Abstract
OBJECTIVES: The objective of the Immediate Staging Pilot Project (ISPP) was to improve linkage to human immunodeficiency virus (HIV) care by increasing the number of referrals made to HIV care, and to decrease the time between diagnosis and linkage to care for newly diagnosed HIV clients. This pilot had the potential to decrease HIV transmission at a population level by engaging clients in treatment earlier.
SETTING: The Bute Street Clinic and Health Initiative for Men Clinic on Davie in Vancouver, British Columbia are low-threshold public health facilities providing HIV/STI testing primarily to men who have sex with men (MSM).
INTERVENTION: To improve engagement of MSM in the cascade of HIV care, the BC Centre for Disease Control implemented a 12-month ISPP in 2012 for clients newly diagnosed with HIV. The pilot offered CD4 and viral load testing at the time of diagnosis, implemented improved referral procedures and enhanced nursing support for clients.
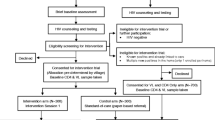
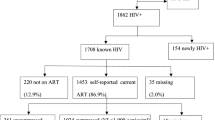
OUTCOMES: Comparing linkage to care outcomes between a group that received the standard of care (SOC) and an intervention group that received immediate staging, the median linkage to care time decreased from 21.5 to 14.0 days respectively (p = 0.053). The referral rates to HIV care were 56.1% in the SOC group and 94.1% in the intervention group (p < 0.001).
CONCLUSION:Creating best practices that include offering CD4 and viral load testing at the time of diagnosis, enhanced nursing support and standardized referral processes has facilitated an improvement in the quality of HIV services provided to MSM clients attending low-threshold clinics.
Résumé
OBJECTIFS: Le projet pilote ISPP (Immediate Staging Pilot Project ou projet pilote de mise en place immédiate) visait à améliorer le lien vers les soins du virus de l’immunodéficience humaine (VIH) en augmentant le nombre d’orientations vers les soins du VIH, et à réduire le délai entre le diagnostic et le lien vers les soins pour les patients ayant reçu un diagnostic récent de VIH. Le projet pilote pouvait potentiellement réduire la transmission du VIH dans l’ensemble de la population en amorçant le traitement des patients plus tôt.
LIEU: Les cliniques Bute Street Clinic et Health Initiative for Men on Davie de Vancouver (Colombie-Britannique) sont des établissements de santé publique à seuil bas qui offrent le dépistage du VIH et des ITS principalement aux hommes ayant des relations sexuelles avec des hommes (HARSAH).
INTERVENTION: Pour améliorer l’intégration des HARSAH dans le flot des soins du VIH, le BC Centre for Disease Control a mis en œuvre ce projet pilote de 12 mois pour les patients ayant reçu un diagnostic récent de VIH. Le projet pilote offrait la numération des lymphocytes CD4 et la mesure de la charge virale au moment du diagnostic, appliquait une procédure d’orientation améliorée et rehaussait le soutien infirmier des patients.
RÉSULTATS: En comparant les résultats du lien vers les soins entre un groupe ayant reçu la norme de soins (NDS) et un groupe d’intervention ayant reçu la mise en place immédiate des soins, la durée médiane du lien vers les soins a diminué, passant de 21,5 à 14 jours, respectivement (p = 0,053). Les taux d’orientation vers les soins du VIH étaient de 56,1% dans le groupe de la NDS et de 94,1% dans le groupe d’intervention (p < 0,001).
CONCLUSION: La création de pratiques exemplaires incluant la numération des lymphocytes CD4 et la mesure de la charge virale au moment du diagnostic, un soutien infirmier renforcé et des processus d’orientation standardisés a favorisé une amélioration de la qualité des services VIH offerts aux patients HARSAH fréquentant des cliniques à seuil bas.
Similar content being viewed by others
References
Joint United Nations Programme on HIV/AIDS. Global Report: UNAROS Report on the Global AIDS Epidemic 2013. Geneva, Switzerland: UNAIDS, 2013. Available at: http://www.unaids.org/sites/default/files/media_asset/UNAlDS_ Global_Report_2013_en_1.pdf (Accessed May 25, 2016).
BC Centre for Disease Control. HIV in British Columbia: Annual Surveillance Report 2014. Vancouver, BC: BCCDC, 2015. Available at: http://www.bccdc.ca/resource-gallery/Documents/StatisticsandResearch/Statisticsand Reports/STI/HIV_Annual_Report_2014-FINAL.pdf (Accessed May 25, 2016).
Gill VS, Lima VD, Zhang W, Wynhoven B, Yip B, Hogg RS, et al. Improved virological outcomes in British Columbia concomitant with decreasing incidence of HIV type 1 drug resistance detection. Clin Infect Dis 2010;50(1):98–105. PMID: 19951169. doi: 10.1086/648729.
