Abstract
Introduction
Split cord malformation (SCM) is a rare congenital spinal abnormality. Clinical presentation varies. Other congenital defects can be associated. Management is surgical.
Material and methods
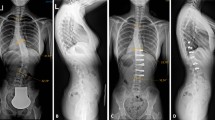
We retrospectively reviewed all our SCM cases and reported our experience for its management. From 1990 to 2014, 37 patients were operated. Five situations lead to the diagnosis (orthopedic disorders (n = 8), orthopedic and neurological disorders (n = 16), pure neurological disorders (n = 5), no symptoms except cutaneous signs (n = 7), antenatal diagnosis (n = 1)). Scoliosis was the most common associated condition. The level of the spur was always under T7 except in one case. There were more type I (n = 22) than type II (n = 15) SCM.
Results
Patients with preoperative neurological symptoms (n = 21) were improved in 71.4%. Five out of nine patients that had preoperative bladder dysfunction were improved. Eleven patients needed surgical correction of the scoliosis.
Conclusions
For us, the surgical procedure is mandatory even in case of asymptomatic discovery in order to avoid late clinical deterioration. In any case, the filum terminale need to be cut in order to untether completely the spinal cord. In case a surgical correction of a spinal deformity is needed, we recommend a two-stage surgery, for both SCM type. The SCM surgery can stop the evolution of the scoliosis and it may just need an orthopedic treatment with a brace.








Similar content being viewed by others
Change history
17 May 2018
The original version of this article unfortunately contained an error. The authors have been published with inverted given and family names. Given in this article are the corrected author names.
Abbreviations
- CSF:
-
Cerebro spinal fluid
- CT scan:
-
computed tomography scanner
- DM:
-
Diplomyelia
- DSM:
-
Diastematomyelia
- MM:
-
Myelomeningocele
- MRI:
-
Magnetic resonance imaging
- SCM:
-
Split cord malformation
- US:
-
Ultrasound scan
References
Ollivier C (1837) Triate des maladies de la moelle épinière. 3rd edn. pp 189
Pang D, Dias MS, Ahab-Barmada M (1992) Split cord malformation: part I: a unified theory of embryogenesis for double spinal cord malformations. Neurosurgery 31:451–480
Bremer JL (1952) Dorsal intestinal fistula; accessory neurenteric canal; diastematomyelia. AMA Arch Pathol 54:132–138
Bentley JF, Smith JR (1960) Developmental posterior enteric remnants and spinal malformations: the split notochord syndrome. Arch Dis Child 35:76–86
Gardner WJ (1964) Diastematomyelia and the Klippel-Feil syndrome. relationship to hydrocephalus, syringomyelia, meningocele, meningomyelocele, and iniencephalus. Cleve Clin Q 31:19–44
Humphreys RP, Hendrick EB, Hoffman HJ (1983) Diastematomyelia. Clin Neurosurg 30:436–456
Rilliet B, Schowing J, Berney J (1992) Pathogenesis of diastematomyelia: can a surgical model in the chick embryo give some clues about the human malformation? Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 8:310–316
Fardon DF (2001) From the clinic...diastematomyelia, when examination of the skin predicts spinal deformity. Spine J Off J North Am Spine Soc 1
Pang D (1992) Split cord malformation: part II: clinical syndrome. Neurosurgery 31:481–500
Schijman E (2003) Split spinal cord malformations: report of 22 cases and review of the literature. Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 19:96–103. https://doi.org/10.1007/s00381-002-0675-z
Mahapatra AK (2011) Split cord malformation—a study of 300 cases at AIIMS 1990-2006. J Pediatr Neurosci 6:S41–S45. https://doi.org/10.4103/1817-1745.85708
Akay KM, Izci Y, Baysefer A, Timurkaynak E (2004) Split cord malformation in adults. Neurosurg Rev 27:99–105. https://doi.org/10.1007/s10143-003-0313-6
Lichtenstein B (1940) “Spinal dysraphism”-spina bifida and myelodysplasia. Arch Neurol Psychiatr 44:792–810
Williams RA, Barth RA (1985) In utero sonographic recognition of diastematomyelia. AJR Am J Roentgenol 144:87–88
Sonigo-Cohen P, Schmit P, Zerah M, Chat L, Simon I, Aubry MC, Gonzales M, Pierre-Kahn A, Brunelle F (2003) Prenatal diagnosis of diastematomyelia. Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 19:555–560. https://doi.org/10.1007/s00381-003-0771-8
Erşahin Y (2013) Split cord malformation types I and II: a personal series of 131 patients. Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 29:1515–1526. https://doi.org/10.1007/s00381-013-2115-7
Barutcuoglu M, Selcuki M, Selcuki D, Umur S, Mete M, Gurgen SG, Umur (2015) Cutting filum terminale is very important in split cord malformation cases to achieve total release. Childs Nerv Syst ChNS Off J Int Soc Pediatr Neurosurg 31:425–432. https://doi.org/10.1007/s00381-014-2586-1
Cheng B, Li FT, Lin L (2012) Diastematomyelia: a retrospective review of 138 patients. J Bone Joint Surg Br 94:365–372. https://doi.org/10.1302/0301-620X.94B3.27897
Proctor MR, Scott RM (2001) Long-term outcome for patients with split cord malformation. Neurosurg Focus 10:e5
Jamil M, Bannister CM (1992) A report of children with spinal dysraphism managed conservatively. Eur J Pediatr Surg Off J Austrian Assoc Pediatr Surg Al Z Kinderchir 2(Suppl 1):26–28. https://doi.org/10.1055/s-2008-1063495
Lewandrowski KU, Rachlin JR, Glazer PA (2004) Diastematomyelia presenting as progressive weakness in an adult after spinal fusion for adolescent idiopathic scoliosis. Spine J Off J North Am Spine Soc 4:116–119
Gupta DK, Ahmed S, Garg K, Mahapatra AK (2010) Regrowth of septal spur in split cord malformation. Pediatr Neurosurg 46:242–244. https://doi.org/10.1159/000318753
Feng F, Shen J, Zhang J, Zhao H, Zhao Y, Li Z, Xue X, Lin Y, Qiu G (2016) Clinical outcomes of different surgical strategy for patients with congenital scoliosis and type I split cord malformation. Spine 41:1310–1316. https://doi.org/10.1097/BRS.0000000000001530
Hui H, Tao H-R, Jiang X-F, Fan HB, Yan M, Luo ZJ (2012) Safety and efficacy of 1-stage surgical treatment of congenital spinal deformity associated with split spinal cord malformation. Spine 37:2104–2113. https://doi.org/10.1097/BRS.0b013e3182608988
Winter RB, Haven JJ, Moe JH, Lagaard SM (1974) Diastematomyelia and congenital spine deformities. J Bone Joint Surg Am 56:27–39
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors
Electronic supplementary material
supplement digital content 1
surgical technique to remove the bony spur (0:02: dissection of the spur; 0:14 coagulation of the veins and arteries; 0:23: removal of the spur) (MOV 255506 kb)
supplement digital content 2
surgical technique to reconstructed a single dural sac (0:01: opening of the dura; 0:10 closure of the dura; 0:31: one single dural sac is obtained) (MOV 351658 kb)
Rights and permissions
About this article
Cite this article
Pierre-Aurelien, B., Federico, D.R., Alexandru, S. et al. Management of split cord malformation in children: the Lyon experience. Childs Nerv Syst 34, 883–891 (2018). https://doi.org/10.1007/s00381-018-3772-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-018-3772-3