Abstract
Background
Few risk models have been provided to predict long-term prognosis after esophagectomy. This study investigated the reliability of a risk calculator as well as classification and regression trees analysis for predicting long-term prognosis after esophagectomy for esophageal cancer.
Methods
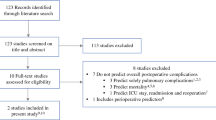
The study enrolled 438 patients who underwent esophagectomy at Keio University Hospital, Tokyo, Japan, between July 2000 and June 2016. Patients who underwent R0 or R1 resection or esophagectomy with combined resection of other organs were included. The authors investigated the usefulness of a risk model for 30-day mortality and operative mortality described in their previous report for predicting long-term prognosis after esophagectomy.
Results
The 438 patients (377 men and 61 women) in this study had a 5-year overall survival (OS) rate of 62.8% and a disease-free survival rate of 54.3%. The OS was higher for the patients with 30-day mortality risk model values lower than 0.675% than for those with values higher than 0.675% (p < 0.001). The cutoff values for prediction were shown to be significant risk factors in the multivariate analysis. The risk calculator was validated by comparing the cutoff values with Harrell’s C-index values of clinical stage. For overall risk, the C-index of operative mortality was 0.697, and the C-index of cStage was 0.671.
Conclusions
The risk calculator was useful for predicting recurrence and death after esophagectomy. Furthermore, because the C-index of the risk model for operative mortality was higher than for clinical tumor-node-metastasis stage, this risk-scoring system may be more useful clinically.

Similar content being viewed by others
References
Takeuchi H, Miyata H, Gotoh M, et al. A risk model for esophagectomy using data of 5354 patients included in a Japanese nationwide web-based database. Ann Surg. 2014;260:259–66.
Kidane B, Sulman J, Xu W, et al. Baseline measure of health-related quality of life (functional assessment of cancer therapy-esophagus) is associated with overall survival in patients with esophageal cancer. J Thorac Cardiovasc Surg. 2016;151:1571–80.
Hamai Y, Hihara J, Emi M, et al. Ability of fluorine-18 fluorodeoxyglucose positron emission tomography to predict outcomes of neoadjuvant chemoradiotherapy followed by surgical treatment for esophageal squamous cell carcinoma. Ann Thorac Surg. 2016;102:1132–39.
Takeuchi H, Saikawa Y, Oyama T, et al. Factors influencing the long-term survival in patients with esophageal cancer who underwent esophagectomy after chemoradiotherapy. World J Surg. 2010;34:277–84.
Booka E, Takeuchi H, Nishi T, et al. The impact of postoperative complications on survivals after esophagectomy for esophageal cancer. Med Baltim. 2015;94:e1369.
Matsuda S, Takeuchi H, Kawakubo H, et al. Cumulative prognostic scores based on plasma fibrinogen and serum albumin levels in esophageal cancer patients treated with transthoracic esophagectomy: comparison with the Glasgow prognostic score. Ann Surg Oncol. 2015;22:302–10.
Sobin L, Gospodarowicz M WC, eds. TNM Classification of Malignant Tumours. 7th ed Wiley-Liss, New York, 2009.
Matsuda S, Takeuchi H, Kawakubo H, et al. Clinical outcome of transthoracic esophagectomy with thoracic duct resection: number of dissected lymph node and distribution of lymph node metastasis around the thoracic duct. Med Baltim. 2016;95:e3839.
Kaburagi T, Takeuchi H, Kawakubo H, et al. Clinical utility of a novel hybrid position combining the left lateral decubitus and prone positions during thoracoscopic esophagectomy. World J Surg. 2014;38:410–18.
Takesue T, Takeuchi H, Ogura M, et al. A prospective randomized trial of enteral nutrition after thoracoscopic esophagectomy for esophageal cancer. Ann Surg Oncol. 2015;22:802–09.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
Breiman L, Friedman JH, Stone CJ, et al. Classification and regression trees. 1984;1:368.
Garzotto M, Beer TM, Hudson RG, et al. Improved detection of prostate cancer using classification and regression tree analysis. J Clin Oncol 2005;23:4322–29.
Loh W-Y. Classification and regression trees. Wiley Interdiscip. Rev. 2011;1:14–23.
Okamura A, Takeuchi H, Matsuda S, et al. Factors affecting cytokine change after esophagectomy for esophageal cancer. Ann Surg Oncol. 2015;22:3130–35.
Ogura M, Takeuchi H, Kawakubo H, et al. Clinical significance of CXCL-8/CXCR-2 network in esophageal squamous cell carcinoma. Surgery. 2013;154:512–20.
Shakhar G, Ben-Eliyahu S. Potential prophylactic measures against postoperative immunosuppression: could they reduce recurrence rates in oncological patients? Ann Surg Oncol. 2003;10:972–92.
Hogan BV, Peter MB, Shenoy HG, et al. Surgery-induced immunosuppression. Surgeon. 2011;9:38–43.
Goldfarb Y, Sorski L, Benish M, et al. Improving postoperative immune status and resistance to cancer metastasis. Ann Surg. 2011;253:798–810.
Abramovitch R, Marikovsky M, Meir G, et al. Stimulation of tumour growth by wound-derived growth factors. Br J Cancer. 1999;79:1392–98.
Ferri LE, Law S, Wong KH, et al. The influence of technical complications on postoperative outcome and survival after esophagectomy. Ann Surg Oncol. 2006;13:557–64.
Feng JF, Huang Y, Lu WS CQ. Preoperative platelet count in esophageal squamous cell carcinoma: is it a prognostic factor? Langenbecks Arch Surg. 2013;398:1115.
Shimada H, Oohira G, Okazumi S, et al. Thrombocytosis associated with poor prognosis in patients with esophageal carcinoma. J Am Coll Surg. 2004;198:737–41.
Tsuruo T, Fujita N. Platelet aggregation in the formation of tumor metastasis. Proc Japan Acad Ser B, Phys Biol Scienes. 2008;84:189–98.
Reeh M, Metze J, Uzunoglu FG, et al. The PER (Preoperative Esophagectomy Risk) Score: a simple risk score to predict short-term and long-term outcome in patients with surgically treated esophageal cancer. Medicine Baltimore. 2016;95:1–8.
Finks JF, Osborne NH, Birkmeyer JD. Trends in hospital volume and operative mortality for high-risk surgery. N Engl J Med. 2011;364:2128–37.
Acknowledgment
The authors thank Kumiko Motooka, who belongs to the staff at the Department of Surgery in Keio University School of Medicine, for her help in the preparation of this report.
Disclosure
There are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Takeuchi, M., Takeuchi, H., Kawakubo, H. et al. Perioperative Risk Calculator Predicts Long-Term Oncologic Outcome for Patients with Esophageal Carcinoma. Ann Surg Oncol 25, 837–843 (2018). https://doi.org/10.1245/s10434-017-6311-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-017-6311-7