Abstract
HLA 1-locus-mismatched unrelated donors (1MMUD) are often considered as alternative donors in allogeneic hematopoietic stem-cell transplantation (allo-HCT) when an HLA-matched related or unrelated donor is unavailable. However, HLA mismatch remains a major risk factor for acute and chronic graft-versus-host disease (GVHD). Antithymocyte globulin (ATG) has been used to prevent acute and chronic GVHD, and multiple studies have shown that use of ATG is associated with decreased acute and chronic GVHD, which is associated with improved QOL. However, at high doses, ATG may lead to an increase in fatal infection, relapse, or delayed engraftment. The optimal ATG dose for MMUD remains unclear. The optimal ATG dose should be determined based on a fine balance between the reduction of GVHD and the risk of relapse, fatal infection, and/or delayed engraftment. Interestingly, promising results from some recent Asian studies suggest that a low dose of ATG may improve non-relapse mortality and overall survival without increasing relapse or fatal infection in allo-HCT from an HLA-mismatched unrelated donor. A randomized control trial is expected to confirm these results in Japan. In addition, pharmacokinetic/pharmacodynamic studies may help to identify the personalized optimal ATG dose.
Similar content being viewed by others
Introduction
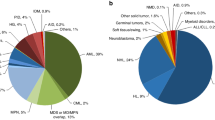
An HLA-matched unrelated donor (MUD) is considered to be the best alternative donor in allogeneic hematopoietic stem-cell transplantation (allo-HCT) for patients who lack an HLA-matched related donor (MRD), because the transplant outcomes from MUD are comparable to those from MRD [1,2,3]. However, at least 70% of patients in Japan do not have a MRD, and it is difficult to find a MUD for patients who have rare HLA haplotypes. Therefore, as shown in Fig. 1, it is not uncommon for alternative donor sources to be selected in allo-HCT. In addition to an HLA 1-locus-mismatched-related donor, umbilical cord blood and HLA-haploidentical donor, an HLA 1-locus-mismatched unrelated donor (1MMUD) has been considered to be an alternative donor in allo-HCT when an HLA-matched related or unrelated donor is unavailable. On the other hand, it is not yet clear which donor source is most suitable as a third donor selection. Therefore, the third donor is selected according to the experience of each institution and/or the patient disease status and clinical condition.
In general, when an unrelated donor is selected, HLA-A, HLA-B, HLA-C, and HLA-DRB1 (± HLA-DQB1) alleles are genotyped in each patient and donor prior to allo-HCT. HLA-mismatching remains a major risk factor for acute and chronic graft-versus-host disease (GVHD) in unrelated transplantation. As a result, overall survival (OS) in allo-HCT from an HLA-mismatched unrelated donor (MMUD) has been shown to be inferior to that of allo-HCT from MUD [4,5,6,7,8]. While antithymocyte or antilymphocyte globulin (ATG) has been used for the prevention of acute and chronic GVHD, ATG can also lead to delayed immune reconstitution of T cells, resulting in increased relapse or infection [9]. Several randomized control trials have evaluated the efficacy of ATG in allo-HCT (Table 1) [10,11,12,13,14,15,16,17]. The incidence of acute and chronic GVHD was significantly lower in the ATG group, but there were no significant differences in relapse rate, non-relapse mortality, or overall survival between the two groups, except for one study. However, the efficacy of ATG for MMUD remains unclear, because most patients in these trials received allo-HCT from MUD or MRD. Therefore, this review focuses on the role of ATG in adult patients who receive allo-HCT from MMUD.
ATG formulation and mechanisms
ATG is a polyclonal immunoglobulin preparation obtained by immunizing animals with human thymocytes (thymoglobulin [Sanofi, Paris, France] and ATGAM [Pfizer, New York, NY]) or Jurkat T lymphoblastoid cells (ATG-Fresenius (ATG-F) [Neovii Biotech, Graefelfing, Germany]) [18]. Thymoglobulin and ATG-F are produced by immunized rabbit, and ATGAM is produced by immunized horse. Lymphoglobulin (Genzyme, Cambridge, MA), which was produced by horse immunized with human thymocytes, was withdrawn from the market in the late 2000s. ATGAM is unavailable in many countries, except for the USA. In Japan, thymoglobulin is the only ATG formulation approved for GVHD prophylaxis under the Japanese National Health Insurance system. Therefore, this review covers rabbit ATG, especially thymoglobulin.
