Summary
Synopsis: Verapamil is a novel antiarrhythmic and antianginal agent which, although introduced in 1962, has only recently gained prominence not only as a significant agent in cardiovascular therapeutics but also as a powerful tool to examine the nature of some of the biophysical phenomena at the membrane of cardiac and other excitable tissues. Verapamil is the prototype of those agents which selectively inhibit membrane transport of calcium, an action which accounts for the drug’s peripheral and coronary vasodilator properties, its effect on excitation-contraction coupling and hence its negative inotropic propensity, as well as its depressant effects on the sinus node and atrioventricular conduction. Its pharmacological effects are largely independent of the autonomic nervous system. The main therapeutic uses of the drug are in the management of atrial tachyarrhythmias, angina, and possibly hypertension. The overall experimental and clinical data suggest that verapamil will become an important and safe addition to existing drug regimens, especially as an agent of choice for the short-term treatment of most cases of paroxysmal supraventricular tachycardias. The initial experience in other arrhythmias, angina and hypertension, is also sufficiently encouraging to justify further detailed clinical trials to define its potential role in cardiovascular therapeutics.
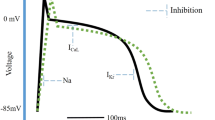
Pharmacodynamic Properties: Verapamil is a weak local anaesthetic; it does not depress the upstroke velocity of the cardiac action potential, nor does it prolong the action potential duration in heart muscle. It selectively depresses nodal tissues, presumably by an effect on the calcium-mediated slow response, an action distinct from that of all other antiarrhythmic agents.
Pharmacokinetics: Preliminary pharmacokinetic studies reveal major discrepancies between the duration of the electrophysiological and haemodynamic effects of verapamil and the presence of unchanged drug in the plasma, raising the possibility of active metabolites. Plasma protein binding of verapamil approaches approximately 90%. Despite almost complete gastrointestinal absorption following oral administration, the overall bioavailability of the drug is about 10 to 22% reflecting substantial first pass hepatic metabolism which may account for the 8 to 10-fold greater oral compared with intravenous doses needed to produce comparable pharmacodynamic effects.
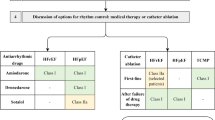
Therapeutic Trials: The antiarrhythmic effects of verapamil are explained largely by its action on the atrioventricular node: intravenously administered verapamil (10mg in adults, 3.5 to 5mg in children) produces prompt reversion to sinus rhythm of 80 to 100% of cases with paroxysmal supraventricular tachycardias, especially those due to AV nodal re-entry. The drug has little effect on the anomalous pathways in the Wolff-Parkinson-White syndrome so that atrial fibrillation or flutter complicating this disorder are not affected by verapamil, in contrast to other cases of atrial fibrillation or flutter in which the ventricular response is consistently reduced in most cases and sinus rhythm restored in a few. The role of oral verapamil used alone or in combination with other agents in the prophylaxis of paroxysmal supraventricular tachycardias and in the maintenance of sinus rhythm following cardioversion of atrial fibrillation remains to be defined. Verapamil is of little value in the control of ventricular arrhythmias.
Verapamil is also effective in angina pectoris in doses in excess of 120mg 3 times daily orally. At this dose schedule, its efficacy is comparable with that of 80mg 3 times daily of oral propranolol, although the latter produces a significant degree of bradycardia whereas verapamil does not. The mode of antianginal action of verapamil is therefore not understood, but unlike propranolol the drug has no effects on lung function. Experimental studies suggest that verapamil might reduce myocardial infarct size and preliminary clinical studies raise the possibility that the drug may be of value in the management of acute hypertensive crisis as well as of treatment of essential hypertension.
Side-effects: Orally administered verapamil is extremely well tolerated and few side-effects have been encountered following intravenous administration of the drug, especially when it is given slowly. Transient hypotension and prolongation of AV conduction time or even AV dissociation may occasionally be seen. Haemodynamic effects in patients with cardiac disease include short-lived decreases in mean arterial pressure, first derivative of the left ventricular pressure, systemic resistance and a rise in left ventricular filling pressure, but with little change in stroke volume, cardiac index or heart rate. Rarely, severe hypotension, bradycardia, or asystole have been reported, most cases occurring in patients previously treated with β-adrenoceptor blocking drugs.
