Abstract
Background
While there is a high burden of methicillin-resistant Staphylococcus aureus (MRSA) infections among pediatric patients, studies on the molecular epidemiology of MRSA infections in Korean children since the 2010s are lacking. This study aimed to investigate the molecular genotypes and clinical characteristics of MRSA isolates from children with MRSA bacteremia at Asan Medical Center Children’s Hospital from 2016 to 2021.
Methods
Clinical data were retrospectively reviewed, and the molecular types of MRSA were determined using multilocus sequence typing (MLST) and Staphylococcal cassette chromosome mec (SCCmec) typing.
Results
The overall methicillin resistance rate of S. aureus bacteremia was 44.8% (77/172); 49.5% in the period 2016–2018 (period 1) and 37.3% in the period 2019–2021 (period 2) (P = 0.116). Community-acquired infections accounted for only 3.9% of cases. The predominant ST group was ST72 group (67.6%), followed by ST5 group (18.9%) and ST1 group (5.4%). The proportion of ST5 was significantly lower in period 2 compared to period 1 (P = 0.02). Compared to the ST5 and ST1 groups, the ST72 group exhibited lower overall antibiotic resistance and multidrug-resistant (MDR) rates (12.0% [6/50] in ST72 group vs. 100.0% [14/14] in ST5 group vs. 50.0% [2/4] in ST1 group; P < 0.001). In the multivariate analysis, the ST1 group was an independent risk factor for 30-day all-cause mortality (aOR, 44.12; 95% CI, 3.46–562.19).
Conclusion
The ST72-MRSA strain remained the most frequently isolated genotype in Korean children, while the ST1 group emerged as an independent risk factor for 30-day all-cause mortality in pediatric MRSA bacteremia. Ongoing efforts to uncover the evolving epidemiology of MRSA are essential for developing effective strategies for prevention and treatment.
Similar content being viewed by others
Introduction
Staphylococcus aureus bacteremia (SAB) can lead to substantial morbidity and mortality, even with appropriate antibiotic treatment [1]. The incidence of S. aureus bacteremia varies among pediatric patients, ranging from 3.7 to 15 per 100,000 individuals in different regions, with particularly high rates among infants under the age of one-year [1,2,3]. MRSA bacteremia has been associated with higher mortality rates compared to methicillin-susceptible S. aureus (MSSA) bacteremia [4]. In South Korea, the prevalence of methicillin-resistant S. aureus (MRSA) among pediatric patients with SAB admitted to a tertiary hospital was notably elevated, ranging from 65.2 to 76.1% between 2002 and 2016 [5].
Understanding the evolving molecular epidemiology of MRSA is important to effectively control MRSA transmission. Molecular typing methods, such as multilocus sequence typing (MLST) and Staphylococcal cassette chromosome mec (SCCmec) typing, allow the investigation of genetic backgrounds and spread of MRSA isolates across different time periods and geographic regions [6]. In South Korea, the sequence type (ST)72-MRSA has been the predominant genotype in both community and hospital settings since the mid-2000s, not only among adults but also in children [7, 8]. However, there is a lack of studies on the changes in the molecular epidemiology of MRSA infections among Korean children since the 2010s.
Moreover, the impact of specific MRSA genotypes on clinical outcomes remains incompletely understood. While there have been reports focusing on ST8-MRSA (USA300), that have not yielded definitive conclusions [9,10,11]. For instance, ST8-MRSA has been associated with severe sepsis in otherwise healthy children [10] and higher mortality in bacteremic patients [9]. However, another study has suggested that ST8 itself may not be directly linked to persistent bacteremia or treatment failure [11].
We aimed to investigate the molecular types and clinical characteristics of MRSA isolates obtained from children with bacteremia admitted to a tertiary children’s hospital in Korea over a span of 6 years. We also aimed to assess the potential impact of MRSA STs on antibiotic resistance patterns, clinical features, and overall outcomes.