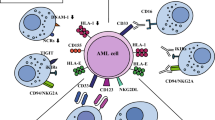
ATG consists of polyclonal antibodies against multiple antigens expressed on T cells, B cells, natural killer cells, dendritic cells, and so on. Thus, ATG has the following diverse effects on the immune system: T-cell depletion in blood and peripheral lymphoid tissues through complement-dependent lysis and T-cell activation and apoptosis, induction of B-cell apoptosis, modulation of key cell-surface molecules that mediate leukocyte/endothelium interactions, interference with the functional properties of dendritic cells, and induction of Treg and NK-T cells [18, 19]. Therefore, ATG is used for GVHD prophylaxis and treatment [20], treatment of severe aplastic anemia [21, 22], and prevention or rescue treatment of acute rejection in organ transplantation [23].
Transplant outcomes by ATG as GVHD prophylaxis
Limited data are available for evaluating the efficacy of ATG as GVHD prophylaxis in allo-HCT from MMUD. Table 2 summarizes the results of retrospective studies on ATG in unrelated allo-HCT. However, there are insufficient data on MMUD. Therefore, this review evaluated the impact of ATG on allo-HCT from MMUD with reference to the results of MUD and a related donor.
GVHD
The use of ATG reduced the incidences of acute and/or chronic GVHD in all of the randomized control trials and most of the retrospective studies (Tables 1, 2). This was confirmed by a meta-analysis of the randomized control trials [24,25,26,27]. In general, the risk of acute and chronic GVHD is higher in allo-HCT from MMUD than in that from MUD [4,5,6,7,8]. Thus, the use of ATG for GVHD prophylaxis is reasonable in allo-HCT from MMUD. In addition, reduction of GVHD, especially chronic GVHD, is expected to improve quality of life (QOL) after allo-HCT, since chronic GVHD is associated with impaired QOL [28,29,30,31]. Two randomized control trials suggested that ATG could improve QOL [11, 15]. Moreover, multiple studies have also reported that the probability of immunosuppressive treatment-free survival was higher in patients who received ATG [13, 15, 32, 33].
Engraftment
In 3 of 6 randomized trials, the median times to neutrophil and platelet engraftment in the ATG group were longer by 3–7 days and 7–17 days than those in the non-ATG group [12, 16, 17]. No significant difference was found in the other trials, although delayed platelet engraftment was noted in the 15 mg/kg group, but not the 7.5 mg/kg group, in the GITMO study [10, 15]. These 3 trials used ATG-F (total dose 30–60 mg/kg), while the other 3 trials used thymoglobulin (total dose 4.5–15 mg/kg). A meta-analysis of the randomized trials demonstrated that neutrophil engraftment was significantly delayed (median 2.66 days) [26]. On the other hand, ATG had no impact on neutrophil or platelet engraftment in retrospective studies that targeted unrelated donors (Table 2). This discrepancy may be due to the difference in the method of ATG preparation and/or the ATG dose, and the presence of HLA-mismatching in addition to the retrospective nature of the study. Further studies are necessary to assess the influence of ATG on neutrophil and platelet engraftment in the MMUD setting.
Infection
Some studies have reported that a higher dose of ATG is associated with a higher incidence of infection [10, 34,35,36]. Bacigalupo et al. reported that a higher dose of thymoglobulin (15 mg/kg) increased the risk of fatal infection, whereas thymoglobulin at 7.5 mg/kg did not [10]. Remberger et al. also showed that thymoglobulin at 10 mg/kg tended to increase infectious mortality in comparison with thymoglobulin at 4–8 mg/kg [34]. These results suggested that a high dose of ATG could cause fatal infection.