Engsig FN, Zangerle R, Katsarou O, Dabis F, Reiss P, Gill J, et al. Long-term mortality in HIV-positive individuals virally suppressed for >3 years with incomplete CD4 recovery. Clin Infect Dis 2014;58(9):1312–21. PMID: 24457342. doi: 10.1093/cid/ciu038.
Castel AD, Greenberg AE, Befus M, Willis S, Samala R, Rocha N, et al. Temporal association between expanded HIV testing and improvements in population-based HIV/AIDS clinical outcomes, District of Columbia. AIDS Care 2014;26(6):785–89. PMID: 24206005. doi: 10.1080/09540121.2013.855296.
HIV-CAUSAL Collaboration, Cain LE, Logan R, Robins JM, Sterne JAC, Sabin C, et al. When to initiate combined antiretroviral therapy to reduce mortality and AIDS-defining illness in HIV-infected persons in developed countries: An observational study. Ann Intern Med 2011;154(8):509–15. PMID: 21502648. doi: 10.7326/0003-4819-154-8-201104190-00001.
Metsch LR, Pereyra M, Messinger S, Del Rio C, Strathdee SA, Anderson-Mahoney P, et al. HIV transmission risk behaviors among HIV-infected persons who are successfully linked to care. Clin Infect Dis 2008;47(4):577–84. PMID: 18624629. doi: 10.1086/590153.
Palella FJ, Armon C, Chmiel JS, Brooks JT, Debes R, Novak RM, et al. Higher CD4 at ART initiation predicts greater long term likelihood of CD4 normalization. Value Health 2014;17(3):A269. doi: 10.1016/j.jval.2014.03.1567.
Gardner EM, McLees MP, Steiner JF, Del Rio C, Burman WJ. The spectrum of engagement in HIV care and its relevance to test-and-treat strategies for prevention of HIV infection. Clin Infect Dis 2011;52(6):793–800. PMID: 21367734. doi: 10.1093/cid/ciq243.
Gilman B, Hidalgo J, Thomas C, Au M, Hargreaves M. Linkages to care for newly diagnosed individuals who test HIV positive in nonprimary care settings. AIDS Patient Care STDs 2012;26(3):132–40. PMID: 22248332. doi: 10. 1089/apc.2011.0305.
Christopoulos K, Das M, Colfax G. Linkage and retention in HIV care among men who have sex with men in the United States. Clin Infect Dis 2011;52(S2): S214–22. PMID: 21342910. doi: 10.1093/cid/ciq045.
National Centre for HIV/AIDS, Viral Hepatitis, STD and TB Prevention. Understanding the HIV Care Continuum. Atlanta, GA: US Centers for Disease Control, 2014. Available at: https://www.cdc.gov/hiv/pdf/library/factsheets/cdc-hiv-care-continuum.pdf (Accessed March 28, 2017).
Lourenço L, Colley G, Nosyk B, Shopin D, Montaner JSG, Lima VD, et al. High levels of heterogeneity in the HIV cascade of care across different population subgroups in British Columbia, Canada. PLoS ONE 2014;9(12):ell5277. PMID: 25541682. doi: 10.1371/journal.pone.0115277.
Heath K, Samji H, Nosyk B, Colley G, Gilbert M, Hogg RS, et al. Cohort profile: Seek and treat for the optimal prevention of HIV/AIDS in British Columbia (STOP HIV/AIDS BC). Int J Epidemiol 2014;43:1073–81. PMID: 24695113. doi: 10.1093/ije/dyu070.
Arreola S, Santos G-M, Beck J, Sundararaj M, Wilson PA, Hebert P, et al. Sexual stigma, criminalization, investment, and access to HIV services among men who have sex with men worldwide. AIDS Behav 2015;19(2):227–34. PMID: 25086670. doi: 10.1007/s10461-014-0869-x.
Spielberg F, Branson BM, Goldbaum GM, Lockhart D, Kurth A, Celum CL, et al. Overcoming barriers to HIV testing: Preferences for new strategies among clients of a needle exchange, a sexually transmitted disease clinic, and sex venues for men who have sex with men. J Acquir Immune Defic Syndr 2003;32(3):318–27. PMID: 12626893. doi: 10.1097/00126334-200303010-00012.
Edland-Gryt M, Skatvedt AH. Thresholds in a low-threshold setting: An empirical study of barriers in a centre for people with drug problems and mental health disorders. Int J Drug Policy 2013;24(3):257–64. PMID: 23036653. doi: 10.1016/j.drugpo.2012.08.002.
Office of the Provincial Health Officer. HIV Testing Guidelines for the Province of British Columbia. Vancouver, BC: BC Ministry of Health, 2014. Available at: http://hivguide.ca/images/HIV_Guide.pdf (Accessed June 19, 2016).
