aged 0–17. 46.8% had comorbidities (i.e., were at risk), mainly cardiovascular and metabolic diseases (45.3%), and chronic conditions (24.7%). The highest hospitalization rates were among the elderly (≥ 75) and the young individuals (0–17), and were 37.6 and 19.5/100,000 inhabitants/year, respectively. The average hospital stay was 8 days (IQR: 14 − 4). It was higher for older individuals (≥ 65 years, 11 days, [17 − 6]) and for those with comorbidities (9 days, [16 − 6]), p-value < 0.001. Similarly, mortality was higher in elderly and those at risk (p-value < 0.001). Respiratory complications occurred in 12.7% of patients, and cardiovascular disorders in 5.9%. Total influenza-related costs were €9.7 million with hospitalization accounting for 95% of them. 47.3% of hospitalization costs were associated with individuals ≥ 65 and 52.9% with patients at risk. The average hospitalisation cost per patient was € 4,007.
Conclusions
This retrospective study showed that during the 2014–2019 influenza seasons in Italy, individuals of extreme ages and those with pre-existing medical conditions, were more likely to be hospitalized with severe influenza. Together with complications and ageing, they worsen patient’s outcome and may lead to a prolonged hospitalization, thus increasing healthcare utilization and costs. Our data generate real-world evidence on the burden of influenza, useful to inform public health decision-making.
Similar content being viewed by others
Background
Influenza is an acute viral respiratory infectious disease which occurs worldwide with a mostly seasonal frequency [1]. Incidence, onset of the epidemic season, and relative duration are characterized by high variability in Italy. Overall, influenza affects on average 9% of the Italian population each year, with a minimum of 4%, observed in the 2005-06 season, and a maximum of 15% recorded in the 2017-18 [2]. Epidemiological differences can also be observed according to the age of individuals, and virus strain. Influenza types/subtypes A (H1N1) and A (H3N2) are more frequent among young children and the elderly respectively, while the subtype B spreads mostly among older children [3,4,5]. Influenza epidemics can cause overcrowding of clinics and hospitals during peak illness periods, high levels of worker/school absenteeism and productivity losses. Although most people recover from symptoms within a week without requiring medical attention, influenza may degenerate into severe conditions, hospitalizations, or death especially in people with pre-existing comorbidities and in vulnerable individuals like the younger and the older. Complications may also arise and lead to a bad prognosis. Among others, respiratory complications, viral or bacterial superinfections (pneumonia), or the worsening of underlying chronic conditions are the most common illnesses (5–6). About 290,000 to 650,000 deaths from respiratory causes alone are attributable to influenza each year [7]. Extra-respiratory complications such as cardiovascular and nervous system complications [8, 9] also play a relevant role. Epidemiological studies [10, 11] have demonstrated an association between influenza epidemics and cardiovascular mortality which is decreased in adults undergoing influenza vaccination, the most effective medical intervention to prevent infection. Quantifying the clinical and economic burden associated to patients hospitalized with influenza in terms of healthcare resource utilization and direct medical costs is therefore important for decision makers to optimize influenza prevention policies. This real-world evidence study aims to assess healthcare resource consumption and direct medical costs using administrative data (AD) from four Local Health Units (LHUs) in Italy.
Methods
Data source
The study was conducted using anonymized claims data from AD of four LHUs (Agenzia di Tutela della Salute (ATS) Brescia, Agenzia di Tutela della Salute (ATS) Bergamo, Azienda Unità Locale Socio-Sanitaria (ULSS) 8 Berica, and Azienda Sanitaria Locale (ASL) Foggia) recording data about hospitalizations and covering reimbursement information for each public or private hospital. LHUs were selected based on the following criteria: (i) data quality; (ii) ethics committee sessions regularly held; (iii) geographical distribution across the country (i.e., each LHU was picked to represent different areas); (iv) large catchment area. Overall, they included approximately 3,300,000 health-assisted individuals. Each database holds the following data:
-
patient demographic data including the year of birth, the gender, and the exemption code (if any).
-
hospitalizations recorded through the Hospital Discharge Records (SDO) which include admission/discharge dates, type of hospitalization (ordinary or day hospital), main and secondary diagnosis coded according to the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM), Diagnosis-Related Group (DRG) reimbursement rate, information on transfer between wards and destination after hospitalization, the exemption code (if any) and the costs.
-
outpatient care which includes specialist visits, medical procedures and exams with dates, exemption code (if any) and costs.
-
Emergency Room (ER) accesses with their relative date, main and secondary diagnoses (coded with ICD-9), treatment received including the pharmacological one, type of exams completed and costs.
-
prescribed drugs from hospitals and pharmacies in the area with the date of prescription, the prescribing physician’s number, and the Anatomical-Therapeutic-Chemical (ATC) code of the prescribed drug, the exemption code (if any) and the costs.
Information extracted by each LHU was organized in five databases (DB): (1) Beneficiaries’ DB containing demographic data; (2) Hospitalization DB including information on hospitalizations; (3) Diagnostic tests Laboratory DB, containing data on laboratory tests, and specialist visits DB with information on outpatient specialist services; (4) ER DB containing information on patients’ access to ER, and (5) Pharmaceuticals DB containing information on medication prescriptions.
Patient’s information was anonymized in full compliance with the Italian code of protection of personal data (Legislative Decree, 101/18 and 196/03). An anonymous and univocal numerical patient identifier was assigned to each participant to guarantee patients’ privacy. All the results of the analysis were produced as aggregated summaries to avoid any direct or indirect link to individual patients.