Precautions: Prior digitalisation is not a contraindication to the use of intravenous or oral verapamil, except in the case of the sick sinus syndrome in which verapamil alone or in combination with other depressant drugs which influence automaticity or conduction may produce severe bradycardia or atrioventricular block. The drug is also contraindicated in unstable atrioventricular block, heart failure (especially that complicating acute myocardial infarction), cardiogenic shock or other hypotensive states. Side-effects resulting from verapamil may be reversed, at least in part, by atropine, isoprenaline, intravenous calcium or glucagon, with ventricular pacing being required occasionally.
Similar content being viewed by others
References
Andreasen, F.; Boye, E.; Christoffersen D.; et al.: Assessment of verapamil in the treatment of angina pectoris. European Journal of Cardiology 2: 443–452 (1975)
Angus, J.A.; Dhumma-Upahorn, P.; Cobbin, L.B. and Goodman, A.H.: Cardiovascular action of verapamil in the dog with particular reference to myocardial contractility and atrioventricular conduction. Cardiovascular Research 10: 623–632 (1976)
Appel, W.: Alpha-isopropyl-alpha (methyl-N-homoveratryl)-gamma-aminopropyl-3, 4-dimethoxyphenyl-acetonitrile. Its demonstration in biological material and its behavior in the blood. Arzneimittel-Forschung. 12: 562–566 (1962)
Aronson, R.S. and Cranefield, P.F.: Electrical activity of canine Purkinje fiber in Na-free Ca-rich solutions. Journal of General Physiology 61: 786–791 (1973)
Attehog, J.H. and Ekelund, L.G: Haemodynamic effects of intravenous verapamil at rest and during exercise in subjectively healthy middle aged males. European Journal of Clinical Pharmacology 8: 317–322 (1975)
Balasubramanian, V.; Khanna, P.K.; Naryanan, G.R. and Hoon, R.S.: Verapamil in ischemic heart disease — quantitative assessment by serial multistage treadmill exercise. Postgraduate Medical Journal 52: 143–147 (1976)
Bateman, F.J.A.: What is a beta blocker? Lancet 1: 419 (1967)
Benaim, M.E.: Asystole after verapamil. British Medical Journal 2: 169–170 (1972)
Bender, F.: Die Behandlung das tachycarden arrhythmien und der arteriellen hypertonie mit verapamil. Arzneimittel-Forschung. 20: 1310–1325 (1970)
Boothby, C.B.; Garrard, C.S. and Pickering, D.: Intravenous verapamil in cardiac arrhythmias. British Medical Journal 2: 349 (1972)
Breithardt G.; Ludger, S.; Eberhard, W. and Loogen, F.: Effect of verapamil on sinus node in patients with normal and abnormal sinus node function. Circulation 54 (Suppl. 2): II–19 (1976)
Brichard, G. and Zimmerman, P.G.: Verapamil in cardiac dysarrhythmias during anaesthesia. British Journal of Anaethesiology 42: 1005–1011 (1970)
Brittinger, W.D.; Schwarzbeck, A.; Wittenmeier, K.W.; Turtkenhoff, W.D.; Stegaru, B.; Huber, W.; Ewald, R.W.; Henning, G.E.V.; Fabricius, M. and Strauch, M.: Klinisch-experimentelle Untersuchungen uber die blutdruckenkende Wirkung von Verapamil. Deutsche Medizinische Wochenschrift 95: 1871–1877 (1970)
Carleton, R.A. and Johnson, A.D.: Coronary arterial spasm. A clinical entity? Modern Concepts in Cardiovascular Disease 43: 87–91 (1974)
Cranefield, P.F.: The Conduction of the Cardiac Impulse (Futura, New York 1975)
Cranefield, P.F.; Aronson, R.S. and Wit, A.L.: Effect of verapamil on the normal action potential and on a calcium-dependent slow response of canine cardiac Purkinje fibers. Circulation Research 34: 204–213 (1974)
Donnelly, G.L. and Scamps, P.: Intravenous verapamil in cardiac arrhythmias (abstract). Australian and New Zealand Journal of Medicine 3: 63 (1973)
Entman, M.L.; Allen, J.C.; Bornet, E.P.; Gillette, P.C.; Wallick, E.T. and Schwartz, A.: Mechanisms of calcium accumulation and transport in cardiac relaxing system (sarcoplasmic reticulum membranes): Effects of verapamil, D-600, X537A and A23187. Journal of Molecular and Cellular Cardiology 4: 681–692 (1972)
