Abstract
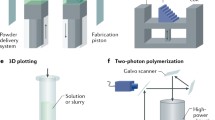
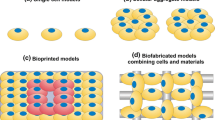
Biofabrication has been extensively explored in tissue engineering over the past two decades. It uses bioactive materials and live cells as the building blocks to create spatially defined geometries. The goal of biofabrication is to create engineered tissue constructs to replace damaged or diseased human tissues with full functionality. The advantage is that it can rapidly fabricate tissue constructs to meet customized needs. The biomaterials used for biofabrication are called bioinks and usually comprise hydrogel precursor solutions or biocompatible thermal plastics. In this review, we review the commonly used biofabrication methods and critical aspects for creating scaffolds for tissue regeneration. We discuss the criteria for developing and selecting suitable biomaterials as the bioinks. Commonly used biomaterials and their applications are summarized to present the versatility of biofabrication. We also aim to highlight the challenges of this technology and initiate new ideas and opportunities in the future developments in the bioprinting approach and bioinks. The refinement in fabrication techniques, exploration in biology, and development in new bioinks are essential elements toward the advancement of biofabrication.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Slaughter BV, Khurshid SS, Fisher OZ, Khademhosseini A, Peppas NA (2009) Hydrogels in regenerative medicine. Adv Mater 21:3307–3329
Subia B, Kundu J, Kundu SC (2010) Biomaterial scaffold fabrication techniques for potential tissue engineering applications. Tissue Eng 3:141–159
Murphy SV, Atala A (2014) 3D bioprinting of tissues and organs. Nat Biotechnol 32(8):773–785
Zhu W, Ma X, Gou M, Mei D, Zhang K, Chen S (2016) 3D printing of functional biomaterials for tissue engineering. Curr Opin Biotechnol 40:103–112
Truby RL, Lewis JA (2016) Printing soft matter in three dimensions. Nature 540(7633):371–378
Malda J et al (2013) 25th anniversary article: engineering hydrogels for biofabrication. Adv Mater 25(36):5011–5028
Cui H, Nowicki M, Fisher JP, Zhang LG (2017) 3D bioprinting for organ regeneration. Adv Healthc Mater 6(1)
Liu X et al (2018) 3D printing of living responsive materials and devices. Adv Mater 30(4)
Yue K, Trujillo-de Santiago G, Alvarez MM, Tamayol A, Annabi N, Khademhosseini A (2015) Synthesis, properties, and biomedical applications of gelatin methacryloyl (GelMA) hydrogels. Biomaterials 73:254–271
Jiang T, Munguia-lopez JG, Flores-torres S, Grant J, De Leon-rodriguez A, Kinsella JM (2017) Directing the self-assembly of tumour spheroids by bioprinting cellular heterogeneous models within alginate / gelatin hydrogels. Sci Rep 7(1):4575
Pedde RD et al (2017) Emerging biofabrication strategies for engineering complex tissue constructs. Adv Mater 29(19):1–27
Kang H, Lee SJ, Ko IK, Kengla C, Yoo JJ, Atala A (2016) A 3D bioprinting system to produce human-scale tissue constructs with structural integrity. Nat Biotechnol 34(3):312–319
Xu T, Zhao W, Zhu JM, Albanna MZ, Yoo JJ, Atala A (2013) Complex heterogeneous tissue constructs containing multiple cell types prepared by inkjet printing technology. Biomaterials 34:130–139
Koch L, Gruene M, Unger C, Chichkov B (2013) Laser assisted cell printing. Curr Pharm Biotechnol 14:91–97
Visser J et al (2013) Biofabrication of multi-material anatomically shaped tissue constructs. Biofabrication 5(3):035007
de Ruijter M et al Out-of-plane 3D-printed microfibers improve the shear properties of hydrogel composites. Small 1702773:2017