Cohort definition
This was a retrospective, non-interventional descriptive study to examine the clinical and economic burden of patients with severe seasonal influenza who required hospital admission. The study period spanned from 1 October 2014 to 1 April 2019 for a total of 5 years and 5 epidemic seasons (Fig. 1). The end of the study was set to 2019 to prevent from the bias due to COVID-pandemic that caused a substantial reduction of influenza transmission. Diagnosis explicitly associated with an influenza virus like influenza with pneumonia, with other (respiratory) manifestations and due to identified influenza viruses were considered and extracted from hospital admissions, and ER access looking at both primary and secondary diagnosis. The following ICD-9 codes were used, based on the literature [12, 13]: 487.0, 487.1, 487.8 and 488. Patients who relocated outside the LHU during the observation period, i.e., in the 6 months of follow-up were excluded. The date corresponding to the first hospitalization with a diagnosis of influenza during the observation period was defined as “Index Date” (ID). Each patient was followed for 6 months after ID according to previous similar research [14] and back for 2 years in the look-back period to evaluate the presence of comorbidities (Fig. 1). Overall, the observation period spanned from 1 October 2012 to 1 October 2019.
The schematic study design. The study design is shown above. The study period spanned from the 1st October 2014 to 1st April 2019: during this period, any patient hospitalized with a diagnosis of influenza was identified. The study Index Date (ID) corresponded to the first hospitalization due to influenza. From the ID, a 6-months follow-up period was considered for each patient, to account for mortality, re-hospitalization, healthcare resource consumption, direct healthcare costs, and influenza related complications (e.g.: for patients enrolled on 1st April 2019 the follow-up period ended on 1st October 2019). A look-back period of 24 months was considered for each patient to account for comorbidities
Information extracted from the databases
To provide demographic characteristics of the study population, information regarding age and sex was extracted for each patient at the time of initial diagnosis. Clinical characteristics consisting in the presence of comorbidities, were identified looking at all ICD-9 or exemption codes for chronic diseases, recorded during the 24-month period before ID. The ones that, based on the literature [15,16,17,18] worsen the clinical outcome and hence defined the risk groups were: diabetes, immune deficiency syndromes, chronic rheumatic heart disease, ischemic heart disease, disease of pulmonary circulation, other forms of heart disease, chronic kidney disease, chronic liver disease, neoplasms, chronic respiratory disease, pregnancy, preterm birth, haemoglobinopathy, metabolic disorders, cystic fibrosis, neuromuscular disorders, neurologic disorders and genetic syndromes. Comorbidities were extracted from SDO and ER access. Morbidities which identify complications observed in patients hospitalized with severe influenza were also considered and searched in the 6 months follow-up period. They were selected based on the available literature [15, 18,19,20,21,22,23,24,25] and were: respiratory complications, cardiovascular, neurological, and diabetic complications, and co- and secondary infections. Exemption codes were not used to identify complications from influenza. Patients were categorized based on the number of comorbidities of interest. A patient without any comorbidity was classified as “not at risk”.
Study outcomes
The main outcomes considered in the analysis were: monthly number of hospitalizations, healthcare resource utilization (HRU) and direct healthcare costs. The last two outcomes referred to pharmacological treatments (number of prescribed drug-packs and days of treatment), outpatient visits (number), diagnostic procedures and laboratory tests (number), ER accesses (number of admissions, treatments, and exams), day hospital (number) and inpatient episodes (number and length of stay). Number of hospitalizations, resource consumption and costs were stratified by age categories (0–17, 18–49, 50–59, 60–64, 65–74, ≥ 75) and risk groups. Total healthcare direct costs were estimated considering the costs associated to all mentioned items. Additionally, all cause-in-hospital mortality following influenza hospitalization, the occurrence of complications, the hospitalization rates based on the total population in the LHU catchment area and the number of all cause re-hospitalizations of influenza cases, all stratified by sex, age category, and risk group, were estimated, and evaluated.
Cost analysis
Drug costs were evaluated using the Italian National Health Service (INHS) purchase price. Hospitalization costs were provided by the LHUs and reported in the SDO. The mean annual health care costs per patient were evaluated based on total resource consumption (considering drugs, hospitalizations, outpatient visits and inpatients episodes, ER access, day hospital, tests and laboratory exams) during the follow-up period. Costs reported in the SDO represent the reimbursement levels of the NHS to health care providers. The outpatient service costs were defined according to the tariffs applied by the evaluated regions.
Statistical analysis
All analysis were performed with SAS® software 9.4 or later and were descriptive. Categorical variables were expressed as numbers (N) and percentages (%), whereas quantitative variables through mean ± SD. The 95% confidence intervals (CIs) for proportions and means were calculated using the Wald confidence interval formula. The non-parametric Mann-Whitney U-Test was used to compare outcomes between two independent groups. The non-parametric Kruskal-Wallis test was used to compare two or more groups for continuous or discrete variables.
Data management and quality control
Data used for the study were collected in the LHU data warehouse. These data are sent every month by the LHUs to the Region of reference, with a delay specific for each data flow. These administrative data are collected for reimbursement purposes and their completeness is implicitly guaranteed by the LHU. After study approval by the LHU and Ethics Committee, LHU staff was requested to extract the data. A process of quality control of data was performed by the LHUs through which the internal consistency of data was verified to ensure the completeness and reliability of them. Given the nature of real-world data, and due to variabilities in efficiency and completeness of records, missing data are likely to be present. No attempt to input missing data was made.
Results
Demographic and clinical characteristics of patients hospitalized with influenza in Italy
Table 1 shows demographic and clinical characteristics of patients hospitalized with a diagnosis of influenza in the Italian LHUs over the whole study period (1 October 2014–1 April 2019). A total of 2,333 patients met the study inclusion criteria. Of these, 1,190 (51%) were males and 1,143 (49%) were females. On average, individuals were aged 50 years (95% CI, 48.7–51.3)Approximately 80% of influenza-related hospitalizations occurred in individuals at extreme age categories (p-value < 0.05), i.e., young adults aged 0–17 (N = 596; 25.6%, 95% CI, 23.8–27.3),of these 68.3% (N = 407) were infants and children aged 0–4, and in adults aged ≥ 65 (N = 1,029; 44.1%, 95% CI, 42.1–46.1). More than half of the enrolled patients (N = 1,240; 53.2%, 95% CI, 51.1–55.1) had no comorbidities. A diagnosis of one comorbidity was observed in 558 patients (23.9%), whilst two comorbidities were recorded in 535 patients (22.9%). The group of patients not at risk was mainly composed of young patients aged 0–17 while the group of patients at risk was composed by elderly individuals. Among the comorbidities, cardiovascular and metabolic diseases were the most prevalent (N = 1,056; 45.3%) followed by chronic medical conditions (N = 577; 24.7%), neoplasms (N = 398; 17.1%) and disorders of pulmonary circulation (N = 234; 10.0%).
