Abstract
Background
The efficacy and safety of clindamycin phosphate 1.2%/tretinoin 0.025% (Clin-RA) were evaluated in three 12-week randomised studies.
Objectives
To perform a pooled analysis of data from these studies to evaluate Clin-RA’s efficacy and safety in a larger overall population, in subgroups of adolescents and according to acne severity.
Materials & Methods
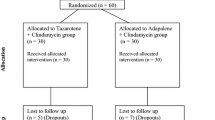
4550 patients were randomised to Clin-RA, clindamycin, tretinoin and vehicle. Evaluations included percentage change in lesions, treatment success rate, proportions of patients with ≥50% or ≥80% continuous reduction in lesions, adverse events and cutaneous tolerability.
Results
In the overall population, the percentage reduction in inflammatory, non-inflammatory and total lesions and the treatment success rate were significantly greater with Clin-RA compared with clindamycin, tretinoin and vehicle alone (all p<0.01). The percentage reduction in all types of lesions was also significantly greater with Clin-RA in the adolescent subgroup (2915 patients, p<0.002) and in patients with mild/moderate acne (3662 patients, p<0.02) versus comparators. In patients with severe acne (n = 880), the percentage reduction in all lesion types was significantly greater with Clin-RA versus vehicle (p<0.0001). A greater proportion of Clin-RA treated patients had a ≥50% or ≥80% continuous reduction in all types of lesions at week 12 compared with clindamycin, tretinoin and vehicle. Adverse event frequencies in the active and vehicle groups were similar. Baseline-adjusted mean tolerability scores over time were <1 (mild) and similar in all groups.
Conclusion
Clin-RA is safe, has superior efficacy to its component monotherapies and should be considered as one of the first-line therapies for mild-to-moderate facial acne.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Thiboutot D, Gollnick H, Bettoli V, et al. New insights into the management of acne: an update from the Global Alliance to Improve Outcomes in Acne group. J Am Acad Dermatol 2009;60:S1–50.
Gollnick H, Cunliffe W, Berson D, et al. Management of acne: a report from a Global Alliance to Improve Outcomes in Acne. J Am Acad Dermatol 2003;49:S1–37.
Nast A, Dreno B, Bettoli V, et al. European evidence-based (S3) guidelines for the treatment of acne. J Eur Acad Dermatol Venereol 2012;26(Suppl 1):1–29.
Thielitz A, Helmdach M, Ropke EM, Gollnick H. Lipid analysis of follicular casts from cyanoacrylate strips as a new method for studying therapeutic effects of antiacne agents. Br J Dermatol 2001;145:19–27.
Abdel-Naser MB, Zouboulis CC. Clindamycin phosphate/tretinoin gel formulation in the treatment of acne vulgaris. Expert Opin Pharmacother 2008;9:2931–2937.
Leyden JJ. A review of the use of combination therapies for the treatment of acne vulgaris. J Am Acad Dermatol 2003;49:S200–S210.
Dreno B. Topical antibacterial therapy for acne vulgaris. Drugs 2004;64:2389–2397.
Jain GK, Ahmed FJ. Adapalene pretreatment increases follicular penetration of clindamycin: in vitro and in vivo studies. Indian J Dermatol Venereol Leprol 2007;73:326–329.
Schlessinger J, Menter A, Gold M, et al. Clinical safety and efficacy studies of a novel formulation combining 1.2% clindamycin phosphate and 0.025% tretinoin for the treatment of acne vulgaris. J Drugs Dermatol 2007;6:607–615.
Del Rosso JQ, Jitpraphai W, Bhambri S, Momin S. Clindamycin phosphate 1.2%-tretinoin 0.025% gel: vehicle characteristics, stability, and tolerability. Cutis 2008;81:405–408.
Del Rosso JQ, Schmidt NF. A review of the anti-inflammatory properties of clindamycin in the treatment of acne vulgaris. Cutis 2010;85:15–24.
Murata K, Tokura Y. Anti-microbial therapies for acne vulgaris: anti-inflammatory actions of anti-microbial drugs and their effectiveness. J UOEH 2007;29:63–71.
Cunliffe WJ, Poncet M, Loesche C, Verschoore M. A comparison of the efficacy and tolerability of adapalene 0.1% gel versus tretinoin 0.025% gel in patients with acne vulgaris: a meta-analysis of five randomized trials. Br J Dermatol 1998;139(Suppl 52):48–56.
Goreshi R, Samrao A, Ehst BD. A double-blind, randomized, bilateral comparison of skin irritancy following application of the combination acne products clindamycin/tretinoin and benzoyl peroxide/adapalene. J Drugs Dermatol 2012;11:1422–1426.
Tanghetti EA. The role of inflammation in the pathology of acne. J Clin Aesthet Dermatol 2013;6:27–35.
Kircik LH, Peredo MI, Bucko AD, et al. Safety of a novel gel formulation of clindamycin phosphate 1.2%-tretinoin 0.025%: results from a 52-week open-label study. Cutis 2008;82:358–366.
Jackson JM, Fu JJ, Almekinder JL. A randomized, investigatorblinded trial to assess the antimicrobial efficacy of a benzoyl peroxide 5%/clindamycin phosphate 1% gel compared with a clindamycin phosphate 1.2%/tretinoin 0.025% gel in the topical treatment of acne vulgaris. J Drugs Dermatol 2010;9:131–136.
Cunliffe WJ, Holland KT, Bojar R, Levy SF. A randomized, doubleblind comparison of a clindamycin phosphate/benzoyl peroxide gel formulation and a matching clindamycin gel with respect to microbiologic activity and clinical efficacy in the topical treatment of acne vulgaris. Clin Ther 2002;24:1117–1133.
Fu LW, Vender RB. Newer approaches in topical combination therapy for acne. Skin Therapy Lett 2011;16:3–6.
Yentzer BA, Ade RA, Fountain JM, et al. Simplifying regimens promotes greater adherence and outcomes with topical acne medications: a randomized controlled trial. Cutis 2010;86:103–108.
Dreno B, Thiboutot D, Gollnick H, et al. Large-scale worldwide observational study of adherence with acne therapy. Int J Dermatol 2010;49:448–456.
Zaghloul SS, Cunliffe WJ, Goodfield MJ. Objective assessment of compliance with treatments in acne. Br J Dermatol 2005;152:1015–1021.
Kellett N, West F, Finlay AY. Conjoint analysis: a novel, rigorous tool for determining patient preferences for topical antibiotic treatment for acne. A randomised controlled trial. Br J Dermatol 2006;154:524–532.
Leyden JJ, Hickman JG, Jarratt MT, Stewart DM, Levy SF. The efficacy and safety of a combination benzoyl peroxide/clindamycin topical gel compared with benzoyl peroxide alone and a benzoyl peroxide/erythromycin combination product. J Cutan Med Surg 2001;5:37–42.
Ellis CN, Leyden J, Katz HI, et al. Therapeutic studies with a new combination benzoyl peroxide/clindamycin topical gel in acne vulgaris. Cutis 2001;67:13–20.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Dréno, B., Bettoli, V., Ochsendorf, F. et al. Efficacy and safety of clindamycin phosphate 1.2%/tretinoin 0.025% formulation for the treatment of acne vulgaris: pooled analysis of data from three randomised, double-blind, parallel-group, phase III studies. Eur J Dermatol 24, 201–209 (2014). https://doi.org/10.1684/ejd.2014.2293
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1684/ejd.2014.2293