Esser, W.; Herms, W. and Wetzels, E.: Die Wirkung verschiedener koronardilatierender Pharmaka auf die Nirenfunktion; in Watschinger (Ed) VI Symposium der Gesellschaft fur Nephrologie, p.593 (Verlag der Wiender Medizinischen Akademie, Wien 1969)
Fleckenstein, A.: Specific inhibitors and promoters of calcium action in the excitation-contraction coupling of heart muscle and their role in the prevention or production of myocardial lesions; in Calcium and the Heart (Academic Press, London 1970)
Fleckenstein, A.; Tritthart, H.; Fleckenstein, B.; Herbst, A. and Grun, G.: Eine neue Gruppe kompetitiuer Ca++ — Antagonisten (Iproveratril, D600, Prenylamin) mit starken Hemmeffekten auf die elektromechanische Koppelung im Warmblutermyokard. Pflugers Archiv fur de gasamte Physiologie des Menschen und de Tiere 307: 25–32 (1969)
Garvey, H.L.: The mechanism of action of verapamil on the sinus and AV nodes. European Journal of Pharmacology 8: 159–165 (1969)
Gibson, D. and Sowton, E.: The use of beta-adrenergic receptor blocking drugs in dysarrhythmias. Progress in Cardiovascular Diseases 12: 16–39 (1969)
Goldreyer, B.N.: Intracardiac electrocardiography in the analysis and understanding of cardiac arrhythmias. Annals of Internal Medicine 77: 117–136 (1972)
Golenhofen, K. and Lammel, E.: Selective suppression of some components of spontaneous activity in various types of smooth muscle by iproveratril (verapamil). Pflugers Archiv fur de gesamte Physiologie des Menschen und de Tiere 331: 233–243 (1972)
Gotsman, M.; Lewis, B.; Bakst, A. and Mitha, A.: Verapamil in life-threatening tachyarrhythmias. South African Medical Journal 46: 2017–2019 (1972)
Greenberg, S. and Wilson, W.R.: Iproveratril: A non-specific antagonist of peripheral vascular reactivity. Canadian Journal of Physiology and Pharmacology 52: 266–271 (1974)
Grendahl, H.; Miller, M. and Sivertssen, E.: Registration of sinus node recovery time in patients with sinus rhythm and in patients with dysrhythmias. Acta Medica Scandinavica 197: 403–408 (1975)
Haas, H. and Hartfelder, G.: α-Isopropyl-α-[N-methyl-N-homoveratryl-α-amino propyl]-3-4 dimethoxyphenylacetonitril, eine Aulstanz mit coronasgefassen Eigenschaften. Arzneimittel-Forschung 12: 549–558 (1962)
Haeusler, G.: Differential effect of verapamil on excitation-contraction coupling in smooth muscle and on excitation-secretion coupling in adrenergic terminals. Journal of Pharmacology and Experimental Therapeutics 180: 672–679 (1972)
Hartel, G. and Hartikainen, M.: Comparison of verapamil and practolol in paroxysmal supraventricularstachycardia. European Journal of Cardiology 4: 87–90 (1976)
Heng, M.K.; Singh, B.N.; Roche, A.H.G.; Norris, R.M. and Mercer, C.J.: Effects of intravenous verapamil on cardiac arrhythmias and on the electrocardiogram. American Heart Journal 90: 487–498 (1975)
Hills, E.A.: Iproveratril and bronchial asthma. British Journal of Clinical Practice 24: 116–117 (1970)
Hoffman, P.: Behandlung koronarer Durchblutungsstorungen mit Isoptin in der Praxis. Medizinische Klinik 59: 1387–1390 (1964)
Husaini, M.H.; Kurasnicka, J.; Ryden, L. and Holmberg, S.: Action of verapamil on sinus node, atrioventricular, and intraventricular conduction. British Heart Journal 35: 734–737 (1973)
Kaumann, A.J. and Aramendia, P.: Prevention of ventricular fibrillation induced by coronary ligation. Journal of Pharmacology and Experimental Therapeutics 164: 326–340 (1968)
Kohlhardt, M.; Bauer, B.; Krause, H. and Fleckenstein, A.: New selective inhibitors of the transmembrane Ca conductivity in mammalian myocardial fibers. Studies with the voltage clamp technique. Experimenta 28: 288–289 (1972)
Krikler, D.M.: Verapamil in cardiology. European Journal of Cardiology 2: 3–10 (1974)
