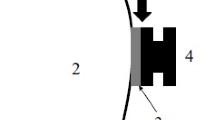
The aim of this study was to investigate the magnitude of debonding stress of an orthodontic bracket bonded to the enamel with resin systems having different elastic properties. For the same purpose, sixty human premolars were randomly divided into four groups according to the adhesive system used for bonding brackets: G Fix flowable resin (GFI) with Everstick NET (ESN), GFI, G Aenial Universal Flow (GAU) with ESN, and GAU. The brackets were stressed in the occlusogingival direction on a universal testing machine. The values of debonding load and displacement were determined at the point of debonding. The elastic modulus of the tested materials was determined using nanoindentation. An analysis of variance showed a significant difference in the loads required to debond the bracket among the groups tested. The GAU group had the highest elastic modulus, followed by the GFI and ESN groups. ARI (Adhesive Remnant Index) scores demonstrated more remnants of the adhesive material on the bracket surface with adhesives having a higher elastic modulus. Taking into consideration results of the present in-vitro study, it can be concluded that the incorporation of a glass-fiber-reinforced composite resin (FRC) with a low elastic modulus between the orthodontic bracket and enamel increases the debonding force and strain more than with adhesive systems having a higher elastic modulus.




Similar content being viewed by others
References
M. Ekambaram, C. K. Y. Yiu, and J. P. Matinlinna, “An overview of solvents in resin–dentin bonding,” Int. J. of Adhesion and Adhesives, 57, 22-33 (2015).
S. E. Bishara, et al., “Comparison of the shear bond strength of 2 self-etch primer/adhesive systems,” Am. J. Orthod Dentofacial Orthop., 125, No. 3, 348-350 (2004).
M. Peumans, et al., “Clinical effectiveness of contemporary adhesives: a systematic review of current clinical trials,” Dent. Mater., 21, No. 9, 864-881 (2005).
D. B. Ryou, et al., “Use of flowable composites for orthodontic bracket bonding,” Angle Orthod., 78, No. 6, 1105-1109 (2008).
M. D’Attilio, et al., “Shear bond strength, bond failure, and scanning electron microscopy analysis of a new flowable composite for orthodontic use,” Angle Orthod., 75, No. 3, 410-415 (2005).
S. Tecco, et al., “A new one-step dental flowable composite for orthodontic use: an in vitro bond strength study,” Angle Orthod., 75, No. 4, 672-677 (2005).
T. R. Katona, “Stresses developed during clinical debonding of stainless steel orthodontic brackets,” The Angle Orthodontist, 67, No. 1, 39-46 (1997).
S. Bouillaguet, et al., “Hydrothermal and mechanical stresses degrade fiber-matrix interfacial bond strength in dental fiber-reinforced composites,” J. Biomed. Mater. Res. B, Appl. Biomater., 76, No. 1, 98-105 (2006).
P. K. Vallittu, “Comparison of two different silane compounds used for improving adhesion between fibres and acrylic denture base material,” J. Oral. Rehabil., 20, No. 5), 533-539 (1993).
Y. K. Lung and J. P. Matinlinna, “Silanes for adhesion promotion and surface modification,” in Silane: Chemistry, Applications and Performance, 2013, Nova Sci Publ.: Hauppauge. p. 87.
S. Garoushi, P. K. Vallittu, and L. V. J. Lassila, “Use of short fiber-reinforced composite with semi-interpenetrating polymer network matrix in fixed partial dentures,” J. Dent., 35,No. 5, 403-408 (2007).
D. C. Smith, “Recent developments and prospects in dental polymers,” J. Prosthet. Dent., 12, No. 6, 1066-1078 (1962).
P. K. Vallittu, “Compositional and weave pattern analyses of glass fibers in dental polymer fiber composites,” J. Prosthodont, 7, No. 3, 170-176 (1998).
T. J. Nohrstrom, P. K. Vallittu, and A. Yli-Urpo, “The effect of placement and quantity of glass fibers on the fracture resistance of interim fixed partial dentures,” Int. J. Prosthodont, 13, No. 1, 72-78 (2000).
K. H. Chong and J. Chai, “Strength and mode of failure of unidirectional and bidirectional glass fiber-reinforced composite materials,” Int. J. Prosthodont, 16, No. 2, 161-166 (2003).
