Abstract
Purpose
The coping mechanisms employed to deal with objective financial burden following a cancer diagnosis are considered mediators of financial toxicity, specifically for the relationship between increased costs and health outcomes. Using qualitative research, the aim of the study was to explore the financial adjustments experienced by cancer patients and identify key coping mechanisms.
Methods
Semistructured interviews with 39 cancer patients (aged from 40 to 86 years) were conducted between May 2017 and April 2018 in Germany. Narratives were transcribed verbatim and analysed via qualitative content analysis.
Results
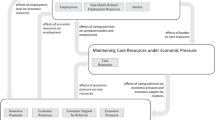
In all, 28 participants reported that they made financial adjustments related to two major categories: (1) reducing expenditures related to basic needs, luxury needs, and health-related decisions, and (2) increasing financial resources by saving less, using savings, investing manpower, obtaining help from third parties, incurring bank debt, and making health-related decisions. Typically, cancer patients both reduced expenditures and increased financial resources, but no typical patterns of combinations of coping mechanisms could be identified. However, reducing spending on basic and luxury needs was found to occur more typically than increasing the available money through incurring bank debt, making health-related decisions, or investing manpower.
Conclusions
This qualitative study provides a comprehensive understanding of the complexity of the coping mechanisms used by patients to address either higher costs or changed needs and priorities following a cancer diagnosis. With regard to understanding patients’ experiences of subjective financial stress, both increasing financial resources and reducing expenditures, particularly those relating to basic needs and luxury needs as distinct categories, might be relevant and should be considered. The financial situation impacts the treatment of cancer patients since health-related decisions were reported to be made with the aim of increasing financial resources by maintaining an ability to work or reducing expenditures through non-adherence.

Similar content being viewed by others
References
Carrera PM, Kantarjian HM, Blinder VS (2018) The financial burden and distress of patients with cancer. CA Cancer J Clin 68(2):153–165. https://doi.org/10.3322/caac.21443
Gordon LG, Merollini KMD, Lowe A, Chan RJ (2017) A systematic review of financial toxicity among cancer survivors. Patient 10(3):295–309. https://doi.org/10.1007/s40271-016-0204-x
Azzani M, Roslani AC, Su TT (2015) The perceived cancer-related financial hardship among patients and their families: a systematic review. Support Care Cancer 23(3):889–898. https://doi.org/10.1007/s00520-014-2474-y
Kale HP, Carroll NV (2016) Self-reported financial burden of cancer care and its effect on physical and mental health-related quality of life among US cancer survivors. Cancer 122(8):283–289. https://doi.org/10.1002/cncr.29808
Ramsey SD, Bansal A, Fedorenko CR, Blough DK, Overstreet KA, Shankaran V, Newcomb P (2016) Financial insolvency as a risk factor for early mortality among patients with cancer. J Clin Oncol 34(9):980–986. https://doi.org/10.1200/JCO.2015.64.6620
Banegas MP, Dickerson JF, Kent EE, de Moor JS, Virgo KS, Guy GP, Ekwueme DU, Zheng Z, Nutt S, Pace L, Varga A, Waiwaiole L, Schneider J, Robin Yabroff K (2018) Exploring barriers to the receipt of necessary medical care among cancer survivors under age 65 years. J Cancer Surviv 12(1):28–37. https://doi.org/10.1007/s11764-017-0640-1
Yabroff KR, Dowling EC, Guy GP Jr et al (2016) Financial hardship associated with cancer in the United States: findings from a population-based sample of adult cancer survivors. J Clin Oncol 34(3):259–267. https://doi.org/10.1200/JCO.2015.62.0468
Shankaran V, Jolly S, Blough D, Ramsey SD (2012) Risk factors for financial hardship in patients receiving adjuvant chemotherapy for colon cancer: a population-based exploratory analysis. J Clin Oncol 30(14):1608–1614. https://doi.org/10.1200/JCO.2011.37.9511
Whitney RL, Bell JF, Reed SC, Lash R, Bold RJ, Kim KK, Davis A, Copenhaver D, Joseph JG (2016) Predictors of financial difficulties and work modifications among cancer survivors in the United States. J Cancer Surviv 10(2):241–250. https://doi.org/10.1007/s11764-015-0470-y
Regenbogen SE, Veenstra CM, Hawley ST, Banerjee M, Ward KC, Kato I, Morris AM (2014) The personal financial burden of complications after colorectal cancer surgery. Cancer 120(19):3074–3081. https://doi.org/10.1002/cncr.28812
Zafar SY, Peppercorn JM, Schrag D, Taylor DH, Goetzinger AM, Zhong X, Abernethy AP (2013) The financial toxicity of cancer treatment: a pilot study assessing out-of-pocket expenses and the insured cancer patient’s experience. Oncologist 18(4):381–390. https://doi.org/10.1634/theoncologist.2012-0279
