Abstract
Internet-based cognitive behavioral therapy (iCBT), provided with guidance, has been shown to outperform wait-list control conditions and appears to perform on par with face-to-face psychotherapy. However, dropout remains an important problem. Dropout rates for iCBT programs for depression have ranged from 0 to 75%, with a mean of 32%. Drawing from a recent study in which 117 people participated in iCBT with support, we examined participant characteristics, participants’ use of iCBT skills, and their experience of technical difficulties with iCBT as predictors of dropout risk. Educational level, extraversion, and participant skill use predicted lower risk of dropout; technical difficulties and openness predicted higher dropout risk. We encourage future research on predictors of dropout in the hope that greater understanding of dropout risk will inform efforts to promote program engagement and retention.
Similar content being viewed by others
Data Availability
Pending IRB approval for sharing, the dataset described in this paper is available from the corresponding author on reasonable request.
Notes
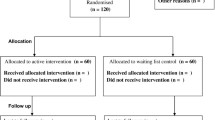
Dropout rates across study segments were: 39% (23 of 59) among those randomized to BtB, 65% (13 of 20) among those randomized to wait-list and subsequently offered BtB, and 45% (17 of 38) among non-randomized participants offered BtB. The 20 participants who had initially been assigned to wait-list were a subset of a larger group of 30, as 10 opted to not continue participation. An initial test suggested that study segment was associated with differential dropout risk (RR = 1.67; 95% CI 1.06–2.62, p = 0.03). However, study segment failed to predict dropout in our multivariate model (see Table 4).
We included the number of contacts as a covariate out of concern for the possibility that our measure of CBT skills could have been confounded with clients who had more contact with their coach and thus more opportunities to convey their use of CBT skills. There was an average of 2.6 (SD = 1.54; range = 0–9) calls completed between participants and their coaches and an average of 5.05 (SD = 2.72; range 0–12) emails exchanged between participants and their coaches.
References
Andersson, G., & Cuijpers, P. (2009). Internet-based and other computerized psychological treatments for adult depression: A meta-analysis. Cognitive Behaviour Therapy, 38, 196–205. https://doi.org/10.1080/16506070903318960.
Andersson, G., Hesser, H., Veilord, A., Svedling, L., Andersson, F., Sleman, O., et al. (2013). Randomised controlled non-inferiority trial with 3-year follow-up of internet-delivered versus face-to-face group cognitive behavioural therapy for depression. Journal of Affective Disorders, 151, 986–994. https://doi.org/10.1016/j.jad.2013.08.022.
Andrews, G., Cuijpers, P., Craske, M. G., McEvoy, P., & Titov, N. (2010). Computer therapy for the anxiety and depressive disorders is effective, acceptable and practical health care: A meta-analysis. PLoS ONE, 5, e13196. https://doi.org/10.1371/journal.pone.0013196.
Bagby, R. M., Quilty, L. C., Segal, Z. V., McBride, C. C., Kennedy, S. H., & Costa, P. T. (2008). Personality and differential treatment response in major depression: A randomized controlled trial comparing cognitive-behavioural therapy and pharmacotherapy. Canadian Journal of Psychiatry, 53, 361–370. https://doi.org/10.1177/070674370805300605.
Benet-Martinez, V., & John, O. P. (1998). Los Cinco Grandes across cultures and ethnic groups: Multitrait-multimethod analyses of the Big Five in Spanish and English. Journal of Personality and Social Psychology, 75, 729–750. https://doi.org/10.1037/0022-3514.75.3.729.
Cohen, P., Cohen, J., Aiken, L. S., & West, S. G. (1999). The problem of units and the circumstance for POMP. Multivariate Behavioral Research, 34, 315–346. https://doi.org/10.1207/S15327906MBR3403_2.
Cuijpers, P., Donker, T., van Straten, A., Li, J., & Andersson, G. (2010). Is guided self-help as effective as face-to-face psychotherapy for depression and anxiety disorders? A systematic review and meta-analysis of comparative outcome studies. Psychological Medicine, 40, 1943–1957. https://doi.org/10.1017/S0033291710000772.