A major concern is whether the use of ATG leads to an increase in viral reactivation such as of cytomegalovirus (CMV) or Epstein-Barr virus (EBV). The use of ATG is considered to be a risk factor for EBV-post-transplantation lymphoproliferative disorders (PTLDs) [37]. Walker et al. reported that EBV reactivation was more common in a ATG group than in a non-ATG group [15]. A meta-analysis showed increased incidences of CMV and EBV reactivation (risk ratio 1.25 and 1.33) [26]. Although a low dose of ATG may not increase fatal infections, it is unclear whether it increases viral infections such as by CMV or EBV. Therefore, viral reactivation should be monitored carefully when ATG is used.
Non-relapse mortality
No significant differences in non-relapse mortality were found between the ATG group and the non-ATG group in randomized control trials, although the incidences of GVHD significantly differed (Table 1). While the precise reason for this finding is not clear, the incidence of infection might influence this result. On the other hand, some retrospective studies that included MMUD showed that the use of ATG was associated with lower non-relapse mortality [32, 34, 38,39,40]. We reported that non-relapse mortality in the ATG group was lower than that in the non-ATG group (HR 0.35; 95% CI 0.19–0.65; p < 0.001) in patients who received allo-HCT from 1MMUD using a recent Japanese registry data [40]. This may suggest that the advantage of ATG (reduction of GVHD) outweighs the disadvantage (risk of infection) in allo-HCT from MMUD.
Relapse
As shown in Tables 1 and 2, there was no significant difference in relapse rate between the ATG group and the non-ATG group in randomized control trials and retrospective studies. On the other hand, two large retrospective studies reported that reduced-intensity conditioning (RIC) with ATG was associated with a higher relapse rate [41, 42]. However, the dose of ATG was unclear and several donor types (MRD, MUD, and/or MMUD) were included in these two studies. Interestingly, Remberger et al. showed that a higher dose of thymoglobulin (8 mg/kg) increased the incidence of relapse in comparison with an intermediate dose (6 mg/kg) after RIC allo-HCT from MUD [43]. The European Group for Blood and Marrow Transplantation (EBMT) study also reported that a higher dose of thymoglobulin (≥ 6 mg/kg) significantly increased the risk of relapse for acute myeloid leukemia patients who received RIC allo-HCT from an HLA-matched sibling [44]. On the other hand, Korean and Japanese studies showed that low-dose ATG was not associated with a high risk of relapse in the setting of MMUD [32, 33, 39, 40]. Therefore, a low or intermediate dose of ATG may not increase the risk of relapse in allo-HCT from MMUD, although we should still pay attention in the RIC setting because of limited data.
Overall survival
In 5 of 6 randomized control trials, ATG was not associated with an improvement of OS (Table 1) [10,11,12,13,14,15,16]. On the other hand, Soiffer et al. reported that OS was lower in the ATG group [17]. Although the cause of this difference is not clear, the dose of ATG and/or donor type might have influenced the results. As shown in Table 2, some retrospective studies showed that OS in the ATG group was superior to that in the non-ATG group in allo-HCT from an unrelated donor, especially MMUD [38,39,40, 45]. A Japanese retrospective study showed that the use of low-dose thymoglobulin (median 2.5 mg/kg) significantly decreased not only acute GVHD, but also non-relapse mortality, without increasing relapse, resulting in an improvement of OS in allo-HCT from 1MMUD [40]. Kim et al. reported comparable results in allo-HCT from MMUD in Korea [39]. These results suggest that the use of ATG may improve OS in patients who received allo-HCT from MMUD, at least in Asia. The use of ATG for MMUD may be more effective than that for MUD or MRD because HLA-mismatch is a risk factor for GVHD.
