Abstract
Purpose
Obesity increases the severity of asthma, and patients with severe asthma are often complicated with obstructive sleep apnea syndrome (OSAS), a concomitant disease of obesity. We investigated whether intermittent hypoxia (IH), which is a physiological feature of OSAS, modifies allergic airway inflammation in a murine model of asthma.
Methods
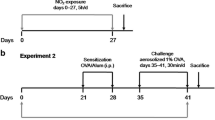
Balb/c mice were sensitized by ovalbumin (OVA) intraperitoneally twice (days 1 and 14) and challenged with intranasal OVA three times (days 21, 22, and 23). The mice were exposed to IH either from days 1 to 24 (long exposure) or only from days 21 to 24 (short exposure). The impact of IH exposure to allergic airway inflammation was investigated using these mice models by histologic, morphometric, and molecular techniques. Additionally, the airway responsiveness to acetylcholine was also assessed.
Results
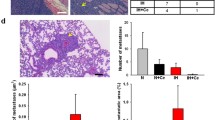
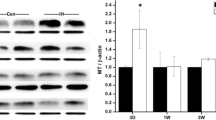
OVA-sensitized and OVA-challenged mice exposed to room air (RA) showed increased total cell and eosinophil numbers in the BALF. The levels of interleukin (IL)-5 and IL-13 in the BALF also increased and goblet cell metaplasia was induced. In contrast, both long and short exposure to IH inhibited the increased total cell and eosinophil numbers. The levels of IL-5 and IL-13 in the BALF also decreased on exposure to IH. Moreover, the goblet cell hyperplasia and airway hyperresponsiveness were significantly reduced in mice exposed to IH compared to those exposed to RA.
Conclusions
These results suggest that IH may not deteriorate the asthmatic condition in a murine model of asthma.






Similar content being viewed by others
References
Partinen M, Telakivi T (1992) Epidemiology of obstructive sleep apnea syndrome. Sleep 15:S1–S4
Durán J, Esnaola S, Rubio R, Iztueta A (2001) Obstructive sleep apnea-hypopnea and related clinical features in a population-based sample of subjects aged 30 to 70 yr. Am J Respir Crit Care Med 163(3 Pt 1):685–689
Peppard PE, Young T, Palta M, Dempsey J, Skatrud J (2000) Longitudinal study of moderate weight change and sleep-disordered breathing. JAMA 284(23):3015–3021
Farah CS, Salome CM (2010) Asthma and obesity: a known association but unknown mechanism. Respirology 17:412–421
Mosen DM, Schatz M, Magid DJ, Camargo CA Jr (2008) The relationship between obesity and asthma severity and control in adults. J Allergy Clin Immunol 122:507–511
Taylor B, Mannino D, Brown C, Crocker D, Twum-Baah N, Holguin F (2008) Body mass index and asthma severity in the National Asthma Survey. Thorax 63:14–20
Vortmann M, Eisner MD (2008) BMI and health status among adults with asthma. Obesity 16:146–152
Julien JY, Martin JG, Ernst P, Olivenstein R, Hamid Q, Lemière C, Pepe C, Naor N, Olha A, Kimoff RJ (2009) Prevalence of obstructive sleep apnea-hypopnea in severe versus moderate asthma. J Allergy Clin Immunol 124:371–376
Teodorescu M, Polomis DA, Hall SV, Teodorescu MC, Gangnon RE, Peterson AG, Xie A, Sorkness CA, Jarjour NN (2010) Association of obstructive sleep apnea risk with asthma control in adults. Chest 138:543–550
Alkhalil M, Schulman E, Getsy J (2009) Obstructive sleep apnea syndrome and asthma: what are the links? J Clin Sleep Med 5(1):71–79
