Abstract
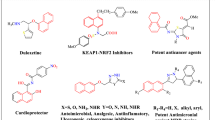
Aspartyl-type peptidases are promising chemotherapeutic targets in protozoan parasites. In the present work, we identified an aspartyl peptidase activity from the soluble extract of Leishmania amazonensis promastigotes, which cleaved the fluorogenic peptide 7-methoxycoumarin-4-acetyl-Gly-Lys-Pro-Ile-Leu-Phe-Phe-Arg-Leu-Lys(DNP)-D-Arg-amide (cathepsin D substrate) under acidic pH conditions at 37°C, showing a KM of 0.58 μM and Vmax of 129.87 fluorescence arbitrary units/s mg protein. The leishmanial aspartyl peptidase activity was blocked by pepstatin A (IC50 = 6.8 μM) and diazo-acetyl-norleucinemetilester (IC50 = 10.2 μM), two classical aspartyl peptidase inhibitors. Subsequently, the effects of 6 asymmetric peptidomimetics, containing L-tartaric acid core, were tested on both aspartyl peptidase and growth of L. amazonensis promastigotes. The peptidomimetics named 88, 154 and 158 promoted a reduction of 50% on the leishmanial aspartyl peptidase activity at concentrations ranging from 40 to 85 μM, whereas the peptidomimetic 157 was by far the most effective, presenting IC50 of 0.04 μM. Furthermore, the peptidomimetics 157 and 154 reduced the parasite proliferation in a dose-dependent manner, displaying IC50 values of 33.7 and 44.5 µM, respectively. Collectively, the peptidomimetic 157 was the most efficient compound able to arrest both aspartyl peptidase activity and leishmanial proliferation, which raises excellent perspectives regarding its use against this human pathogenic protozoan.
Similar content being viewed by others
References
Abrahim-Vieira B., da Costa E.C.B., de Azevedo P.H.R., Portela A.C., Dias L.R.S., Pinheiro S., et al. 2014. Novel isomannide-based peptide mimetics containing a tartaric acid backbone as serine protease inhibitors. Medicinal Chemistry Research, 23, 5305–5320. DOI 10.1007/s00044-014-1058-1
Alfonso Y., Monzote L. 2011. HIV protease inhibitors: effect on the opportunistic protozoan parasites. The Open Medicinal Chemistry Journal, 5, 40–50. DOI: 10.2174/1874104501105010040
Alves C.R., Corte-Real S., Bourguignon S.C., Chaves C.S., Saraiva E.M. 2005. Leishmania amazonensis: early proteinase activities during promastigote-amastigote differentiation in vitro, Experimental Parasitology, 109, 38–48. DOI:10.1016/j.exp-para.2004.10.005
Barros J.C., da Silva J.F.M., Calazans A., Tanuri A., Brindeiro R.M., Williamson J.S., et al. 2006. Synthesis of pseudopeptides derived from (R, R)-tartaric acid as potential inhibitors of HIV-protease. Letters in Organic Chemistry, 3, 882–886
Bastos I.M., Motta F.N., Grellier P., Santana J.M. 2013. Parasite prolyl oligopeptidases and the challenge of designing chemother-apeuticals for Chagas disease, leishmaniasis and African trypanosomiasis. Current Medicinal Chemistry, 20, 3103–3115. DOI: 10.2174/0929867311320250006
Bates P.A., Robertson C.D., Coombs G.H. 1994. Expression of cys-teine proteinases by metacyclic promastigotes of Leishmania mexicana. Journal of Eukaryotic Microbiology, 41, 199–203. DOI: 10.1111/j.1550-7408
Branquinha M.H., Sangenito L.S., Sodré C.L., Kneipp L.F., d’ Avila-Levy C.M., Santos A.L.S. 2017. The widespread anti-proto-zoal action of HIV aspartic peptidase inhibitors: focus on Plasmodium spp., Leishmania spp. and Trypanosoma cruzi. Current Topics in Medicinal Chemistry, 17, 1303–1317. DOI:10.2174/1568026616666161025161153
Caffrey C.R., Lima A.P., Steverding D. 2011. Cysteine peptidases of kinetoplastid parasites, Advances in Experimental Medicine and Biology, 712, 84–99. DOI:10.1007/978-1-4419-8414-2_6
Coates L., Erskine P.T., Mall S., Gill R., Wood S.P., Myles D.A., et al. 2006. X-Ray, neutron and NMR studies of the catalytic mechanism of aspartic proteinases. European Biophysics Journal, 35, 559–566. DOI: 10.1007/s00249-006-0065-7
Dali B., Keita M., Megnassan E., Frecer V., Miertus S. 2012. Insight into selectivity of peptidomimetic inhibitors with modified statine core for plasmepsin II of Plasmodium falciparum over human cathepsin D. Chemical Biology and Drug Design, 79, 411–430. DOI: 10.1111/j.1747-0285.2011.01276.x