Optimal ATG dose and timing
The optimal ATG dose in allo-HCT from MMUD remains unclear. Although a high ATG dose could reduce the incidence of acute and chronic GVHD, it may lead to an increase in fatal infection, relapse, or delayed engraftment due to delayed immune reconstitution of T cells. On the other hand, a low ATG dose may decrease infection and/or relapse, but may be insufficient to prevent GVHD. Thus, we should determine the optimal ATG dose based on a delicate balance between the reduction of GVHD and the risk of relapse, fatal infection, and/or delayed engraftment. This balance may vary according to the risk of GVHD and the disease condition, such as donor type, stem cell source, race, conditioning regimen, and disease stage. The EBMT and the European LeukemiaNet working group recommend that the dose of ATG-F should be 30 mg/kg and that of thymoglobulin should be 7.5 mg/kg in allo-HCT from MUD [20]. On the other hand, Japanese and Korean studies showed that a low dose of thymoglobulin (median 2.5 mg/kg) could lead to promising transplant outcomes despite allo-HCT from 1 to 2 MMUD [39, 40]. These results suggest that the optimal ATG dose for Asian patients may be lower than that for Caucasian patients. The difference may be due to the risk of GVHD, because several studies have demonstrated that the incidence of GVHD in Asian patients is lower than that in Caucasian patients [46,47,48]. In addition, peripheral blood stem cells have been commonly used in unrelated transplantation in the Europe and the United states [49, 50], whereas bone marrow has been still widely used in Japan. Some studies have shown that the risk of GVHD is higher in allo-HCT of peripheral blood stem cells from an unrelated donor than in that of bone marrow [51, 52]. Therefore, the difference of the dominant stem-cell source may affect the ATG dose. Thus, the optimal ATG dose may be differ according to stem cell sources. Japanese patients may receive great benefit from, ATG because only low-dose ATG can control GVHD and lead to decreases in fatal infection and relapse, resulting in the improvement of OS. Interestingly, a randomized controlled trial is being conducted to evaluate the efficacy of low-dose ATG (thymoglobulin: 2.5 mg/kg) for patients in Japan who received allo-HCT from 1MMUD (UMIN000028008). This trial is expected to evaluate the efficacy of low-dose ATG for 1MMUD and determine the optimal dose of ATG for Japanese patients.
Pharmacokinetic/Pharmacodynamic (PK/PD) studies are also important for evaluating the optimal dose of ATG. Admiraal et al. recently reported that an optimum ATG exposure was associated with higher overall survival because of lower relapse-related mortality and lower non-relapse mortality, whereas a below-optimum ATG exposure increased GVHD and non-relapse mortality, and an above-optimum ATG exposure increased relapse [53]. Interestingly, they showed that recipient’s absolute lymphocyte count before administration of ATG was the relevant predictor for ATG pharmacokinetics in adults. Thus, the optimum ATG dose may have to be determined based on absolute lymphocyte count rather than bodyweight. In addition, the timing of ATG administration may also affect transplant outcomes. The late administration of ATG may lead to a decrease in GVHD, but delayed engraftment, in comparison with the early administration of ATG [9]. However, there are insufficient data to determine the optimal timing of ATG administration. The optimal timing probably interacts with the ATG dose. Therefore, it is necessary to investigate the timing of ATG in conjunction with the ATG dose.
Conclusions and future perspectives
The use of ATG in allo-HCT from MMUD can be a promising intervention approach for not only preventing acute and chronic GVHD but also improving QOL. In addition, ATG may improve OS through lower non-relapse mortality, if a low or intermediate dose of ATG can control GVHD despite a higher risk of GVHD for MMUD. Further studies are necessary to evaluate the effect of ATG in various settings, because the optimal dose and timing of ATG for MMUD remain unclear. PK/PD studies may also help to identify the personalized optimal ATG dose. Furthermore, careful monitoring, and prophylaxis and pretreatment of viral reactivation may further improve overall survival by reducing viral infections such as by CMV or EBV. Therefore, 1MMUD is expected to be a suitable alternative donor if the optimal dose of ATG is used.
References
Yakoub-Agha I, Mesnil F, Kuentz M, Boiron JM, Ifrah N, Milpied N, et al. Allogeneic marrow stem-cell transplantation from human leukocyte antigen-identical siblings versus human leukocyte antigen-allelic-matched unrelated donors (10/10) in patients with standard-risk hematologic malignancy: a prospective study from the French Society of Bone Marrow Transplantation and Cell Therapy. J Clin Oncol. 2006;24(36):5695–702.
Schetelig J, Bornhauser M, Schmid C, Hertenstein B, Schwerdtfeger R, Martin H, et al. Matched unrelated or matched sibling donors result in comparable survival after allogeneic stem-cell transplantation in elderly patients with acute myeloid leukemia: a report from the cooperative German Transplant Study Group. J Clin Oncol. 2008;26(32):5183–91.
