Abstract
Sepsis is a rapidly evolving disease with a high mortality rate. The early identification of sepsis and the implementation of early evidence-based therapies have been recognized to improve outcome and decrease sepsis-related mortality. The aim of this study was to compare the accuracy of the standard diagnostic work-up of septic patients with an integrated approach using early point of care ultrasound (POCUS) to identify the source of infection and to speed up the time to diagnosis. We enrolled a consecutive sample of adult patients admitted to the ED who met the Surviving Sepsis Campaign (SSC) criteria for sepsis. For every patient, the emergency physician was asked to identify the septic source after the initial clinical assessment and after POCUS. Patients were then addressed to the standard predefined work-up. The impression at the initial clinical assessment and POCUS-implemented diagnosis was compared with the final diagnosis of the septic source, determined by independent review of the entire medical record after discharge. Two hundred consecutive patients entered the study. A final diagnosis of the septic source was obtained in 178 out of 200 patients (89 %). POCUS-implemented diagnosis had a sensitivity of 73 % (95 % CI 66–79 %), a specificity of 95 % (95 % CI 77–99 %), and an accuracy of 75 %. Clinical impression after the initial clinical assessment (T0) had a sensitivity of 48 % (CI 95 % 41–55 %) and a specificity of 86 % (CI 95 % 66–95 %). POCUS improved the sensitivity of the initial clinical impression by 25 %. POCUS-implemented diagnoses were always obtained within 10 min. Instead the septic source was identified within 1 h in only 21.9 % and within 3 h in 52.8 % with a standard work-up. POCUS-implemented diagnosis is an effective and reliable tool for the identification of septic source, and it is superior to the initial clinical evaluation alone. It is likely that a wider use of POCUS in an emergency setting will allow a faster diagnosis of the septic source, leading to more appropriate and prompt antimicrobial therapy and source control strategies.


Similar content being viewed by others
References
Levy MM, Dellinger RP, Townsend SR, Campaign Surviving Sepsis (2010) The Surviving Sepsis Campaign: results of an international guideline-based performance improvement program targeting severe sepsis. Crit Care Med 38:367–374
Esteban A et al (2007) Sepsis incidence and outcome: contrasting the intensive care unit with the hospital ward. Crit Care Med 35(5):1284–1289
Jones AE, Shapiro NI, Trzeciak S, Emergency MEDICINE SHOCK RESEARCH NETWORk (EMShockNet) Investigators et al (2010) Lactate clearance vs central venous oxygen saturation as goals of early sepsis therapy: a randomized clinical trial. JAMA 303:739–746
Jansen TC, van Bommel J, Schoonderbeek FJ et al (2010) Early lactate-guided therapy in intensive care unit patients: a multicenter, open label, randomized controlled trial. Am J Respir Crit Care Med 182:752–761
Cinel I, Dellinger RP (2006) Current treatment of severe sepsis. Curr Infect Dis Rep 8(358–365):210
Barie PS, Hydo LJ, Shou J et al (2005) Influence of antibiotic therapy on mortality of critical illness caused or complicated by infection. Surg Infect 6:41–54
Kumar A, Roberts D, Wood KE et al (2006) Duration of hypotension prior to initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock. Crit Care Med 34:1589–1596
Kollef MH, Sherman G, Ward S, Fraser VJ (1999) Inadequate antimicrobial treatment of infections: a risk factor for hospital mortality among critically ill patients. Chest 115:462–474. doi:10.1378/chest.115.2.462
Lueangarun S, Leelarasamee A (2012) Impact of inappropriate empiric antimicrobial therapy on mortality of septic patients with bacteremia: a retrospective study. Interdiscip Perspect Infect Dis. 2012:765205. doi:10.1155/2012/765205
Marquet K, Liesenborgs A, Bergs J, Vleugels A, Claes N (2015) Incidence and outcome of inappropriate in-hospital empiric antibiotics for severe infection: a systematic review and meta-analysis. Crit Care 16(19):63. doi:10.1186/s13054-015-0795-y
Ibrahim EH, Sherman G, Ward S, Fraser VJ, Kollef MH (2000) The influence of inadequate antimicrobial treatment of bloodstream infections on patient outcomes in the ICU setting. Chest 118:146–155. doi:10.1378/chest.118.1.146
Dellinger Levy MM, Rhodes A, Annane D, Gerlach H et al (2013) Surviving Sepsis Campaign: international guidelines for management of severe sepsis and septic shock: 2012. Crit Care Med 41(2):580–637
Carlbom DJ, Rubenfeld GD (2007) Barriers to implementing protocol-based sepsis resuscitation in the emergency department—results of a national survey. Crit Care Med 35:25–32
Jimenez MF, Marshall JC (2001) Source control in the management of sepsis. Intensive Care Med 27:S49–S62
Marshall JC, Maier RV, Jimenez M, Dellinger EP (2004) Source control in the management of severe sepsis and septic shock: an evidence-based review. Crit Care Med 32(11 Suppl):S513–S526
Azhuata T, Kinoshita K, Kawano D, Komatsu T, Sakurai A, Chiba Y, Tanjho K (2014) Time from admission to initiation of surgery for source control is a critical determinant of survival in patients with gastrointestinal perforation with associated septic shock. Crit Care 18(3):R87
Coen D, Cortellaro F, Pasini S, Tombini V et al (2014) Towards a less invasive approach to the early goal-directed treatment of septic shock in the ED. Am J Emerg Med 32(6):563–568
Cortellaro F, Colombo S, Coen D, Duca PG (2012) Lung ultrasound is an accurate diagnostic tool for the diagnosis of pneumonia in the emergency department. Emerg Med J. 29(1):19–23
Da Dalrymple NC et al (2009) Diagnostica per immagini dell’addome: problem solving. Elsevier Masson, Amsterdam
Martino F et al (2006) Ecografia dell’apparato osteo-articolare: anatomia, semeiotica e quadri patologici. Springer, London
Otto CM (2009) Textbook of clinical echocardiography. Saunders, Philadelphia
Shinkins B, Thompson M, Mallett S, Perera R et al (2013) Diagnostic accuracy studies: how to report and analyze inconclusive test results. BMJ 346:f2778
Fleiss JL, Levin B, Paik MC (2003) Statistical methods for rates and proportions. Wiley Interscience, New York, p 379
Jones AE, Tayal VS, Sullivan DM, Kline J (2004) Randomized, controlled trial of immediate versus delayed goal-directed ultrasound to identify the cause of nontraumatic hypotension in emergency department patients. Crit Care Med 32(8):1703–1708
Fish DN (2002) Optimal antimicrobial therapy for sepsis. Am Soc Health Syst Pharm 59:s13–s19
Musher DM et al (2013) An etiologic agent be identified in adults who are hospitalized for community-acquired pneumonia: results of a one-year study. J Infect 67:11–18
Lewy MM, Fink MP et al (2013) 2001 SCCM/ESICM/ACCP/ATS/SIS international sepsis definition conferenze. Crit Care Med 31:1250–1256
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Appendices
Appendix 1. Informed consent to participate