Materials and methods
Study population and definitions
This retrospective observational study focused on pediatric patients aged ≤ 19 years who had MRSA bacteremia at Asan Medical Center Children’s Hospital, a 270-bed university-affiliated tertiary center located in Seoul, Korea, between January 2016 and December 2021. Relevant demographic and clinical data, including underlying diseases, primary sources of infection, severe presentation, persistent bacteremia, and mortality, were extracted from electronic medical records. Only the initial MRSA isolates detected during a single episode of MRSA bacteremia were included in the analysis with duplicates from the same patient being excluded. Although at least two sets of blood cultures were drawn for diagnosis in most cases of S. aureus bacteremia, the detection of S. aureus from blood cultures is considered a true infection due to the high probability of its true positivity of S. aureus from blood cultures and the clinical significance of S. aureus bacteremia.
MRSA infections were classified as community-onset (CO) if the first positive blood culture was obtained in an outpatient setting or within 48 h of hospital admission, and as hospital-onset (HO) infections if the first positive culture was obtained ≥ 48 h after hospital admission. Further classification of CO infections included community-acquired (CA) or healthcare-associated (HCA) infections based on healthcare-associated risk factors defined by Friedman et al. [12].
Primary bacteremia is defined as a condition where bacteremia occurs without an apparent or localized source of infection. The primary source of bacteremia was categorized as central line-associated bloodstream infection (CLABSI), bone and joint infection (BJI), skin soft tissue infection (SSTI), surgical site infection (SSI), or pneumonia, as per the definitions provided by the Centers for Disease Control and Prevention (CDC)’s National Healthcare Safety Network (NHSN) [13]. Infective endocarditis was defined according to the modified Duke criteria [14]. Severe presentation was defined as an episode requiring the initiation of vasopressors, an escalation in their dosage, or the commencement of mechanical ventilation within 48 h of MRSA bacteremia onset. Separate episodes were considered for cases in which MRSA was isolated again from the blood after at least a 3-month interval of culture-negativity. Persistent bacteremia at day 3 and day 7 was defined as a positive blood culture for more than 3 or 7 days, respectively, despite appropriate anti-MRSA therapy initiation. Mortality was evaluated by 30-day all-cause mortality and MRSA-related mortality, which was attributed directly to MRSA bacteremia without any other reasonable explanation. Clinical and microbiological outcomes were evaluated based on 30-day all-cause mortality and persistent bacteremia at day 7, respectively.
Strain identification and antimicrobial susceptibility testing
Strain identification and antimicrobial susceptibility testing were carried out using MicroScan WalkAway 96-Combo Pos 28 panels (Siemens, West Sacramento, CA, USA) for S. aureus isolates. The panel contained six wells with vancomycin concentrations ranging from 0.5 to 16.0 µg/mL. Additionally, the panel encompassed various antibiotics for susceptibility testing, including oxacillin, penicillin, ampicillin, amoxicillin/clavulanate, azithromycin, clindamycin, ciprofloxacin, daptomycin, erythromycin, fusidic acid, fosfomycin, gentamycin, imipenem, levofloxacin, linezolid, mupirocin, moxifloxacin, rifampin, quinupristin/dalfopristin, trimethoprim/sulfamethoxazole (TMP/SMX), tetracycline, and teicoplanin.
MRSA isolates of intermediate resistance or full resistance were defined as resistant. The in vitro macrolide-lincosamide-streptogramin B (MLSB)-inducible phenotype was detected by the D-zone test (double-disk diffusion test). Multidrug resistance (MDR) was defined as acquired non-susceptibility to at least one agent in three or more different classes of non-ß-lactam antibiotics [15]. The minimal inhibitory concentration (MIC) breakpoints were interpreted according to the standard criteria of the Clinical and Laboratory Standards Institute (CLSI) document M100 [16].
Multilocus sequence type (MLST) analysis and SCC mec typing
MLST analysis and SCCmec typing were conducted using the first MRSA isolates obtained during each bacteremic episode and stored at -70℃ for molecular analysis. MLST was performed by polymerase chain reaction (PCR) amplification and sequencing of seven housekeeping genes (arc, aroE, glpF, gmk, pta, tpi, ygiL), as described previously [17]. Each sequence was submitted to the MLST database (http://pubmlst.org) to assign an allelic profile and ST. Staphylococcal cassette chromosome mec (SCCmec) typing was carried out using multiplex PCR, as described previously [18].