Kanda J, Saji H, Fukuda T, Kobayashi T, Miyamura K, Eto T, et al. Related transplantation with HLA-1 Ag mismatch in the GVH direction and HLA-8/8 allele-matched unrelated transplantation: a nationwide retrospective study. Blood. 2012;119(10):2409–16.
Flomenberg N, Baxter-Lowe LA, Confer D, Fernandez-Vina M, Filipovich A, Horowitz M, et al. Impact of HLA class I and class II high-resolution matching on outcomes of unrelated donor bone marrow transplantation: HLA-C mismatching is associated with a strong adverse effect on transplantation outcome. Blood. 2004;104(7):1923–30.
Lee SJ, Klein J, Haagenson M, Baxter-Lowe LA, Confer DL, Eapen M, et al. High-resolution donor-recipient HLA matching contributes to the success of unrelated donor marrow transplantation. Blood. 2007;110(13):4576–83.
Kanda Y, Kanda J, Atsuta Y, Maeda Y, Ichinohe T, Ohashi K, et al. Impact of a single human leucocyte antigen (HLA) allele mismatch on the outcome of unrelated bone marrow transplantation over two time periods. A retrospective analysis of 3003 patients from the HLA Working Group of the Japan Society for Blood and Marrow Transplantation. Br J Haematol. 2013;161(4):566–77.
Kanda J, Ichinohe T, Fuji S, Maeda Y, Ohashi K, Fukuda T, et al. Impact of HLA mismatch direction on the outcome of unrelated bone marrow transplantation: a retrospective analysis from the Japan Society for Hematopoietic Cell Transplantation. Biol Blood Marrow Transplant. 2015;21(2):305–11.
Morishima Y, Kashiwase K, Matsuo K, Azuma F, Morishima S, Onizuka M, et al. Biological significance of HLA locus matching in unrelated donor bone marrow transplantation. Blood. 2015;125(7):1189–97.
Lindemans CA, Chiesa R, Amrolia PJ, Rao K, Nikolajeva O, de Wildt A, et al. Impact of thymoglobulin prior to pediatric unrelated umbilical cord blood transplantation on immune reconstitution and clinical outcome. Blood. 2014;123(1):126–32.
Bacigalupo A, Lamparelli T, Bruzzi P, Guidi S, Alessandrino PE, di Bartolomeo P, et al. Antithymocyte globulin for graft-versus-host disease prophylaxis in transplants from unrelated donors: 2 randomized studies from Gruppo Italiano Trapianti Midollo Osseo (GITMO). Blood. 2001;98(10):2942–7.
Bacigalupo A, Lamparelli T, Barisione G, Bruzzi P, Guidi S, Alessandrino PE, et al. Thymoglobulin prevents chronic graft-versus-host disease, chronic lung dysfunction, and late transplant-related mortality: long-term follow-up of a randomized trial in patients undergoing unrelated donor transplantation. Biol Blood Marrow Transplant. 2006;12(5):560–5.
Finke J, Bethge WA, Schmoor C, Ottinger HD, Stelljes M, Zander AR, et al. Standard graft-versus-host disease prophylaxis with or without anti-T-cell globulin in haematopoietic cell transplantation from matched unrelated donors: a randomised, open-label, multicentre phase 3 trial. Lancet Oncol. 2009;10(9):855–64.
Socie G, Schmoor C, Bethge WA, Ottinger HD, Stelljes M, Zander AR, et al. Chronic graft-versus-host disease: long-term results from a randomized trial on graft-versus-host disease prophylaxis with or without anti-T-cell globulin ATG-Fresenius. Blood. 2011;117(23):6375–82.
Finke J, Schmoor C, Bethge WA, Ottinger H, Stelljes M, Volin L, et al. Long-term outcomes after standard graft-versus-host disease prophylaxis with or without anti-human-T-lymphocyte immunoglobulin in haemopoietic cell transplantation from matched unrelated donors: final results of a randomised controlled trial. Lancet Haematol. 2017;4(6):e293–301.
