Abstract
Introduction
Increased levels of pro- and anti-inflammatory cytokines were observed in various segments of histologically-intact small intestine in animal models of acute and chronic colitis. Whether these cytokines are produced locally or spread from the inflamed colon is not known. In addition, the role of gut innervation in this upregulation is not fully understood.
Aims
To examine whether cytokines are produced de novo in the small intestine in two rat models of colitis; and to investigate the role of capsaicin-sensitive primary afferents in the synthesis of these inflammatory cytokines.
Methods
Colitis was induced by rectal instillation of iodoacetamide (IA) or trinitrobenzene sulphonic acid (TNBS) in adult Sprague-Dawley rats. Using reverse transcriptase (RT) and real-time PCR, TNF-α, and IL-10 mRNA expression was measured in mucosal scrapings of the duodenum, jejunum, ileum and colon at different time intervals after induction of colitis. Capsaicin-sensitive primary afferents (CSPA) were ablated using subcutaneous injections of capsaicin at time 0, 8 and 32 h, and the experiment was repeated at specific time intervals to detect any effect on cytokines expression.
Results
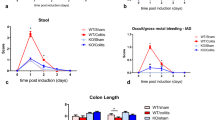
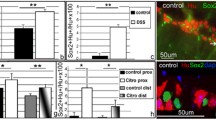
TNF-α mRNA expression increased by 3-40 times in the different intestinal segments (p<0.05 to p<0.001), 48h after IA-induced colitis. CSPA ablation completely inhibited this upregulation in the small intestine, but not in the colon. Similar results were obtained in TNBS-induced colitis at 24 h. Intestinal IL-10 mRNA expression significantly decreased at 12 h and then increased by 6-43 times (p<0.05 to p<0.001) 48h after IA administration. This increase was abolished in rats subjected to CSPA ablation except in the colon, where IL-10 further increased by twice (p<0.05). In the TNBS group, there was 4-12- and 4-7-fold increases in small intestinal IL-10 mRNA expression at 1 and 21 days after colitis induction, respectively (both p<0.01). This increase was not observed in rats pretreated with capsaicin. Capsaicin-treated and untreated rats had comparable visual ulcer scores after colitis induction.
Conclusion
Inflammatory cytokines are produced de novo in distant intestinal segments in colitis. CSPA fibers play a key role in the upregulation of this synthesis.
Similar content being viewed by others
References
Haskell H, Andrews Jr. CW, Reddy SI, et al. Pathologic features and clinical significance of “backwash” ileitis in ulcerative colitis. Am J Surg Pathol 2005; 29: 1472.
Chakravarti KR, Sehgal AK, Chakravarti RN, Chhuttani PN. A study of intestinal function and morphology in nonspecific ulcerative colitis in acute phase and remission in India. Am J Dig Dis 1973; 18: 191.
Binder HJ, Ptak T. Jejunal absorption of water and electrolytes in inflammatory bowel disease. J Lab Clin Med 1970; 76: 915.
Andersson H, Dotevall G, Gillberg G, Jagenburg R, Kock NG. Absorption studies in patients with Crohn’s disease and in patients with ulcerative colitis. Acta Med Scand 1971; 190: 407.
Salem SN, Truelove SC. Small-intestinal and gastric abnormalities in ulcerative colitis. BMJ 1965; 27: 827.
Barada KA, Kafrouni MI, Khoury CI, et al. Experimental colitis decreases rat jejunal amino acid absorption: role of capsaicin sensitive primary afferents. Life Sci 2001; 69: 3121.
Vrees MD, Pricolo VE, Potenti FM, Cao W. Abnormal motility in patients with ulcerative colitis: the role of inflammatory cytokines. Arch Surg 2002; 137: 439.
Jurjus A, Barada K, Khoury N, et al. Morphological and biochemical alterations in the jejunum following iodoacetamide-induced colitis in rats. Can J Physiol Pharmacol 2006; 84: 1191.
Mourad FH, Barada KA, Bou Rached NA, Khoury CI, Saade NE, Nassar CF. Inhibitory effect of experimental colitis on fluid absorption in rat jejunum: role of the enteric nervous system, VIP, and nitric oxide. Am J Physiol Gastrointest Liver Physiol 2006; 290: G262.
Reimund JM, Wittersheim C, Dumont S, et al. Increased production of tumour necrosis factor-alpha interleukin-1 beta, and interleukin-6 by morphologically normal intestinal biopsies from patients with Crohn’s disease. Gut 1996; 39: 684.
Reinecker HC, Steffen M, Witthoeft T, et al. Enhanced secretion of tumour necrosis factor-alpha, IL-6, and IL-1 beta by isolated lamina propria mononuclear cells from patients with ulcerative colitis and Crohn’s disease. Clin Exp Immunol 1993; 94: 174.