Statistical analyses
The incidence of SAB was calculated as the annual number of episodes per 1,000 inpatients. The analysis of SAB incidence was performed using a Poisson regression model. For categorical variables, Chi-square or Fisher’s exact test was used, while the Mann–Whitney U test was employed for continuous variables. These tests were utilized to compare data between two periods (period 1, 2016–2018, and period 2, 2019–2021) and among three distinct ST groups: ST72, ST5, and ST1, each with its corresponding specific single locus variants(SLVs).
Univariate and multivariate logistic regression analyses were performed to identify independent risk factors associated with persistent bacteremia lasting more than 7 days and 30-day all-cause mortality. The multivariable analysis included variables with a P-value < 0.20 in univariate analysis. Statistical analysises were performed using SPSS version 23.0 (SPP Inc., Chicago, IL, USA). All significance tests were two-tailed, and P-values of ≤ 0.05 were considered statistically significant.
Results
Study population
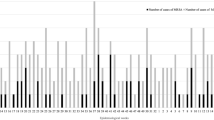
During the study period from January 2016 to December 2021, a total of 172 patients encountered SAB, resulting in an overall incidence rate of 2.39 per 1,000 patient-years (Fig. 1). An evident annual decline of 14% was observed in the overall incidence of SAB (from 2.74/1,000 inpatients in 2016 to 2.01/1,000 inpatients in 2021; P = 0.002) (Fig. 2). This reduction was primarily attributed to a yearly decrease of 23% in the incidence of MRSA bacteremia (from 1.33/1,000 inpatients in 2016 to 1.13/1,000 inpatients in 2021; P = 0.001). The overall methicillin resistance rate among SAB cases was 44.8% (77/172); this was 49.5% (52/95) during the period 2016–2018 (period 1) and 37.3% (25/67) during the period 2019–2021 (period 2) (P = 0.116).
The demographic and clinical characteristics of the 77 patients with MRSA bacteremia are presented in Table 1. The median age of the patients was 1.0 year (interquartile range [IQR], 0.0–6.0). 71 (92.5%) had underlying medical conditions, with 19 having hemato-oncologic disease and 11 having a history of stem cell or solid organ transplantation. Fifty-five cases (71.4%) were classified as HO MRSA infections, with 42 (54.6%) of them occurring during stays in intensive care units (ICUs): 16 in the neonatal ICU (NICU) and 26 in the pediatric ICU (PICU). During this study period, routine nasal surveillance for MRSA was conducted for all patients in the PICUs upon admission to PICU and then weekly thereafter. Pior to the onset of MRSA bacteremia, 43 (55.8%) patients were colonized with MRSA in the anterior nares. The most common primary source of MRSA bacteremia was the CLABSI (50.6%), followed by SSTI (10.4%). Primary bacteremia accounted for 19.5% of all infections. Out of the 39 MRSA CLABSI episodes, 10 (25.6%) were complicated bacteremia, including venous thrombi (n = 6), septic emboli (n = 3), and infective endocarditis (n = 1). The four instances of SSI involved deep-seated infections, including mediastinitis (n = 2) and complicated pleural effusion (n = 2). Only 3.9% of MRSA bacteremia occurred in previously healthy children without healthcare risk factors, with SSTI (n = 2) and BJI (n = 1) as the primary foci. All patients with MRSA bacteremia were treated with in vitro susceptible glycopeptides within 48 h of bacteremia onset.
Severe presentation, requiring vasopressors administration or mechanical ventilation within 48 h of bacteremia onset, was observed in 13 cases (16.9%), and the 30-day all-cause mortality rate was 10.4% (8/77). Among the three MRSA-related deaths, the median time from bacteremia onset to death was 5.0 days (IQR, 1.0–10.5). The median duration of bacteremia was 3.0 days (IQR, 1.0–4.0), with 22 (28.9%) patients experiencing persistent bacteremia at day 3 and 9 (12.0%) at day 7, despite initiation of appropriate antibiotic therapy.