Davidson, K. W., Kupfer, D. J., Bigger, J. T., Califf, R. M., Carney, R. M., Coyne, J. C., et al. (2006). Assessment and treatment of depression in patients with cardiovascular disease: National Heart, Lung, and Blood Institute Working Group Report. Psychosomatic Medicine, 68, 645–650. https://doi.org/10.1097/01.psy.0000233233.48738.22.
DeRubeis, R. J., Cohen, Z. D., Forand, N. R., Fournier, J. C., Gelfand, L. A., & Lorenzo-Luaces, L. (2014). The Personalized Advantage Index: Translating research on prediction into individualized treatment recommendations. A demonstration. PLoS ONE, 9, e83875.
Duffecy, J., Kinsinger, S., Ludman, E., & Mohr, D. C. (2011). Brief telephone support program to enhance patient adherence to Technology Assisted Behavioral Interventions (TABIs): Therapist manual. Unpublished Manuscript.
Forand, N. R., Barnett, J. G., Strunk, D. R., Hindiyeh, M. U., Feinberg, J. E., & Keefe, J. R. (2017). Efficacy of guided iCBT for depression and mediation of change by CBT skill acquisition. Behavior Therapy, 42, 612–623. https://doi.org/10.1016/j.beth.2017.04.004.
Gellatly, J., Bower, P., Hennessy, S., Richards, D., Gilbody, S., & Lovell, K. (2007). What makes self-help interventions effective in the management of depressive symptoms? Meta-analysis and meta-regression. Psychological Medicine., 37, 1217–1228. https://doi.org/10.1017/S0033291707000062.
Hosmer, D. W., Lemeshow, S., & Sturdivant, R. X. (2013). Sample size issues when fitting logistic regression models. In D. W. Hosmer (Ed.), Applied logistic regression (3rd edn., pp. 347–399). New York: Wiley-International Publication.
Hundt, N. E., Mignogna, J., Underhill, C., & Cully, J. A. (2013). The relationship between use of CBT skills and depression treatment outcome: A theoretical and methodological review of the literature. Behavior Therapy, 44, 12–26. https://doi.org/10.1016/j.beth.2012.10.001.
Jarrett, R. B., Minhajuddin, A., Kangas, J. L., Friedman, E. S., Callan, J. A., & Thase, M. E. (2013). Acute phase cognitive therapy for recurrent major depressive disorder: Who drops out and how much do patient skills influence response? Behaviour Research and Therapy, 51, 221–230. https://doi.org/10.1016/j.brat.2013.01.006.
Jarrett, R. B., Vittengl, J. R., Clark, L. A., & Thase, M. E. (2011). Skills of Cognitive Therapy (SoCT): A new measure of patients’ comprehension and use. Psychological Assessment, 23, 578–586. https://doi.org/10.1037/a0022485.
Johansson, R., & Andersson, G. (2012). Internet-based psychological treatments for depression. Expert Review of Neurotherapeutics, 12, 861–869. https://doi.org/10.7717/peerj.178.
John, O. P., Donahue, E. M., & Kentle, R. L. (1991). The Big Five Inventory—Versions 4a and 54. Berkeley: University of California, Berkeley, Institute of Personality and Social Research.
John, O. P., & Srivastava, S. (1999). The Big-Five trait taxonomy: History, measurement, and theoretical perspectives. In L. A. Pervin & O. P. John (Eds.), Handbook of personality: Theory and research (pp. 78–80). New York: Guilford Press.
Kaltenthaler, E., Sutcliffe, P., Parry, G., Beverley, C., Rees, A., & Ferriter, M. (2008). The acceptability to patients of computerized cognitive behaviour therapy for depression: A systematic review. Psychological Medicine, 38, 1521–1530. https://doi.org/10.1017/S0033291707002607.
Karyotaki, E., Kleiboer, A., Smit, F., Turner, D. T., Pastor, A. M., Andersson, G., et al. (2015). Predictors of treatment dropout in self-guided web-based interventions for depression: An ‘individual patient data meta-analysis. Psychological Medicine, 45, 2717–2726. https://doi.org/10.1017/S0033291715000665.