O’Bryan CS et al (2017) Self-assembled micro-organogels for 3D printing silicone structures. Sci Adv 5:3
Guillotin B et al (2010) Laser assisted bioprinting of engineered tissue with high cell density and microscale organization. Biomaterials 31(28):7250–7256
Xu T et al (2006) Viability and electrophysiology of neural cell structures generated by the inkjet printing method. Biomaterials 27(18):3580–3588
Bracaglia LG, Smith BT, Watson E, Arumugasaamy N, Mikos AG, Fisher JP (2017) 3D printing for the design and fabrication of polymer-based gradient scaffolds. Acta Biomater 56:3–13
Kim JD, Choi JS, Kim BS, Choi YC, Cho YW (2010) Piezoelectric inkjet printing of polymers: stem cell patterning on polymer substrates. Polymer 51(10):2147–2154
Guillotin B, Guillemot F (2011) Cell patterning technologies for organotypic tissue fabrication. Trends Biotechnol 29(4):183–190
Abbadessa A et al (2016) A synthetic thermosensitive hydrogel for cartilage bioprinting and its biofunctionalization with polysaccharides. Biomacromolecules 17:2137–2147
Rutz AL, Hyland KE, Jakus AE, Burghardt WR, Shah RN (2015) A multimaterial bioink method for 3D printing tunable, cell-compatible hydrogels. Adv Mater 27(9):1607–1614
Klotz BJ, Gawlitta D, Rosenberg AJWP, Malda J, Melchels FPW (2016) Gelatin-methacryloyl hydrogels: towards biofabrication-based tissue repair. Trends Biotechnol 34(5):394–407
Hornick J (2017) 3D printing in healthcare. J 3D Print Med 1(1):13–17
Hinton TJ et al (2015) Three-dimensional printing of complex biological structures by freeform reversible embedding of suspended hydrogels. Sci Adv 1(9):e1500758
Ouyang L, Highley CB, Sun W, Burdick JA (2017) A generalizable strategy for the 3D bioprinting of hydrogels from nonviscous photo-crosslinkable inks. Adv Mater 29(8)
Bose S, Vahabzadeh S, Bandyopadhyay A (2013) Bone tissue engineering using 3D printing. Mater Today 16(12):496–504
Mouser VHM, Melchels FPW, Visser J, Dhert WJA, Gawlitta D, Malda J (2016) Yield stress determines bioprintability of hydrogels based on gelatin-methacryloyl and gellan gum for cartilage bioprinting. Biofabrication 8(3):035003
Colosi C et al (2016) Microfluidic bioprinting of heterogeneous 3d tissue constructs using low-viscosity bioink. Adv Mater 28:677–684
Liu W et al (2017) Rapid continuous multimaterial extrusion bioprinting. Adv Mater 29(3)
Ribeiro A et al (2018) Assessing bioink shape fidelity to aid material development in 3D bioprinting. Biofabrication 10(1):014102
Blaeser A, Duarte Campos DF, Puster U, Richtering W, Stevens MM, Fischer H (2016) Controlling shear stress in 3D bioprinting is a key factor to balance printing resolution and stem cell integrity. Adv Healthc Mater 5(3):326–333
Suntornnond R, Tan EYS, An J, Chua CK (2016) A mathematical model on the resolution of extrusion bioprinting for the development of new bioinks. Materials 9(9)
Jin Y, Chai W, Huang Y (2017) Printability study of hydrogel solution extrusion in nanoclay yield-stress bath during printing-then-gelation biofabrication. Mater Sci Eng C 80:313–325
Yuk H, Zhao X (2018) A new 3D printing strategy by harnessing deformation, instability, and fracture of viscoelastic inks. Adv Mater 30(6)
Huang Z, Zhang Y, Kotaki M, Ramakrishna S (2003) A review on polymer nanofibers by electrospinning and their applications in nanocomposites. Compos Sci Technol 63:2223–2253
Liu S, Reneker DH (2019) Droplet-jet shape parameters predict electrospun polymer nanofiber diameter. Polymer 168:155–158
Visser J et al (2015) Reinforcement of hydrogels using three-dimensionally printed microfibres. Nat Commun 6:1–10