Comparing period 2 to period 1, the rate of primary bacteremia was significantly lower (26.9% [14/52] in period 1 vs. 4.0% [1/25] in period 2; P = 0.03), and persistent bacteremia at day 3 was observed more frequently (21.6% [11/52] in period 1 vs. 44.0% [11/25] in period 2; P = 0.04).
Molecular characterization
A total of 74 available MRSA isolates underwent molecular characterization, all of which tested positive for the mec A gene. Among these, SCCmec types I, II, and IV were detected, with SCCmec type IV being the most prevalent (71.4%). The proportion of SCCmec type IV increased during period 2 (84.0%) compared to period 1 (71.4%) (p = 0.2) (Table 2). Within the ST72 group (n = 50), which included ST72 (n = 47) and its single locus variants (SLVs) ST2084 (n = 2) and a novel SLV (n = 1), SCCmec type IV was most frequently detected (n = 47; 94.0%), with three isolates exhibiting SCCmec type II (n = 2) and SCCmec type I (n = 1). All ST5 isolates (n = 9) and its SLVs, including ST632 (n = 1) and novel SLVs (n = 3) (referred to hereafter as the ST5 group), harbored only SCCmec type II. Among the ST1 group including ST1 (n = 3) and one novel SLV of ST1 (n = 1), only SCCmec type IV was identified.
In period 2 compared to period 1, the proportion of the ST72 group was higher (63.3% [31/49] vs. 76.0% [19/25]; P = 0.27), and that of the ST5 group was lower (22.4% [11/49] vs. 12.0% [3/25]; P = 0.36), although there was no statistical significance. Furthermore, all the ST5 MRSA strains were identified only during period 1 (18.4% [9/20] in period 1 vs. 0% [0/25] in period 2; P = 0.02).
Regardless of hospital or community settings, ST72 group predominated (67.6%), followed by ST5 group (18.9%) and ST1 group (5.4%). Notably, ST5 and ST1 were exclusively observed in HO infections. The ST72 group showed a lower likelihood of being associated with HO infection (62.0% [31/50] vs. 94.4% [17/18]; P = 0.014) and previous MRSA colonization (46.0% [23/50] vs. 88.9% [16/18], P = 0.002) compared to the ST1 or ST5 groups.
Clinical significance of three different ST groups
Regarding clinical outcomes, the 30-day all-cause mortality rates for each ST group were as follows: 75% (3/4) for the ST1 group, 10% (5/50) for the ST72 group, and none for the ST5 group. After adjusting for primary bacteremia and ST1 group, multivariate analysis revealed that the ST1 group was an independent risk factor for 30-day all-cause mortality (adjusted odds ratio [aOR], 44.12; 95% confidence interval [CI], 3.46–562.19) (Table 3).
Considering microbiological outcomes, within the ST1 group, 50% (2/4) of cases exhibited persistent bacteremia at day 7, while the corresponding figures for the ST5 and ST72 groups were 7.1% (1/14) and 10% (5/50), respectively. In addition, MRSA bacteremic pneumonia was associated with persistent bacteremia at day 7 (aOR, 8.63; 95% CI, 1.25–56.62). Although univariate analysis indicated an association between the ST1 group and persistent bacteremia at day 7 (OR, 17.71; 95% CI, 1.42–221.15), after adjusting for bacteremic pneumonia and ST1 group, the ST1 group itself did not remain a significant risk factor for persistent bacteremia at day 7 (aOR, 14.37; 95% CI, 0.96–216.06).
Antimicrobial resistance rates
All MRSA isolates were susceptible to vancomycin with 88.3% (68/75) having a vancomycin MIC of 1.0 μg/mL (Additional file 1: Table S1). The MDR rate was 38.8% (26/77), and the clindamycin resistance rate was 32.5% (25/77), including 20.8% (16/77) constitutive resistance and 31.0% (9/29) inducible resistance. No statistically significant differences in resistance rates were observed between the two periods for each antibiotic.