Dash C., Kulkarni A., Dunn B., Rao M. 2003. Aspartic peptidase inhibitors: implications in drug development. Critical Reviews in Biochemistry and Molecular Biology, 38, 89–119. DOI: 10.1080/713609213
Davies D.R. 1990. The structure and function of the aspartic pro-teinases. Annual Review of Biophysics and Biophysical Chemistry, 19, 189–215. DOI: 10.1146/annurev.bb.19.060190.001201
Dominguez D.I., Hartmann D., De Strooper B. 2004. BACE1 and presenilin: two unusual aspartic proteases involved in Alzheimer’s disease. Neurodegenerative Disease, 1, 168–174. DOI:10.1159/000080982
Eder J., Hommel U., Cumin F., Martoglio B., Gerhartz B. 2007. Aspartic proteases in drug discovery. Current Pharmaceutical Design. 13, 271–285. DOI: 10.2174/138161207779313560
Gazdik M., Jarman K.E., O’Neill M.T., Hodder A.N., Lowes K.N., Jousset Sabroux H., et al. 2016. Exploration of the P3 region of PEXEL peptidomimetics leads to a potent inhibitor of the Plasmodium protease, plasmepsin V. Bioorganic and Medicinal Chemistry, 24, 1993–2010. DOI: 10.1016/j.bmc.2016.03.027
Gonzalez A.A., Prieto M.C. 2015. Renin and the (pro)renin receptor in the renal collecting duct: role in the pathogenesis of hypertension. Clinical and Experimental Pharmacology and Physiology, 42, 14–21. DOI: 10.1111/1440-1681.12319
Hamada Y., Kiso Y. 2016. New directions for protease inhibitors directed drug discovery. Biopolymers, 106, 563–579. DOI: 10.1002/bip.22780
Harris J.L., Backes B.J., Leonetti F., Mahrus S., Ellman J.A., Craik C.S. 2000. Rapid and general profiling of protease specificity by using combinatorial fluorogenic substrate libraries. Proceedings of the National Academy of Sciences of the United States of America, 97, 7754–7759. DOI: 10.1073/pnas. 140132697
Hernández-Chinea C., Maimone L., Campos Y., Mosca W., Romero P.J. 2017. Apparent isocitrate lyase activity in Leishmania amazonensis. Acta Parasitologica, 62, 701–707. DOI: 10.1515/ap-2017-0084
Horimoto Y., Dee D.R., Yada R.Y. 2009. Multifunctional aspartic peptidase prosegments. New Biotechnology, 25, 318–324. DOI: 10.1016/j.nbt.2009.03.010
Koehler J.W., Morales M.E., Shelby B.D., Brindley P.J. 2007. Aspartic protease activities of schistosomes cleave mammalian hemoglobins in a host-specific manner. Memórias do Instituto Oswaldo Cruz, 102, 83–85
Lima A.K.C., Elias C.G.R., Souza J.E.O., Santos A.L.S., Dutra P.M.L. 2009. Dissimilar peptidase production by avirulent and virulent promastigotes of Leishmania braziliensis: inference on the parasite proliferation and interaction with macrophages. Parasitology, 136, 1179–1191. DOI: 10.1017/S0031182009990540
Lowry O.H., Rosebrough N.J., Farr A.L., Randal R.J. 1951. Protein measurement with the folin phenol reagent. Journal of Biological Chemistry, 193, 264–275
Majer F., Pavlícková L., Majer P., Hradilek M., Dolejsí E., Hrusková-Heidingsfeldová O., et al. 2006. Structure-based specificity mapping of secreted aspartic proteases of Candida parapsilosis, Candida albicans, and Candida tropicalis using peptidomimetic inhibitors and homology modeling. Biological Chemistry, 387, 1247–1254. DOI: 10.1515/BC.2006.154
Nielsen P.E. 2004. Pseudo-peptides in drug discovery. John Wiley and Sons, ISBN: 978-3-527, 30633–30636
Olivier M., Atayde V.D., Isnard A., Hassani K., Shio M.T. 2012. Leishmania virulence factors: focus on the metalloprotease GP63. Microbes and Infection, 14, 1377–1389. DOI: 10. 1016/j.micinf.2012.05.014
Peçanha E.P., Figueiredo L.J., Brindeiro R.M., Tanuri A., Calazans A.R., Antunes O.A. 2003. Synthesis and anti-HIV activity of new C2 symmetric derivatives designed as HIV-1 protease inhibitors. Farmaco, 58, 149–157. doi.org/10.1016/S0014-827X(02)00016-2
Perteguer M.J., Gómez-Puertas P., Cañavate C., Dagger F., Gárate T., Valdivieso E. 2012. Ddi1-like protein from Leishmania major is an active aspartyl proteinase. Cell Stress Chaperones, 18, 171–181. DOI: 10.1007/s12192-012-0368-9
Pranjol M.Z., Gutowski N., Hannemann M., Whatmore J. 2015. The potential role of the proteases cathepsin D and cathepsin L in the progression and metastasis of epithelial ovarian cancer. Biomolecules, 5, 3260–3279. DOI:10.3390/biom50 43260