Walker I, Panzarella T, Couban S, Couture F, Devins G, Elemary M, et al. Pretreatment with anti-thymocyte globulin versus no anti-thymocyte globulin in patients with haematological malignancies undergoing haemopoietic cell transplantation from unrelated donors: a randomised, controlled, open-label, phase 3, multicentre trial. Lancet Oncol. 2016;17(2):164–73.
Kroger N, Solano C, Wolschke C, Bandini G, Patriarca F, Pini M, et al. Antilymphocyte globulin for prevention of chronic graft-versus-host disease. N Engl J Med. 2016;374(1):43–53.
Soiffer RJ, Kim HT, McGuirk J, Horwitz ME, Johnston L, Patnaik MM, et al. Prospective, randomized, double-blind, phase III clinical trial of anti-T-lymphocyte globulin to assess impact on chronic graft-versus-host disease-free survival in patients undergoing HLA-matched unrelated myeloablative hematopoietic cell transplantation. J Clin Oncol. 2017;35(36):4003–11.
Storek J, Mohty M, Boelens JJ. Rabbit anti-T cell globulin in allogeneic hematopoietic cell transplantation. Biol Blood Marrow Transplant. 2015;21(6):959–70.
Mohty M. Mechanisms of action of antithymocyte globulin: T-cell depletion and beyond. Leukemia. 2007;21(7):1387–94.
Ruutu T, Gratwohl A, de Witte T, Afanasyev B, Apperley J, Bacigalupo A, et al. Prophylaxis and treatment of GVHD: EBMT-ELN working group recommendations for a standardized practice. Bone Marrow Transplant. 2014;49(2):168–73.
Scheinberg P, Nunez O, Weinstein B, Scheinberg P, Biancotto A, Wu CO, et al. Horse versus rabbit antithymocyte globulin in acquired aplastic anemia. N Engl J Med. 2011;365(5):430–8.
Hayakawa J, Kanda J, Akahoshi Y, Harada N, Kameda K, Ugai T, et al. Meta-analysis of treatment with rabbit and horse antithymocyte globulin for aplastic anemia. Int J Hematol. 2017;105(5):578–86.
Beiras-Fernandez A, Thein E, Hammer C. Induction of immunosuppression with polyclonal antithymocyte globulins: an overview. Exp Clin Transplant. 2003;1(2):79–84.
Kumar A, Mhaskar AR, Reljic T, Mhaskar RS, Kharfan-Dabaja MA, Anasetti C, et al. Antithymocyte globulin for acute-graft-versus-host-disease prophylaxis in patients undergoing allogeneic hematopoietic cell transplantation: a systematic review. Leukemia. 2012;26(4):582–8.
Gagelmann N, Ayuk F, Wolschke C, Kroger N. Comparison of different rabbit anti-thymocyte globulin formulations in allogeneic stem cell transplantation: systematic literature review and network meta-analysis. Biol Blood Marrow Transplant. 2017;23(12):2184–91.
Arai Y, Jo T, Matsui H, Kondo T, Takaori-Kondo A. Efficacy of antithymocyte globulin for allogeneic hematopoietic cell transplantation: a systematic review and meta-analysis. Leukemia Lymphoma. 2017;58(8):1840–8.
Yuan J, Pei R, Su W, Cao J, Lu Y. Meta-analysis of the actions of antithymocyte globulin in patients undergoing allogeneic hematopoietic cell transplantation. Oncotarget. 2017;8(7):10871–82.
Fraser CJ, Bhatia S, Ness K, Carter A, Francisco L, Arora M, et al. Impact of chronic graft-versus-host disease on the health status of hematopoietic cell transplantation survivors: a report from the Bone Marrow Transplant Survivor Study. Blood. 2006;108(8):2867–73.
Lee SJ, Kim HT, Ho VT, Cutler C, Alyea EP, Soiffer RJ, et al. Quality of life associated with acute and chronic graft-versus-host disease. Bone Marrow Transplant. 2006;38(4):305–10.
Pidala J, Kurland B, Chai X, Majhail N, Weisdorf DJ, Pavletic S, et al. Patient-reported quality of life is associated with severity of chronic graft-versus-host disease as measured by NIH criteria: report on baseline data from the Chronic GVHD Consortium. Blood. 2011;117(17):4651–7.