In comparison to the ST5 and ST1 groups, the MRSA ST72 group demonstrated lower overall antibiotic resistance and MDR rates among the three different ST groups (Additional file 1: Table S2). The clindamycin resistance rate within the ST5 group was 100%, while it was 12% (6/50) within the ST72 group. Among the five MRSA isolates with a vancomycin MIC of 2 μg/mL, three were from the ST72 group, and two were from the ST5 group.
Discussion
This study focused on pediatric MRSA bacteremia demonstrates that ST72-SCCmec type IV MRSA has been the predominant strain between 2016 and 2021, replacing the ST5-SCCmec type II strain in hospital-onset infections among Korean children. Furthermore, the ST1 group was identified as an independent risk factor for 30-day all-cause mortality.
While MRSA rates in SAB have been decreasing in Europe and the United States since the 2000s [2, 19, 20], and a similar trend has been observed in adults in South Korea [21, 22], the MRSA rate among SAB cases in Korean children remained high, ranging from 51.9 to 76.1% between 2002 and 2016 [5]. However, during the study period, the incidence of pediatric MRSA bacteremia decreased by 23% annually, with MRSA accounting for 47.5% of SAB cases. Although the exact reason for this decreasing trend is unclear, the hospital`s efforts to strengthen infection prevention measures, including active MRSA surveillance, targeted precautions, and bundle approaches for CLABSI or ventilator-associated pneumonia, may have played a role. Notably, HO infections constituted approximately 70% of MRSA bacteremia cases, highlighting the significance of hospital-based infection control strategies.
Although understanding the molecular epidemiology of MRSA is crucial for controlling MRSA transmission in healthcare settings [6], there is limited pediatric data available. In the past, MRSA genotypes were distinguishable between community and hospital settings, but this differentiation has become challenging since the 1990s [4]. In our study, the predominant genotype was ST72-MRSA-SCCmec type IV, which was initially associated with the community but has now become prevalent in hospital settings, especially in the PICU. This observation aligns with the finding that ST72 has become endemic within the Korean pediatric population and exhibits effective spread among children in hospital settings [8, 23].
The study revealed that ST5, previously recognized as a pandemic hospital genotype, declined significantly during the study period. This finding is consistent with previous research in Korean adult populations, indicating a decrease in the prevalence of ST5 since the mid-2000s [7, 22]. This reduction could be related to infection control measures targeting central venous catheters, given that ST5 has been associated with S. aureus central-line related infection [22]. However, our study found that ST5 was being replaced by ST72 in pediatric MRSA CLABSI without significantly changing the overall incidence of CLABSI.
The ST1 (USA 400) emerged as the third most common genotype, with its prevalence remaining relatively constant throughout the study period, despite being infrequently detected in previous pediatric MRSA studies in Korea [8, 23]. ST1 has shown higher lethality in a rabbit model of S. aureus endocarditis [24], and lower virulence than ST8 in a rat model of MRSA pneumonia [25]. However, its impact on the clinical significance of human MRSA infections has rarely been reported. Our study revealed that the ST1 group was independently associated with higher mortality compared to the ST5 and ST72 groups. While an adult MRSA bacteremia study found that ST72 was independently associated with lower mortality than ST5 [26], our study did not reveal that ST72 or ST5 increased mortality with statistical significance. Overall, these findings underscore the importance of considering the specific ST of MRSA when assessing the clinical significance and mortality risk of MRSA infections. Different STs may possess varying virulence factors and impact patient outcomes differently. Further research to explore virulence factors according to ST will be necessary to validate the clinical significance of ST.
