Abstract
Objectives
Chronic respiratory diseases (CRD) put patients at increased risk of respiratory infection and antimicrobial use, but surveillance results on community antimicrobial use are generally not adjusted for this risk factor. The objective of this study was to demonstrate the importance of accounting for CRD when interpreting indicators of community antimicrobial use in people over 65 years old, in Québec, Canada.
Methods
Retrospective cohort study of antimicrobial use according to CRD status in individuals over 65 years old covered by Québec’s public drug insurance plan between 2010 and 2015. Defined daily doses per 1000 person-days (DID) were computed per antimicrobial class and were further stratified according to chronic disease group, fiscal year, gender and age group.
Results
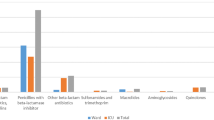
Antimicrobial use was 2.3 times higher in the CRD group (29.7 DID) compared with the other chronic disease group (13.1 DID) and 3.1 times higher than in the no chronic disease group (9.6 DID). The same gradient was reflected as well in use per antimicrobial class, per age group, per gender, and in time. Antimicrobial use increased throughout the study period and was higher in older age groups and in women.
Conclusions
Interpretation of results of antimicrobial use surveillance should consider the prevalence of CRD in populations. In order to identify opportunities for adapted interventions targeting inappropriate use, finer analyses are necessary.
Résumé
Objectifs
Les maladies respiratoires chroniques (MRC) accroissent le risque d’infection respiratoire des patients ainsi que leur utilisation d’antibiotiques, mais les résultats de surveillance de l’utilisation communautaire d’antibiotiques ne sont généralement pas ajustés pour ce facteur. L’objectif était de démontrer l’importance de prendre les MRC en compte lors de l’interprétation des indicateurs d’utilisation communautaire d’antibiotiques chez les personnes de plus de 65 ans au Québec, Canada.
Méthodologie
Étude de cohorte rétrospective portant sur l’utilisation d’antibiotiques selon la présence de MRC chez les individus de plus de 65 ans qui étaient couverts par le régime public d’assurance médicament du Québec, entre 2010 et 2015. Les doses journalières définies par 1000 individus-jours (DIJ) ont été calculées selon la classe d’antibiotiques, le groupe de maladie chronique, l’année financière, le genre et le groupe d’âge.
Résultats
L’utilisation d’antibiotiques était 2,3 fois plus élevée chez les individus ayant une MRC (29,7 DIJ) que chez ceux ayant une autre maladie chronique (13,1 DIJ) et 3,1 fois plus élevée que chez les individus n’ayant pas de maladie chronique (9,6 DIJ). Le même gradient était observable par classe d’antibiotiques, groupe d’âge, genre et année. L’utilisation d’antibiotiques a augmenté tout au long de la période à l’étude et elle était plus élevée chez les personnes plus âgées et chez les femmes.
Conclusions
La prévalence des MRC devrait être prise en compte lors de l’interprétation des résultats de surveillance de l’utilisation d’antibiotiques. Des analyses plus fines sont nécessaires afin d’identifier des opportunités d’interventions adaptées ciblant l’usage inapproprié des antibiotiques.
Similar content being viewed by others
References
Adeloye, D., Chua, S., Lee, C., Basquill, C., Papana, A., Theodoratou, E., et al. (2015). Global and regional estimates of COPD prevalence: systematic review and meta–analysis. J Glob Health, 5(2).
Agence de la santé publique du Canada. (2017). Système canadien de surveillance de la résistance aux antimicrobiens – Rapport de 2017. Gouvernement du Canada 139 p.
BCCDC. (2014). Antibiotic utilization in the Province of British Columbia. Vancouver: BCCDC 110 p. http://www.bccdc.ca/resourcegallery/Documents/Statistics%20and%20Research/Statistics%20and%20Reports/Epid/Antibiotics/Reportonantibioticutilization2013_Nov12_FINAL.pdf. Consulted June 6th, 2019.
Blais, C., Jean, S., Sirois, C., Rochette, L., Plante, C., Larocque, I., et al. (2014). Quebec Integrated Chronic Disease Surveillance System (QICDSS), an innovative approach. Chronic Dis Inj Can, 34(4), 226–235.