Kurosawa S, Oshima K, Yamaguchi T, Yanagisawa A, Fukuda T, Kanamori H, et al. Quality of life after allogeneic hematopoietic cell transplantation according to affected organ and severity of chronic graft-versus-host disease. Biol Blood Marrow Transplant. 2017;23(10):1749–58.
Fuji S, Ueno N, Hiramoto N, Asakura Y, Yakushijin K, Kamiyama Y, et al. Reduced-intensity conditioning regimen with low-dose ATG-F for unrelated bone marrow transplant is associated with lower non-relapse mortality than a regimen with low-dose TBI: a single-center retrospective analysis of 103 cases. Int J Hematol. 2013;98(5):608–14.
Kuriyama K, Fuji S, Inamoto Y, Tajima K, Tanaka T, Inoue Y, et al. Impact of low-dose rabbit anti-thymocyte globulin in unrelated hematopoietic stem cell transplantation. Int J Hematol. 2016;103(4):453–60.
Remberger M, Svahn BM, Mattsson J, Ringden O. Dose study of thymoglobulin during conditioning for unrelated donor allogeneic stem-cell transplantation. Transplantation. 2004;78(1):122–7.
Hamadani M, Blum W, Phillips G, Elder P, Andritsos L, Hofmeister C, et al. Improved nonrelapse mortality and infection rate with lower dose of antithymocyte globulin in patients undergoing reduced-intensity conditioning allogeneic transplantation for hematologic malignancies. Biol Blood Marrow Transplant. 2009;15(11):1422–30.
Kennedy VE, Chen H, Savani BN, Greer J, Kassim AA, Engelhardt BG, et al. Optimizing antithymocyte globulin dosing for unrelated donor allogeneic hematopoietic cell transplantation based on recipient absolute lymphocyte count. Biol Blood Marrow Transplant. 2018;24(1):150–5.
Landgren O, Gilbert ES, Rizzo JD, Socie G, Banks PM, Sobocinski KA, et al. Risk factors for lymphoproliferative disorders after allogeneic hematopoietic cell transplantation. Blood. 2009;113(20):4992–5001.
Zander AR, Kroger N, Schleuning M, Finke J, Zabelina T, Beelen D, et al. ATG as part of the conditioning regimen reduces transplant-related mortality (TRM) and improves overall survival after unrelated stem cell transplantation in patients with chronic myelogenous leukemia (CML). Bone Marrow Transplant. 2003;32(4):355–61.
Kim HJ, Min WS, Cho BS, Eom KS, Kim YJ, Min CK, et al. Successful prevention of acute graft-versus-host disease using low-dose antithymocyte globulin after mismatched, unrelated, hematopoietic stem cell transplantation for acute myelogenous leukemia. Biol Blood Marrow Transplant. 2009;15(6):704–17.
Kawamura K, Kanda J, Fuji S, Murata M, Ikegame K, Yoshioka K, et al. Impact of the presence of HLA 1-locus mismatch and the use of low-dose antithymocyte globulin in unrelated bone marrow transplantation. Bone Marrow Transplant. 2017;52(10):1390–8.
Soiffer RJ, Lerademacher J, Ho V, Kan F, Artz A, Champlin RE, et al. Impact of immune modulation with anti-T-cell antibodies on the outcome of reduced-intensity allogeneic hematopoietic stem cell transplantation for hematologic malignancies. Blood. 2011;117(25):6963–70.
Baron F, Labopin M, Niederwieser D, Vigouroux S, Cornelissen JJ, Malm C, et al. Impact of graft-versus-host disease after reduced-intensity conditioning allogeneic stem cell transplantation for acute myeloid leukemia: a report from the Acute Leukemia Working Party of the European Group for Blood and Marrow Transplantation. Leukemia. 2012;26(12):2462–8.
Remberger M, Ringden O, Hagglund H, Svahn BM, Ljungman P, Uhlin M, et al. A high antithymocyte globulin dose increases the risk of relapse after reduced intensity conditioning HSCT with unrelated donors. Clin Transplant. 2013;27(4):E368–74.
