Abstract
Background
Laparoscopic splenectomy has gained popularity in the management of children with benign hematological disease who required splenectomy. We aim to report the outcome after standardization of techniques in laparoscopic splenectomy.
Materials and methods
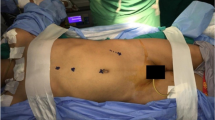
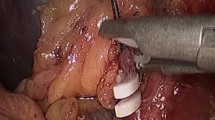
A retrospective study was conducted in which all children with benign hematological disease underwent laparoscopic splenectomy in our institute from 2003 to 2017. The demographics and outcomes before (Group 1) and after (Group 2) standardization of techniques were compared. The laparoscopic techniques were standardized in Group 2. They all underwent multiport laparoscopic splenectomy and the splenic pedicles were divided by bipolar sealing device (LigaSure). In Group 1, splenectomy could be performed by single port or multiple ports approach. The splenic pedicles could be divided by endovascular stapler or LigaSure.
Results
Group 1 included 14 children who underwent splenectomy from 2003 to 2010 and Group 2 included 9 children who were operated from 2011 to 2017. The demographics were comparable between the two groups. Group 2 was associated with lower complication (0 vs. 5, p = 0.043), shorter operative time in splenectomy (146 min vs. 173 min, p = 0.056) and shorter mean hospital stay (3.8 days vs. 7.1 days, p < 0.0001).
Conclusions
Superior outcomes including lower complication rates and shorter hospital stay were observed after standardization of surgical techniques in laparoscopic splenectomy in children using multiple ports and LigaSure.


Similar content being viewed by others
References
Rice HE, Englum BR, Rothman J, Leonard S, Reiter A, Thornburg C et al (2015) Splenectomy in Congenital Hemolytic Anemia (SICHA) Consortium. Clinical outcomes of splenectomy in children: report of the splenectomy in congenital hemolytic anemia registry. Am J Hematol 90:187–192
Ahmed R, Devasia AJ, Viswabandya A, Lakshmi KM, Abraham A, Karl S, Mathai J et al (2016) Long-term outcome following splenectomy for chronic and persistent immune thrombocytopenia (ITP) in adults and children: splenectomy in ITP. Ann Hematol 95:1429–1434
Murawski M, Patkowski D, Korlacki W, Czauderna P, Sroka M, Makarewicz W et al (2008) Laparoscopic splenectomy in children—a multicenter experience. J Pediatr Surg 43:951–954
Rescorla FJ, West KW, Engum SA, Grosfeld JL (2007) Laparoscopic splenic procedures in children: experience in 231 children. Ann Surg 246:683–687
Feng S, Qiu Y, Li X, Yang H, Wang C, Yang J et al (2016) Laparoscopic versus open splenectomy in children: a systematic review and meta-analysis. Pediatr Surg Int 32:253–259
Li S, Li M, Xu W, Sun C, Liu L (2015) Single-incision laparoscopic splenectomy using the suture suspension technique for splenomegaly in children with hereditary spherocytosis. J Laparoendosc Adv Surg Tech A 25:770–774
Tam YH, Lee KH, Chan KW, Sihoe JD, Cheung ST, Pang KK (2010) Technical report on the initial cases of single-incision laparoscopic combined cholecystectomy and splenectomy in children, using conventional instruments. Surg Innov 17:264–268
Giza DE, Tudor S, Purnichescu-Purtan RR, Vasilescu C (2014) Robotic splenectomy: what is the real benefit? World J Surg 38:3067–3073
Shabahang H, Maddah G, Tavassoli A, Jangjoo A, Alvandipour M, Abdollahi A et al (2012) Laparoscopic splenectomy: ligasure or clip ligation? Surg Laparosc Endosc Percutan Tech 22(2):136–138
Danielson PD, Shaul DB, Phillips JD, Stein JE, Anderson KD (2000) Technical advances in pediatric laparoscopy have had a beneficial impact on splenectomy. J Pediatr Surg 35:1578–1581
