Abstract
Purpose
We conducted a meta-analysis to systematically assess the prospective association between vitamin K and cardiovascular disease (CVD) events and all-cause mortality.
Methods
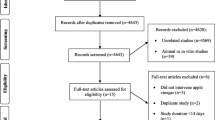
We searched PubMed and EMBASE through January 2019 for prospective studies that reported the association of vitamin K (assessed by dietary intake or circulating concentration) with CVD events [including total CVD, CVD mortality, total coronary heart disease (CHD), fatal CHD, nonfatal myocardial infarction (MI), and stroke] and all-cause mortality. Multivariable-adjusted hazard ratios (HRs) comparing top versus bottom tertiles of vitamin K were combined using random-effects meta-analysis.
Results
Twenty-one articles were included with 222,592 participants. A significant association was found between dietary phylloquinone and total CHD (pooled HR 0.92; 95% CI 0.84, 0.99; I2 = 0%; four studies), as well as menaquinone and total CHD (0.70; 95% CI 0.53, 0.93; I2 = 32.1%; two studies). No significant association was observed between dietary vitamin K and all-cause mortality, CVD mortality, or stroke. Elevated plasma desphospho-uncarboxylated MGP (dp-ucMGP), a marker of vitamin K deficiency, was associated with an increased risk of all-cause mortality (1.84; 95% CI 1.48, 2.28; I2 = 16.8%; five studies) and CVD mortality (1.96; 95% CI 1.47, 2.61; I2 = 0%; two studies). No significant association was observed between circulating total osteocalcin and all-cause mortality or total CVD.
Conclusions
Our findings showed that higher dietary vitamin K consumption was associated with a moderately lower risk of CHD, and higher plasma dp-ucMGP concentration, but not total circulating osteocalcin, was associated with increased risks of all-cause and CVD mortality. However, causal relations cannot be established because of limited number of available studies, and larger prospective studies and randomized clinical trials are needed to validate the findings.






Similar content being viewed by others
References
GBD 2016 Disease and Injury Incidence and Prevalence Collaborators (2017) Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet 390(10100):1211–1259. https://doi.org/10.1016/S0140-6736(17)32154-2
Pan A, Lin X, Hemler E, Hu FB (2018) Diet and cardiovascular disease: advances and challenges in population-based studies. Cell Metab 27(3):489–496. https://doi.org/10.1016/j.cmet.2018.02.017
Du H, Li L, Bennett D, Guo Y, Key TJ, Bian Z, Sherliker P, Gao H, Chen Y, Yang L, Chen J, Wang S, Du R, Su H, Collins R, Peto R, Chen Z, China Kadoorie Biobank S (2016) Fresh fruit consumption and major cardiovascular disease in China. N Engl J Med 374(14):1332–1343. https://doi.org/10.1056/NEJMoa1501451
Wang X, Ouyang Y, Liu J, Zhu M, Zhao G, Bao W, Hu FB (2014) Fruit and vegetable consumption and mortality from all causes, cardiovascular disease, and cancer: systematic review and dose-response meta-analysis of prospective cohort studies. BMJ 349:g4490. https://doi.org/10.1136/bmj.g4490
Scarborough P, Morgan R, Webster P, Rayner M (2011) Differences in coronary heart disease, stroke and cancer mortality rates between England, Wales, Scotland and Northern Ireland: the role of diet and nutrition. BMJ Open 1(1):e000263. https://doi.org/10.1136/bmjopen-2011-000263
Schurgers LJ, Vermeer C (2000) Determination of phylloquinone and menaquinones in food. Effect of food matrix on circulating vitamin K concentrations. Haemostasis 30(6):298–307. https://doi.org/10.1159/000054147
Shearer MJ (1995) Vitamin K. Lancet 345(8944):229–234
Furie B, Bouchard BA, Furie BC (1999) Vitamin K-dependent biosynthesis of gamma-carboxyglutamic acid. Blood 93(6):1798–1808
Dalmeijer GW, van der Schouw YT, Vermeer C, Magdeleyns EJ, Schurgers LJ, Beulens JWJ (2013) Circulating matrix Gla protein is associated with coronary artery calcification and vitamin K status in healthy women. J Nutr Biochem 24(4):624–628. https://doi.org/10.1016/j.jnutbio.2012.02.012