Krikler, D.M. and Spurrell, R.A.J.: Verapamil in the treatment of paroxysmal supraventricular tachycardia. Postgraduate Medical Journal 50: 447–453 (1974)
Lewis, B.; Mitha, A. and Gotsman, M.: Immediate haemodynamic effects of verapamil in man. Cardiology 60: 366–376 (1976)
Livesley, B.; Catley, P.F.; Campbell, R.C. and Oram, S.: Double blind evaluation of verapamil, propranolol and isosorbide dinitrate against a placebo in the treatment of angina pectoris. British Medical Journal 1: 375–378 (1973)
Luebs, E.D.; Cohen, A.; Zaleski, E.J. and Bing, R.J.: Report on therapy: Effect of nitroglycerin, intensain, isoptin and papaverine on coronary blood flow in man. American Journal of Cardiology 17: 535–541 (1966)
McAllister, R.G. and Howell, S.M.: Fluorometric assay of verapamil in biological fluids and tissues. Journal of Pharmaceutical Sciences 65: 431–432 (1976)
McHenney, H.M.: Metabolism of 14C-verapamil. Journal of Medical Chemistry 14: 1178–1184 (1971)
Melville, K.I. and Benfey, B.C.: Coronary vasodilatory and cardiac adrenergic blocking effects of iproveratril. Canadian Journal of Physiology and Pharmacology 43: 339–342 (1965)
Melville, K.I.; Shister, H.E. and Huq, S.: Iproveratril: Experimental data on coronary-dilatation and antiarrhythmic action. Canadian Medical Association Journal 90: 761–770 (1964)
Mignault S.H.: Coronary cineangiographic study of intravenously administered isoptin. Canadian Medical Association Journal 95: 1252–1253 (1966)
Nayler, W.; Grau, A. and Slade, A.: A protective effect of verapamil on hypoxic heart muscle. Cardiovascular Research 10: 650–662 (1976)
Nayler, W. and Krikler, D.: Verapamil and the myocardium. Postgraduate Medical Journal 50: 441–446 (1974)
Nayler, W.G.; McInnes, L; Swann, J.B.; Carson, V. and Lowe, T.E.: Effect of propranolol, a beta adrenergic antagonist on blood flow in the coronary and other vascular fields. American Heart Journal 73: 207–216 (1967)
Nayler, W.G.; McInnes, I.; Swann, J.B.; Price, J.M.; Carson, V.; Race, D. and Lowe, T.E.: Some effects of iproveratril (isoptin) on the cardiovascular system. Journal of Pharmacology and Experimental Therapeutics 161: 247–261 (1968)
Nayler, W.G. and Szeto, J.: Effect of verapamil on contractility, oxygen utilisation and calcium exchangeability in mammalian heart muscle. Cardiovascular Research 6: 120–128 (1972)
Neumann, M. and Luisada, A.A.: Studies of iproveratril on oral administration in double blind trials in patients with angina pectoris. American Journal of Medical Sciences 251: 552–556 (1966)
Neuss, H.; Nowak, F.G.; Schlepper, M. and Wusten, B.: The effects of anti-anginal drugs on AV conduction in normal subjects. Arzneimittel-Forschung 24: 213–216 (1974)
Neuss, H. and Schlepper, M: Influence of various antiarrhythmic drugs (aprindine, ajmaline, verapamil, oxprenolol, orciprenaline) on functional properties of accessory AV pathways. Acta Cardiologica (Suppl.) 18: 279–288 (1974)
Okada, T: Effect of verapamil on electrical activities of SA node, ventricular muscle, and Purkinje fibers in isolated rabbit hearts. Japan Circulation Journal 40: 329–341 (1976)
Puech, P.: Dissection de la conduction sinoventriculaire pour l’etude du verapamil injectable. Centre Hospitalier, Montpellier (1972) Cited in Krikler (1974)
Reimer, K.A.; Lowe, J.E. and Jennings, R.B.: Effect of the calcium antagonist verapamil on necrosis following temporary coronary artery occlusion in dogs. Circulation 55: 581–587 (1977)
Rodriguez-Pereira, E. and Viana, A.P.: The actions of verapamil on experimental arrhythmias. Arzneimittel-Forschung 18: 175–179 (1968)
Rosen, M.R.; Wit, A.L. and Hoffman, B.F.: Appraisal and reappraisal of cardiac therapy. Electrophysiology and pharmacology of cardiac arrhythmias. VI. Cardiac effects of verapamil. American Heart Journal 89: 665–673 (1976)
Ross, G. and Jorgensen, C.R.: Cardiovascular action of iproveratril. Journal of Pharmacology and Experimental Therapeutics 158: 504–509 (1967)
