Abstract
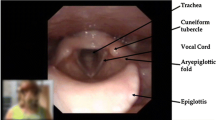
Exercise-induced laryngeal obstruction (EILO) is an umbrella term describing a dynamic closure of laryngeal structures during exercise, causing breathing problems. Recent population studies have shown that EILO is a relatively prevalent entity, most often affecting adolescents or young adults. EILO typically causes inspiratory symptoms and may have considerable functional impact on physical activity. Visualization of the laryngeal lumen during exercise is important for classification (i.e., glottic or supraglottic) and subsequent treatment planning. The continuous laryngoscopy exercise (CLE) test is therefore a useful tool in the evaluation of EILO patients. Information about the diagnosis and demonstration of the CLE test video often has a reassuring effect, and the differential diagnosis toward asthma is important. Small studies and case reports indicate effect from speech therapy, biofeedback, and inspiratory muscle training. Robust treatment algorithms and follow-up based on proper patient selection should be established. Supraglottic EILO is characterized as folding of the aryepiglottic folds comparable to that observed in infants with congenital laryngomalacia (CLM). This observation has encouraged surgeons to treat supraglottic EILO with supraglottoplasty. Although this procedure is proven efficient and safe, it is irreversible with potential risks for complication and should be restricted to selected cases.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Notes
- 1.
If the inducer is exercise, the suggested term is exercise-induced laryngeal obstruction (EILO).
- 2.
The circumstances for the diagnostic laryngoscopy should be described and findings reported in detail for sub-categorization, e.g., laryngeal level of obstruction (supraglottic, glottic, or a combination of both).
References
Olin JT, et al. Inducible laryngeal obstruction during exercise: moving beyond vocal cords with new insights. Phys Sportsmed. 2015;43(1):13–21.
Dunglison R. The practice of medicine a treatise on special pathology and therapeutics, vol. 2. Philadelphia: Lea & Blanchard; 1844.
Patterson R, Schatz M, Horton M. Munchausen’s stridor: non-organic laryngeal obstruction. Clin Allergy. 1974;4(3):307–10.
Christopher KL, et al. Vocal-cord dysfunction presenting as asthma. N Engl J Med. 1983;308(26):1566–70.
Kellman RM, Leopold DA. Paradoxical vocal cord motion: an important cause of stridor. Laryngoscope. 1982;92(1):58–60.
Christensen PM, et al. ERS/ELS/ACCP 2013 international consensus conference nomenclature on inducible laryngeal obstructions. Eur Respir Rev. 2015;24(137):445–50.
England SJ, Bartlett D Jr. Changes in respiratory movements of the human vocal cords during hyperpnea. J Appl Physiol Respir Environ Exerc Physiol. 1982;52(3):780–5.
Belmont JR, Grundfast K. Congenital laryngeal stridor (laryngomalacia): etiologic factors and associated disorders. Ann Otol Rhinol Laryngol. 1984;93(5 Pt 1):430–7.
Liyanagedera S, McLeod R, Elhassan HA. Exercise induced laryngeal obstruction: a review of diagnosis and management. Eur Arch Otorhinolaryngol. 2017;274(4):1781–9.
Røksund OD, et al. Larynx during exercise: the unexplored bottleneck of the airways. Eur Arch Otorhinolaryngol. 2015;272(9):2101–9.
Morris MJ, Christopher KL. Diagnostic criteria for the classification of vocal cord dysfunction. Chest. 2010;138(5):1213–23.
Shembel AC, et al. Perceptual clinical features in exercise-induced laryngeal obstruction (EILO): toward improved diagnostic approaches. J Voice. 2019;33(6):880–93.
Anderson SD, et al. Exercise-induced asthma. Br J Dis Chest. 1975;69(1):1–39.
Griffin SA, Walsted ES, Hull JH. Infographic. The breathless athlete: EILO. Br J Sports Med. 2019;53(10):616–7.
Johansson H, et al. Prevalence of exercise-induced bronchoconstriction and exercise-induced laryngeal obstruction in a general adolescent population. Thorax. 2015;70(1):57–63.
McFadden ER Jr, Zawadski DK. Vocal cord dysfunction masquerading as exercise-induced asthma. A physiologic cause for “choking” during athletic activities. Am J Respir Crit Care Med. 1996;153(3):942–7.
Hull JH, et al. Feasibility of portable continuous laryngoscopy during exercise testing. ERJ Open Res. 2019;5(1):00219–2018.
Heimdal JH, et al. Continuous laryngoscopy exercise test: a method for visualizing laryngeal dysfunction during exercise. Laryngoscope. 2006;116(1):52–7.