Hospital burden of patients with influenza
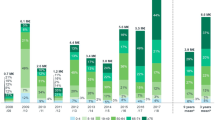
Hospitalizations due to influenza (N), re-hospitalizations of influenza patients due to all-causes (N) and stay duration (mean (SD) and median (Q3-Q1)) are reported in Table 2 and refer to the whole study period or to the influenza season. Data are shown by age category and risk group. The study cohort (N = 2,333) contributed to a total of 2,349 hospitalizations, including re-admissions, recorded during the entire observation period. Over the five seasons 2,202 influenza hospitalizations were recorded. Forty-eight re-hospitalizations of influenza patients due to all causes were observed over the 5-year period. The rate of influenza hospitalizations varied among influenza seasons from 6.7/100.000 (inhabitants) in 2015–2016, to 16.0/100.000 and 17.3/100.000 in 2017–2018 and 2018–2019 respectively (Fig. 2 and Table S1), and reflected the national incidence of influenza infections and intensity [24]. The highest number of influenza hospital admissions and re-admissions during the whole study period, was observed among adults aged ≥ 75 (N = 718), and among individuals in the age category 0–17 (N = 604). The mean hospitalization rate over 5 years, was of 19.5 (95% CI, 18.7–56.4) and 37.6 (95% CI, 9.0–30.0) respectively (Fig. 2 and Table S1). The total number of hospitalizations and re-hospitalizations due to influenza over the whole observation period was comparable between high-risk and not at -risk patients (N = 1,107, and N = 1,242, p-value 0.525). The same was observed for the total hospitalizations due to influenza during each influenza season (Table 2). From ID to the end of the study period (1 April 2019), 48 patients were re-hospitalized due to influenza (Table 2). Almost 38% (N = 18) of them were < 17 years and 33% (N = 16) were ≥ 65. The median (Q3-Q1) inpatient length of stay (LOS) was of 8 days (14 − 4) and increased with age ≥ 65, N = 11 (17 − 6) and the presence of comorbidities, N = 9 (16 − 6). Overall, almost 39.0% (N = 919) of patients (N = 2,333) were managed by the general medicine department, 22.3% (N = 520) by the paediatrics department, 11.5% (N = 268) by the infectious and tropical diseases department. Around 8% (N = 177) required intensive care unit, adult or neonatal (Table S2). Of the 919 patients admitted to the general medicine department, 60.1% (N = 560) were at risk. Similarly, almost half (N = 128; 47.8%) adult patients hospitalized at the infectious and tropical diseases department had at least one comorbidity as well as patients hospitalized at the pneumology ward (N = 66, 60.0%). Only 74 young patients (14.2%) hospitalized at the paediatric department (N = 520) had comorbidities. Overall, most patients went home after discharge (N = 2,122; 91%; Table S3). Around 75% (N = 21) of patients institutionalized post hospital discharge (N = 28) were elderly (≥ 75). More than half of individuals transferred to another hospital or health facility (N = 127) were at risk (N = 73; 57.4%) and ≥ 75 (N = 57; 44.9%).
Healthcare resource consumption
Table 3 shows resource consumption referred to day hospitals and ER access during the follow-up time, outpatient visits, tests, and lab exams from the admission date to one week after discharge. ER accesses before hospitalization were 1,980 corresponding to 84.3%(95% CI, 82.9–85.8) of 2,349 total admissions due to influenza during the entire period. The highest number of ER visits was reported for elderly patients (age ≥ 75; N = 616; 31.1%, 95% CI, 29.1–33.1) and for young individuals (age 0–17; N = 538; 27.2%, (95% CI, 25.2–29.1)). On average, 1.3 (SD = 4.9) tests or lab exams per-patient were recorded from the hospital admission date (ID) to one week after discharge. Patients with at least one comorbidity, perform more diagnostic and laboratory exams (N = 1,787; 57.7%) than individuals without comorbidities (N = 1,309; 42.3%), p < 0.001. Similarly, the number of tests was higher in patients aged ≥ 75 (N = 966; 31.2%) than in patients in the other age categories. Day hospital was infrequent. Only 32 events were recorded overall. They were observed in individuals aged 0–17 (N = 10; 31.3%) and 18–49 (N = 12; 37.5%). A total of 275 outpatient consultations were recorded. Most of them were done by patients in the age category 0–17 (N = 86; 31.3%, 95% CI, 25.8–36.8) and ≥ 75 (N = 74; 26.9%, 95% CI, 21.6–32.1). The number of visits was higher in patients at risk (N = 154; 56.0%) and particularly in those with one pre-existing comorbidity (N = 92; 33.5%) compared to patients not at risk (N = 121, 44.0%), p-value 0.031.
