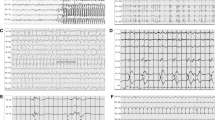
Abstract
Recording or monitoring the EEG or evoked potentials (EPs) in the ICU provides useful information in acutely neurologically ill patients whenever a relationship exists between the electrical activity and the (1) functional integrity of CNS structures; (2) clinical status; (3) diagnosis or (4) prognosis. In brain death such a correlation is clearly present. In certain countries, including ViennaItaly, an EEG is required by law before a diagnosis of brain death can be made and donor organs removed. In other countries, including the United Kingdom and the United States, the diagnosis of brain death can be made on clinical grounds alone, although an EEG is often obtained to confirm this diagnosis. A clinical diagnosis of brain death requires demonstrating the absence of brain and brainstem function when depressant drug intoxication and hypothermia can be excluded. Hypothermia poses no problem since the patient can be warmed and the examination repeated. Excluding the presence of depressant drugs is more difficult. Electrocerebral inactivity or electrocerebral silence which is consistent with a clinical diagnosis of brain death is defined as no EEG activity over 2μV when recording from scalp electrode pairs 10 or more cm apart with interelectrode impedances under 10,000 ohms but over 100 ohms. The value of 2μV was selected because many EEG machines have noise levels of up to 2 μV. The EEG is often recorded with difficulty in the electrically hostile environment of the ICU. It is imperative that technicians are well trained, taught to apply electrodes with care, and identify, and, when possible, eliminate artifact.
Chapter PDF
Similar content being viewed by others
References
Cracco RQ, Bodis-Wollner I (1986) Evoked potentials. Alan R Liss Inc, New York
Chiappa K (1983) Evoked potentials in clinical medicine. Raven Press, New York
Bodis-Wollner I (1982) Evoked potentials. Ann New York Acad Sci, pp 388
Hassan NF, Rossini PM, Cracco RQ, Cracco JB (1985) Unexposed motor cortex activation by low voltage stimuli. In: Morocutti C, Rizzo PA (eds) Evoked potentials: Neurophysiological and clinical aspects. Elsevier, Amsterdam, pp 107–113
Klass DW, Daly D (1979) Current practice of clinical electroencephalography. Raven Press, New York
Neurosurgery (Supplement on Motor Evoked Potentials). Jan 1987, Vol 20: 1
Journal of Clinical Neurophysiol (Supplement on Guidelines). Jan 1987
Lueders H et al (1986) Subdural electrodes. In: Engel J (ed) Surgical management of the epilepsies. Raven Press, New York
Young RR, Cracco RQ (1985) Clinical neurophysiology of conduction in central motor pathways. Ann Neurol 18: 606–610
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 1988 Springer-Verlag Wien
About this chapter
Cite this chapter
Cracco, R.Q. (1988). EEG and Evoked Potentials: Rationale for ICU Recording and Monitoring. In: Grundy, B.L., Villani, R.M. (eds) Evoked Potentials. Springer, Vienna. https://doi.org/10.1007/978-3-7091-4431-2_1
Download citation
DOI: https://doi.org/10.1007/978-3-7091-4431-2_1
Publisher Name: Springer, Vienna
Print ISBN: 978-3-211-82059-9
Online ISBN: 978-3-7091-4431-2
eBook Packages: Springer Book Archive