Abstract
Background
The prognostic impact of pancreatic ductal adenocarcinoma (PDAC) invasion to the splenic vessel is controversial.
Objective
The aim of this study was to assess the clinical value of pathological and radiological splenic vessel invasion in PDACs of the body and tail.
Methods
Medical records of patients with resectable PDAC of the body and tail who underwent distal pancreatectomy between 2003 and 2016 at the Kobe University Hospital were retrospectively analyzed.
Results
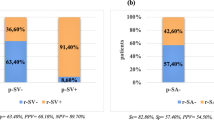
Overall, 68 patients (29 female and 39 male patients) were enrolled. Pathologically determined splenic vein invasion (p-SV) and splenic artery invasion (p-SA) were identified in 21 (30.9%) and 5 (7.4%) patients, respectively. The p-SV (but not p-SA) was an independent prognostic factor in multivariate analysis (p = 0.009). On analysis of recurrence patterns, patients with PDAC positive for p-SV were at a higher risk for liver metastasis (p = 0.022); however, the associations were not significant for other recurrence patterns. Liver metastasis occurred earlier in patients who were positive for p-SV (p = 0.015). Preoperative computed tomography effectively diagnosed pathological vessel invasion (SV: sensitivity, 95.2%, specificity, 72.3%; SA: sensitivity, 100%, specificity, 84.1%). Radiological SV invasion remained significant in multivariate analysis regarding postoperative survival (p = 0.007), and was also associated with early liver metastases (p = 0.008).
Conclusions
Pathological/radiological SV invasion were independent adverse prognostic factors associated with early liver metastasis in patients with PDAC of the body/tail. Assessment of these findings may be useful in determining optimal therapeutic options in these patients.



Similar content being viewed by others
References
Warshaw AL, Fernandez-del Castillo C. Pancreatic carcinoma. N Engl J Med. 1992;326:455–65.
Sener SF, Fremgen A, Menck HR, Winchester DP. Pancreatic cancer: a report of treatment and survival trends for 100,313 patients diagnosed from 1985 to 1995, using the National Cancer Database. J Am Coll Surg. 1999;189:1–7.
National Comprehensive Cancer Network (2017). NCCN clinical practice guidelines in oncology (NCCN Guidelines). Pancreatic adenocarcinoma. Version 1. http://www.nccn.org/professionals/physician_gls/f_guidelines.asp. Accessed 10 Jan 2017.
Murakami Y, Satoi S, Sho M, et al. National comprehensive cancer network resectability status for pancreatic carcinoma predicts overall survival. World J Surg. 2015;39:2306–14.
Wang F, Gill AJ, Neale M et al. Adverse tumor biology associated with mesenterico-portal vein resection influences survival in patients with pancreatic ductal adenocarcinoma. Ann Surg Oncol. 2014;21:1937–47.
Yamada S, Fujii T, Sugimoto H, Nomoto S, Takeda S, Kodera Y, Nakao A. Aggressive surgery for borderline resectable pancreatic cancer: evaluation of National Comprehensive Cancer Network guidelines. Pancreas. 2013;42:1004–10.
Mierke F, Hempel S, Distler M, Aust DE, Saeger HD, Weitz J, et al. Impact of portal vein involvement from pancreatic cancer on metastatic pattern after surgical resection. Ann Surg Oncol. 2016;23:730–6.
Cloyd JM, Katz MH, Prakash L et al. Preoperative therapy and pancreatoduodenectomy for pancreatic ductal adenocarcinoma: a 25-year single-institution experience. J Gastrointest Surg. 2017;21:164–74.
Barugola G, Partelli S, Crippa S, Capelli P, D’Onofrio M, Pederzoli P, et al. Outcomes after resection of locally advanced or borderline resectable pancreatic cancer after neoadjuvant therapy. Am J Surg. 2012;203:132–9.
Ferrone CR, Marchegiani G, Hong TS, et al. Radiological and surgical implications of neoadjuvant treatment with FOLFIRINOX for locally advanced and borderline resectable pancreatic cancer. Ann Surg. 2015;261:12–17.
Shimada K, Sakamoto Y, Sano T, Kosuge T. Prognostic factors after distal pancreatectomy with extended lymphadenectomy for invasive pancreatic adenocarcinoma of the body and tail. Surgery. 2006;139:288–95.
Kanda M, Fujii T, Sahin TT et al. Invasion of the splenic artery is a crucial prognostic factor in carcinoma of the body and tail of the pancreas. Ann Surg. 2010;251:483–7.
Partelli S, Crippa S, Barugola G et al. Splenic artery invasion in pancreatic adenocarcinoma of the body and tail: a novel prognostic parameter for patient selection. Ann Surg Oncol. 2011;18:3608–14.
Fukami Y, Kaneoka Y, Maeda A, Takayama Y, Onoe S. Prognostic impact of splenic artery invasion for pancreatic cancer of the body and tail. Int J Surg. 2016;35:64–8.
Sobin LH, Gospodarowicz MK, Wittekind C. TNM classification of malignant tumors. 7th ed. New York: Wiley; 2009.
Bissolati M, Sandri MT, Burtulo G, Zorzino L, Balzano G, Braga M. Portal vein-circulating tumor cells predict liver metastases in patients with resectable pancreatic cancer. Tumour Biol. 2015;36:991–6.
Disclosures
Takuya Mizumoto, Hirochika Toyama, Sadaki Asari, Sachio Terai, Hideyo Mukubo, Hironori Yamashita, Sachiyo Shirakawa, Yoshihide Nanno, Yuki Ueda, Keitaro Sofue, Motofumi Tanaka, Masahiro Kido, Tetsuo Ajiki, and Takumi Fukumoto have no conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mizumoto, T., Toyama, H., Asari, S. et al. Pathological and Radiological Splenic Vein Involvement are Predictors of Poor Prognosis and Early Liver Metastasis After Surgery in Patients with Pancreatic Adenocarcinoma of the Body and Tail. Ann Surg Oncol 25, 638–646 (2018). https://doi.org/10.1245/s10434-017-6274-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-017-6274-8