Healthcare costs associated with HRU in patients hospitalized with influenza
Table 4 shows the healthcare resource utilization (HRU), in terms of hospitalizations, day hospitals, outpatient visits, ER access laboratory tests and exams, prescribed drugs, and related direct costs per patient, overall, by age categories and risk groups for the entire study period. Overall, the mean (SD) cost-per-patient was € 4,185 (7,684) and was mainly attributable to hospitalization (€ 4,007, [7,620]). The highest median (Q3-Q1) costs were reported for adult individuals aged 65–74 (€ 3,030, [(4,742-2,250)]) and ≥ 75 (€ 3,230, [4,066 − 2,250]), p-value < 0.001, and were due to hospitalization (€ 2,679, [4,461-2,239] and € 3,096, [3,893-2,239] respectively). Direct overall healthcare costs were higher in patients at risk than in patients not at risk. The median (Q3-Q1) per patients’ cost was € 2,734 (4,098 − 1,866) for individuals with at least one comorbidity whilst it was € 2,257 (3,374-1,290) for patients not at risk and was mainly due to hospitalization. On average, costs were higher for patients with multiple comorbidities compared to patients with one comorbidity (Table 4). Age and risk-related patterns were observed also for outpatient visits. On average, costs were higher in individuals at extreme age categories, i.e., aged 0–17 (€ 4.3 [16.4]) and ≥ 75 (€ 3.5 [28.4]) and in individuals with at least one comorbidity (€4.6 [24.6]) compared to individuals not at risk (€ 2.6 [10.6]), p-value < 0.05. ER accesses, tests and lab exams and treatments have a minor impact on the overall economic burden, compared to hospitalization. Although the distribution of the associated costs was heterogeneous across age-categories and high costs were observed also in intermediate age groups, higher costs were recorded in patients at risk than in patients not at risk.
The clinical burden of influenza-related complications
Figure 3a and b show the rate of influenza related complications during 6-months follow-up stratified by age categories, risk group and sex. The prevalence and type of complication varied depending on the age group and disease type. Cardiovascular complications were mostly observed in adults. Patients aged ≥ 75 years (N = 711) showed the highest percentage of cardiovascular disorders (n = 102, 14.4%, 95% CI, 11.8–17.0), p-value < 0.001. Accordingly, also individuals at risk showed a high prevalence of cardiovascular diseases (≥ 2 comorbidities, n = 90, 16.8%, N = 535, 95% CI, 13.7–20.0). Respiratory complications were common across all age categories. Overall, they required hospital treatment or ER access in 12.7% (n = 296, 95% CI, 11.3–14.0) of the patients in the study cohort (N = 2,333). Their prevalence was high (p-value < 0.001) in patients at risk but even higher in patients with ≥ 2 comorbidities (N = 91, 17%) than in those with one comorbidity (N = 88, 15.8%) or not at risk (N = 117, 9.4%). It was higher in males (n = 182, 15.3%) than in females (N = 114, 10.0%), p-value < 0.001. Although the occurrence of respiratory complications was the lowest for patients aged 18–49 compared to the other age categories, it was the most frequently observed for those patients. Few diabetic complications were recorded (3.1% overall). They were mainly observed in adults aged ≥ 50 and in patients with two comorbidities (n = 47, 8.9%, 95% CI, 6.4–11.2). Neurological and co- and secondary infections were infrequent or even absent.
In-hospital and overall mortality following hospitalization due to influenza
Table 5 shows in-hospital mortality due to all causes following hospitalization due to influenza overall and by epidemic season stratified by age categories and risk groups. The overall mortality during the follow-up is also reported. The age-related mortality was observed for the in-hospital deaths of influenza patients, due to all causes. Overall, mortality was higher in adults ≥ 65 years than in young individuals. The highest numbers of deaths were recorded among patients aged ≥ 75 (N = 34, N = 72, 47.2%) and among patients at risk (N = 46, N = 72, 63.9%) compared to patients not at risk (N = 26, N = 72, 36.1%). A total of 196 (8.4%, 95% CI, 7.3–10.0) patients of the entire cohort (N = 2,333) died during the 6-months follow-up period. Around 56.1% (N = 110, 95% CI, 49.2–63.1) of them, were ≥ 75. Eight patients died in the age group 0–17 (4.1%). Higher mortality in adults ≥ 65 years and in patients at risk was consistent across all epidemic seasons and reflected their relative severity. The seasons 2014–2015 (n = 19), 2016–2017 (n = 20) and 2017–2018 (n = 19) were the ones with the highest number of deaths, of which 78.9% (n = 15), 70.0% (n = 14) and 52.6% (n = 10) respectively occurred among individuals aged ≥ 65 years.
Discussion
The aim of this retrospective observational study was to investigate the clinical and economic burden of patients with severe seasonal influenza in Italy across five epidemiological influenza seasons (2014–2019). Administrative data from 4 LHUs were used to describe hospitalization, mortality, and resource utilization, including direct costs, of a cohort of 2,333 patients hospitalized with flu. The presence of comorbidities at the admission and the occurrence of complications after discharge, were also considered for a more detailed description of the healthcare burden of the disease.
Overall, in this study, the number of females and males hospitalized with severe disease was comparable although with a prevalence of males (51%) compared to females (49%). The mean age of study participants at admission was 50 years.
Of the entire cohort, individuals aged 17 years (25.6%) or less, and adults aged ≥ 65 (56.0%) were the most affected by serious illness, consistently with what observed in other high-income countries [25,26,27,28,29,30]. The two groups represent vulnerable individuals at higher risk than individuals of other age categories, because of immunosenescence or a weaker immune system [31]. A history of at least one comorbidity before the first hospitalization for flu was observed in almost half (46%) of the patients. The most frequently observed were elderly illnesses, like cardiovascular and metabolic diseases, chronic medical conditions like diabetes, disorders of pulmonary circulation and neoplasms. Together with older age, they represent risk factors of severe influenza that require hospitalization, and disease-related complications particularly in older adults [29, 32, 33].
Consistently with age-related fragility and co-existence of additional medical conditions, the mean hospitalization rate over the 5 influenza seasons, was significantly higher in older patients (i.e., ≥ 65 years old) in line with what observed in other countries [34,35,36]. From our data, rates of hospitalization between males and females were comparable. The overall number of admissions was higher for patients with comorbidities than for patients without them.
