Abstract
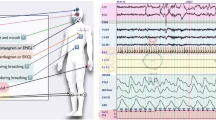
The relationship between epilepsy and sleep is complex and bidirectional. Ictal awakening is probably a common and well-described phenomenon. In this small observational study we describe arousal from sleep as the only, or at least main, manifestation of some epileptic seizures. We coin the term “hypnopompic seizures” to describe this entity. Five patients with intractable epilepsy were monitored by continuous video-electroencephalogram. Four of them had left temporal lobe epilepsy and one patient had generalised epilepsy. Hypnopompic seizures accounted for 30–100% of their seizure types captured during monitoring. All the seizures occurred during stage II sleep and were brief. Hypnopompic seizures are extremely subtle and may be underdiagnosed and underreported. Future larger studies are needed to shed some light on this unique entity and its neuropathophysiology. Epileptologists should be aware of this type of seizure and careful review of electroencephalograms during the transition from sleep to arousal is imperative to capture these seizures. Physicians, patients and families also need to be aware of such a subtle manifestation of seizures. Improved awareness of hypnopompic seizures and subtle seizures, in general, help guide accurate and early diagnosis, thorough monitoring and appropriate management.
Article PDF
Similar content being viewed by others
References
Afifi AK, Bergman RA. Functional Neuroanatomy. In: New York: The McGraw Hill Companies Inc, 2005:402–403.
Blumfield H. Neuroanatomy through Clinical Cases. Sunderland: Massachussets: Sinauer Associates Inc, 2002:590–591.
Dasheiff RM, Kofke WA. Primarily generalized seizures are more effective than partial seizures in arousing patients from sleep. Neurol Res 2003;25:63–67.
Giovacchini G, Toczek MT, Bonwetsch R, et al. 5-HT 1A receptors are reduced in temporal lobe epilepsy after partial-volume correction. J Nucl Med 2005;46:1128–1135.
Janz D. Epilepsy and the sleeping-waking cycle. In: Magnus O, Lorentz de Hass, AM. The Epilepsies, Ch 26. Handbook of Clinical Neurology, Vol 15. New York: Elsevier, 1974.
Janz D. Aufwach-Epilepsien. Arch Psychiatr Nervenkr 1953;191:73–98.
Malow BA, Bowes RJ, Ross D. Relationship of temporal lobe seizures to sleep and arousal: A combined scalp-intracranial electrode study. Sleep 2000;23:231–234.
Manni R, Galimberti CA, Sartori I, Politini L, Murelli R, Tartara A. Nocturnal partial seizures and arousals/awakenings from sleep: an ambulatory EEG study. Funct Neurol 1997;12:107–111.
Marcus JN, Aschkenasi CJ, Lee CE, et al. Differential expression of orexin receptors 1 and 2 in the rat brain. J Comp Neurol 2001;435:6–25.
Nestler EJ, Hyman SE, Malenka RC. Molecular Neuropharmacology. A Foundation for Clinical Neuroscience. In: New York: McGraw-Hill Companies, 2001:289–313.
Posner JB, Saper CB, Schiff ND, Plum F. Plum and Plosner’s diagnosis of stupor and coma. In: New York: Oxford University Press, 2007:328.
Sakurai T. Discovery of orexin. Nippon Yakurigaku Zasshi 2007;130:19–22.
Saper CB. Brainstem modulation of sensation, movement and consciousness. In: Kandel ER, Schwartz JH, Jessell TM, eds. Principles of Neural Science. New York: McGraw-Hill, 2000:889–909.
Shouse MN. Thalamocortical mechanisms of state-dependent seizures during amygdala kindling and systemic penicillin epilepsy in cats. Brain Res 1987;425:198–203.
Wieser HG. Temporal lobe epilepsy, sleep and arousal: stereo-EEG findings. Epilepsy Res 1991; 2(Suppl.): 97–119.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Awad, A.M., Lüders, H.O. Hypnopompic seizures. Epileptic Disord 12, 270–274 (2010). https://doi.org/10.1684/epd.2010.0336
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1684/epd.2010.0336