Shea MK, Booth SL (2016) Concepts and controversies in evaluating vitamin K status in population-based studies. Nutrients 8:8. https://doi.org/10.3390/nu8010008
Cranenburg EC, Koos R, Schurgers LJ, Magdeleyns EJ, Schoonbrood TH, Landewe RB, Brandenburg VM, Bekers O, Vermeer C (2010) Characterisation and potential diagnostic value of circulating matrix Gla protein (MGP) species. Thromb Haemost 104(4):811–822. https://doi.org/10.1160/TH09-11-0786
Rees K, Guraewal S, Wong YL, Majanbu DL, Mavrodaris A, Stranges S, Kandala NB, Clarke A, Franco OH (2010) Is vitamin K consumption associated with cardio-metabolic disorders? A systematic review. Maturitas 67(2):121–128. https://doi.org/10.1016/j.maturitas.2010.05.006
Hartley L, Clar C, Ghannam O, Flowers N, Stranges S, Rees K (2015) Vitamin K for the primary prevention of cardiovascular disease. Cochrane Database Syst Rev 9:CD011148. https://doi.org/10.1002/14651858.CD011148.pub2
Harshman SG, Shea MK (2016) The role of vitamin K in chronic aging diseases: inflammation, cardiovascular disease, and osteoarthritis. Curr Nutr Rep 5(2):90–98. https://doi.org/10.1007/s13668-016-0162-x
Zhang S, Guo L, Bu C (2019) Vitamin K status and cardiovascular events or mortality: a meta-analysis. Eur J Prev Cardiol 26:549–553. https://doi.org/10.1177/2047487318808066
Moher D, Liberati A, Tetzlaff J, Altman D (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P (2012) The Newcastle-Ottawa Scale (NOS) for assessing the quality if nonrandomized studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (cited 1 June 2018)
Danesh J, Collins R, Appleby P, Peto R (1998) Association of fibrinogen, C-reactive protein, albumin, or leukocyte count with coronary heart disease: meta-analyses of prospective studies. JAMA 279(18):1477–1482. https://doi.org/10.1001/jama.279.18.1477
Chêne G, Thompson SG (1996) Methods for summarizing the risk associations of quantitative variables in epidemiologic studies in a consistent form. Am J Epidemiol 144(6):610–621. https://doi.org/10.1093/oxfordjournals.aje.a008971
Combettes E, Mazoit JX, Benhamou D, Beloeil H (2015) Modelling of vitamin K half-life in patients treated with vitamin K antagonists before hip fracture surgery. Anaesth Crit Care Pain Med 34(5):295–299. https://doi.org/10.1016/j.accpm.2015.06.003
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Geleijnse JM, Vermeer C, Grobbee DE, Schurgers LJ, Knapen MH, van der Meer IM, Hofman A, Witteman JC (2004) Dietary intake of menaquinone is associated with a reduced risk of coronary heart disease: the Rotterdam Study. J Nutr 134(11):3100–3105. https://doi.org/10.1093/jn/134.11.3100
Erkkila AT, Booth SL, Hu FB, Jacques PF, Manson JE, Rexrode KM, Stampfer MJ, Lichtenstein AH (2005) Phylloquinone intake as a marker for coronary heart disease risk but not stroke in women. Eur J Clin Nutr 59(2):196–204. https://doi.org/10.1038/sj.ejcn.1602058
Erkkila AT, Booth SL, Hu FB, Jacques PF, Lichtenstein AH (2007) Phylloquinone intake and risk of cardiovascular diseases in men. Nutr Metab Cardiovasc Dis 17(1):58–62. https://doi.org/10.1016/j.numecd.2006.03.008
Gast GC, de Roos NM, Sluijs I, Bots ML, Beulens JW, Geleijnse JM, Witteman JC, Grobbee DE, Peeters PH, van der Schouw YT (2009) A high menaquinone intake reduces the incidence of coronary heart disease. Nutr Metab Cardiovasc Dis 19(7):504–510. https://doi.org/10.1016/j.numecd.2008.10.004
Vissers LE, Dalmeijer GW, Boer JM, Monique Verschuren WM, van der Schouw YT, Beulens JW (2013) Intake of dietary phylloquinone and menaquinones and risk of stroke. J Am Heart Assoc 2(6):e000455. https://doi.org/10.1161/jaha.113.000455