Jiang T, Munguia-lopez JG, Flores-torres S, Kort-mascort J, Kinsella JM Extrusion bioprinting of soft materials: an emerging technique for biological model fabrication. Appl Phys Rev 6(1):011310, 2019
Loh QL, Choong C (2013) Three-dimensional scaffolds for tissue engineering applications: Role of porosity and pore size. Tissue Eng Part B Rev 19(6):485–502
Hubbell JA, West JL (1999) Polymeric biomaterials with degradation sites for proteases involved in cell migration. Macromolecules 32(1):241–244
Caliari SR, Burdick JA (2016) A practical guide to hydrogels for cell culture. Nat Methods 13(5):405–414
Monette A, Ceccaldi C, Assaad E, Lerouge S, Lapointe R (2016) Chitosan thermogels for local expansion and delivery of tumor-specific T lymphocytes towards enhanced cancer immunotherapies. Biomaterials 75:237–249
Kolesky DB, Truby RL, Gladman AS, Busbee TA, Homan KA, Lewis JA (2014) 3D bioprinting of vascularized, heterogeneous cell-laden tissue constructs. Adv Mater 26(19):3124–3130
Hospodiuk M, Dey M, Sosnoski D, Ozbolat IT (2017) The bioink: a comprehensive review on bioprintable materials. Biotechnol Adv 35:217–239
Burdick JA, Murphy WL (2012) Moving from static to dynamic complexity in hydrogel design. Nat Commun 3:1–8
Ozbolat IT, Hospodiuk M (2016) Current advances and future perspectives in extrusion-based bioprinting. Biomaterials 76:321–343
Berger J, Reist M, Mayer JM, Felt O, Peppas NA, Gurny R (2004) Structure and interactions in covalently and ionically crosslinked chitosan hydrogels for biomedical applications. Eur J Pharm Biopharm 57:19–34
Wang J, Lin L, Cheng Q, Jiang L (2012) A strong bio-inspired layered PNIPAM-clay nanocomposite hydrogel. Angew Chem Int Ed 51(19):4676–4680
Jin R et al (2010) Synthesis and characterization of hyaluronic acid–poly(ethylene glycol) hydrogels via Michael addition: an injectable biomaterial for cartilage repair. Acta Biomater 6(6):1968–1977
Chen D, et al. Drilling by light: ice-templated photo-patterning enabled by a dynamically crosslinked hydrogel. Materials Horizons; 2019.
Hou J, Li C, Guan Y, Zhang Y, Zhu XX (2015) Enzymatically crosslinked alginate hydrogels with improved adhesion properties. Polym Chem 6(12):2204–2213
Kular JK, Basu S, Sharma RI (2014) The extracellular matrix: structure, composition, age-related differences, tools for analysis and applications for tissue engineering. J Tissue Eng 5:1–17
Wen JH et al (2014) Interplay of matrix stiffness and protein tethering in stem cell differentiation. Nat Mater 13(10):979–987
Khetan S, Burdick JA (2010) Biomaterials patterning network structure to spatially control cellular remodeling and stem cell fate within 3-dimensional hydrogels. Biomaterials 31(32):8228–8234
Chaudhuri O et al (2016) Hydrogels with tunable stress relaxation regulate stem cell fate and activity. Nat Mater 15(3):326–334
Zhao X, Huebsch N, Mooney DJ, Suo Z (2010) Stress-relaxation behavior in gels with ionic and covalent crosslinks. J Appl Phys 107(6)
Lou J, Stowers R, Nam S, Xia Y, Chaudhuri O (2018) Stress relaxing hyaluronic acid-collagen hydrogels promote cell spreading, fiber remodeling, and focal adhesion formation in 3D cell culture. Biomaterials 154:213–222
Chiu YC et al (2011) The role of pore size on vascularization and tissue remodeling in PEG hydrogels. Biomaterials 32(26):6045–6051
Oh SH, Park IK, Kim JM, Lee JH (2007) In vitro and in vivo characteristics of PCL scaffolds with pore size gradient fabricated by a centrifugation method. Biomaterials 28(9):1664–1671
Yannas IV, Lee E, Orgill DP, Skrabut EM, Murphy GF (1989) Synthesis and characterization of a model extracellular matrix that induces partial regeneration of adult mammalian skin. Proc Natl Acad Sci 86(3):933–937