Romano F, Gelmini R, Caprotti R, Andreotti A, Guaglio M, Franzoni C, Uggeri F et al (2007) Laparoscopic splenectomy: ligasure versus EndoGIA: a comparative study. J Laparoendosc Adv Surg Tech A 17:763–767
Guaglio M, Romano F, Garancini M, Degrate L, Luperto M, Uggeri F et al (2012) Is expertise in pediatric surgery necessary to perform laparoscopic splenectomy in children? An experience from a department of general surgery. Updates Surg 64:119–123
Zhu J, Ye H, Wang Y, Zhao T, Zhu Y, Xie Z et al (2011) Laparoscopic versus open pediatric splenectomy for massive splenomegaly. Surg Innov 18:349–353
Qureshi FG, Ergun O, Sandulache VC, Nadler EP, Ford HR, Hackam DJ et al (2005) Laparoscopic splenectomy in children. JSLS 9:389–392
Oomen MW, Bakx R, van Minden M, van Rijn RR, Peters M, Heij HA et al (2013) Implementation of laparoscopic splenectomy in children and the incidence of portal vein thrombosis diagnosed by ultrasonography. J Pediatr Surg 48:2276–2280
Tulman S, Holcomb GW 3rd, Karamanoukian HL, Reynhout J (1993) Pediatric laparoscopic splenectomy. J Pediatr Surg 28:689–692
Vargün R, Göllü G, Fitöz S, Yagmurlu A (2007) En-bloc stapling of the splenic hilum in laparoscopic splenectomy. Minim Invas Ther Allied Technol 16:360–362
Schaarschmidt K, Kolberg-Schwerdt A, Lempe M, Saxena A (2002) Ultrasonic shear coagulation of main hilar vessels: a 4-year experience of 23 pediatric laparoscopic splenectomies without staples. J Pediatr Surg 37:614–616
Fujioka S, Yoshida K, Okamoto T, Yanaga K (2013) Stapleless laparoscopic splenectomy using harmonic scalpel by 2-step sealing. Int Surg 98:385–387
Gelmini R, Romano F, Quaranta N, Caprotti R, Tazzioli G et al (2006) Sutureless and stapleless laparoscopic splenectomy using radiofrequency: LigaSure device. Surg Endosc 20:991–994
Romano F, Caprotti R, Franciosi C, De Fina S, Colombo G, Sartori P et al (2003) The use of LigaSure during pediatric laparoscopic splenectomy: a preliminary report. Pediatr Surg Int 19:721–724
Tam YH, Lee KH, Sihoe JD, Chan KW, Cheung ST, Pang KK (2010) Initial experience in children using conventional laparoscopic instruments in single-incision laparoscopic surgery. J Pediatr Surg 45:2381–2385
Scerbo MW, Britt RC, Stefanidis D (2017) Differences in mental workload between traditional and single-incision laparoscopic procedures measured with a secondary task. Am J Surg 213:244–248
Koca D, Yıldız S, Soyupek F, Günyeli İ, Erdemoglu E, Soyupek S et al (2015) Physical and mental workload in single-incision laparoscopic surgery and conventional laparoscopy. Surg Innov 22:294–302
Chan KW, Lee KH, Tsui SY, Wong YS, Pang KY, Mou JW et al (2012) Laparoscopic versus open Kasai portoenterostomy in infant with biliary atresia: a retrospective review on the 5-year native liver survival. Pediatr Surg Int 28:1109–1113
Chan KW, Lee KH, Wong HY, Tsui SY, Wong YS, Pang KY et al (2014) From laparoscopic to open Kasai portoenterostomy: the outcome after reintroduction of open Kasai portoenterostomy in infant with biliary atresia. Pediatr Surg Int 30:605–608
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interest.
Rights and permissions
About this article
Cite this article
Chan, K.W.E., Lee, K.H. & Wong, H.Y.V. Improved outcome in laparoscopic splenectomy in children with benign hematological disease after standardization of techniques. J Ped Endosc Surg 1, 65–69 (2019). https://doi.org/10.1007/s42804-019-00016-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42804-019-00016-x