Roy, P.R.; Spurrell, R.A.J. and Sowton, G.E.: The effect of verapamil on the conduction system in man. Postgraduate Medical Journal 50: 270–275 (1974)
Ryden, L. and Saetre, H.: The haemodynamic effect of verapamil. European Journal of Clinical Pharmacology 3: 153–157 (1971)
Sacks, H. and Kennelly, B.M.: Verapamil in cardiac arrhythmias. British Medical Journal 2: 716–721 (1972)
Sandler, G.; Clayton, G.A. and Thornicroft, S.: Clinical evaluation of verapamil in angina pectoris. British Medical Journal 3: 224–227 (1968)
Schamroth, L.: Immediate effects of intravenous verapamil on atrial fibrillation. Cardiovascular Research 5: 419–424 (1971)
Schamroth, L.; Krikler, D.M. and Garrett, C.: Immediate effects of intravenous verapamil in cardiac arrhythmias. British Medical Journal 1: 660–664 (1972)
Schlepper, M.; Thormann, I. and Schwarz, F.: The pharmacodynamics of orally taken verapamil and verapamil retard as judged by negative dromotropic effects. Arzneimittel-Forschung 25: 1452–1455 (1975)
Schlepper, M. and Witzlei, E.: Tierexperimentelle Untersuchungen uber die Veranderungen von Coronarduchblung und Sauerstoffuesbrauch des Herzens nach α-Isopropyl-α-[N-methyl-N-methyl-N-homoveratryl]-γ aminopropyl-3, 4-di-methoxyphenylacetonitrile. Arzneimittel-Forschung 12: 559–563 (1962)
Schmitt, G.: Uber die protektive Wirkung von Iproveratril bei hypertonie bedingten Myokarderkrankungen im Tierexperiment. Medizinische Welt 18: 2943–2949(1967)
Schmid, J.R. and Hanna C.: A comparison of the antiarrhythmic actions of two new synthetic compounds, iproveratril and MJ 1999, with quinidine and pronethalol. Journal of Pharmacology and Experimental Therapeutics 156: 331–338 (1967)
Schomerus, M.; Spiegelhalder, B.; Stieren, B. and Eichelbaum, M.: Physiological disposition of verapamil in man. Cardiovascular Research 10: 605–612 (1976)
Seabra-Gomes, R.; Rickards, A. and Sutton, R.: Hemodynamic effects of verapamil and practolol in man. European Journal of Cardiology 4: 79–85 (1976)
Shand, D.G. and Ragno, R.E.: The disposition of propranolol: Elimination during oral absorption in man. Pharmacology 7: 159–168(1972)
Shigenobu, K.; Schneider, J.A. and Sperelakis, N.: Verapamil blockade of slow Na+ and Ca++ responses in myocardial cells. Journal of Pharmacology and Experimental Therapeutics 190: 280–288 (1974)
Singh, B.N.: A study of the pharmacological actions of certain drugs and hormones with particular reference to cardiac muscle. D.Phil. Thesis, University of Oxford, England(1971)
Singh, B.N.: Verapamil and the heart: Pharmacological and therapeutic considerations. New Zealand Medical Journal 82: 339–343(1975)
Singh, B.N. and Roche, A.H.G.: Effects of intravenous verapamil on hemodynamics in patients with heart disease. American Heart Journal. In press (1977)
Singh, B.N.; Smith, H.J. and Norris, R.M.: Reduction in infarct size following experimental coronary occlusion by administration of verapamil; in Roy and Roma (Eds) The Metabolism of Contraction, pp.435–452 (University Park Press, Baltimore 1975)
Singh, B.N. and Vaughan Williams, E.M.: The effect of amiodarone. A new anti-anginal drug on cardiac muscle. British Journal of Pharmacology 39: 657–668 (1970)
Singh, B.N. and Vaughan Williams, E.M.: Effect of altering potassium concentration on the action of lidocaine and diphenylhydantoin on rabbit and ventricular muscle. Circulation Research 29: 286–297 (1971)
Singh, B.N. and Vaughan Williams, E.M.: A fourth class of anti-dysrhythmic action? Effect of verapamil on ouabain toxicity on atrial and ventricular intracellular potentials and on other features of cardiac function. Cardiovascular Research 6: 109–119 (1972)
Smith, H.J.; Singh, B.N.; Nisbet, H.D. and Norris, R.M.: Effects of verapamil on infarct size following experimental coronary occlusion. Cardiovascular Research 9: 569–578 (1975)