Ying G-L et al (2018) Aqueous two-phase emulsion bioink-enabled 3D bioprinting of porous hydrogels. Adv Mater 30(50):e1805460
Li J, Mooney DJ (2016) Designing hydrogels for controlled drug delivery. Nat Rev Mater 1(12):16071
Deshayes S, Kasko AM (2013) Polymeric biomaterials with engineered degradation. J Polym Sci Pt A Polym Chem 51(17):3531–3566
Vold IMN, Christensen BE (2005) Periodate oxidation of chitosans with different chemical compositions. Carbohydr Res 340(4):679–684
Boontheekul T, Kong HJ, Mooney DJ (2005) Controlling alginate gel degradation utilizing partial oxidation and bimodal molecular weight distribution. Biomaterials 26(15):2455–2465
Göpferich A (1996) Mechanisms of polymer degradation and erosion. Biomaterials 17(2):103–114
Kost J, Leong K, Langer R (1989) Ultrasound-enhanced polymer degradation and release of incorporated substances. Proc Natl Acad Sci 86:7663–7666
O’Bryan CS et al (2017) Three-dimensional printing with sacrificial materials for soft matter manufacturing. MRS Bull 42(8):571–577
Hinton TJ, Hudson A, Pusch K, Lee A, Feinberg AW (2016) 3D printing PDMS elastomer in a hydrophilic support bath via freeform reversible embedding. ACS Biomater Sci Eng 2(10):1781–1786
Grosskopf AK, Truby RL, Kim H, Perazzo A, Lewis JA, Stone HA (2018) Viscoplastic matrix materials for embedded 3D printing. ACS Appl Mater Interfaces 10(27):23353–23361
Hoesli CA et al (2012) Reversal of diabetes by βtC3 cells encapsulated in alginate beads generated by emulsion and internal gelation. J Biomed Mater Res - Part B Appl Biomater 100 B(4):1017–1028
Jia J et al (2014) Engineering alginate as bioink for bioprinting. Acta Biomater 10(10):4323–4331
Beyer ST, Bsoul A, Ahmadi A, Walus K (2013) 3D alginate constructs for tissue engineering printed using a coaxial flow focusing microfluidic device. In: 2013 transducers eurosensors XXVII 17th Int. Conf. solid-state sensors, actuators microsystems, pp 1206–1209
Wüst S, Godla ME, Müller R, Hofmann S (2014) Tunable hydrogel composite with two-step processing in combination with innovative hardware upgrade for cell-based three-dimensional bioprinting. Acta Biomater 10(2)
Jeon O, Alt DS, Ahmed SM, Alsberg E (2012) The effect of oxidation on the degradation of photocrosslinkable alginate hydrogels. Biomaterials 33(13):3503–3514
Das S et al (2015) Bioprintable, cell-laden silk fibroin-gelatin hydrogel supporting multilineage differentiation of stem cells for fabrication of three-dimensional tissue constructs. Acta Biomater 11:233–246
Ng WL, Yeong WY, Naing MW (2016) Polyelectrolyte gelatin-chitosan hydrogel optimized for 3D bioprinting in skin tissue engineering. Int J Bioprinting 2(1):53–62
Lim KS et al (2016) New visible-light photoinitiating system for improved print fidelity in gelatin-based bioinks. ACS Biomater Sci Eng 2(10):1752–1762
Kolesky DB, Homan KA, Skylar-scott MA, Lewis JA (2016) Three-dimensional bioprinting of thick vascularized tissues. PNAS 113(12):3179–3184
Park JY et al (2014) A comparative study on collagen type I and hyaluronic acid dependent cell behavior for osteochondral tissue bioprinting. Biofabrication 6(3)
Yuan Y, Chesnutt BM, Haggard WO, Bumgardner JD (2011) Deacetylation of chitosan: material characterization and in vitro evaluation via albumin adsorption and pre-osteoblastic cell cultures. Materials 4(8):1399–1416
Assaad E, Maire M, Lerouge S (2015) Injectable thermosensitive chitosan hydrogels with controlled gelation kinetics and enhanced mechanical resistance. Carbohydr Polym 130:87–96