Variability in influenza-associated hospitalization rates was observed throughout the epidemic seasons and was consistent with national trends of influenza severity and intensity [37]. The 2015–2016 influenza season was recorded as the less severe in Italy, in Europe [38] and US [39], while seasons 2014–2015, 2017–2018 and 2018–2019 were reported as the ones with the highest influenza activity. Consistently, we observed a decrease in the hospitalization rate in the 2015–2016 season and an increase in the remaining seasons, thus reflecting the trend observed in national influenza surveillance data based on cases reported by general practitioners. This, highlights that although the patients included in this study represent a sample of the entire Italian population, our cohort from the 4 LHUs was effective in representing a broader national scenario and providing a robust description of the influenza burden in Italy.
When hospitalized, patients with severe influenza stayed 8 days, on average. This duration was longer for adults aged ≥ 65 years and for patients at risk (11 days). Prolonged hospitalization for severe adult patients and for those with additional chronic conditions (about 9 days) has also been observed in other countries [40] although with a certain degree of variability due to different national healthcare frameworks and cohort heterogeneity [41, 42]. More than 50% of admissions were managed by the general medicine and pediatric departments. Few readmissions occurred in the 6 months following discharge, most of which involved patients in extreme age categories. From our data, re-hospitalization does not represent a significant healthcare burden.
Mortality of influenza patients in our cohort was low. Few patients (N = 72; 3% of 2,333) died of any cause during hospitalization for influenza or within 6 months after discharge. Most of them (47.2%) were elderly (≥ 75) and with chronic diseases (63%). As recently shown [19, 43, 44], patients accumulating comorbidities and of older age, have a higher mortality risk than those without. This highlights an interplay between influenza infection and pre-existing medical conditions and the role of the latter as predictors of worse outcomes.
As discussed by Macias et al. [15]. , complications directly resulting from the viral infection, or the exacerbation of underlying conditions represent a secondary burden of influenza with a considerable impact on healthcare and economic systems. In a Spanish study, approximately 12% of severe ill patients with a confirmed influenza diagnosis, experienced at least one acute cardiovascular event in the presence of underlying chronic conditions [45]. Patients in our cohort also developed serious complications that required hospital care or ER access. Cardiovascular and chronic diseases such as diabetes, were mainly observed in adults while respiratory complications were also common in young patients in line with what has been reported by Macias et al. [15]. , and in other studies [46,47,48] from different countries.
Hospitalization was the major HRU together with emergency room access which occurred before 84% of all admissions and was more frequent among young and elderly individuals. Few tests or laboratory exams (~ 1) were performed, on average during the hospital stay. An increase was observed in patients at risk, that required more investigations. Similarly, outpatient visits were more frequent among young children, individuals with underlying medical conditions, and the elderly. On average, the total costs were considerable and amounted to €9.7 million for the entire study period. Hospitalization costs accounted for almost 95% of the total direct costs of influenza, with €9.3 million. Of these, €2.6 million were attributed to elderly (≥ 75 years) and €2.6 million to patients at risk. The same was observed, on average, for outpatient visits whose impact on the economic burden weas greater for individuals in extreme age categories (i.e., 0–17 and ≥ 65) and with underlying comorbidities. Overall, the average cost (SD) per-inpatient stay was €4,007 (€ 7,620) for all epidemic seasons. Similarly, a recent study [49] on Turkish population aged > 18 years referring to the epidemic season 2018–2019 showed daily hospital costs equal to 3,274 USD in the influenza-positive group (N = 55), a higher value than non-influenza patients (N = 137; 2,765 USD) but also patients admitted with other respiratory infections but not influenza (N = 70; 3,103 USD). Taken together, our data highlight the significant clinical burden of seasonal influenza mainly on vulnerable individuals, and the high economic impact on the Italian healthcare system. Immunization with influenza vaccine [50] in addition with non-pharmaceutical public health measures [51, 52] may reduce the risk of getting severe illness, reduce the burden of its complications and the costs to the national government.
Limitations of the study
This study is based on data from four LHUs in Italy. Although the results are interesting from a public health perspective, they may not be fully generalized as the LHUs may not be representative of the whole national medical practice. The selection of geographically distributed mixture of heterogeneous centres, allowed to reduce the limited representativeness of the results but larger studies are needed to confirm our findings. Furthermore, as this is a retrospective real-world longitudinal study on Administrative Databases, data are not standardized across participating centres, and might be incomplete or differentially reported. Selection bias, i.e., the loss of patients using health services in a different region, and information bias, i.e., treatments in private hospitals for which reimbursement flow is not available, may also have an impact on the robustness of the results. Furthermore, patients were not classified according to vaccination status due to the lack of data on vaccine administration in Administrative Databases in Italy. Therefore, the impact of vaccination on clinical and economic burden cannot be directly assessed in the present study. Further data from vaccination centres, pharmacies and general practitioners are needed to investigate and quantify the effect of immunization on the hospital burden of influenza. Finally, the actual number of patients hospitalized with influenza might be underestimated due to the incorrect coding of flu diagnosis frequently observed in the SDO and due to the low number of diagnostic tests.
Conclusions
This is the first nationwide study that analyse the clinical and economic burden of hospitalized patients in Italy, with severe influenza during 5 epidemic seasons (2014–2019) and over a wide range of individual ages, from claims data. Our results show that age and underlying medical conditions increase the risk to develop severe illness that requires hospitalization. A weak and underdeveloped immune system in infants and young children and, conversely immunosenescence resulting from aging in adults and particularly in the elderly are the main determinants of the observed increase in the incidence of serious viral infection among these vulnerable individuals. Complications, mainly cardiac and respiratory, directly resulting from influenza or due to exacerbation of pre-existing comorbidities also worsen the clinical outcome of them and give rise to an additional influenza burden with an economic impact mainly due to required hospitalization or ER access and prolonged hospital stay. Although with limitations, mainly due to poor diagnosis and coding practices, our study broadly describes the Italian clinical burden of severe influenza reflecting the national trends reported by surveillance systems and provides data on the economic burden on the national government. Our results should be used to inform public health decision-making.