Smith, H.J.; Singh, B.N.: Norris, R.M.; Nisbet, H.D.; John, M.B. and Hurley, P.J.: The effect of verapamil on experimental myocardial ischaemia with a particular reference to regional myocardial blood flow and metabolism. Australian and New Zealand Journal of Medicine 7: 114–121 (1977)
Sodi-Pallares, D.; Bisteni, A.; Medrano, G.A.; de Leon, J.P.; de Michelli, A. and Ariza, D.: El efecto del verapamil (iproveratril) sobre los caimbios electrocardiograficos y de contraccion observados en el corazon del perro despues de la ligdura de la coronaria descendente anterior. Revista Peruana de Cardiologia 14: 3–12 (1968)
Spurrell, R.A.J.; Krikler, D.M. and Sowton, G.E.: The effect of verapamil on the electrophysiological properties of the anomalous atrioventricular connexions in Wolff-Parkinson-White syndrome. British Heart Journal 36: 256–257 (1974a)
Spurrell, R.A.J.; Krikler, D.M. and Sowton, G.E.: Concealed bypasses of the atrioventricular node in patients with paroxysmal supraventricular tachycardia revealed by intracardiac electrical stimulation and verapamil. American Journal of Cardiology 33: 590–595 (1974b)
Storstein, O. and Landmark, K.H.: Verapamil in the treatment of atrial tachycardia with block. Acta Medica Scandinavica 198: 483–488 (1975)
Storstein, O. and Rasmussen, K.: Digitalis and atrial tachycardia with block. British Heart Journal 36: 171–176 (1974)
Tschirdewahn, B. and Klepzig, H.: Klinische Untersuchung uber die Wirkung von Ioptin und Ioptin S bei Patienten mit Koronarinsuffizienz. Deutsche Medizinsche Wochenschrift 88: 1702–1710 (1963)
Vohra, I.; Peter, C.T.; Hunt, D. and Sloman, G.: Verapamil induced premature ventricular beats before reversion of supraventricular tachycardia. British Heart Journal 36: 1186–1193 (1974a)
Vohra, I.; Hunt, D; Stuckey, J. and Sloman, G.: Cycle length alternation in supraventricular tachycardia after administration of verapamil. British Heart Journal 36: 570–576 (1974b)
Vohra, J.; Sloman, G. and Hunt, D.: Antiarrhythmic and hemodynamic properties of verapamil. (abstract). Australian and New Zealand Journal of Medicine 4: 102 (1974c)
Wellens, H.J.J. and Durrer, D.: Effect of digitalis on atrioventricular conduction and circus movement tachycardias in patients with the Wolff-Parkinson-White syndrome. Circulation 47: 1229–1238 (1973)
Winbury, M.M.; Howe, B.B. and Hefner, M.A.: Effect of nitrates and other coronary dilators on large and small coronary vessels: an hypothesis for the mechanism of action of nitrates. Journal of Pharmacology and Experimental Therapeutics 168: 70–95 (1969)
Wit, A.L. and Cranefield, P.: Effect of verapamil on the sinoatrial and atrioventricular nodes of the rabbit and the mechanism by which it arrests re-entrant atrioventricular nodal tachycardia. Circulation Research 35: 413–425 (1974)
Wit, A.L.; Fenoglio, J.J.; Wagner, B.M. and Bassett, A.L.: Electrophysiological properties of cardiac muscle in the anterior mitral valve leaflet and adjacent atrium of the dog: Possible implications for the genesis of atrial arrhythmias. Circulation Research 32: 731–738 (1973)
Zipes, D.P. and Fischer, J.C.: Effects of agents which inhibit the slow channel on sinus node automaticity and atrioventricular conduction in the dog. Circulation Research 34: 184–192 (1974)
Author information
Authors and Affiliations
Additional information
Supported in part by the SCOR Grant No. HL17651, National Institute of Health, Bethesda, Maryland.
Isoptin (Knoll AG): Cordilox (Abbott).
Rights and permissions
About this article
Cite this article
Singh, B.N., Ellrodt, G. & Peter, C.T. Verapamil: A Review of its Pharmacological Properties and Therapeutic Use. Drugs 15, 169–197 (1978). https://doi.org/10.2165/00003495-197815030-00001
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-197815030-00001