Chenite A et al (2000) Novel injectable neutral solutions of chitosan form biodegradable gels in situ. Biomaterials 21:2155–2161
Li B et al (2015) Hydrosoluble, UV-crosslinkable and injectable chitosan for patterned cell-laden microgel and rapid transdermal curing hydrogel in vivo. Acta Biomater 22:59–69
Yang J, Bai R, Suo Z (2018) Topological adhesion of wet materials. Adv Mater 1800671:1–7
Li J et al (2017) Tough adhesives for diverse wet surfaces. Science 357(6349):378–381
Murphy SV, Skardal A, Atala A (2013) Evaluation of hydrogels for bio-printing applications. J Biomed Mater Res Pt A 101A(1):272–284
Gasperini L, Mano JF, Reis RL (2014) Natural polymers for the microencapsulation of cells. J R Soc Interface 11(100):20140817
Skardal A et al (2015) A hydrogel bioink toolkit for mimicking native tissue biochemical and mechanical properties in bioprinted tissue constructs. Acta Biomater 25:24–34
Lee Y-B et al (2010) Bio-printing of collagen and VEGF-releasing fibrin gel scaffolds for neural stem cell culture. Exp Neurol 223(2):645–652
Snyder JE et al (2011) Bioprinting cell-laden matrigel for radioprotection study of liver by pro-drug conversion in a dual-tissue microfluidic chip. Biofabrication 3(3):034112
Pati F et al (2014) Printing three-dimensional tissue analogues with decellularized extracellular matrix bioink. Nat Commun 5:3935
Wang Z, Abdulla R, Parker B, Samanipour R, Ghosh S, Kim K (2015) A simple and high-resolution stereolithography-based 3D bioprinting system using visible light crosslinkable bioinks. Biofabrication 7(4):045009
Bertassoni LE et al (2014) Hydrogel bioprinted microchannel networks for vascularization of tissue engineering constructs. Lab Chip 14:2202–2211
F. Y. Hsieh, H. H. Lin, and S. H. Hsu, “3D bioprinting of neural stem cell-laden thermoresponsive biodegradable polyurethane hydrogel and potential in central nervous system repair,” Biomaterials, vol. 71:48–57, 2015.
Levato R, Visser J, Planell JA, Engel E, Malda J, Mateos-Timoneda MA (2014) Biofabrication of tissue constructs by 3D bioprinting of cell-laden microcarriers. Biofabrication 6:035020
Jung JW, Lee JS, Cho DW (2016) Computer-aided multiple-head 3D printing system for printing of heterogeneous organ/tissue constructs. Sci Rep 6(February):1–9
Righetti PG, Brost BCW, Snyder RS (1981) On the limiting pore size of hydrophilic gels for electrophoresis and isoelectric focussing. J Biochem Biophys Methods 4:347–363
Buckley CT, Thorpe SD, O’Brien FJ, Robinson AJ, Kelly DJ (2009) The effect of concentration, thermal history and cell seeding density on the initial mechanical properties of agarose hydrogels. J Mech Behav Biomed Mater 2(5):512–521
Duarte Campos DF et al (2015) The stiffness and structure of three-dimensional printed hydrogels direct the differentiation of mesenchymal stromal cells toward adipogenic and osteogenic lineages. Tissue Eng Pt A 21(3–4):740–756
Armstrong JPK, Burke M, Carter BM, Davis SA, Perriman AW (2016) 3D bioprinting using a templated porous bioink. Adv Healthc Mater 5(14):1724–1730
Gao Q, He Y, Fu JZ, Liu A, Ma L (2015) Coaxial nozzle-assisted 3D bioprinting with built-in microchannels for nutrients delivery. Biomaterials 61:203–215
Bencherif SA et al (2012) Injectable preformed scaffolds with shape-memory properties. Proc Natl Acad Sci 109(48):19590–19595
Wang L et al (2017) UV-crosslinkable and thermo-responsive chitosan hybrid hydrogel for NIR-triggered localized on-demand drug delivery. Carbohydr Polym 174(July):904–914
Wu Q, Therriault D, Heuzey MC (2018) Processing and properties of chitosan inks for 3D printing of hydrogel microstructures. ACS Biomater Sci Eng 4(7):2643–2652