Data availability
Data can be made available on request on a case-by-case basis and depending on legal/privacy regulations.
Abbreviations
- ADs:
-
Administrative Databases
- LHUs:
-
Local Health Units
- ID:
-
Index date
- IQR:
-
Interquartile Range
- AD:
-
Administrative Data
- ATS:
-
Agenzia di Tutela della Salute
- ULSS:
-
Unità Locale Socio–Sanitaria
- ASL:
-
Azienda Sanitaria Locale
- SDO:
-
Scheda di Dimissione Ospedaliera
- DRG:
-
Diagnosis-Related Group
- ER:
-
Emergency Room
- ATC:
-
Anatomical-Therapeutic-Chemical
- EC:
-
Ethics Committee
- HRU:
-
Healthcare Resource Utilization
- INHS:
-
National Health Service
- SD:
-
Standard Deviation
- LTCF:
-
Long-term Care Facilities
- CIs:
-
Confidence Intervals
References
CDC, Centers for Disease Control and Prevention Types of Influenza Viruses. About Flu. https://www.cdc.gov/flu/about/viruses/types.htm#:~:text=There%20are%20four%20types%20of,global%20epidemics%20of%20flu%20disease. Accessed 20 November 2023.
EpiCentro. Influenza epidemiologia in Italia. https://www.epicentro.iss.it/influenza/epidemiologia-italia. Accessed 20 November 2023.
Boccalini S, Fiaschi P, Panatto D, Amicizia D, Lai PL, Gasparini R, Bechini A, Bonanni P. Epidemiologia dell’influenza stagionale negli anziani: Un’analisi dei dati italiani sulla sorveglianza clinico-epidemiologica e virologica. Ital J Public Health. 2017;6:4.
Influenza. (Seasonal). https://www.who.int/news-room/fact-sheets/detail/influenza-(seasonal). Accessed 20 November 2023.
CDC, Centers for Disease Control and Prevention. Epidemiology and Prevention of Vaccine-Preventable Diseases, Chap. 12: Influenza. https://www.cdc.gov/vaccines/pubs/pinkbook/flu.html#impact. Accessed 11 May 2023.
Iuliano AD, Roguski KM, Chang HH, Muscatello DJ, Palekar R, Tempia S, et al. Estimates of global seasonal influenza-associated respiratory mortality: a modelling study. Lancet. 2018;391(10127):1285–300.
Paget J, Spreeuwenberg P, Charu V, Taylor RJ, Iuliano AD, Bresee J, et al. Global mortality associated with seasonal influenza epidemics: New burden estimates and predictors from the GLaMOR Project. J Glob Health. 2019;9(2):020421.
Sellers SA, Hagan RS, Hayden FG, Fischer WA. The hidden burden of influenza: a review of the extra-pulmonary complications of influenza infection. Influenza Other Respir Viruses. 2017;11(5):372–93.
Mamas MA, Fraser D, Neyses L. Cardiovascular manifestations associated with influenza virus infection. Int J Cardiol. 2008;130(3):304–9.
Behrouzi B, Bhatt DL, Cannon CP, Vardeny O, Lee DS, Solomon SD, et al. Association of Influenza Vaccination with Cardiovascular Risk: a Meta-analysis. JAMA Netw Open. 2022;5(4):e228873.
Yedlapati SH, Khan SU, Talluri S, Lone AN, Khan MZ, Khan MS, et al. Effects of Influenza Vaccine on Mortality and Cardiovascular outcomes in patients with Cardiovascular Disease: a systematic review and Meta-analysis. J Am Heart Assoc. 2021;10(6):e019636.
San-Román-Montero JM, Gil Prieto R, Gallardo Pino C, Hinojosa Mena J, Zapatero Gaviria A, Gil de Miguel A. Inpatient hospital fatality related to coding (ICD-9-CM) of the influenza diagnosis in Spain (2009–2015). BMC Infect Dis. 2019;19(1):700.
Bertolani A, Fattore G, Pregliasco F. The hospitalization burden of influenza: just the tip of the iceberg? Grhta [Internet]. 2018 Jul. 10 [cited 2023 Nov. 20];5(1).
Divino V, Krishnarajah G, Pelton SI, Mould-Quevedo J, Anupindi VR, DeKoven M, et al. A real-world study evaluating the relative vaccine effectiveness of a cell-based quadrivalent influenza vaccine compared to egg-based quadrivalent influenza vaccine in the US during the 2017-18 influenza season. Vaccine. 2020;38(40):6334–43.
Macias AE, McElhaney JE, Chaves SS, Nealon J, Nunes MC, Samson SI, et al. The disease burden of influenza beyond respiratory illness. Vaccine. 2021;39(Suppl 1):A6–14.
Paules C, Subbarao K, Influenza. Lancet. 2017;390(10095):697–708.
Mehta SR, Afenyi-Annan A, Byrns PJ, Lottenberg R. Opportunities to improve outcomes in sickle cell disease. Am Fam Physician. 2006;74(2):303–10.
Uyeki TM, Bernstein HH, Bradley JS, Englund JA, File TM, Fry AM, et al. Clinical practice guidelines by the Infectious Diseases Society of America: 2018 update on diagnosis, treatment, Chemoprophylaxis, and Institutional Outbreak Management of Seasonal Influenzaa. Clin Infect Dis. 2019;68(6):895–902.
GBD 2017 Influenza Collaborators. Mortality, morbidity, and hospitalisations due to influenza lower respiratory tract infections, 2017: an analysis for the global burden of Disease Study 2017. Lancet Respir Med. 2019;7(1):69–89.
