Abstract
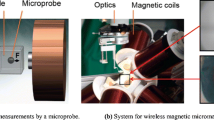
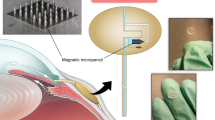
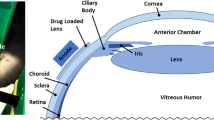
The progress of wet age-related macular degeneration can now be controlled by intravitreal drug injection. This approach requires repeated injections, which could be avoided by delivering the drug to the retina. Intraocular implants are a promising solution for drug delivery near the retina. Currently, their accurate placement is challenging, and they can only be removed after a vitrectomy. In this paper, we introduce an approach for minimally invasive retinal drug delivery using magnetic intraocular inserts. We briefly discuss the electromagnetic-control system for magnetic implants and then focus on evaluating their ability to move in the vitreous humor. The mobility of magnetic intraocular implants is estimated in vitro with synthesized vitreous humors, and ex vivo with experiments on cadaver porcine eyes. Preliminary results show that with such magnetic implants a vitrectomy can be avoided.
This work was supported by the NCCR Co-Me of the Swiss National Science Foundation.
Chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
References
Congdon, N., O’Colmain, B., Klaver, C.C., Klein, R., Munoz, B., Friedman, D.S., Kempen, J., Taylor, H.R., Mitchell, P.: Causes and prevalence of visual impairment among adults in the United States. Arch. Ophthalmology 122(4), 477–485 (2004)
Nowak, J.Z.: Age-related macular degeneration: pathogenesis and therapy. Pharmacological Reports 58(3), 353–363 (2006)
Lee, S.S., Robinson, M.R.: Novel drug delivery systems for retinal diseases. Ophthalmic Research 41(3), 124–135 (2009)
Danckwerts, M.P., Fassihi, A.: Implantable controlled release drug delivery systems. Drug Development and Industrial Pharmacy 17(11), 1465–1502 (1991)
Yasukawa, T., Ogura, Y., Tabata, Y., Kimura, H., Wiedemann, P., Honda, Y.: Drug delivery systems for vitreoretinal diseases. Progress in Retinal and Eye Research 23(3), 253–281 (2004)
Nelson, B.J., Kaliakatsos, I.K., Abbott, J.J.: Microrobots for minimally invasive medicine. Annual Review of Biomedical Engineering 12, 55–85 (2010)
Yeşin, K.B., Vollmers, K., Nelson, B.J.: Modeling and control of untethered biomicrorobots in a fluidic environment using electromagnetic fields. Int. J. Robotics Research 25(5-6), 527–536 (2006)
Ishiyama, K., Sendoh, M., Yamazaki, A., Arai, K.I.: Swimming micro-machine driven by magnetic torque. Sensor and Actuators A: Physical 91(1–2), 141–144 (2001)
Sivaraman, K.M., Bayrakceken, K., Ergeneman, O., Pane, S., Lühmann, T., Hall, H., Nelson, B.J.: Tailoring the drug loading capacity of polypyrrole films for use in intraocular biomicrorobots. In: IEEE Int. Conf. Engineering in Medicine and Biology, pp. 4359–4362 (2010)
Choonara, Y.E., Pillay, V., Danckwerts, M.P., Carmichael, T.R., Du Toit, L.C.: A review of implantable intravitreal drug delivery technologies for the treatment of posterior segment eye diseases. J. Pharmaceutical Sciences 99(5), 2219–2239 (2010)
Kummer, M.P., Abbott, J.J., Kratochvil, B.E., Borer, R., Sengul, A., Nelson, B.J.: OctoMag: An electromagnetic system for 5-DOF wireless micromanipulation. IEEE Trans. Robotics 26(6), 1006–1017 (2010)
Gupta, P.K., Jensen, P.S., de Juan Jr., E.: Surgical forces and tactile perception during retinal microsurgery. In: Taylor, C., Colchester, A. (eds.) MICCAI 1999. LNCS, vol. 1679, pp. 1218–1225. Springer, Heidelberg (1999)
Kummer, M.P., Abbott, J.J., Dinser, S., Nelson, B.J.: Artificial vitreous humor for in vitro experiments. In: IEEE Int. Conf. Engineering in Medicine and Biology, pp. 6406–6409 (2007)
Nickerson, C.S.: Engineering the mechanical properties of ocular tissues. PhD thesis, California Institute of Technology (2005)
Los, L.I., Van der Worp, R.J., Van Luyn, M.J.A., Hooymans, J.M.M.: Age-related liquefaction of the human vitreous body: LM and TEM evaluation of the role of proteoglycans and collagen. Investigative Ophthalmology and Visual Science 44(7), 2828–2833 (2003)
Lee, B., Litt, M., Buchsbaum, G.: Rheology of the vitreous body: Part 2. viscoelasticity of bovine and porcine vitreous. Biorheology 31(4), 327–338 (1994)
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2011 Springer-Verlag Berlin Heidelberg
About this paper
Cite this paper
Bergeles, C., Kummer, M.P., Kratochvil, B.E., Framme, C., Nelson, B.J. (2011). Steerable Intravitreal Inserts for Drug Delivery: In Vitro and Ex Vivo Mobility Experiments. In: Fichtinger, G., Martel, A., Peters, T. (eds) Medical Image Computing and Computer-Assisted Intervention – MICCAI 2011. MICCAI 2011. Lecture Notes in Computer Science, vol 6891. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-642-23623-5_5
Download citation
DOI: https://doi.org/10.1007/978-3-642-23623-5_5
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-642-23622-8
Online ISBN: 978-3-642-23623-5
eBook Packages: Computer ScienceComputer Science (R0)