Juanola-Falgarona M, Salas-Salvado J, Martinez-Gonzalez MA, Corella D, Estruch R, Ros E, Fito M, Aros F, Gomez-Gracia E, Fiol M, Lapetra J, Basora J, Lamuela-Raventos RM, Serra-Majem L, Pinto X, Munoz MA, Ruiz-Gutierrez V, Fernandez-Ballart J, Bullo M (2014) Dietary intake of vitamin K is inversely associated with mortality risk. J Nutr 144(5):743–750. https://doi.org/10.3945/jn.113.187740
Zwakenberg SR, den Braver NR, Engelen AI, Feskens EJ, Vermeer C, Boer JM, Verschuren WM, van der Schouw YT, Beulens JW (2016) Vitamin K intake and all-cause and cause specific mortality. Clin Nutr 36(5):1294–1300. https://doi.org/10.1016/j.clnu.2016.08.017
Ueland T, Gullestad L, Dahl CP, Aukrust P, Aakhus S, Solberg OG, Vermeer C, Schurgers LJ (2010) Undercarboxylated matrix Gla protein is associated with indices of heart failure and mortality in symptomatic aortic stenosis. J Intern Med 268(5):483–492. https://doi.org/10.1111/j.1365-2796.2010.02264.x
Schurgers LJ, Barreto DV, Barreto FC, Liabeuf S, Renard C, Magdeleyns EJ, Vermeer C, Choukroun G, Massy ZA (2010) The circulating inactive form of matrix Gla protein is a surrogate marker for vascular calcification in chronic kidney disease: a preliminary report. Clin J Am Soc Nephrol 5:568–575. https://doi.org/10.2215/cjn.07081009
Dalmeijer GW, van der Schouw YT, Magdeleyns EJ, Vermeer C, Verschuren WM, Boer JM, Beulens JW (2013) Matrix Gla protein species and risk of cardiovascular events in type 2 diabetic patients. Diabetes Care 36(11):3766–3771. https://doi.org/10.2337/dc13-0065
van den Heuvel EG, van Schoor NM, Lips P, Magdeleyns EJ, Deeg DJ, Vermeer C, den Heijer M (2014) Circulating uncarboxylated matrix Gla protein, a marker of vitamin K status, as a risk factor of cardiovascular disease. Maturitas 77(2):137–141. https://doi.org/10.1016/j.maturitas.2013.10.008
Dalmeijer GW, van der Schouw YT, Magdeleyns EJ, Vermeer C, Verschuren WM, Boer JM, Beulens JW (2014) Circulating desphospho-uncarboxylated matrix gamma-carboxyglutamate protein and the risk of coronary heart disease and stroke. J Thromb Haemost 12(7):1028–1034. https://doi.org/10.1111/jth.12609
Keyzer CA, Vermeer C, Joosten MM, Knapen MH, Drummen NE, Navis G, Bakker SJ, de Borst MH (2015) Vitamin K status and mortality after kidney transplantation: a cohort study. Am J Kidney Dis 65(3):474–483. https://doi.org/10.1053/j.ajkd.2014.09.014
Mayer O Jr, Seidlerova J, Vanek J, Karnosova P, Bruthans J, Filipovsky J, Wohlfahrt P, Cifkova R, Windrichova J, Knapen MH, Drummen NE, Vermeer C (2016) The abnormal status of uncarboxylated matrix Gla protein species represents an additional mortality risk in heart failure patients with vascular disease. Int J Cardiol 203:916–922. https://doi.org/10.1016/j.ijcard.2015.10.226
Zwakenberg SR, van der Schouw YT, Vermeer C, Pasterkamp G, den Ruijter HM, Beulens JWJ (2018) Matrix Gla protein, plaque stability, and cardiovascular events in patients with severe atherosclerotic disease. Cardiology 141:32–36. https://doi.org/10.1159/000493006
Yeap BB, Chubb SA, Flicker L, McCaul KA, Ebeling PR, Hankey GJ, Beilby JP, Norman PE (2012) Associations of total osteocalcin with all-cause and cardiovascular mortality in older men. The Health In Men Study. Osteoporos Int 23:599–606. https://doi.org/10.1007/s00198-011-1586-1
Yamashita T, Okano K, Tsuruta Y, Akiba T, Nitta K (2013) Serum osteocalcin levels are useful as a predictor of cardiovascular events in maintenance hemodialysis patients. Int Urol Nephrol 45:207–214. https://doi.org/10.1007/s11255-012-0156-6
Holvik K, van Schoor NM, Eekhoff EM, den Heijer M, Deeg DJ, Lips P, de Jongh R (2014) Plasma osteocalcin levels as a predictor of cardiovascular disease in older men and women: a population-based cohort study. Eur J Endocrinol 171:161–170. https://doi.org/10.1530/eje-13-1044
Hwang YC, Kang M, Cho IJ, Jeong IK, Ahn KJ, Chung HY, Lee MK (2015) Association between the circulating total osteocalcin level and the development of cardiovascular disease in middle-aged men: a mean 8.7-year longitudinal follow-up study. J Atheroscler Thromb 22:136–143. https://doi.org/10.5551/jat.25718