Klein, D. N., Kotov, R., & Bufferd, S. J. (2011). Personality and depression: Explanatory models and review of the evidence. Annual Review of Clinical Psychology, 7, 269–295. https://doi.org/10.1146/annurev-clinpsy-032210-104540.
Knowles, S. E., Toms, G., Sanders, C., Bee, P., Lovell, K., Rennick-Egglestone, S., et al. (2014). Qualitative meta-synthesis of user experience of computerised therapy for depression and anxiety. PLoS ONE, 9, e84323. https://doi.org/10.1371/journal.pone.0084323.
Kroenke, K., Spitzer, R. L., & Williams, J. B. (2001). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine, 16, 606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x.
Lutz, W., Schwartz, B., Hofmann, S. G., Fisher, A. J., Husen, K., & Rubel, J. A. (2018). Using network analysis for the prediction of treatment dropout in patients with mood and anxiety disorders: A methodological proof-of-concept study. Scientific Reports, 8, 7819. https://doi.org/10.1038/s41598-018-25953-0.
McGraw, K. O., & Wong, S. P. (1996). Forming inferences about some intraclass correlation coefficients. Psychological Methods, 1, 30–46. https://doi.org/10.1037/1082-989X.1.1.30.
Mohr, D. C., Cuijpers, P., & Lehman, K. (2011). Supportive accountability: A model for providing human support to enhance adherence to eHealth interventions. Journal of Medical Internet Research, 13, e30. https://doi.org/10.2196/jmir.1602.
Mohr, D. C., Duffecy, J., Ho, J., Kwasny, M., Cai, X., Burns, M. N., & Begale, M. (2013). A randomized controlled trial evaluating a manualized TeleCoaching protocol for improving adherence to a web-based intervention for the treatment of depression. PLoS ONE, 8, e70086. https://doi.org/10.1371/journal.pone.0070086.
Mohr, D. C., Tomasino, K. N., Lattie, E. G., Palac, H. L., Kwasny, M. J., Weingardt, K., et al. (2017). IntelliCare: An eclectic, skills-based app suite for the treatment of depression and anxiety. Journal of Medical Internet Research, 19, e10. https://doi.org/10.2196/jmir.6645.
Proudfoot, J., Goldberg, D., Mann, A., Everitt, B., Marks, I., & Gray, J. A. (2003). Computerized, interactive, multimedia cognitive-behavioural program for anxiety and depression in general practice. Psychological Medicine, 33, 217–227. https://doi.org/10.1192/bjp.185.1.46.
Proudfoot, J., Ryden, C., Everitt, B., Shapiro, D. A., Goldberg, D., Mann, A., et al. Gray, J. A. (2004). Clinical efficacy of computerised cognitive–behavioural therapy for anxiety and depression in primary care: Randomised controlled trial. The British Journal of Psychiatry, 185, 46–54. https://doi.org/10.1192/bjp.185.1.46.
Quilty, L. C., De Fruyt, F., Rolland, J.-P., Kennedy, S. H., Rouillon, P. F., & Bagby, R. M. (2008). Dimensional personality traits and treatment outcome in patients with major depressive disorder. Journal of Affective Disorders, 108, 241–250. https://doi.org/10.1016/j.jad.2007.10.022.
Richards, D., & Richardson, T. (2012). Computer-based psychological treatments for depression: A systematic review and meta-analysis. Clinical Psychology Review, 32, 329–342. https://doi.org/10.1016/j.cpr.2012.02.004.
Sasso, K. E., & Strunk, D. R. (2013). Thin slice ratings of client characteristics in intake assessments: Predicting symptom change and dropout in cognitive therapy for depression. Behaviour Research and Therapy, 51, 443–450. https://doi.org/10.1016/j.brat.2013.04.007.
Sheehan, D. V., Lecrubier, Y., Sheehan, K. H., Amorim, P., Janavs, J., Weiller, E., et al. (1998). The Mini-International Neuropsychiatric Interview (M.I.N.I.): The development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. The Journal of Clinical Psychiatry, 59(Suppl 20), 22–33.