Yamamoto T, Maruyama Y, Umegae S, Matsumoto K, Saniabadi AR. Mucosal inflammation in the terminal ileum of ulcerative colitis patients: endoscopic findings and cytokine profiles. Dig Liver Dis 2008; 40: 253.
Leon AJ, Gomez E, Garrote JA, et al. High levels of proinflammatory cytokines, but not markers of tissue injury, in unaffected intestinal areas from patients with IBD. Mediators Inflamm 2009; 2009: 580450.
Barada K, Mourad FH, Noutsi B, Saade NE. Electrocautery-induced localized colonic injury elicits increased levels of pro-inflammatory cytokines in small bowel and decreases jejunal alanine absorption. Cytokine 2014; 71: 109.
Barada KA, Mourad FH, Sawah SI, et al. Localized colonic inflammation increases cytokine levels in distant small intestinal segments in the rat. Life Sci 2006; 79: 2032.
Mourad FH, Barada KA, Noutsi B, Saade NE. Troubleshooting in animal models of colitis: the use of a novel electrocautery model. J Pharmacol Toxicol Methods 2010; 61: 122.
Barada KA, Mourad FH, Sawah SI, et al. Up-regulation of nerve growth factor and interleukin-10 in inflamed and non-inflamed intestinal segments in rats with experimental colitis. Cytokine 2007; 37: 236.
Blandizzi C, Fornai M, Colucci R, et al. Altered prejunctional modulation of intestinal cholinergic and noradrenergic pathways by alpha2-adrenoceptors in the presence of experimental colitis. Br J Pharmacol 2003; 139: 309.
Geboes K, Collins S. Structural abnormalities of the nervous system in Crohn’s disease and ulcerative colitis. Neurogastroenterol Motil 1998; 10: 189.
Grider JR. Interleukin-1 beta selectively increases substance P release and augments the ascending phase of the peristaltic reflex. Neurogastroenterol Motil 2003; 15: 607.
Kelles A, Janssens J, Tack J. IL-1beta and IL-6 excite neurones and suppress cholinergic neurotransmission in the myenteric plexus of the guinea pig. Neurogastroenterol Motil 2000; 12: 531.
Linden DR. Colitis: it is not just for the colon anymore. Br J Pharmacol 2003; 139: 185.
Sanovic S, Lamb DP, Blennerhassett MG. Damage to the enteric nervous system in experimental colitis. Am J Pathol 1999; 155: 1051.
Morris GP, Beck PL, Herridge MS, Depew WT, Szewczuk MR, Wallace JL. Hapten-induced model of chronic inflammation and ulceration in the rat colon. Gastroenterology 1989; 96: 795.
Satoh H, Sato F, Takami K, Szabo S. New ulcerative colitis model induced by sulfhydryl blockers in rats and the effects of antiinflammatory drugs on the colitis. Jpn J Pharmacol 1997; 73: 299.
Braegger CP, Nicholls S, Murch SH, Stephens S, MacDonald TT. Tumour necrosis factor alpha in stool as a marker of intestinal inflammation. Lancet 1992; 339: 89–91.
Brown KA, Back SJ, Ruchelli ED, et al. Lamina propria and circulating interleukin-6 in newly diagnosed pediatric inflammatory bowel disease patients. Am J Gastroenterol 2002; 97: 2603.
Dieleman LA, Elson CO, Tennyson GS, Beagley KW. Kinetics of cytokine expression during healing of acute colitis in mice. Am J Physiol 1996; 271: G130.
Stevens C, Walz G, Singaram C, et al. Tumor necrosis factor-alpha, interleukin-1 beta, and interleukin-6 expression in inflammatory bowel disease. Dig Dis Sci 1992; 37: 818.
Carty E, De Brabander M, Feakins RM, Rampton DS. Measurement of in vivo rectal mucosal cytokine and eicosanoid production in ulcerative colitis using filter paper. Gut 2000; 46: 487.
Malefyt RD, Abrams J, Bennett B, Figdor CG, Devries JE. Interleukin-10(Il-10) inhibits cytokine synthesis by human monocytes- an autoregulatory role of Il-10 produced by monocytes. J Exp Med 1991; 174: 1209.
Ma D, Wolvers D, Stanisz AM, Bienenstock J. Interleukin-10 and nerve growth factor have reciprocal upregulatory effects on intestinal epithelial cells. Am J Physiol Regul Integr Comp Physiol 2003; 284: R1323.
Cassatella MA, Meda L, Gasperini S, Calzetti F, Bonora S. Interleukin 10 (IL-10) upregulates IL-1 receptor antagonist production from lipopolysaccharide-stimulated human polymorphonuclear leukocytes by delaying mRNA degradation. J Exp Med 1994; 179: 1695.