Miyake H, Kanazawa I, Sugimoto T (2018) Association of bone mineral density, bone turnover markers, and vertebral fractures with all-cause mortality in type 2 diabetes mellitus. Calcif Tissue Int 102:1–13. https://doi.org/10.1007/s00223-017-0324-x
Zwakenberg SR, van der Schouw YT, Schalkwijk CG, Spijkerman AMW, Beulens JWJ (2018) Bone markers and cardiovascular risk in type 2 diabetes patients. Cardiovasc Diabetol 17:45. https://doi.org/10.1186/s12933-018-0691-2
Cheung CL, Sahni S, Cheung BM, Sing CW, Wong IC (2015) Vitamin K intake and mortality in people with chronic kidney disease from NHANES III. Clin Nutr 34(2):235–240. https://doi.org/10.1016/j.clnu.2014.03.011
Liu YP, Gu YM, Thijs L, Knapen MH, Salvi E, Citterio L, Petit T, Carpini SD, Zhang Z, Jacobs L, Jin Y, Barlassina C, Manunta P, Kuznetsova T, Verhamme P, Struijker-Boudier HA, Cusi D, Vermeer C, Staessen JA (2015) Inactive matrix Gla protein is causally related to adverse health outcomes: a Mendelian randomization study in a Flemish population. Hypertension 65(2):463–470. https://doi.org/10.1161/hypertensionaha.114.04494
Riphagen IJ, Keyzer CA, Drummen NEA, de Borst MH, Beulens JWJ, Gansevoort RT, Geleijnse JM, Muskiet FAJ, Navis G, Visser ST, Vermeer C, Kema IP, Bakker SJL (2017) Prevalence and effects of functional vitamin K insufficiency: the PREVEND Study. Nutrients 9(12):1334. https://doi.org/10.3390/nu9121334
Shea MK, Booth SL, Weiner DE, Brinkley TE, Kanaya AM, Murphy RA, Simonsick EM, Wassel CL, Vermeer C, Kritchevsky SB (2017) Circulating vitamin K is inversely associated with incident cardiovascular disease risk among those treated for hypertension in the Health, Aging, and Body Composition Study (Health ABC). J Nutr 147(5):888–895. https://doi.org/10.1161/strokeaha.117.01720610.3945/jn.117.249375
Guo J, Astrup A, Lovegrove JA, Gijsbers L, Givens DI, Soedamah-Muthu SS (2017) Milk and dairy consumption and risk of cardiovascular diseases and all-cause mortality: dose-response meta-analysis of prospective cohort studies. Eur J Epidemiol 32:269–287. https://doi.org/10.1007/s10654-017-0243-1
Rong Y, Chen L, Zhu T, Song Y, Yu M, Shan Z, Sands A, Hu FB, Liu L (2013) Egg consumption and risk of coronary heart disease and stroke: dose-response meta-analysis of prospective cohort studies. BMJ 346:e8539. https://doi.org/10.1136/bmj.e8539
Bechthold A, Boeing H, Schwedhelm C, Hoffmann G, Knuppel S, Iqbal K, De Henauw S, Michels N, Devleesschauwer B, Schlesinger S, Schwingshackl L (2019) Food groups and risk of coronary heart disease, stroke and heart failure: a systematic review and dose-response meta-analysis of prospective studies. Crit Rev Food Sci Nutr 59:1071–1090. https://doi.org/10.1080/10408398.2017.1392288
Holick CN, Michaud DS, Stolzenberg-Solomon R, Mayne ST, Pietinen P, Taylor PR, Virtamo J, Albanes D (2002) Dietary carotenoids, serum beta-carotene, and retinol and risk of lung cancer in the alpha-tocopherol, beta-carotene cohort study. Am J Epidemiol 156(6):536–547. https://doi.org/10.1093/aje/kwf072
Dietary Assessment Primer (2016) Food frequency questionnaire at a Glance. National Cancer Institute, National Institutes of Health. https://dietassessmentprimer.cancer.gov/profiles/questionnaire/ (cited 1 June 2018)
Lawlor DA, Smith GD, Bruckdorfer KR, Kundu D, Ebrahim S (2004) Those confounded vitamins: what can we learn from the differences between observational versus randomised trial evidence? Lancet 363(9422):1724–1727. https://doi.org/10.1016/s0140-6736(04)16260-0
Pan A, Chen M, Chowdhury R, Wu JH, Sun Q, Campos H, Mozaffarian D, Hu FB (2012) alpha-Linolenic acid and risk of cardiovascular disease: a systematic review and meta-analysis. Am J Clin Nutr 96(6):1262–1273. https://doi.org/10.3945/ajcn.112.044040