The ST72 group of MRSA strains exhibited relatively lower MDR and higher susceptibility to non-β-lactam antibiotics such as clindamycin, which can be considered as an option for empirical treatment in the outpatient setting. Our study revealed that all cases of BJIs and SSTIs occurred in the ST72 group, aligning with findings from a previous Korean pediatric study that identified ST72 as the most common ST in children with SSTI/BJI [27]. Considering the presence of inducible clindamycin resistance in a notable portion of ST72-MRSA isolates, performing a D-test is recommended to prevent treatment failure in MRSA infections like BJIs and SSTIs, which are frequently encountered in the community settings among Korean children.
Antibiotic resistance varied among genotypes; ST5, carrying SCCmec type IV, generally exhibited higher susceptibility to non-β-lactam antibiotics due to the absence of resistance-conferring genes compared to SCCmec types I and II [4]. Moreover, antibiotic resistance patterns could be influenced by spa types or regional differences [22, 28], and antibiotic pressure in hospital settings might contribute to the emergence of multi-drug resistance [29, 30]. In addition, certain genotypes may evolve easily, leading to the acquisition of resistance to specific antibiotics. For istance, ST5 showed increased resistance to chlorhexidine after the implementation of chlorhexidine bathing in hospital settings in Korea [30]. Fortunately, our study did not observe an increase in antibiotic resistance among ST72 during the study period. However, given the increasing prevalence of ST72 in hospital settings, it remains crucial to monitor any potential alterations in antibiotic resistance within this genotype.
There are several limitations to this study. Firstly, the findings cannot be extrapolated to other pediatric populations, including general pediatric population in South Korea, different hospitals, or different geographical areas. This is because the study was conducted solely at a single referral tertiary hospital, which serves a pediatric patient population with oncologic, hematopoietic stem cell transplantation, and solid organ transplantation backgrounds. Additionally, our study specifically focused on MRSA isolates obtained from pediatric patients with bacteremia, which may make its applicability more relevant to severe MRSA infections, such as complicated S. aureus bacteremia associated with underlying comorbidities. Secondly, the number of isolates analyzed may have been insufficient to achieve statistical significance when identifying risk factors for outcomes. However, the assessment of clinical impacts associated with specific STs in the context of pediatric patients in Korea, where ST72 predominates, is a rare endeavor. While our findings revealed that the ST72 group was not a risk factor for mortality or persistent bacteremia, consistent with previous adult studies [26], the ST1 emerged as an independent risk factor for 30-day all-cause mortality. Further research is warranted to delve into the factors contributing to clinical severity or virulence within ST1-MRSA strains. Large-scale studies might provide more robust statistical power to identify risk factors for outcomes. Thirdly, strain-specific virulence genes of MRSA isolates that could play pivotal roles in virulence were not identified in this study. Additionally, we did not establish associations between specific STs and clinical outcomes in relation to virulence factors. Therefore, further studies involving comprehensive whole-genome studies are necessary to validate the roles of virulence factors and their implications in clinical contexts.
Conclusion
The ST72-MRSA strain was the most frequently identified strain over a 6-year period, from 2016 to 2021, among Korean children. ST1 was an independent risk factor for 30-day all-cause mortality in pediatric patients with MRSA bacteremia. Continous surveillance and monitoring of MRSA are important to gain a deeper understanding of the evolving epidemiology of MRSA and to inform effective strategies for prevention and treatment.
Data availability
All data generated or analysed during this study are included in this published article and its additional information files.
References
McMullan BJ, Bowen A, Blyth CC, Van Hal S, Korman TM, Buttery J, et al. Epidemiology and mortality of Staphylococcus aureus Bacteremia in Australian and New Zealand children. JAMA Pediatr. 2016;170(10):979–86.
Cobos-Carrascosa E, Soler-Palacin P, Nieves Larrosa M, Bartolome R, Martin-Nalda A, Antoinette Frick M, et al. Staphylococcus aureus Bacteremia in Children: changes during eighteen years. Pediatr Infect Dis J. 2015;34(12):1329–34.
Oestergaard LB, Schmiegelow MDS, Bruun NE, Skov R, Andersen PS, Larsen AR, et al. Staphylococcus aureus Bacteremia in Children aged 5–18 years-risk factors in the New Millennium. J Pediatr. 2018;203:108–15e3.