Autschbach F, Braunstein J, Helmke B, et al. In situ expression of interleukin-10 in non-inflamed human gut and in inflammatory bowel disease. Am J Pathol 1998; 153: 121.
Kuhn R, Lohler J, Rennick D, Rajewsky K, Muller W. Interleukin-10-deficient mice develop chronic enterocolitis. Cell 1993; 75: 263.
Kucharzik T, Stoll R, Lugering N, Domschke W. Circulating antiinflammatory cytokine IL-10 in patients with inflammatory bowel disease (IBD). Clin Exp Immunol 1995; 100: 452.
Mitsuyama K, Sata M, Tanikawa K. Significance of interleukin-6 in patients with inflammatory bowel disease. Gastroenterol Jpn 1991; 26: 20.
Gross V, Andus T, Caesar I, Roth M, Scholmerich J. Evidence for continuous stimulation of interleukin-6 production in Crohn’s disease. Gastroenterology 1992; 102: 514.
Lakhan SE, Kirchgessner A. Neuroinflammation in inflammatory bowel disease. J Neuroinflammation 2010; 7: 37.
Brierley SM, Linden DR. Neuroplasticity and dysfunction after gastrointestinal inflammation. Nat Rev Gastroenterol Hepatol 2014; 11: 611.
Mawe GM, Strong DS, Sharkey KA. Plasticity of enteric nerve functions in the inflamed and postinflamed gut. Neurogastroenterol Motil 2009; 21: 481.
Jacobson K, McHugh K, Collins SM. Experimental colitis alters myenteric nerve function at inflamed and non-inflamed sites in the rat. Gastroenterology 1995; 109: 718.
Jacobson K, McHugh K, Collins SM. The mechanism of altered neural function in a rat model of acute colitis. Gastroenterology 1997; 112: 156.
Hurst S, Collins SM. Interleukin-1 beta modulation of norepinephrine release from rat myenteric nerves. Am J Physiol 1993; 264: G30–35.
Gougeon PY, Lourenssen S, Han TY, Nair DG, Ropeleski MJ, Blennerhassett MG. The pro-inflammatory cytokines IL-1beta and TNFalpha are neurotrophic for enteric neurons. J Neurosci 2013; 33: 3339.
Martelli L, Ragazzi E, di Mario F, et al. A potential role for the vanilloid receptor TRPV1 in the therapeutic effect of curcumin in dinitrobenzene sulphonic acid-induced colitis in mice. Neurogastroenterol Motil 2007; 19: 668.
Massa F, Monory K. Endocannabinoids and the gastrointestinal tract. J Endocrinol Invest 2006; 29: 47.
Van Der Zanden EP, Boeckxstaens GE, de Jonge WJ. The vagus nerve as a modulator of intestinal inflammation. Neurogastroenterol Motil 2009; 21: 6–17.
van der Zanden EP, Snoek SA, Heinsbroek SE, et al. Vagus nerve activity augments intestinal macrophage phagocytosis via nicotinic acetylcholine receptor alpha4beta2. Gastroenterology 2009; 137: 1029.
Feher E, Fodor M, Burnstock G. Distribution of somatostatinimmunoreactive nerve fibres in Peyer’s patches. Gut 1992; 33: 1195.
Stead RH, Bienenstock J, Stanisz AM. Neuropeptide regulation of mucosal immunity. Immunol Rev 1987; 100: 333.
Ottaway CA, Lewis DL, Asa SL. Vasoactive intestinal peptidecontaining nerves in Peyer’s patches. Brain Behav Immun 1987; 1: 148.
Feher E, Altdorfer K, Bagameri G, Feher J. Neuroimmune interactions in experimental colitis. An immunoelectron microscopic study. Neuroimmunomodulation 2001; 9: 247.
Gross KJ, Pothoulakis C. Role of neuropeptides in inflammatory bowel disease. Inflamm Bowel Dis 2007; 13: 918.
Ottaway CA. Neuroimmunomodulation in the intestinal mucosa. Gastroenterol Clin North Am 1991; 20: 511.
Stead RH. Innervation of mucosal immune cells in the gastrointestinal tract. Reg Immunol 1992; 4: 91.
Stead RH, Dixon MF, Bramwell NH, Riddell RH, Bienenstock J. Mast cells are closely apposed to nerves in the human gastrointestinal mucosa. Gastroenterology 1989; 97: 575.
Newson B, Dahlstrom A, Enerback L, Ahlman H. Suggestive evidence for a direct innervation of mucosal mast cells. Neuroscience 1983; 10: 565.