Bent JP III, et al. Pediatric exercise-induced laryngomalacia. Ann Otol Rhinol Laryngol. 1996;105(3):169–75.
Weinberger M, Abu-Hasan M. Pseudo-asthma: when cough, wheezing, and dyspnea are not asthma. Pediatrics. 2007;120(4):855–64.
McArdle WD, Katch FI, Katch VL. Exercise physiology. Philadelphia: Lippincott Williams & Wilkins; 1995. p. 217–32.
Panchasara B, et al. Lesson of the month: rowing-induced laryngeal obstruction: a novel cause of exertional dyspnoea: characterised by direct laryngoscopy. Thorax. 2015;70(1):95–7.
Walsted ES, et al. Laryngoscopy during swimming: a novel diagnostic technique to characterize swimming-induced laryngeal obstruction. Laryngoscope. 2017;127(10):2298–301.
Maat RC, et al. Audiovisual assessment of exercise-induced laryngeal obstruction: reliability and validity of observations. Eur Arch Otorhinolaryngol. 2009;266(12):1929–36.
Christensen P, et al. Exercise-induced laryngeal obstructions objectively assessed using EILOMEA. Eur Arch Otorhinolaryngol. 2010;267(3):401–7.
Norlander K, et al. Differences in laryngeal movements during exercise in healthy and dyspnoeic adolescents. Int J Pediatr Otorhinolaryngol. 2020;129:109765.
Fretheim-Kelly Z, et al. Feasibility and tolerability of measuring translaryngeal pressure during exercise. Laryngoscope. 2019;129(12):2748–53.
Christensen PM, et al. Exercise-induced laryngeal obstructions: prevalence and symptoms in the general public. Eur Arch Otorhinolaryngol. 2011;268(9):1313–9.
Halvorsen T, et al. Inducible laryngeal obstruction: an official joint European Respiratory Society and European Laryngological Society statement. Eur Respir J. 2017;50(3):1602221.
Nonomura N, et al. Acquired airway obstruction caused by hypertrophic mucosa of the arytenoids and aryepiglottic folds. Am J Otolaryngol. 1996;17(1):71–4.
Logemann JA, et al. Closure mechanisms of laryngeal vestibule during swallow. Am J Physiol. 1992;262(2 Pt 1):G338–44.
Reidenbach MM. Aryepiglottic fold: normal topography and clinical implications. Clin Anat. 1998;11(4):223–35.
Smith RJ, et al. Exercise-induced laryngomalacia. Ann Otol Rhinol Laryngol. 1995;104(7):537–41.
Hilland M, et al. Congenital laryngomalacia is related to exercise-induced laryngeal obstruction in adolescence. Arch Dis Child. 2016;101(5):443–8.
Arora R, Gal TJ, Hagan LL. An unusual case of laryngomalacia presenting as asthma refractory to therapy. Ann Allergy Asthma Immunol. 2005;95(6):607–11.
Peron DL, Graffino DB, Zenker DO. The redundant aryepiglottic fold: report of a new cause of stridor. Laryngoscope. 1988;98(6 Pt 1):659–63.
Ayres JG, Gabbott PL. Vocal cord dysfunction and laryngeal hyperresponsiveness: a function of altered autonomic balance? Thorax. 2002;57(4):284–5.
Shiba K, Isono S, Nakazawa K. Paradoxical vocal cord motion: a review focused on multiple system atrophy. Auris Nasus Larynx. 2007;34(4):443–52.
Petcu LG, Sasaki CT. Laryngeal anatomy and physiology. Clin Chest Med. 1991;12(3):415–23.
Perkner JJ, et al. Irritant-associated vocal cord dysfunction. J Occup Environ Med. 1998;40(2):136–43.
Thompson DM. Abnormal sensorimotor integrative function of the larynx in congenital laryngomalacia: a new theory of etiology. Laryngoscope. 2007;117(6 Pt 2 Suppl 114):1–33.
Sinclair CF, Téllez MJ, Ulkatan S. Human laryngeal sensory receptor mapping illuminates the mechanisms of laryngeal adductor reflex control. Laryngoscope. 2018;128(11):E365–e370.
Strohl KP, Butler JP, Malhotra A. Mechanical properties of the upper airway. Compr Physiol. 2012;2(3):1853–72.
Gimenez LM, Zafra H. Vocal cord dysfunction: an update. Ann Allergy Asthma Immunol. 2011;106(4):267–74; quiz 275.
Taramarcaz P, et al. Transient postviral vocal cord dysfunction. J Allergy Clin Immunol. 2004;114(6):1471–2.
Kenn K, Balkissoon R. Vocal cord dysfunction: what do we know? Eur Respir J. 2011;37(1):194–200.