Duan B, Kapetanovic E, Hockaday LA, Butcher JT (2014) Three-dimensional printed trileaflet valve conduits using biological hydrogels and human valve interstitial cells. Acta Biomater 10(5):1836–1846
Matthews JA, Wnek GE, Simpson DG, Bowlin GL (2002) Electrospinning of collagen nanofibers. Biomacromolecules 3(2):232–238
Jang J, Kim TG, Kim BS, Kim SW, Kwon SM, Cho DW (2016) Tailoring mechanical properties of decellularized extracellular matrix bioink by vitamin B2-induced photo-crosslinking. Acta Biomater 33:88–95
Wu Z, Su X, Xu Y, Kong B, Sun W, Mi S (2016) Bioprinting three-dimensional cell-laden tissue constructs with controllable degradation. Sci Rep 6:24474
Zhao Y, Li Y, Mao S, Sun W, Yao R (2015) The influence of printing parameters on cell survival rate and printability in microextrusion-based 3D cell printing technology. Biofabrication 7(4):045002
Müller M, Becher J, Schnabelrauch M, Zenobi-Wong M (2015) Nanostructured pluronic hydrogels as bioinks for 3D bioprinting. Biofabrication 7(3):035006
Highley CB, Song KH, Daly AC, Burdick JA (2019) Jammed microgel inks for 3D printing applications. Adv Sci 6(1):1801076
Lee JS, Hong JM, Jung JW, Shim JH, Oh JH, Cho DW (2014) 3D printing of composite tissue with complex shape applied to ear regeneration. Biofabrication 6(2):024103
Kundu J, Shim JH, Jang J, Kim SW, Cho DW (2015) An additive manufacturing-based PCL-alginate-chondrocyte bioprinted scaffold for cartilage tissue engineering. J Tissue Eng Regen Med 9(11):1286–1297
Zheng Z et al (2018) 3D bioprinting of self-standing silk-based bioink. Adv Healthc Mater 7(6):1–12
Wu D et al (2018) 3D bioprinting of gellan gum and poly (ethylene glycol) diacrylate based hydrogels to produce human-scale constructs with high-fidelity. Mater Des 160:486–495
Almeida CR, Serra T, Oliveira MI, Planell JA, Barbosa MA, Navarro M (2014) Acta Biomaterialia Impact of 3-D printed PLA- and chitosan-based scaffolds on human monocyte / macrophage responses : Unraveling the effect of 3-D structures on inflammation. Acta Biomater 10(2):613–622
Xiaohua L, Peter M (2004) Polymeric scaffolds for bone tissue engineering. Ann Biomed Eng 32(3):477–486
Karageorgiou V, Kaplan D (2005) Porosity of 3D biomaterial scaffolds and osteogenesis. Biomaterials 26(27):5474–5491
Homan KA et al (2016) Bioprinting of 3D convoluted renal proximal tubules on perfusable chips. Sci Rep 6:1–13
Sell SA, McClure MJ, Garg K, Wolfe PS, Bowlin GL (2009) Electrospinning of collagen/biopolymers for regenerative medicine and cardiovascular tissue engineering. Adv Drug Deliv Rev 61(12):1007–1019
Zhang H, Liu X, Yang M, Zhu L (2015) Silk fibroin/sodium alginate composite nano-fibrous scaffold prepared through thermally induced phase-separation (TIPS) method for biomedical applications. Mater Sci Eng C 55:8–13
Rodriguez MJ, Brown J, Giordano J, Lin SJ, Omenetto FG, Kaplan DL (2017) Silk based bioinks for soft tissue reconstruction using 3-dimensional (3D) printing with in vitro and in vivo assessments. Biomaterials 117:105–115
Shanjani Y, Pan CC, Elomaa L, Yang Y (2015) A novel bioprinting method and system for forming hybrid tissue engineering constructs A novel bioprinting method and system for forming hybrid tissue engineering constructs. Biofabrication 7(4):045008
Ouyang L, Highley CB, Rodell CB, Sun W, Burdick JA (2016) 3D printing of shear-thinning hyaluronic acid hydrogels with secondary cross-linking. ACS Biomater Sci Eng 2(10):1752–1762
Duan B, Hockaday LA, Kang KH, Butcher JT (2013) 3D bioprinting of heterogeneous aortic valve conduits with alginate/gelatin hydrogels. J Biomed Mater Res Pt A 101A(5):1255–1264