Appendix 2. Surviving Sepsis Campaign criteria for sepsis
Criteri diagnostici per sepsi. Adapt. Ref. [27].

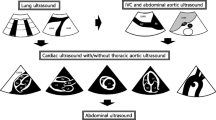
Appendix 3. Technical approach of POCUS
Descriptive POCUS findings
Anatomic district | Normal findings | Pathological findings |
|---|---|---|
Lung Anterolateral and posterior scans (two anterior, two lateral, one posterior) Convex 3.5–5 MHz probe/linear 5–7 mHz probe | ||
Sub-pleural lung consolidation, presenting a tissutal pattern with dynamic air or multiple hyper-echogenic spots | No | Yes |
Focal interstitial syndrome | No | Yes |
Presence of pleural fluid | No | Yes |
Heart Parasternal view (long and short axis), apical view, subcostal view (4-chambers) Sector 2–2.5 MHz probe | ||
Presence of vegetation on the valve surface | No | Yes |
Abdomen | ||
(1) Gallbladder and biliary duct Convex 3.5–5 MHz probe | ||
Wall thickness >4 mm | No | Yes |
Pericholecystic fluid | No | Yes |
Gallstones/sludge | No | Yes |
Echographic murphy sign | No | Yes |
Common bile duct >5 mm | No | Yes |
(2) Liver Convex 3.5–5 MHz probe | ||
Hepatic abscess | ||
Ascites (primary PBS) | No | Yes |
(3) Diverticula Convex 3.5–5 MHz probe/linear 5–7 mHz probe | ||
Presence of diverticula | No | Yes |
Wall thickness >3 mm | No | Yes |
Inflammatory peri-colonic fat | No | Yes |
Presence of abscesses | No | Yes |
Peri-colonic free fluid | No | Yes |
(4) Appendix Convex 3.5–5 MHz probe/linear 5–7 mHz probe | ||
Total diameter on cross section >6 mm or Wall thickness >3 mm | ||
Non compressible-appendix | No | Yes |
Inflammatory peri-appendiceal fat | No | Yes |
Presence of abscesses | No | Yes |
Peri-appendiceal free fluid | No | Yes |
(5) Abdominal-muscle abscesses Convex 3.5–5 MHz probe | ||
Presence of abscesses | No | Yes |
(6) Kidney Convex 3.5–5 MHz probe | ||
Hydronephrosis | No | Yes |
Presence of renal abscess | No | Yes |
Urethorolithyasis | No | Yes |
Joints Linear 5–7 mHz probe | ||
Intra-articular fluid | No | Yes |
Rights and permissions
About this article
Cite this article
Cortellaro, F., Ferrari, L., Molteni, F. et al. Accuracy of point of care ultrasound to identify the source of infection in septic patients: a prospective study. Intern Emerg Med 12, 371–378 (2017). https://doi.org/10.1007/s11739-016-1470-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-016-1470-2