Jones KS, Bluck LJ, Wang LY, Coward WA (2008) A stable isotope method for the simultaneous measurement of vitamin K1 (phylloquinone) kinetics and absorption. Eur J Clin Nutr 62(11):1273–1281. https://doi.org/10.1038/sj.ejcn.1602859
van Ballegooijen AJ, Beulens JW (2017) The role of vitamin K status in cardiovascular health: evidence from observational and clinical studies. Curr Nutr Rep 6:197–205. https://doi.org/10.1007/s13668-017-0208-8
EFSA NDA Panel (EFSA Panel on Dietetic Products, Nutrition and Allergies), Turck D, Bresson JL, Burlingame B, Dean T, Fairweather-Tait S, Heinonen M, Hirsch-Ernst KI, Mangelsdorf I, McArdle HJ, Naska A, Nowicka G, Pentieva K, Sanz Y, Siani A, Sjodin A, Stern M, Tome D, Van Loveren H, Vinceti M, Willatts P, Lamberg-Allardt C, Przyrembel H, Tetens I, Dumas C, Fabiani L, Ioannidou S, Neuhauser-Berthold M, Nutr EPDP (2017) Scientific Opinion on the dietary reference values for vitamin K. EFSA J 15(5):4780. https://doi.org/10.2903/j.efsa.2017.4780
Shea MK, O’Donnell CJ, Hoffmann U, Dallal GE, Dawson-Hughes B, Ordovas JM, Price PA, Williamson MK, Booth SL (2009) Vitamin K supplementation and progression of coronary artery calcium in older men and women. Am J Clin Nutr 89(6):1799–1807. https://doi.org/10.3945/ajcn.2008.27338
Knapen MH, Braam LA, Drummen NE, Bekers O, Hoeks AP, Vermeer C (2015) Menaquinone-7 supplementation improves arterial stiffness in healthy postmenopausal women. A double-blind randomised clinical trial. Thromb Haemost 113(5):1135–1144. https://doi.org/10.1160/TH14-08-0675
Schurgers LJ, Uitto J, Reutelingsperger CP (2013) Vitamin K-dependent carboxylation of matrix Gla-protein: a crucial switch to control ectopic mineralization. Trends Mol Med 19(4):217–226. https://doi.org/10.1016/j.molmed.2012.12.008
Cranenburg EC, Schurgers LJ, Vermeer C (2007) Vitamin K: the coagulation vitamin that became omnipotent. Thromb Haemost 98(1):120–125. https://doi.org/10.1160/TH07-04-0266
Spronk HM, Soute BA, Schurgers LJ, Thijssen HH, De Mey JG, Vermeer C (2003) Tissue-specific utilization of menaquinone-4 results in the prevention of arterial calcification in warfarin-treated rats. J Vasc Res 40(6):531–537. https://doi.org/10.1159/000075344
Tsugawa N (2015) Cardiovascular diseases and fat soluble vitamins: vitamin D and vitamin K. J Nutr Sci Vitaminol (Tokyo) 61(Suppl):S170–S172. https://doi.org/10.3177/jnsv.61.S170
Acknowledgements
We thank Geertje W. Dalmeijer and Sabine R. Zwakenberg (Julius Center for Health Sciences and Primary Care, University Medical Center Utrecht, Utrecht, The Netherlands) for providing re-analyzed data on dp-ucMGP and total CVD.
Funding
The work was supported by the National Key Research and Development Program of China (2017YFC0907500 and 2017YFC0907504), and Hubei Province Science Fund for Distinguished Young Scholars (2018CFA033).
Author information
Authors and Affiliations
Contributions
H-GC performed the statistical analysis; contributed to the discussion, wrote the manuscript, and reviewed and edited the manuscript. H-GC and L-TS conducted the research, screened the references and extracted the data. Y-BZ, A-LC, and Y-WL researched and proofed the data. SKK transformed the data to comparison of top third with bottom third. LJ and AP planned and designed the study. H-GC and AP had full access to the data in this study and take complete responsibility for the integrity of the data and the accuracy of the data analysis. All authors critically reviewed, discussed, and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
AP reported receiving a research grant from the BY-HEALTH CO., LTD, outside the submitted work. Other authors declare no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, HG., Sheng, LT., Zhang, YB. et al. Association of vitamin K with cardiovascular events and all-cause mortality: a systematic review and meta-analysis. Eur J Nutr 58, 2191–2205 (2019). https://doi.org/10.1007/s00394-019-01998-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-019-01998-3