Abstract
Background
Whether hepatic arterial infusion (HAI) of oxaliplatin influences the rates of complete pathologic response (CPR) and severe oxaliplatin-related lesions (SOxL) in patients with colorectal liver metastases (CRLM) is unknown. This study aimed to compare the incidence of CPR and SOxL between systemic (intravenous, IV) and HAI administration.
Methods
All patients with initially unresectable CRLM who had undergone hepatic resection in two expert centers between 2004 and 2010 after at least 6 cycles of oxaliplatin-based chemotherapy administered either via HAI (n = 18) or IV (n = 50) were included. The presence of CPR and SOxL were evaluated by two pathologists. A 1:2 case match using a propensity score was used.
Results
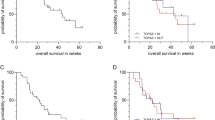
A CPR was observed significantly more often after HAI (33 vs. 10 %, P = 0.03). However, SOxL had occurred more frequently in patients in the HAI group versus the IV group, 66 and 20 %, respectively (P < 0.001). On a well-balanced cohort, HAI was associated with higher chance of CPR (odds ratio 9.33, 95 % confidence interval 1.59–54.7) but also higher risk of SOxL (odds ratio 13.7, 95 % confidence interval 3.08–61.3). A CPR markedly enhanced overall survival (OS) and disease-free survival (median OS of 114 vs. 42 months, P = 0.02; median disease-free survival of 51 vs. 12 months, P = 0.002). Patients with SOxL did not experience different outcome (median OS of 42 vs. 50 months, respectively; P = 0.92)
Conclusions
HAI of oxaliplatin increases the likelihood of a CPR at the cost of a higher incidence of SOxL in patients with initially unresectable CRLM.

Similar content being viewed by others
References
Bismuth H, Adam R, Levi F, et al. Resection of nonresectable liver metastases from colorectal cancer after neoadjuvant chemotherapy. Ann Surg. 1996;224:509–20.
Adam R, Wicherts DA, de Haas RJ, et al. Patients with initially unresectable colorectal liver metastases: is there a possibility of cure? J Clin Oncol. 2009;27:1829–35.
Mocellin S, Pasquali S, Nitti D. Fluoropyrimidine-HAI (hepatic arterial infusion) versus systemic chemotherapy (SCT) for unresectable liver metastases from colorectal cancer. Cochrane Database Syst Rev. 2009;3:CD007823.
Kemeny NE, Melendez FD, Capanu M, et al. Conversion to resectability using hepatic artery infusion plus systemic chemotherapy for the treatment of unresectable liver metastases from colorectal carcinoma. J Clin Oncol. 2009;27:3465–71.
Ducreux M, Ychou M, Laplanche A, et al. Hepatic arterial oxaliplatin infusion plus intravenous chemotherapy in colorectal cancer with inoperable hepatic metastases: a trial of the gastrointestinal group of the Federation Nationale des Centres de Lutte Contre le Cancer. J Clin Oncol. 2005;23:4881–7.
Goere D, Deshaies I, de Baere T, et al. Prolonged survival of initially unresectable hepatic colorectal cancer patients treated with hepatic arterial infusion of oxaliplatin followed by radical surgery of metastases. Ann Surg. 2010;251:686–91.
Adam R, Wicherts DA, de Haas RJ, et al. Complete pathologic response after preoperative chemotherapy for colorectal liver metastases: myth or reality? J Clin Oncol. 2008;26:1635–41.
Blazer DG 3rd, Kishi Y, Maru DM, et al. Pathologic response to preoperative chemotherapy: a new outcome end point after resection of hepatic colorectal metastases. J Clin Oncol. 2008;26:5344–51.
Guthoff I, Lotspeich E, Fester C, et al. Hepatic artery infusion using oxaliplatin in combination with 5-fluorouracil, folinic acid and mitomycin C: oxaliplatin pharmacokinetics and feasibility. Anticancer Res. 2003;23(6D):5203–8.
Rubbia-Brandt L, Lauwers GY, Wang H, et al. Sinusoidal obstruction syndrome and nodular regenerative hyperplasia are frequent oxaliplatin-associated liver lesions and partially prevented by bevacizumab in patients with hepatic colorectal metastasis. Histopathology. 2010;56:430–9.
Rubbia-Brandt L, Audard V, Sartoretti P, et al. Severe hepatic sinusoidal obstruction associated with oxaliplatin-based chemotherapy in patients with metastatic colorectal cancer. Ann Oncol. 2004;15:460–6.
Rubbia-Brandt L, Tauzin S, Brezault C, et al. Gene expression profiling provides insights into pathways of oxaliplatin-related sinusoidal obstruction syndrome in humans. Mol Cancer Ther. 2011;10:687–96.
Rubbia-Brandt L, Giostra E, Brezault C, et al. Importance of histological tumor response assessment in predicting the outcome in patients with colorectal liver metastases treated with neo-adjuvant chemotherapy followed by liver surgery. Ann Oncol. 2007;18:299–304.
Wicherts DA, de Haas RJ, Sebagh M, et al. Regenerative nodular hyperplasia of the liver related to chemotherapy: impact on outcome of liver surgery for colorectal metastases. Ann Surg Oncol. 2011;18:659–69.
Vreuls CP, Van Den Broek MA, Winstanley A, et al. Hepatic sinusoidal obstruction syndrome (SOS) reduces the effect of oxaliplatin in colorectal liver metastases. Histopathology. 2012;61:314–8.
Tamandl D, Klinger M, Eipeldauer S, et al. Sinusoidal obstruction syndrome impairs long-term outcome of colorectal liver metastases treated with resection after neoadjuvant chemotherapy. Ann Surg Oncol. 2011;18:421–30.