Ibrahim WH, et al. Paradoxical vocal cord motion disorder: past, present and future. Postgrad Med J. 2007;83(977):164–72.
Andreatta RD, et al. Mucosal afferents mediate laryngeal adductor responses in the cat. J Appl Physiol (1985). 2002;93(5):1622–9.
Rundell KW, Spiering BA. Inspiratory stridor in elite athletes. Chest. 2003;123(2):468–74.
Koufman JA, Block C. Differential diagnosis of paradoxical vocal fold movement. Am J Speech Lang Pathol. 2008;17(4):327–34.
Maschka DA, et al. A classification scheme for paradoxical vocal cord motion. Laryngoscope. 1997;107(11 Pt 1):1429–35.
McFadden ER Jr. Glottic function and dysfunction. J Allergy Clin Immunol. 1987;79(5):707–10.
Fink BR. Folding mechanism of the human larynx. Acta Otolaryngol. 1974;78(1–2):124–8.
Beaty MM, Wilson JS, Smith RJ. Laryngeal motion during exercise. Laryngoscope. 1999;109(1):136–9.
Røksund OD, et al. Exercise induced dyspnea in the young. Larynx as the bottleneck of the airways. Respir Med. 2009;103(12):1911–8.
Haines J, Hull JH, Fowler SJ. Clinical presentation, assessment, and management of inducible laryngeal obstruction. Curr Opin Otolaryngol Head Neck Surg. 2018;26(3):174–9.
Hull JH. Multidisciplinary team working for vocal cord dysfunction: now it’s GO time. Respirology. 2019;24(8):714–5.
Maat RC, et al. Exercise-induced laryngeal obstruction: natural history and effect of surgical treatment. Eur Arch Otorhinolaryngol. 2011;268(10):1485–92.
Olin JT, et al. Therapeutic laryngoscopy during exercise: a novel non-surgical therapy for refractory EILO. Pediatr Pulmonol. 2017;52(6):813–9.
Boris M, Goldblatt A, Krigsman A. Laryngeal dysfunction: a common cause of respiratory distress, often misdiagnosed as asthma and responsive to antireflux therapy. Allergy Asthma Proc. 2002;23(2):133–9.
Woolnough K, et al. Acid suppression does not reduce symptoms from vocal cord dysfunction, where gastro-laryngeal reflux is a known trigger. Respirology. 2013;18(3):553–4.
Guglani L, et al. A systematic review of psychological interventions for adult and pediatric patients with vocal cord dysfunction. Front Pediatr. 2014;2:82.
Shaffer M, et al. Speech-language pathology as a primary treatment for exercise-induced laryngeal obstruction. Immunol Allergy Clin N Am. 2018;38(2):293–302.
Sandnes A, et al. Exercise-induced laryngeal obstruction in athletes treated with inspiratory muscle training. BMJ Open Sport Exerc Med. 2019;5(1):e000436.
Maat RC, et al. Surgical treatment of exercise-induced laryngeal dysfunction. Eur Arch Otorhinolaryngol. 2007;264(4):401–7.
Norlander K, et al. Surgical treatment is effective in severe cases of exercise-induced laryngeal obstruction: a follow-up study. Acta Otolaryngol. 2015;135(11):1152–9.
Mehlum CS, et al. Supraglottoplasty as treatment of exercise induced laryngeal obstruction (EILO). Eur Arch Otorhinolaryngol. 2016;273(4):945–51.
Famokunwa B, Sandhu G, Hull JH. Surgical intervention for exercise-induced laryngeal obstruction: a UK perspective. Laryngoscope. 2020;130:E667–73.
Sidell DR, et al. Pediatric exercise stress laryngoscopy following laryngotracheoplasty: a comparative review. Otolaryngol Head Neck Surg. 2014;150(6):1056–61.
Heimdal JH, Maat R, Nordang L. Surgical intervention for exercise-induced laryngeal obstruction. Immunol Allergy Clin N Am. 2018;38(2):317–24.
Siewers K, Backer V, Walsted ES. A systematic review of surgical treatment for supraglottic exercise-induced laryngeal obstruction. Laryngoscope Investig Otolaryngol. 2019;4(2):227–33.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Heimdal, JH., Maat, R., Hilland, M., Nordang, L. (2022). Exercise-Induced Laryngeal Obstruction. In: Remacle, M., Eckel, H.E. (eds) Textbook of Surgery of Larynx and Trachea. Springer, Cham. https://doi.org/10.1007/978-3-031-09621-1_11
Download citation
DOI: https://doi.org/10.1007/978-3-031-09621-1_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-09620-4
Online ISBN: 978-3-031-09621-1
eBook Packages: MedicineMedicine (R0)