Qidwai T. 2015. Hemoglobin Degrading proteases of Plasmodium falciparum as antimalarial drug targets. Current Drug Targets, 16, 1133–1141. DOI: 10.2174/1389450116666150304104123
Qiu X., Liu Z.P. 2011. Recent developments of peptidomimetic HIV-1 protease inhibitors. Current Medicinal Chemistry, 18, 4513–4537. DOI: 10.2174/092986711797287566
Resende G.O., João F.C., da Silva F.C., Cotrim B.A., Antunes O.A.C., Aguiar L.C.S. 2007. Synthesis of asymmetric peptide mimetic compounds containing tartaric acid core. Potential inhibitors of HIV-1 protease. Letters in Organic Chemistry, 4, 146–150. DOI: 10.2174/157017807780737200
Sádlová J., Volf P., Victoir K., Dujardin J., Votypka J. 2006. Virulent and attenuated lines of Leishmania major: DNA karyotypes and differences in metalloproteinase GP63. Folia Parasitologica, 53, 81–90. DOI: 10.14411/fp.2006.011
Sangenito L.S., Gonçalves D.S., Seabra S.H., d’Avila-Levy C.M., Santos A.L.S., Branquinha M.H. 2016. HIV aspartic peptidase inhibitors are effective drugs against the trypomastigote form of the human pathogen Trypanosoma cruzi. International Journal of Antimicrobial Agents, 48, 440–444. DOI: 10.1016/j.ijantimicag.2016.06.024
Santos L.O., Marinho F.A., Altoé E.F., Vitório B.S., Alves C.R., Britto C., et al. 2009. HIV aspartyl peptidase inhibitors interfere with cellular proliferation, ultrastructure and macrophage infection of Leishmania amazonensis. PLoS ONE, 4, e4918. DOI: 10.1371/journal.pone.0004918
Santos L.O., Garcia-Gomes A.S., Catanho M., Sodre C.L., Santos A.L.S., Branquinha M.H., et al. 2013a. Aspartic peptidases of human pathogenic trypanosomatids: perspectives and trends for chemotherapy. Current Medicinal Chemistry, 20, 3116–3333. DOI: 10.2174/0929867311320250007
Santos L.O., Vitório B.S., Branquinha M.H., Pedrozo C., Santos A.L.S., d’Avila-Levy C.M. 2013b. Nelfinavir, an HIV aspartyl peptidase inhibitor, is effective in inhibiting the multiplication and aspartyl peptidase activity of several Leishmania species, including strains obtained from HIV-positive patients. Journal of Antmicrobial Chemotherapy, 68, 348–353. DOI: 10.1093/jac/dks410
Savoia D. 2015. Recent updates and perspectives on leishmaniasis. The Journal of Infection in Developing Countries, 9, 588–596. DOI: 10.3855/jidc.6833
Silva N.C., Nery J.M., Dias A.L. 2014. Aspartic proteinases of Candida spp.: role in pathogenicity and antifungal resistance. Mycoses, 57, 1–11. DOI: 10.1111/myc.12095
Sojka D., Hartmann D., Bartošová-Sojková P., Dvořák J. 2016. Parasite cathepsin D-like peptidases and their relevance as therapeutic targets. Trends in Parasitology, 32, 708–723. DOI: 10.1016/j.pt.2016.05.015
Trudel N., Garg R., Messier N., Sundar S., Ouellette S.M., Tremblay M.J. 2008. Intracellular survival of Leishmania species that cause visceral leishmaniasis is significantly reduced by HIV-1 protease inhibitors. The Journal of Infectious Diseases, 198, 1292–1299. DOI:10.1086/592280
Valdivieso E., Dagger F., Rascón A. 2007. Leishmania mexicana: identification and characterization of an aspartic proteinase activity. Experimental Parasitology, 116, 77–82E. DOI: 10.1016/j.exppara.2006.10.006
Valdivieso A., Rangel J., Moreno J.M., Saugar C., Cañavate J., Alvar F., et al. 2010. Effects of HIV aspartyl proteinase inhibitors on Leishmania sp., Experimental Parasitology, 126, 557–563. DOI: 10.1016/j.exppara.2010.06.002
Wensing A.M., Van Maarseveen N.M., Nijhuis M. 2010. Fifteen years of HIV protease inhibitors: raising the barrier to resistance. Antiviral Research, 85, 59–74. DOI: 10.1016/j.antiviral.2009.10.003
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Santos, A.L.S., Matteoli, F.P., Sangenito, L.S. et al. Asymmetric peptidomimetics containing L-tartaric acid core inhibit the aspartyl peptidase activity and growth of Leishmania amazonensis promastigotes. Acta Parasit. 63, 114–124 (2018). https://doi.org/10.1515/ap-2018-0013
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1515/ap-2018-0013