Cadieux, G., Tamblyn, R., Dauphinee, D., & Libman, M. (2007). Predictors of inappropriate antibiotic prescribing among primary care physicians. Can Med Assoc J, 177(8), 877–883.
Dziurda, D. R., Polak, S., Skowron, A., Kuschill-Dziurda, J., & Brandys, J. (2008 Jun). Antibacterial drug prescription for outpatients: age, seasonal and pulmonary disease dependency. Acta Pol Pharm, 65(3), 391–397.
ECDC (2019). European Surveillance of Antimicrobial Consumption Network (ESAC-Net). Available from: http://ecdc.europa.eu/en/healthtopics/antimicrobial-resistance-and-consumption/antimicrobial-consumption/ESAC-Net/Pages/ESAC-Net.aspx. Consulted June 6th, 2019.
Fleming-Dutra, K. E., Hersh, A. L., Shapiro, D. J., Bartoces, M., Enns, E. A., File, T. M., et al. (2016). Prevalence of inappropriate antibiotic prescriptions among US ambulatory care visits, 2010-2011. JAMA., 315(17), 1864.
Gaardbo Kuhn, K., Hammerum, A. M., & Jensen, U. S. (2014). The association between demographic factors and increased antibiotic consumption in Denmark 2001 to 2010. Scand J Infect Dis, 46(8), 599–604.
Gershon, A. S., Wang, C., Guan, J., Vasilevska-Ristovska, J., Cicutto, L., & To T. (2009a). Identifying patients with physician-diagnosed asthma in health administrative databases. Can Respir J, 16(6), 183–188.
Gershon, A. S., Wang, C., Guan, J., Vasilevska-Ristovska, J., Cicutto, L., & To T. (2009b). Identifying individuals with physician diagnosed COPD in health administrative databases. COPD J Chronic Obstr Pulm Dis, 6(5), 388–394.
Institut de la statistique du Québec (2014). Le bilan démographique du Québec. Gouvernement du Québec. 163 p.
Institut national de santé publique du Québec, Comité d’experts sur la résistance aux antibiotiques, Bourgault, A.-M., Domingo, M.-C., Fortin, A., Malouin, F., et al. (2015). Surveillance intégrée de la résistance aux antibiotiques: cadre de référence. Gouvernement du Québec 51 p.
Public Health England. (2017). English surveillance programme for antimicrobial utilisation and resistance (ESPAUR) - Report 2017. London: Public Health England 188 p.
Santos, S., Marín, A., Serra-Batlles, J., de la Rosa, D., Solanes, I., Pomares, X., et al. (2016). Treatment of patients with COPD and recurrent exacerbations: the role of infection and inflammation. Int J Chron Obstruct Pulmon Dis, 515.
Statens Serum Institut, National Veterinary Institute, National Food Institute. (2017). DANMAP 2016 - Use of antimicrobial agents and occurrence of antimicrobial resistance in bacteria from food animals, food and humans in Denmark. Lyngby: National Food Institute and Statens Serum Institut 130 p.
The White House. (2014). National strategy for combating antibiotic-resistant bacteria. Washington: The White House Available from: https://obamawhitehouse.archives.gov/sites/default/files/docs/carb_national_strategy.pdf. Consulted June 6th, 2019.
Transatlantic Taskforce on Antimicrobial Resistance (2014). Transatlantic taskforce on antimicrobial resistance progress report - recommendations for future collaboration between the US and EU. Available from: http://www.cdc.gov/drugresistance/pdf/TATFAR-Progress_report_2014.pdf. Consulted June 6th, 2019.
WHO Collaborating Centre for Drug Statistics Methodology; Norwegian Institute of Public Health. (2019). Guidelines for ATC classification and DDD assignment (22nd ed.). Oslo: WHO Collaborating Centre for Drug Statistics Methodology 283 p.
Funding
This work was supported by the Ministère de la Santé et des services sociaux du Québec.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PDF 388 kb)
Rights and permissions
About this article
Cite this article
Fortin, É., Jean, S., Sirois, C. et al. Chronic respiratory disease should be considered when interpreting indicators of community antimicrobial use in people over 65 years old. Can J Public Health 111, 443–447 (2020). https://doi.org/10.17269/s41997-019-00278-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.17269/s41997-019-00278-1