Vojnov L, Markby J, Boeke C, Harris L, Ford N, Peter T. POC CD4 testing improves linkage to HIV care and timeliness of ART initiation in a public health approach: A systematic review and meta-analysis. PLoS ONE 2016;11(5):e0155256. PMID: 27175484. doi: 10.1371/journal.pone.0155256.
Montaner JSG, Lima VD, Barrios R, Yip B, Wood E, Kerr T, et al. Association of highly active antiretroviral therapy coverage, population viral load, and yearly new HIV diagnoses in British Columbia, Canada: A population-based study. Lancet (London, England) 2010;376:532–39. doi: 10.1016/S0140-6736(10)60936-1.
Montaner JSG, Lima VD, Harrigan PR, Lourenço L, Yip B, Nosyk B, et al. Expansion of HAART coverage is associated with sustained decreases in HIV/AIDS morbidity, mortality and HIV transmission: The HIV Treatment as Prevention experience in a Canadian setting. PLoS ONE 2014;9:e87872. PMID: 24533061. doi: 10.1371/journal.pone.0087872.
Thompson M, Mugavero M, Amico R, Cargill V, Chang L, Gross R, et al. Guidelines for improving entry into and retention in care and antiretroviral adherence for persons with HIV: Evidence-based recommendations from an International Association of Physicians in AIDS Care panel. Ann Intern Med 2012;156:817–33, W-284-94. PMID: 22393036. doi: 10.7326/0003-4819-156-11-201206050-00419.
Hightow-Weidman LB, Jones K, Wohl AR, Futterman D, Outlaw A, Phillips G, et al. Early linkage and retention in care: Findings from the outreach, linkage, and retention in care initiative among young men of color who have sex with men. AIDS Patient Care STDs 2011;25(Suppl 1):S31–38. PMID: 21711141. doi: 10.1089/apc.2011.9878.
Gerbert B, Love C, Caspers N, Linkins K, Burack JH. Making all the difference in the world: How physicians can help HIV-seropositive patients become more involved in their healthcare. AIDS Patient Care STDs 1999;13(1):29–39. PMID: 11362084. doi: 10.1089/apc.1999.13.29.
Larson BA, Schnippel K, Ndibongo B, Xulu T, Brennan A, Long L, et al. Rapid point-of-care CD4 testing at mobile HIV testing sites to increase linkage to care: An evaluation of a pilot program in South Africa. J Acquir Immune Defic Syndr 2012;61(2):e13–17. PMID: 22659650. doi: 10.1097/QAI.0b013e31825eec60.
Saleem HT, Mushi D, Hassan S, Bruce RD, Cooke A, Mbwambo J, et al. “Can’t you initiate me here?”: Challenges to timely initiation on antiretroviral therapy among methadone clients in Dar es Salaam, Tanzania. Int J Drug Policy 2016;30:59–65. PMID: 26831364. doi: 10.1016/j.drugpo.2015.12.009.
Wynberg E, Cooke G, Shroufi A, Reid SD, Ford N. Impact of point-of-care CD4 testing on linkage to HIV care: A systematic review. J Int AIDS Soc 2014;17:18809. PMID: 24447595. doi: 10.7448/IAS.17.1.18809.
Liu Y, Osborn CY, Qian H-Z, Yin L, Xiao D, Ruan Y, et al. Barriers and facilitators of linkage to and engagement in HIV care among HIV-positive men who have sex with men in China: A qualitative study. AIDS Patient Care STDs 2016;30(2):70–77. PMID: 26784360. doi: 10.1089/apc.2015.0296.
Nosyk B, Montaner JSG, Colley G, Lima VD, Chan K, Heath K, et al. The cascade of HIV care in British Columbia, Canada, 1996–2011: A population-based retrospective cohort study. Lancet Infect Dis 2014;14(1):40–49. PMID: 24076277. doi: 10.1016/S1473-3099(13)70254-8.
Author information
Authors and Affiliations
Corresponding author
Additional information
Acknowledgements: The authors acknowledge the nurses at the Bute Street and HIM on Davie Clinics, Annelies Becu, Teddy Consolacion and Heather Pedersen, whose contributions made this program possible. This project was operationally supported by the BC Centre for Disease Control.
Conflict of Interest: None to declare.
Rights and permissions
About this article
Cite this article
Brownrigg, B., Taylor, D., Phan, F. et al. Improving linkage to HIV care at low-threshold STI/HIV testing sites: An evaluation of the Immediate Staging Pilot Project in Vancouver, British Columbia. Can J Public Health 108, e79–e84 (2017). https://doi.org/10.17269/CJPH.108.5753
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.17269/CJPH.108.5753
Key Words
- Linkage to care
- continuum of care
- HIV
- men who have sex with men
- low-threshold sites
- outcome assessment (health care)