Alkhalil M, Schulman ES, Getsy J (2008) Obstructive sleep apnea syndrome and asthma: the role of continuous positive airway pressure treatment. Ann Allergy Asthma Immunol 101:350–357
Lafond C, Sériè F, Lemière C (2007) Impact of CPAP on asthmatic patients with obstructive sleep apnea. Eur Respir J 29:307–311
Ciftci TU, Ciftci B, Guven SF, Kokturk O, Turktas H (2005) Effect of nasal continuous positive airway pressure in uncontrolled nocturnal asthmatic patients with obstructive sleep apnea syndrome. Respir Med 99(5):529–534
Chan CS, Woolcock AJ, Sullivan CE (1988) Nocturnal asthma: role of snoring and obstructive sleep apnea. Am Rev Respir Dis 137:1502–1504
Martin JM, Carrizo SJ, Vicente E, Agusti AG (2005) Long-term cardiovascular outcomes in me with obstructive sleep apnea-hypopnea with or without treatment with continuous positive airway pressure: an observational study. Lancet 365:1046–1053
Arzt M, Young T, Finn L, Skatrud JB, Bradley TD (2005) Association of sleep-disordered breathing and the occurrence of stroke. Am J Repir Crit Care Med 172:1447–1451
Yaggi HK, Concato J, Keman WN, Lichtman JH, Brass LM, Mohsenin V (2005) Obstructive sleep apnea as a risk factor for stroke and death. N Engl J Med 535:2034–2041
Peker Y, Hedner J, Norum J, Kraiczi H, Carlson J (2002) Increased incidence of cardiovascular disease in middle-aged men with obstructive sleep apnea: a 7-year follow up. Am J Repir Crit Care Med 166:159–165
Shahar E, Whitney CW, Redline S, Lee ET, Newman AB, Javier NF, O’Connor GT, Boland LL, Schwartz JE, Samet JM (2001) Sleep-disordered breathing and cardiovascular disease: cross-sectional results of the Sleep Heart Health study. Am J Repir Crit Care Med 163:19–25
Minoguchi K, Yokoe T, Tazaki T, Minoguchi H, Oda N, Tanaka A, Yamamoto Y, Ohta S, O’Donnell CP, Adachi M (2007) Silent brain infarction and platelet activation in obstructive sleep apnea. Am J Repir Crit Care Med 175:612–617
Ryan S, Taylor CT, McNicholas WT (2005) Selective activation of inflammatory pathways by intermittent hypoxia in obstructive sleep apnea syndrome. Circulation 112:2660–2667
Hansson GK, Libby P (2006) The immune response in atherosclerosis: a double-edged sword. Nat Rev Immunol 6:508–519
Tedgui A, Mallat Z (2006) Cytokines in atherosclerosis: pathogenic and regulatory pathways. Physiol Rev 86:515–581
Nadeem R, Molnar J, Madbouly EM, Nida M, Aggarwal S, Sajid H, Naseem J, Loomba R (2013) Serum inflammatory markers in obstructive sleep apnea: a meta-analysis. J Clin Sleep Med 9(10):1003–1012
Minoguchi K, Yokoe T, Tazaki T, Minoguchi H, Tanaka A, Oda N, Okada S, Ohta S, Naito H, Adachi M (2005) Increased carotid intima-media thickness and serum inflammatory markers in obstructive sleep apnea. Am J Repir Crit Care Med 172:625–630
Arnaud C, Beguin PC, Lantuejoul S, Pépin JL, Guillermet C, Pelli G, Burger F, Buatois V, Ribuot C, Baguet JP, Mach F, Lévy P, Dematteis M (2011) The inflammatory preatherosclerotic remodeling induced by intermittent hypoxia is attenuated by RANTES/CCL5 inhibition. Am J Respir Crit Care Med 184:724–731
Stanke-Labesque F, Bäck M, Lefebvre B, Tamisier R, Baguet JP, Arnol N, Lévy P, Pépin JL (2009) Increased urinary leukotriene B4 excretion in obstructive sleep apnea: effects of obesity and hypoxia. J Allergy Clin Immunol 124:364–370
Lefebvre B, Pépin JL, Baguet JP, Roustit M, Riedweg K, Bessard G, Lévy P, Stanke-Labesque F (2008) Leukotriene B4: early mediator of atherosclerosis in obstructive sleep apnea? Eur Respir J 32:113–120