Lakhundi S, Zhang K. Methicillin-Resistant Staphylococcus aureus: molecular characterization, evolution, and Epidemiology. Clin Microbiol Rev. 2018;31(4).
Lim S, Ha SG, Tchah H, Jeon IS, Ryoo E, Son DW et al. Epidemiology of Staphylococcus aureus Bacteremia in Children at a single Center from 2002 to 2016. Pediatr Infect Vaccine. 2019;26(1).
Deurenberg RH, Stobberingh EE. The evolution of Staphylococcus aureus. Infect Genet Evol. 2008;8(6):747–63.
Chen CJ, Huang YC. New epidemiology of Staphylococcus aureus Infection in Asia. Clin Microbiol Infect. 2014;20(7):605–23.
Sung JY, Lee J, Choi EH, Lee HJ. Changes in molecular epidemiology of community-associated and health care-associated methicillin-resistant Staphylococcus aureus in Korean children. Diagn Microbiol Infect Dis. 2012;74(1):28–33.
Kempker RR, Farley MM, Ladson JL, Satola S, Ray SM. Association of methicillin-resistant Staphylococcus aureus (MRSA) USA300 genotype with mortality in MRSA bacteremia. J Infect. 2010;61(5):372–81.
Gonzalez BE, Martinez-Aguilar G, Hulten KG, Hammerman WA, Coss-Bu J, Avalos-Mishaan A, et al. Severe staphylococcal sepsis in adolescents in the era of community-acquired methicillin-resistant Staphylococcus aureus. Pediatrics. 2005;115(3):642–8.
Lalani T, Federspiel JJ, Boucher HW, Rude TH, Bae I-G, Rybak MJ, et al. Associations between the genotypes of Staphylococcus aureus Bloodstream isolates and clinical characteristics and outcomes of bacteremic patients. J Clin Microbiol. 2008;46(9):2890–6.
Friedman ND, Kaye KS, Stout JE, McGarry SA, Trivette SL, Briggs JP, et al. Health care–associated bloodstream Infections in adults: a reason to change the accepted definition of community-acquired Infections. Ann Intern Med. 2002;137(10):791–7.
Centers for Disease Control and Prevention. National Healthcare Safety Network (NHSN) Patient Safety Component Manual. 2023. https://www.cdc.gov/nhsn/psc/index.html Accessed 10 July 2023.
Baltimore RS, Gewitz M, Baddour LM, Beerman LB, Jackson MA, Lockhart PB, et al. Infective endocarditis in Childhood: 2015 Update: A Scientific Statement from the American Heart Association. Circulation. 2015;132(15):1487–515.
Pillar CM, Draghi DC, Sheehan DJ, Sahm DF. Prevalence of multidrug-resistant, methicillin-resistant Staphylococcus aureus in the United States: findings of the stratified analysis of the 2004 to 2005 LEADER Surveillance Programs. Diagn Microbiol Infect Dis. 2008;60(2):221–4.
Cllinical and Laboratory Standards Institute (CLSI). Performance standards for antimicrobial susceptibility testing. 33rd ed. USA: Cllinical and Laboratory Standards Institute; 2023.
Enright MC, Day NP, Davies CE, Peacock SJ, Spratt BG. Multilocus sequence typing for characterization of methicillin-resistant and methicillin-susceptible clones of Staphylococcus aureus. J Clin Microbiol. 2000;38(3):1008–15.
Milheirico C, Oliveira DC, de Lencastre H. Update to the multiplex PCR strategy for assignment of mec element types in Staphylococcus aureus. Antimicrob Agents Chemother. 2007;51(9):3374–7.
Dantes R, Mu Y, Belflower R, Aragon D, Dumyati G, Harrison LH, et al. National burden of invasive methicillin-resistant Staphylococcus aureus Infections, United States, 2011. JAMA Intern Med. 2013;173(21):1970–8.
de Kraker ME, Jarlier V, Monen JC, Heuer OE, van de Sande N, Grundmann H. The changing epidemiology of bacteraemias in Europe: trends from the European Antimicrobial Resistance Surveillance System. Clin Microbiol Infect. 2013;19(9):860–8.