Newland JG, Laurich VM, Rosenquist AW, Heydon K, Licht DJ, Keren R, et al. Neurologic complications in children hospitalized with influenza: characteristics, incidence, and risk factors. J Pediatr. 2007;150(3):306–10.
Dell KM, Schulman SL. Rhabdomyolysis and acute renal failure in a child with influenza A infection. Pediatr Nephrol. 1997;11(3):363–5.
Brinar VV, Habek M, Brinar M, Malojcić B, Boban M. The differential diagnosis of acute transverse myelitis. Clin Neurol Neurosurg. 2006;108(3):278–83.
MacDonald KL, Osterholm MT, Hedberg CW, Schrock CG, Peterson GF, Jentzen JM, et al. Toxic shock syndrome. A newly recognized complication of influenza and influenzalike illness. JAMA. 1987;257(8):1053–8.
InfluNet. the Italian nationwide sentinel surveillance system for influenza. https://www.epicentro.iss.it/influenza/influnet. Accessed 20 November 2023.
Trentini F, Pariani E, Bella A, Diurno G, Crottogini L, Rizzo C, et al. Characterizing the transmission patterns of seasonal influenza in Italy: lessons from the last decade. BMC Public Health. 2022;22(1):19.
Caini S, Spreeuwenberg P, Kusznierz GF, Rudi JM, Owen R, Pennington K, et al. Distribution of influenza virus types by age using case-based global surveillance data from twenty-nine countries, 1999–2014. BMC Infect Dis. 2018;18(1):269.
Giacchetta I, Primieri C, Cavalieri R, Domnich A, de Waure C. The burden of seasonal influenza in Italy: a systematic review of influenza-related complications, hospitalizations, and mortality. Influenza Other Respir Viruses. 2022;16(2):351–65.
Zhang AJX, To KKW, Tse H, Chan KH, Guo KY, Li C, et al. High incidence of severe influenza among individuals over 50 years of age. Clin Vaccine Immunol. 2011;18(11):1918–24.
Langer J, Welch VL, Moran MM, Cane A, Lopez SMC, Srivastava A, et al. High clinical burden of Influenza Disease in adults aged ≥ 65 years: can we do better? A systematic literature review. Adv Ther. 2023;40(4):1601–27.
Ruf BR, Knuf M. The burden of seasonal and pandemic influenza in infants and children. Eur J Pediatr. 2014;173(3):265–76.
Krammer F, Smith GJD, Fouchier RAM, Peiris M, Kedzierska K, Doherty PC, et al. Influenza Nat Rev Dis Primers. 2018;4(1):3.
Andrew MK, Pott H, Staadegaard L, Paget J, Chaves SS, Ortiz JR, et al. Age differences in Comorbidities, presenting symptoms, and outcomes of Influenza Illness requiring hospitalization: a Worldwide Perspective from the Global Influenza Hospital Surveillance Network. Open Forum Infect Dis. 2023;10(6):ofad244.
Near AM, Tse J, Young-Xu Y, Hong DK, Reyes CM. Burden of influenza hospitalization among high-risk groups in the United States. BMC Health Serv Res. 2022;22(1):1209.
Czaja CA, Miller L, Alden N, Wald HL, Cummings CN, Rolfes MA, et al. Age-related differences in hospitalization rates, clinical presentation, and outcomes among older adults hospitalized with Influenza-U.S. Influenza Hospitalization Surveillance Network (FluSurv-NET). Open Forum Infect Dis. 2019;6(7):ofz225.
Aziz F, Aberer F, Moser O, Sourij C, von Lewinski D, Kaser S, et al. Impact of comorbidities on mortality in hospitalized influenza patients with diabetes - analysis of the Austrian Health Insurance. Diabetes Res Clin Pract. 2021;174:108758.
El Guerche-Séblain C, Etcheto A, Parmentier F, Afshar M, Macias E, Puentes A. Hospital admissions with influenza and impact of age and comorbidities on severe clinical outcomes in Brazil and Mexico. PLoS ONE. 2022;17(11):e0273837.
InfluNet. the Italian nationwide sentinel surveillance system for influenza: https://www.epicentro.iss.it/influenza/influnet. Accessed 27 November 2023.
European Centre for Disease Prevention and Control. Summary of the influenza 2015–2016 season in Europe. https://www.ecdc.europa.eu/en/publications-data/summary-influenza-2015-2016-season-europe. Accessed 27 November 2023.
CDC, Centers for Disease Control and Prevention Influenza Activity. — United States, 2015–16 season and composition of the 2016–17 influenza vaccine. Accessed 27 November 2023.
Lina B, Georges A, Burtseva E, Nunes MC, Andrew MK, McNeil SA, et al. Complicated hospitalization due to influenza: results from the Global Hospital Influenza Network for the 2017–2018 season. BMC Infect Dis. 2020;20(1):465.
Ludwig M, Jacob J, Basedow F, Andersohn F, Walker J. Clinical outcomes and characteristics of patients hospitalized for influenza or COVID-19 in Germany. Int J Infect Dis. 2021;103:316–22.
Soldevila N, Acosta L, Martínez A, Godoy P, Torner N, Rius C, et al. Behavior of hospitalized severe influenza cases according to the outcome variable in Catalonia, Spain, during the 2017–2018 season. Sci Rep. 2021;11(1):13587.
Owusu D, Rolfes MA, Arriola CS, Daily Kirley P, Alden NB, Meek J, et al. Rates of severe Influenza-Associated outcomes among older adults living with Diabetes-Influenza Hospitalization Surveillance Network (FluSurv-NET), 2012–2017. Open Forum Infect Dis. 2022;9(5):ofac131.
Allard R, Leclerc P, Tremblay C, Tannenbaum TN. Diabetes and the severity of pandemic influenza A (H1N1) infection. Diabetes Care. 2010;33(7):1491–3.
