Abstract
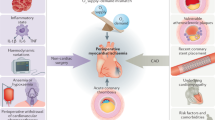
Mechanical complications of coronary artery disease are rare but frequently lead to fatal outcomes. Saving critically ill patients may be possible with optimal timing of surgical intervention. While selecting the most appropriate patients for these life-saving therapies is difficult in the acuity of the moment, certain perioperative variables can guide clinicians’ decision-making.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Jeppsson A, Liden H, Johnsson P, Hartford M, Kjell R. Surgical repair of post-infarction ventricular septal defects: a national experience. Eur J Cardiothorac Surg. 2005;27(2):216–21.
Birnbaum Y, Fishbein MC, Blanche C, Siegel RJ. Ventricular septal rupture after acute myocardial infarction. N Engl J Med. 2002;347(18):1426–32.
Crenshaw BS, Granger CB, Birnbaum Y, et al. Risk factors, angiographic patterns, and outcomes in patients with ventricular septal defect complicating acute myocardial infarction. GUSTO-I (Global Utilization of Streptokinase and TPA for Occluded Coronary Arteries) Trial Investigators. Circulation. 2000;101(1):27–32.
Barker TA, Ramnarine IR, Woo EB, et al. Repair of post-infarct ventricular septal defect with or without coronary artery bypass grafting in the northwest of England: a 5-year multi-institutional experience. Eur J Cardiothorac Surg. 2003;24(6):940–6.
Perrotta S, Lentini S. In patients undergoing surgical repair of post-infarction ventricular septal defect, does concomitant revascularization improve prognosis? Interact Cardiovasc Thorac Surg. 2009;9(5):879–87.
Lundblad R, Abdelnoor M, Geiran OR, Sennevig E. Surgical repair of postinfarction ventricular septal rupture: risk factors of early and late death. J Thorac Cardiovasc Surg. 2009;137(4):862–8.
Braunwald E, Bonow R. Braunwald’s heart disease: a textbook of cardiovascular medicine. Philadelphia: Saunders; 2001.
Cabin H, Roberts W. True left ventricular aneurysm and healed myocardial infarction. Clinical and necropsy observations including quantification of degrees of coronary arterial narrowing. Am J Cardiol. 1980;46(5):754–63.
Lascault G, Reeves F, Drobinski G. Evidence of the inaccuracy of standard echocardiographic and angiographic criteria used for the recognition of true and “false” left ventricular inferior aneurysms. Br Heart J. 1988;60(2):125–7.
Levin D, Fallon J. Significance of the angiographic morphology of localized coronary stenoses: histopathologic correlations. Circulation. 1982;66(2):316–20.
March KL, Sawada SG, Tarver RD, Kesler KA, Armstrong WF. Current concepts of left ventricular pseudoaneurysm: pathophysiology, therapy, and diagnostic imaging methods. Clin Cardiol. 1989;12(9):531–40.
Lee R, Hoercher K, McCarthy P. Ventricular reconstruction surgery for congestive heart failure. Cardiology. 2004;101(1–3):61–71.
Franco-Cereceda A, McCarthy EH, Blackstone KJ, et al. Partial left ventriculectomy for dilated cardiomyopathy: is this an alternative to transplantation? J Thorac Cardiovasc Surg. 2001;121(5):879–93.
Bredin F, Franco-Cereceda F. Midterm results of passive containment surgery using the acorn Cor Cap cardiac support device in dilated cardiomyopathy. J Card Surg. 2010;25(1):107–12.
Jones RH, Velazquez EJ, Michler RE, et al. Coronary bypass surgery with or without surgical ventricular reconstruction. N Engl J Med. 2009;360(17):1705–17.
Bizzarri F, Consalvo M, Massimo R, et al. Cardiogenic shock as a complication of acute mitral valve regurgitation following posteromedial papillary muscle infarction in the absence of coronary artery disease. J Cardiothorac Surg. 2008;3:61.
Chevalier P, Burri H, Fahrat F, et al. Perioperative outcome and long-term survival of surgery for acute post-infarction mitral regurgitation. Eur J Cardiothorac Surg. 2004;26(2):330–5.
Estes EH, Dalton FM, Entman ML, et al. The anatomy and blood supply of the papillary muscles of the left ventricle. Am Heart J. 1966;71(3):356–62.
Jouan J, Tapia M, Cook RC, Lansac E, Acar C. Ischemic mitral valve prolapse: mechanisms and implications for valve repair. Eur J Cardiothorac Surg. 2004;26(6):1112–7.
Kan CB, Chu IT, Chang RY, Chang JP. Postinfarction left ventricular rupture salvaged by resuscitation-induced pericardial tear. Ann Thorac Surg. 2010;89(6):2030–2.
Edwards J. An atlas of acquired diseases of the heart and great vessels. Philadelphia: Saunders; 1961.
Atik FA, Navia JL, Vega PR, et al. Surgical treatment of postinfarction left ventricular pseudoaneurysm. Ann Thorac Surg. 2007;83(2):526–31.
Eren E, Bozbuga N, Keles C, et al. Surgical treatment of post-infarction left ventricular pseudoaneurysm: a two-decade experience. Tex Heart Inst J. 2007;34(1):47–51.
Sakaguchi G, Komiya T, Tamura N, Kobayashi T. Surgical treatment for postinfarction left ventricular free wall rupture. Ann Thorac Surg. 2008;85(4):1344–6.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2012 Springer Science+Business Media, LLC
About this chapter
Cite this chapter
Komanapalli, C.B., Krishnan, B., John, R. (2012). Noncoronary Surgical Therapy for Ischemic Heart Disease. In: Vlodaver, Z., Wilson, R., Garry, D. (eds) Coronary Heart Disease. Springer, Boston, MA. https://doi.org/10.1007/978-1-4614-1475-9_23
Download citation
DOI: https://doi.org/10.1007/978-1-4614-1475-9_23
Published:
Publisher Name: Springer, Boston, MA
Print ISBN: 978-1-4614-1474-2
Online ISBN: 978-1-4614-1475-9
eBook Packages: MedicineMedicine (R0)