Nipp RD, Zullig LL, Samsa G, Peppercorn JM, Schrag D, Taylor DH Jr, Abernethy AP, Zafar SY (2016) Identifying cancer patients who alter care or lifestyle due to treatment-related financial distress. Psycho-oncology 25(6):719–725. https://doi.org/10.1002/pon.3911
Altice CK, Banegas MP, Tucker-Seeley RD, Yabroff KR (2017) Financial hardships experienced by cancer survivors. J Natl Cancer Inst 109(2):djw205. https://doi.org/10.1093/jnci/djw205
Timmons A, Gooberman-Hill R, Sharp L (2013) “It’s at a time in your life when you are most vulnerable”: a qualitative exploration of the financial impact of a cancer diagnosis and implications for financial protection in health. PLoS One 8(11):e77549. https://doi.org/10.1371/journal.pone.0077549
Amir Z, Wilson K, Hennings J, Young A (2012) The meaning of cancer: implications for family finances and consequent impact on lifestyle, activities, roles and relationships. Psychooncology 21(11):1167–1174. https://doi.org/10.1002/pon.2021
Bradley S, Sherwood PR, Donovan HS, Hamilton R, Rosenzweig M, Hricik A, Newberry A, Bender C (2007) I could lose everything: understanding the cost of a brain tumor. J Neuro-Oncol 85(3):329–338. https://doi.org/10.1007/s11060-007-9425-0
Head B, Harris L, Kayser K, Martin A, Smith L (2018) As if the disease was not enough. Support Care Cancer 26(3):975–987. https://doi.org/10.1007/s00520-017-3918-y
Büttner M, König H-H, Löbner M, Briest S, Konnopka A, Dietz A, Riedel-Heller S, Singer S (2018) Out-of-pocket-payments and the financial burden of 502 cancer patients of working age in Germany. Support Care Cancer 27:2221–2228. https://doi.org/10.1007/s00520-018-4498-1
Barbaret C, Brosse C, Rhondali W, Ruer M, Monsarrat L, Michaud P, Schott AM, Delgado-Guay M, Bruera E, Sanchez S, Filbet M (2017) Financial distress in patients with advanced cancer. PLoS One 12(5):e0176470. https://doi.org/10.1371/journal.pone.0176470
Schreier M (2012) Qualitative content analysis in practice, 1st edn. Sage, Los Angeles
Moffatt S, Noble E, Exley C (2010) “Done more for me in a fortnight than anybody done in all me life.” How welfare rights advice can help people with cancer. BMC Health Serv Res 10:259. https://doi.org/10.1186/1472-6963-10-259
Céilleachair AÓ, Costello L, Finn C et al (2012) Inter-relationships between the economic and emotional consequences of colorectal cancer for patients and their families: a qualitative study. BMC Gastroenterol 12:62. https://doi.org/10.1186/1471-230X-12-62
McGrath P (2015) Informal financial assistance for patients with a hematological malignancy: implications for oncology social work practice. Soc Work Health Care 54(10):892–908. https://doi.org/10.1080/00981389.2015.1061088
McNulty J, Khera N (2015) Financial hardship—an unwanted consequence of cancer treatment. Curr Hematol Malig Rep 10(3):205–212. https://doi.org/10.1007/s11899-015-0266-1
Timmons A, Gooberman-Hill R, Sharp L (2013) The multidimensional nature of the financial and economic burden of a cancer diagnosis on patients and their families: qualitative findings from a country with a mixed public-private healthcare system. Support Care Cancer 21(1):107–117. https://doi.org/10.1007/s00520-012-1498-4
Lazarus RS (1999) Stress and emotion. A new synthesis. Free Assoc. Books, London
Longo CJ, Fitch M, Grignon M, McAndrew A (2016) Understanding the full breadth of cancer-related patient costs in Ontario: a qualitative exploration. Support Care Cancer 24(11):4541–4548. https://doi.org/10.1007/s00520-016-3293-0
Goldstein DA (2017) Financial toxicity in cancer care-edging toward solutions. Cancer 123(8):1301–1302. https://doi.org/10.1002/cncr.30555
Acknowledgements
We thank the patients who participated in this study and shared their experiences regarding this personal topic with us. For their assistance with recruiting patients for this study, we acknowledge scientific assistants Julia Faltus and Johannes Niebuhr and our cooperation partners within the outpatient departments and doctors’ practices. We thank Jürgen Walther and Marie Rösler from the German Cancer Society and Sven Weise from the Cancer Society of Saxony-Anhalt for their topical discussions on and insights into the issue of financial toxicity from the viewpoint of social counselling.
Funding
We thank the German Cancer Aid for financing the study (grant number 70112452).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 80 kb)
Rights and permissions
About this article
Cite this article
Schröder, S.L., Schumann, N., Fink, A. et al. Coping mechanisms for financial toxicity: a qualitative study of cancer patients’ experiences in Germany. Support Care Cancer 28, 1131–1139 (2020). https://doi.org/10.1007/s00520-019-04915-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-019-04915-w