Gautier-Veyret E, Arnoud C, Bäck M, Pépin JL, Petri MH, Baguet JP, Tamisier R, Lévy P, Stanke-Labesque F (2013) Intermittent hypoxia-activated cyclooxygenase pathway: role in atherosclerosis. Eur Respir J 42:404–413
Yokoe T, Alonso LC, Romano LC, Rosa TC, O’Doherty RM, Garcia-Ocana A, Minoguchi K, O’Donnell CP (2008) Intermittent hypoxia reverses the diurnal glucose rhythm and causes pancreatic β-cell replication in mice. J Physiol 586:899–911
Myou S, Leff AR, Myo S, Boetticher E, Tong J, Meliton AY, Liu J, Munoz NM, Zhu X (2003) Blockade of inflammation and airway hyperresponsiveness in immune-sensitized mice by dominant-negative phosphoinositide 3-kinase-TAT. J Exp Med 198(10):1573–1582
Ohta S, Oda N, Yokoe T, Yamamoto Y, Watanabe Y, Minoguchi K, Ohnishi T, Hirose T, Nagase H, Ohta K, Adachi M (2010) Effect of tiotropium bromide on airway inflammation and remodeling in a mouse model of asthma. Clin Exp Allergy 40:1266–1275
Yamashita N, Sekine K, Miyasaka T, Kawashima R, Nakajima Y, Nakano J, Yamamoto T, Horiuchi T, Hirai K, Ohta K (2001) Platelet-derived growth factor is involved in the augmentation of airway responsiveness through remodeling of airways in diesel exhaust particulate-treated mice. J Allergy Clin Immunol 107:135–142
Broytman O, Braun RK, Morgan BJ, Pegelow DF, Hsu PN, Mei LS, Koya AK, Eldridge M, Teodorescu M (2015) Effects of chronic intermittent hypoxia on allergen-induced airway inflammation in rats. Am J Respir Cell Mol Biol 52(2):162–170
Drager LF, Yao Q, Hernandez KL, Shin MK, Bevans-Fonti S, Gay J (2013) Chronic intermittent hypoxia induces atherosclerosis via activation of adipose-angiopoietin-like 4. Am J Respir Crit Care Med 188(2):240–248
Dumitrascu R, Heitmann J, Seeger W, Weissmann N, Schulz R (2013) Obstructive sleep apnea, oxidative stress and cardiovascular disease: lessons from animal studies. Eur Respir J 42(2):404–413
Quercioli A, Mach F, Montecucco F (2010) Inflammation accelerates atherosclerotic processes in obstructive sleep apnea syndrome (OSAS). Sleep Breath 14(3):261–269
Jun J, Savransky V, Nanayakkara A, Bevans S, Li J, Smith PL, Polotsky VY (2008) Intermittent hypoxia has organ-specific effects on oxidative stress. Am J Physiol Regul Integr Comp Physiol 295(4):1274–1281
Raghuraman G, Rai V, Peng YJ, Prabhakar NR, Kumar GK (2009) Pattern-specific sustained activation of tyrosine hydroxylase by intermittent hypoxia: role of reactive oxygen species-dependent downregulation of protein phosphatase 2A and upregulation of protein kinases. Antioxid Redox Signal 11(8):1777–1789
Acknowledgments
We would like to thank Kyoko Inui and Manami Matsuda for their skillful technical assistance. We would also like to thank Editage (www.editage.jp) for English language editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All applicable international, national, and institutional guidelines for the care and use of animals were followed. This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ohta, S., Tanaka, A., Jinno, M. et al. Exposure to intermittent hypoxia inhibits allergic airway inflammation in a murine model of asthma. Sleep Breath 24, 523–532 (2020). https://doi.org/10.1007/s11325-019-01892-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-019-01892-6