Abstract
Background
High-grade appendiceal adenocarcinoma is a rare malignancy with propensity for peritoneal metastases (PM). The impact of neoadjuvant chemotherapy on operative cytoreduction (CRS) and intraperitoneal chemotherapy (HIPEC) and patient survival was reviewed.
Methods
A total of 45 patients with PM from high-grade appendiceal adenocarcinoma were identified from a prospective database. All patients had laparotomy with intent to undergo CRS and HIPEC. Operative parameters, complications, and survival outcomes were analyzed.
Results
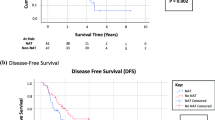
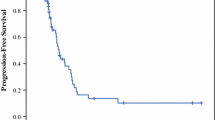
Of the 45 patients (male: 27, female: 18; median age: 55 years), 26 received neoadjuvant chemotherapy ± bevacizumab. Of the 26, 15 (58 %) had a response based on improvement in imaging, biomarkers, or both and 9 (34 %) had stable disease. The median peritoneal cancer index (PCI) was 27. Also, 30 (67 %) had a completeness of cytoreduction score (CCR) of ≤1 and 37 (82 %) received HIPEC. There were no differences in PCI, CCR score, operative blood loss, or major organ resection between those who received or did not receive neoadjuvant chemotherapy. Operative time was significantly shorter in those who did not receive neoadjuvant chemotherapy. Major complications and length of hospital stay were similar between the groups. The median actuarial overall survival calculated from the date of initial therapeutic intervention was not different in those treated with or without neoadjuvant therapy.
Conclusions
Neoadjuvant chemotherapy has marked clinical activity in patients with PM from high-grade appendiceal adenocarcinoma and does not adversely affect operative outcomes. These data support conducting a prospective clinical trial to define the role of neoadjuvant chemotherapy in this clinical setting.

Similar content being viewed by others
References
McCusker ME, Cote TR, Clegg LX, Sobin LH. Primary malignant neoplasms of the appendix: a population-based study from the surveillance, epidemiology and end-results program, 1973–1998. Cancer. 2002;94:3307–12.
Ronnett BM, Zahn CM, Kurman RJ, Kass ME, Sugarbaker PH, Shmookler BM. Disseminated peritoneal adenomucinosis and peritoneal mucinous carcinomatosis. A clinicopathologic analysis of 109 cases with emphasis on distinguishing pathologic features, site of origin, prognosis, and relationship to “pseudomyxoma peritonei”. Am J Surg Pathol. 1995;19:1390–408.
Ronnett BM, Yan H, Kurman RJ, Shmookler BM, Wu L, Sugarbaker PH. Patients with pseudomyxoma peritonei associated with disseminated peritoneal adenomucinosis have a significantly more favorable prognosis than patients with peritoneal mucinous carcinomatosis. Cancer. 2001;92:85–91.
Yan TD, Links M, Xu ZY, Kam PC, Glenn D, Morris DL. Cytoreductive surgery and perioperative intraperitoneal chemotherapy for pseudomyxoma peritonei from appendiceal mucinous neoplasms. Br J Surg. 2006;93:1270–6.
El Halabi H, Gushchin V, Francis J, Athas N, Macdonald R, Nieroda C, et al. The role of cytoreductive surgery and heated intraperitoneal chemotherapy (CRS/HIPEC) in patients with high-grade appendiceal carcinoma and extensive peritoneal carcinomatosis. Ann Surg Oncol. 2012;19:110–4.
Baratti D, Kusamura S, Nonaka D, Langer M, Andreola S, Favaro M, et al. Pseudomyxoma peritonei: clinical pathological and biological prognostic factors in patients treated with cytoreductive surgery and hyperthermic intraperitoneal chemotherapy (HIPEC). Ann Surg Oncol. 2008;15:526–34.
Loungnarath R, Causeret S, Bossard N, Faheez M, Sayag-Beaujard AC, Brigand C, et al. Cytoreductive surgery with intraperitoneal chemohyperthermia for the treatment of pseudomyxoma peritonei: a prospective study. Dis Colon Rectum. 2005;48:1372–9.
Stewart JH, Shen P, Russell GB, Bradley RF, Hundley JC, Loggie BL, et al. Appendiceal neoplasms with peritoneal dissemination: outcomes after cytoreductive surgery and intraperitoneal hyperthermic chemotherapy. Ann Surg Oncol. 2006;13:624–34.
Sugarbaker PH, Chang D. Results of treatment of 385 patients with peritoneal surface spread of appendiceal malignancy. Ann Surg Oncol. 1999;6:727–31.
Moran B, Baratti D, Yan TD, Kusamura S, Deraco M. Consensus statement on the loco-regional treatment of appendiceal mucinous neoplasms with peritoneal dissemination (pseudomyxoma peritonei). J Surg Oncol. 2008;98:277–82.
Sugarbaker PH, Bijelic L, Chang D, Yoo D. Neoadjuvant FOLFOX chemotherapy in 34 consecutive patients with mucinous peritoneal carcinomatosis of appendiceal origin. J Surg Oncol. 2010;102:576–81.
Jacquet P, Sugarbaker PH. Clinical research methodologies in diagnosis and staging of patients with peritoneal carcinomatosis. Cancer Treat Res. 1996;82:359–74.
Chua TC, Pelz JO, Kerscher A, Morris DL, Esquivel J. Critical analysis of 33 patients with peritoneal carcinomatosis secondary to colorectal and appendiceal signet ring cell carcinoma. Ann Surg Oncol. 2009;16:2765–70.
Glehen O, Osinsky D, Cotte E, Kwiatkowski F, Freyer G, Isaac S, et al. Intraperitoneal chemohyperthermia using a closed abdominal procedure and cytoreductive surgery for the treatment of peritoneal carcinomatosis: morbidity and mortality analysis of 216 consecutive procedures. Ann Surg Oncol. 2003;10:863–9.
Gusani NJ, Cho SW, Colovos C, Seo S, Franko J, Richard SD, et al. Aggressive surgical management of peritoneal carcinomatosis with low mortality in a high-volume tertiary cancer center. Ann Surg Oncol. 2008;15:754–63.
Elias D, Blot F, El Otmany A, Antoun S, Lasser P, Boige V, et al. Curative treatment of peritoneal carcinomatosis arising from colorectal cancer by complete resection and intraperitoneal chemotherapy. Cancer. 2001;92:71–6.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Turner, K.M., Hanna, N.N., Zhu, Y. et al. Assessment of Neoadjuvant Chemotherapy on Operative Parameters and Outcome in Patients with Peritoneal Dissemination from High-Grade Appendiceal Cancer. Ann Surg Oncol 20, 1068–1073 (2013). https://doi.org/10.1245/s10434-012-2789-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-012-2789-1