Bae E, Kim CK, Jang JH, Sung H, Choi Y, Kim MN. Impact of community-onset methicillin-resistant Staphylococcus aureus on Staphylococcus aureus Bacteremia in a Central Korea Veterans Health Service Hospital. Ann Lab Med. 2019;39(2):158–66.
Choi SH, Lee J, Jung J, Kim ES, Kim MJ, Chong YP, et al. A longitudinal study of adult patients with Staphylococcus aureus Bacteremia over 11 years in Korea. J Korean Med Sci. 2021;36(16):e104.
Kang S, Lee J, Kim M. The association between Staphylococcus aureus nasal colonization and symptomatic Infection in children in Korea where ST72 is the major genotype: a prospective observational study. Med (Baltim). 2017;96(34):e7838.
King JM, Kulhankova K, Stach CS, Vu BG, Salgado-Pabon W. Phenotypes and virulence among Staphylococcus aureus USA100, USA200, USA300, USA400, and USA600 Clonal lineages. mSphere. 2016;1(3).
Montgomery CP, Boyle-Vavra S, Adem PV, Lee JC, Husain AN, Clasen J, et al. Comparison of virulence in community-associated methicillin-resistant Staphylococcus aureus pulsotypes USA300 and USA400 in a rat model of Pneumonia. J Infect Dis. 2008;198(4):561–70.
Park KH, Chong YP, Kim SH, Lee SO, Choi SH, Lee MS, et al. Community-associated MRSA strain ST72-SCCmecIV causing bloodstream Infections: clinical outcomes and bacterial virulence factors. J Antimicrob Chemother. 2015;70(4):1185–92.
Park SG, Lee HS, Park JY, Lee H. Molecular Epidemiology of Staphylococcus aureus in skin and soft tissue Infections and bone and joint Infections in Korean Children. J Korean Med Sci. 2019;34(49):e315.
Kaku N, Sasaki D, Ota K, Miyazaki T, Yanagihara K. Changing molecular epidemiology and characteristics of MRSA isolated from bloodstream Infections: nationwide surveillance in Japan in 2019. J Antimicrob Chemother. 2022;77(8):2130–41.
Naimi TS, LeDell KH, Como-Sabetti K, Borchardt SM, Boxrud DJ, Etienne J, et al. Comparison of community- and health care-associated methicillin-resistant Staphylococcus aureus Infection. JAMA. 2003;290(22):2976–84.
Kim H, Park S, Seo H, Chung H, Kim ES, Sung H, et al. Clinical impact of and microbiological risk factors for qacA/B positivity in ICU-acquired ST5-methicillin-resistant SCCmec type II Staphylococcus aureus bacteremia. Sci Rep. 2022;12(1):11413.
Acknowledgements
We would like to express our gratitude to Professor Mina Kim and Heungsup Sung at the Department of Laboratory Medicine, Asan Medical Center.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
GK as first writing author conceived and designed the study. GK, SL, YL and JHK collected and analyzed data. GK interpretated data and wrote the paper. JL, corresponding author, supervised and reviewed the paper. All authors have read and approved the published version of the manuscript.
Corresponding author
Ethics declarations
Ethical approval and consent to participate
Our study protocol was reviewed and approved by the Institutional Review Board of the Asan Medical Center (IRB No. 2023-0099). Requirements for informed consent were waived by ethics committee of Asan Medical Center Institutional Review Board due to the retrospective, de-identified data collection and analysis. The study was approved by the institutional review board of the Asan Medical Center (AMC) (IRB No. 2023 − 1155).
Cosent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Kim, G., Lee, S., Lee, Y. et al. The molecular epidemiology and clinical implication of methicillin-resistant Staphylococcus aureus (MRSA) sequence types in pediatric bacteremia: a restrospective observational study, 2016–2021. BMC Infect Dis 24, 259 (2024). https://doi.org/10.1186/s12879-023-08914-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12879-023-08914-5