D. Edelhoff, H. Spiekermann, and M. Yildirim, “Metal-free inlay-retained fixed partial dentures,” Quintessence Int., 32, No. 4, 269-281 (2001).
T. N. Gohring, P. R. Schmidlin, and F. Lutz, “Two-year clinical and SEM evaluation of glass-fiber-reinforced inlay fixed partial dentures.” Am. J. Dent., 15, No. 1, 35-40 (2002).
C. Kolbeck, et al., “In vitro examination of the fracture strength of 3 different fiber-reinforced composite and 1 allceramic posterior inlay fixed partial denture systems,” J. Prosthodont., 11, No. 4, 248-253 (2002).
C. Monaco, et al., “Clinical evaluation of fiber-reinforced composite inlay FPDs,” Int. J. Prosthodont., 16, No. 3, 319-325 (2003).
Petersen, R.C., Discontinuous fiber-reinforced composites above critical length. J. Dent. Res., 84, No. 4, 365-370 (2005).
P. Valyi, et al., “Effect of occlusal therapy with FRC splint on periodontal parameters in maintenance phase,” Fogorv Sz, 98,No. 4, 159-163 (2005).
V. Cacciafesta, et al., “Flexural strengths of fiber-reinforced composites polymerized with conventional light-curing and additional postcuring,” Am. J. Orthod. Dentofacial Orthop., 132, No. 4, 524-527 (2007).
A. Scribante, V. Cacciafesta, and M. F. Sfondrini, “Effect of various adhesive systems on the shear bond strength of fiber-reinforced composite,” Am. J. Orthod. Dentofacial Orthop., 130, No. 2, 224-227 (2006).
T. M. Lastumaki, T. T. Kallio, and P. K. Vallittu, “The bond strength of light-curing composite resin to finally polymerized and aged glass fiber-reinforced composite substrate.” Biomaterials, 23, No. 23, 4533-4539 (2002).
P. K. Vallittu, “Interpenetrating polymer Networks (IPNs) in dental polymers and composites,” J. of Adhesion Sci. and Technol., 23, No. 7-8, 961-972 (2009).
J. Artun and S. Bergland, “Clinical trials with crystal growth conditioning as an alternative to acid-etch enamel pretreatment,” Am. J. Orthod., 85, No. 4, 333-340 (1984).
B. Pick, et al., “Are flowable resin-based composites a reliable material for metal orthodontic bracket bonding?” J. Contemp. Dent. Pract., 11, No. 4, E017-E024 (2010).
M. Shinya, et al., “Enhanced degree of monomer conversion of orthodontic adhesives using a glass-fiber layer under the bracket,” Angle Orthod., 79, No. 3, 546-550 (2009).
G. V. Newman, et al., “Adhesion promoters, their effect on the bond strength of metal brackets,” Am. J. Orthod. Dentofacial Orthop., 108, No. 3, 237-241 (1995).
R. M., Carvalho, et al., “Effects of prism orientation on tensile strength of enamel,” J. Adhes. Dent., 2, No. 4, 251-257 (2000).
I. R., Reynolds, “A review of direct orthodontic bonding,” Br. J. Orthodont., 2, 171-178 (1975).
M. D. Turgut, et al., “Comparison of shear bond strengths of orthodontic brackets bonded with flowable composites,” Dent. Mater. J., 30, No. 1, 66-71 (2011).
Acknowledgments
The project was financially supported by the Vice Deanship of Research Chairs, King Saud University. The investigation was carried out at the Turku Clinical Biomaterials Centre-TCBC, Institute of Dentistry, University of Turku, Finland and Dental Biomaterials Research Chair, College of Applied Medical Sciences, King Saud University, Riyadh, Saudi Arabia.
Author information
Authors and Affiliations
Corresponding author
Additional information
Russian translation published in Mekhanika Kompozitnykh Materialov, Vol. 51, No. 6, pp. 1141-1154 , November-December, 2015.
Rights and permissions
About this article
Cite this article
Durgesh, B.H., Alkheraif, A.A., Al Sharawy, M. et al. Damage of the Interface Between an Orthodontic Bracket and Enamel – the Effect of Some Elastic Properties of the Adhesive Material. Mech Compos Mater 51, 805–812 (2016). https://doi.org/10.1007/s11029-016-9551-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11029-016-9551-x