Adam R, Delvart V, Pascal G, et al. Rescue surgery for unresectable colorectal liver metastases downstaged by chemotherapy: a model to predict long-term survival. Ann Surg. 2004;240:644–57.
Adam R, Laurent A, Azoulay D, Castaing D, Bismuth H. Two-stage hepatectomy: a planned strategy to treat irresectable liver tumors. Ann Surg. 2000;232:777–85.
Levi F, Boige V, Hebbar M, et al. Final results of first European phase II trial of intravenous cetuximab and hepatic artery infusion of irinotecan, 5-fluorouracil, and oxaliplatin in patients with unresectable liver metastases from wt KRAS colorectal cancer after systemic treatment failure (OPTILIV, NCT00852228) [abstract 466]. J Clin Oncol. 2013;31(suppl 4).
Deschamps F, Rao P, Teriitehau C, et al. Percutaneous femoral implantation of an arterial port catheter for intraarterial chemotherapy: feasibility and predictive factors of long-term functionality. J Vasc Interv Radiol. 2010;21:1681–8.
Honore C, Goere D, Dumont F, Elias D. Catheter placement for intra-arterial hepatic chemotherapy. J Visc Surg. 2012;149:389–94.
Malka DEP, Caramella C, Boucher E, et al. Hepatic arterial infusion (HAI) of oxaliplatin plus intravenous (iv) fluorouracil (FU), leucovorin (LV), and cetuximab for first-line treatment of unresectable colorectal liver metastases (CRLM) (CHOICE): a multicenter phase II study. J Clin Oncol. 2010;28(15 suppl):3558.
Colucci G, Gebbia V, Paoletti G, et al. Phase III randomized trial of FOLFIRI versus FOLFOX4 in the treatment of advanced colorectal cancer: a multicenter study of the Gruppo Oncologico Dell’Italia Meridionale. J Clin Oncol. 2005;23:4866–75.
Tournigand C, Andre T, Achille E, et al. FOLFIRI followed by FOLFOX6 or the reverse sequence in advanced colorectal cancer: a randomized GERCOR study. J Clin Oncol. 2004;22:229–37.
Imamura H, Sano K, Sugawara Y, Kokudo N, Makuuchi M. Assessment of hepatic reserve for indication of hepatic resection: decision tree incorporating indocyanine green test. J Hepatobiliary Pancreat Surg. 2005;12:16–22.
Soubrane O, Brouquet A, Zalinski S, et al. Predicting high grade lesions of sinusoidal obstruction syndrome related to oxaliplatin-based chemotherapy for colorectal liver metastases: correlation with post-hepatectomy outcome. Ann Surg. 2010;251:454–60.
Elias D, Lasser P, Rougier P, Ducreux M, Bognel C, Roche A. Frequency, technical aspects, results, and indications of major hepatectomy after prolonged intra-arterial hepatic chemotherapy for initially unresectable hepatic tumors. J Am Coll Surg. 1995;180:213–9.
Bismuth H. [Anatomy of the liver and hepatectomy techniques]. Ann Chir. 1998;52:61–3.
Balzan S, Belghiti J, Farges O, et al. The “50–50 criteria” on postoperative day 5: an accurate predictor of liver failure and death after hepatectomy. Ann Surg. 2005;242:824–8.
Kemeny NE. The re-birth of hepatic arterial infusion for colorectal liver metastases. J Gastrointest Oncol. 2013;4:118–20.
Vigano L, Capussotti L, De Rosa G, De Saussure WO, Mentha G, Rubbia-Brandt L. Liver resection for colorectal metastases after chemotherapy: impact of chemotherapy-related liver injuries, pathological tumor response, and micrometastases on long-term survival. Ann Surg. 2013;258:731–40.
Aloia T, Sebagh M, Plasse M, et al. Liver histology and surgical outcomes after preoperative chemotherapy with fluorouracil plus oxaliplatin in colorectal cancer liver metastases. J Clin Oncol. 2006;24:4983–90.
Nakano H, Oussoultzoglou E, Rosso E, et al. Sinusoidal injury increases morbidity after major hepatectomy in patients with colorectal liver metastases receiving preoperative chemotherapy. Ann Surg. 2008;247:118–24.
Narita M, Oussoultzoglou E, Chenard MP, et al. Liver injury due to chemotherapy-induced sinusoidal obstruction syndrome is associated with sinusoidal capillarization. Ann Surg Oncol. 2012;19:2230–7.
Makowiec F, Mohrle S, Neeff H, et al. Chemotherapy, liver injury, and postoperative complications in colorectal liver metastases. J Gastrointest Surg. 2011;15:153–64.
Ryan P, Nanji S, Pollett A, et al. Chemotherapy-induced liver injury in metastatic colorectal cancer: semiquantitative histologic analysis of 334 resected liver specimens shows that vascular injury but not steatohepatitis is associated with preoperative chemotherapy. Am J Surg Pathol. 2010;34:784–91.
Acknowledgment
The authors would like to thank Dr. David Malka, who provided the clinical data from the CHOICE study, and Lorna Saint Ange for editing.
Disclosure
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Allard, M.A., Sebagh, M., Baillie, G. et al. Comparison of Complete Pathologic Response and Hepatic Injuries Between Hepatic Arterial Infusion and Systemic Administration of Oxaliplatin in Patients with Colorectal Liver Metastases. Ann Surg Oncol 22, 1925–1932 (2015). https://doi.org/10.1245/s10434-014-4272-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-014-4272-7