Kulkarni-Narla A, Beitz AJ, Brown DR. Catecholaminergic, cholinergic and peptidergic innervation of gut-associated lymphoid tissue in porcine jejunum and ileum. Cell Tissue Res 1999; 298: 275.
Genton L, Kudsk KA. Interactions between the enteric nervous system and the immune system: role of neuropeptides and nutrition. Am J Surg 2003; 186: 253.
McCormack RJ, Hart RP, Ganea D. Expression of NK-1 receptor mRNA in murine T lymphocytes. Neuroimmunomodulation 1996; 3: 35.
Liu L, Shang F, Markus I, Burcher E. Roles of substance P receptors in human colon circular muscle: alterations in diverticular disease. J Pharmacol Exp Ther 2002; 302: 627.
Lai JP, Douglas SD, Ho WZ. Human lymphocytes express substance P and its receptor. J Neuroimmunol 1998; 86: 80.
Ho WZ, Stavropoulos G, Lai JP, et al. Substance P C-terminal octapeptide analogues augment tumor necrosis factor-alpha release by human blood monocytes and macrophages. J Neuroimmunol 1998; 82: 126.
Castagliuolo I, Keates AC, Qiu B, et al. Increased substance P responses in dorsal root ganglia and intestinal macrophages during Clostridium difficile toxin A enteritis in rats. Proc Natl Acad Sci U S A 1997; 94: 4788.
Forsgren S, Hockerfelt U, Norrgard O, Henriksson R, Franzen L. Pronounced substance P innervation in irradiation-induced enteropathy–a study on human colon. Regul Pept 2000; 88: 1.
Renzi D, Pellegrini B, Tonelli F, Surrenti C, Calabro A. Substance P (neurokinin-1) and neurokinin A (neurokinin-2) receptor gene and protein expression in the healthy and inflamed human intestine. Am J Path 2000; 157: 1511.
Riegler M, Castagliuolo I, So PT, et al. Effects of substance P on human colonic mucosa in vitro. Am J Physiol 1999; 276: G1473.
Shanahan F, Denburg JA, Fox J, Bienenstock J, Befus D. Mast cell heterogeneity: effects of neuroenteric peptides on histamine release. J Immunol 1985; 135: 1331.
Castagliuolo I, Wang CC, Valenick L, et al. Neurotensin is a proinflammatory neuropeptide in colonic inflammation. J Clin Invest 1999; 103: 843.
Laurenzi MA, Persson MA, Dalsgaard CJ, Haegerstrand A. The neuropeptide substance P stimulates production of interleukin 1 in human blood monocytes: activated cells are preferentially influenced by the neuropeptide. Scand J Immunol 1990; 31: 529.
McGillis JP, Mitsuhashi M, Payan DG. Immunomodulation by tachykinin neuropeptides. Ann N Y Acad Sci 1990; 594: 85.
Bueno L. Neuroimmune alterations of ENS functioning. Gut 2000; 47: iv63.
Jessell TM, Iversen LL, Cuello AC. Capsaicin-induced depletion of substance P from primary sensory neurones. Brain Res 1978; 152: 183.
Gamse R, Leeman SE, Holzer P, Lembeck F. Differential effects of capsaicin on the content of somatostatin, substance P, and neurotensin in the nervous system of the rat. Naunyn Schmiedebergs Arch Pharmacol 1981; 317: 140.
Metwali A, Blum AM, Ferraris L, Klein JS, Fiocchi C, Weinstock JV. Eosinophils within the healthy or inflamed human intestine produce substance P and vasoactive intestinal peptide. J Neuroimmunol 1994; 52: 69.
Delgado M. VIP: a very important peptide in T helper differentiation. Trends Immunol 2003; 24: 221.
Goode T, O’Connell J, Anton P, et al. Neurokinin-1 receptor expression in inflammatory bowel disease: molecular quantitation and localisation. Gut 2000; 47: 387.
Renzi D, Mantellini P, Calabro A, et al. Substance P and vasoactive intestinal polypeptide but not calcitonin gene-related peptide concentrations are reduced in patients with moderate and severe ulcerative colitis. Ital J Gastroenterol Hepatol 1998; 30: 62.
Miampamba M, Sharkey KA. Distribution of calcitonin generelated peptide, somatostatin, substance P and vasoactive intestinal polypeptide in experimental colitis in rats. Neurogastroenterol Motil 1998; 10: 315.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Mourad, F.H., Hamdi, T., Barada, K.A. et al. Experimental colitis in rats induces de novo synthesis of cytokines at distant intestinal sites: role of capsaicin-sensitive primary afferent fibers. Eur Cytokine Netw 27, 41–53 (2016). https://doi.org/10.1684/ecn.2016.0376
Published:
Issue Date:
DOI: https://doi.org/10.1684/ecn.2016.0376