Shipley, W. C. (1940). A self-administering scale for measuring intellectual impairment and deterioration. Journal of Psychology: Interdisciplinary and Applied, 9, 371–377. https://doi.org/10.1080/00223980.1940.9917704.
Spek, V., Nyklícek, I., Smits, N., Cuijpers, P., Riper, H., Keyzer, J., & Pop, V. (2007). Internet-based cognitive behavioural therapy for subthreshold depression in people over 50 years old: A randomized controlled clinical trial. Psychological Medicine, 37, 1797–1806. https://doi.org/10.1017/S0033291707000542.
Srivastava, S., John, O. P., Gosling, S. D., & Potter, J. (2003). Development of personality in early and middle adulthood: Set like plaster or persistent change? Journal of Personality and Social Psychology, 84, 1041–1053. https://doi.org/10.1037/0022-3514.84.5.1041.
Strunk, D. R., DeRubeis, R. J., Chui, A., & Alvarez, J. A. (2007). Patients’ competence in and performance of cognitive therapy skills: Relation to the reduction of relapse risk following treatment for depression. Journal of Consulting and Clinical Psychology, 75, 523–530. https://doi.org/10.1037/0022-006X.75.4.523.
Swift, J. K., & Greenberg, R. P. (2012). Premature discontinuation in adult psychotherapy: A meta-analysis. Journal of Consulting and Clinical Psychology, 80, 547–559. https://doi.org/10.1037/a0028226.
Thombs, B. D., & Ziegelstein, R. C. (2014). Does depression screening improve depression outcomes in primary care? BMJ (Clinical Research Ed.). 348. g1253.
Wagner, B., Horn, A. B., & Maercker, A. (2014). Internet-based versus face-to-face cognitive-behavioral intervention for depression: A randomized controlled non-inferiority trial. Journal of Affective Disorders, 152, 113–121. https://doi.org/10.1016/j.jad.2013.06.032.
Waller, R., & Gilbody, S. (2009). Barriers to the uptake of computerized cognitive behavioural therapy: A systematic review of the quantitative and qualitative evidence. Psychological Medicine, 39, 705–712. https://doi.org/10.1017/S0033291708004224.
Warmerdam, L., van Straten, A., Twisk, J., Riper, H., & Cuijpers, P. (2008). Internet-based treatment for adults with depressive symptoms: Randomized controlled trial. Journal of Medical Internet Research, 10, e44. https://doi.org/10.2196/jmir.1094.
Wright, J. H., Wright, A. S., Albano, A. M., Basco, M. R., Goldsmith, L. J., Raffield, T., & Otto, M. W. (2005). Computer-assisted cognitive therapy for depression: Maintaining efficacy while reducing therapist time. The American Journal of Psychiatry, 162, 1158–1164. https://doi.org/10.1176/appi.ajp.162.6.1158.
Zilcha-Mano, S., Keefe, J. R., Chui, H., Rubin, A., Barrett, M. S., & Barber, J. P. (2016). Reducing dropout in treatment for depression: Translating dropout predictors into individualized treatment recommendations. The Journal of Clinical Psychiatry, 77, e1584–e1590. https://doi.org/10.4088/JCP.15m10081.
Zou, G. (2004). A modified Poisson regression approach to prospective studies with binary data. American Journal of Epidemiology, 159, 702–706. https://doi.org/10.1093/aje/kwh090.
Funding
This study was funded in part by the National Center for Advancing Translational Sciences Award Number Grant KL2TR001068, awarded to NRF. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Center for Advancing Translational Sciences or the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Iony D. Schmidt, Nicholas R. Forand, and Daniel R. Strunk declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Schmidt, I.D., Forand, N.R. & Strunk, D.R. Predictors of Dropout in Internet-Based Cognitive Behavioral Therapy for Depression. Cogn Ther Res 43, 620–630 (2019). https://doi.org/10.1007/s10608-018-9979-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10608-018-9979-5