Chow EJ, Rolfes MA, O’Halloran A, Anderson EJ, Bennett NM, Billing L, et al. Acute Cardiovascular events Associated with Influenza in hospitalized adults: a cross-sectional study. Ann Intern Med. 2020;173(8):605–13.
Daoud A, Laktineh A, Macrander C, Mushtaq A, Soubani AO. Pulmonary complications of influenza infection: a targeted narrative review. Postgrad Med. 2019;131(5):299–308.
Skaarup KG, Modin D, Nielsen L, Jensen JUS, Biering-Sørensen T. Influenza and cardiovascular disease pathophysiology: strings attached. Eur Heart J Suppl. 2023;25(Suppl A):A5–11.
Dicembrini I, Silverii GA, Clerico A, Fornengo R, Gabutti G, Sordi V, et al. Influenza: diabetes as a risk factor for severe related-outcomes and the effectiveness of vaccination in diabetic population. A meta-analysis of observational studies. Nutr Metab Cardiovasc Dis. 2023;33(6):1099–110.
Bolek H, Ozisik L, Caliskan Z, Tanriover MD. Clinical outcomes and economic burden of seasonal influenza and other respiratory virus infections in hospitalized adults. J Med Virol. 2023;95(1):e28153.
Minozzi S, Lytras T, Gianola S, Gonzalez-Lorenzo M, Castellini G, Galli C, et al. Comparative efficacy and safety of vaccines to prevent seasonal influenza: a systematic review and network meta-analysis. EClinicalMedicine. 2022;46:101331.
World Health Organization. Non-pharmaceutical public health measures for mitigating the risk and impact of epidemic and pandemic influenza. https://www.who.int/publications/i/item/non-pharmaceutical-public-health-measuresfor-mitigating-the-risk-and-impact-of-epidemic-and-pandemic-influenza. Accessed 01 February 2024.
Fricke LM, Glöckner S, Dreier M, Lange B. Impact of non-pharmaceutical interventions targeted at COVID-19 pandemic on influenza burden - a systematic review. J Infect. 2021;82(1):1–35.
Acknowledgements
We are very grateful to all patients participating in this study. IQVIA Solution Italy supported the conduction, scientific support, data management, and statistical analysis of the study.
Funding
This study was funded by Sanofi, Italy.
Author information
Authors and Affiliations
Contributions
R.C. administered and supervised the project. S.F. prepared the data and performed the statistical analyses. R.C., M.V.A., L.Z. and E.L. carried out data interpretation. E.L. wrote the main manuscript and prepared all figures and tables. G.M., M.M., P.V. and A.Z. were responsible of data extraction. R.C., M.V.A., L.Z., M.R.G., E.X., P.G.M. and S.C. conceptualized the design of the study. All authors revised and edited the manuscript and have approved the final version for publication.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study has been notified and approved by the local Ethics Committees (ECs) of the four LHUs, according to the Italian regulation on observational studies. The ECs are: Comitato Etico di Brescia, Comitato Etico di Bergamo, Comitato Etico per le Sperimentazioni Cliniche (CESC) della Provincia di Vicenza, comitato Etico Interprovinciale Area 1 (A.O.U. Foggia, ASL Foggia, ASL BAT). A formal consent is not required for this type of retrospective observational study relying on secondary data that contains no directly identifiable data.
Consent for publication
Not applicable.
Competing interests
The authors declare the following financial interests/personal relationships which may be considered as potential competing interests: E. X. have disclosed that in the last two years she took part in advisory boards organized by: Eli Lilly, Regeneron Pharmaceuticals, Diurnal Limited, GSK Spa, Incyte Biosciences Italy Srl, Bristol-Mayers Squibb & Affiliates, Blueprint Medicines Italy Srl, Bayer AG, Takeda Pharmaceutical International AG, Astellas Pharma Europe Ltd, Takeda Italia Spa, Actelion Pharmaceuticals Ltd, Genzyme Europe BV, Gilead Sciences Srl, Sanofi Spa and other Italian and international consulting companies. She disclosed that she was engaged in consulting activities with Gilead Sciences Srl, Zambon Italia, Insmed Italy Srl. For the activities mentioned above, all unrelated to this article, she disclosed to have received fees. M.R. G. have disclosed that she received a fee by Sanofi, for a lecture.R. C., S. F., and E. L. have disclosed that they are employees of IQVIA Solutions SRL. M.V.A. and L. Z. are employees of Sanofi, the manufacturer of influenza vaccines, and may hold shares and/or stock options in the company.The remaining authors declare that they have no competing interests. E. X. have disclosed that in the last two years she took part in advisory boards organized by: Eli Lilly, Regeneron Pharmaceuticals, Diurnal Limited, GSK Spa, Incyte Biosciences Italy Srl, Bristol-Mayers Squibb & Affiliates, Blueprint Medicines Italy Srl, Bayer AG, Takeda Pharmaceutical International AG, Astellas Pharma Europe Ltd, Takeda Italia Spa, Actelion Pharmaceuticals Ltd, Genzyme Europe BV, Gilead Sciences Srl, Sanofi Spa and other Italian and international consulting companies. She disclosed that she was engaged in consulting activities with Gilead Sciences Srl, Zambon Italia, Insmed Italy Srl. For the activities mentioned above, all unrelated to this article, she disclosed to have received fees. M.R. G. have disclosed that she received a fee by Sanofi, for a lecture. R. C., S. F., and E. L. have disclosed that they are employees of IQVIA Solutions SRL. M.V.A. and L. Z. are employees of Sanofi, the manufacturer of influenza vaccines, and may hold shares and/or stock options in the company. The remaining authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Cipelli, R., Falato, S., Lusito, E. et al. The Hospital Burden of Flu in Italy: a retrospective study on administrative data from season 2014–2015 to 2018–2019. BMC Infect Dis 24, 572 (2024). https://doi.org/10.1186/s12879-024-09446-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12879-024-09446-2