Rhee S, Puetzer JL, Mason BN, Reinhart-King CA, Bonassar LJ (2016) 3D bioprinting of spatially heterogeneous collagen constructs for cartilage tissue engineering. ACS Biomater Sci Eng 2(10):1800–1805
Lee V et al (2014) Design and fabrication of human skin by three-dimensional bioprinting. Tissue Eng Part C Methods 20(6):473–484
Ng WL, Yeong WY, Naing MW (2016) Development of polyelectrolyte chitosan-gelatin hydrogels for skin bioprinting. Proc CIRP 49:105–112
Martínez Ávila H, Schwarz S, Rotter N, Gatenholm P (2016) 3D bioprinting of human chondrocyte-laden nanocellulose hydrogels for patient-specific auricular cartilage regeneration. Bioprinting:1, 22–2, 35
Mironov V, Visconti RP, Kasyanov V, Forgacs G, Drake CJ, Markwald RR (2009) Biomaterials organ printing : Tissue spheroids as building blocks. Biomaterials 30(12):2164–2174
Lee VK et al (2014) Creating perfused functional vascular channels using 3D bio-printing technology. Biomaterials 35(28):8092–8102
Wüst S, Müller R, Hofmann S (2015) 3D Bioprinting of complex channels—effects of material, orientation, geometry, and cell embedding. J Biomed Mater Res Pt A 103(8):2558–2570
Ozbolat IT (2015) Bioprinting scale-up tissue and organ constructs for transplantation. Trends Biotechnol 33(7):395–400
Veiseh O et al (2015) Size- and shape-dependent foreign body immune response to materials implanted in rodents and non-human primates. Nat Mater 14(6):643–651
Ratner BD et al (2010) Proangiogenic scaffolds as functional templates for cardiac tissue engineering. Proc Natl Acad Sci 107(34):15211–15216
Kim YK, Que R, Wang S-W, Liu WF (2014) Modification of biomaterials with a self-protein inhibits the macrophage response. Adv Healthc Mater 3(7):989–994
Tsai RK, Rodriguez PL, Discher DE, Pantano DA, Harada T, Christian DA (2013) Minimal ‘self’ peptides that inhibit phagocytic clearance and enhance delivery of nanoparticles. Science 339(6122):971–975
Becker ST et al (2012) Endocultivation: the influence of delayed vs. simultaneous application of BMP-2 onto individually formed hydroxyapatite matrices for heterotopic bone induction. Int J Oral Maxillofac Surg 41(9):1153–1160
Lake GJ, Thomas AG (1967) The Strength of Highly Elastic Materials. Proc R Soc A Math Phys Eng Sci 300(1460):108–119
Zhao X (2014) Multi-scale multi-mechanism design of tough hydrogels: Building dissipation into stretchy networks. Soft Matter 10(5):672–687
Gong JP, Katsuyama Y, Kurokawa T, Osada Y (2003) Double-network hydrogels with extremely high mechanical strength. Adv Mater 15(14):1155–1158
Sun J et al (2012) Highly stretchable and tough hydrogels. Nature 489(7414):133–136
Yang Y, Wang X, Yang F, Shen H, Wu D (2016) A universal soaking strategy to convert composite hydrogels into extremely tough and rapidly recoverable double-network hydrogels. Adv Mater:7178–7184
Bai R, Yang J, Suo Z (2019) Fatigue of hydrogels. Eur J Mech A/Solids 74(2018):337–370
Acknowledgements
I would like to thank Dr. Luc Mongeau and Dr. Jianyu Li (Department of Mechanical Engineering, McGill University) for inspiring my research on biofabrication for tissue engineering.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Bao, G. (2020). Biofabrication in Tissue Engineering. In: Li, B., Moriarty, T., Webster, T., Xing, M. (eds) Racing for the Surface. Springer, Cham. https://doi.org/10.1007/978-3-030-34471-9_12
Download citation
DOI: https://doi.org/10.1007/978-3-030-34471-9_12
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-34470-2
Online ISBN: 978-3-030-34471-9
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)