Devillier R, Labopin M, Chevallier P, Ledoux MP, Socie G, Huynh A, et al. Impact of antithymocyte globulin doses in reduced intensity conditioning before allogeneic transplantation from matched sibling donor for patients with acute myeloid leukemia: a report from the acute leukemia working party of European Group of Bone Marrow Transplantation. Bone Marrow Transplant. 2018;53(4):431–7.
Schattenberg A, van der Meer A, Preijers F, Schaap N, Rinkes M, van der Maazen R, et al. Addition of ATG to the conditioning regimen is a major determinant for outcome after transplantation with partially lymphocyte-depleted grafts from voluntary unrelated donors. Bone Marrow Transplant. 2004;33(11):1115–21.
Oh H, Loberiza FR Jr., Zhang MJ, Ringden O, Akiyama H, Asai T, et al. Comparison of graft-versus-host-disease and survival after HLA-identical sibling bone marrow transplantation in ethnic populations. Blood. 2005;105(4):1408–16.
Morishima Y, Kawase T, Malkki M, Morishima S, Spellman S, Kashiwase K, et al. Significance of ethnicity in the risk of acute graft-versus-host disease and leukemia relapse after unrelated donor hematopoietic stem cell transplantation. Biol Blood Marrow Transplant. 2013;19(8):1197–203.
Kanda J, Brazauskas R, Hu ZH, Kuwatsuka Y, Nagafuji K, Kanamori H, et al. Graft-versus-host disease after HLA-matched sibling bone marrow or peripheral blood stem cell transplantation: comparison of North American Caucasian and Japanese populations. Biol Blood Marrow Transplant. 2016;22(4):744–51.
Passweg JR, Baldomero H, Bader P, Bonini C, Cesaro S, Dreger P, et al. Hematopoietic stem cell transplantation in Europe 2014: more than 40 000 transplants annually. Bone Marrow Transplant. 2016;51(6):786–92.
Khera N, Mau LW, Denzen EM, Meyer C, Houg K, Lee SJ, et al. Translation of clinical research into practice: an impact assessment of the results from the blood and marrow transplant clinical trials network protocol 0201 on unrelated graft source utilization. Biol Blood Marrow Transplant. 2018;24(11):2204–10.
Eapen M, Logan BR, Confer DL, Haagenson M, Wagner JE, Weisdorf DJ, et al. Peripheral blood grafts from unrelated donors are associated with increased acute and chronic graft-versus-host disease without improved survival. Biol Blood Marrow Transplant. 2007;13(12):1461–8.
Anasetti C, Logan BR, Lee SJ, Waller EK, Weisdorf DJ, Wingard JR, et al. Peripheral-blood stem cells versus bone marrow from unrelated donors. N Engl J Med. 2012;367(16):1487–96.
Admiraal R, Nierkens S, de Witte MA, Petersen EJ, Fleurke GJ, Verrest L, et al. Association between anti-thymocyte globulin exposure and survival outcomes in adult unrelated haemopoietic cell transplantation: a multicentre, retrospective, pharmacodynamic cohort analysis. Lancet Haematol. 2017;4(4):e183–e191.
Basara N, Baurmann H, Kolbe K, Yaman A, Labopin M, Burchardt A, et al. Antithymocyte globulin for the prevention of graft-versus-host disease after unrelated hematopoietic stem cell transplantation for acute myeloid leukemia: results from the multicenter German cooperative study group. Bone Marrow Transplant. 2005;35(10):1011–1018
Mohty M, Labopin M, Balere ML, Socie G, Milpied N, Tabrizi R, et al. Antithymocyte globulins and chronic graft-vs-host disease after myeloablative allogeneic stem cell transplantation from HLA-matched unrelated donors: a report from the Societe Francaise de Greffe de Moelle et de Therapie Cellulaire. Leukemia. 2010;24(11):1867–74.
Acknowledgements
This work was supported in part by the Japan Leukemia Research Fund. The author is grateful to Drs. Yoshinobu Kanda (Jichi Medical University) and Junya Kanda (Kyoto University) for their suggestions and advice.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Kawamura, K. Effect of antithymocyte globulin on HLA-mismatched unrelated transplantation. Int J Hematol 110, 22–29 (2019). https://doi.org/10.1007/s12185-019-02597-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-019-02597-y