Abstract
Background
Advances in the treatment of Ewing sarcoma family of tumors (ESFT) are the result of improvements in systemic and local therapies. Clinical data of extraosseous ESFT are scarce.
Methods
A retrospective analysis of all patients with extraosseous ESFT treated at St. Jude Children’s Research Hospital (SJCRH) from June 1982 to August 2009.
Results
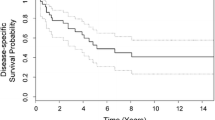
Forty-six patients with extraosseous ESFT were identified. The mean age at diagnosis was 13.8 years. The majority of patients were male and white. The most common site of primary tumor was the trunk. Twelve patients had subcutaneous tumors. The median tumor size was 8 cm. Six patients (13 %) had metastatic disease at diagnosis. A total of 59 % of patients were alive at the time of analysis, with a median follow-up from diagnosis of 15.3 years. Fifteen-year estimates of survival and event-free survival (EFS) for all patients were 53.3 ± 9.4 and 50 ± 9.1 %, respectively. Fifteen-year estimates of survival and EFS with localized disease were 61.4 ± 9.8 and 57.6 ± 9.7 %, respectively. Stage and subcutaneous ESFT were significant predictors of outcome. There was no significant difference in patient’s demographics and tumor characteristics between patients with skeletal ESFT and extraosseous Ewing sarcoma. The outcome for patients with localized extraosseous Ewing sarcoma was similar to that reported for all localized ESFT patients treated at SJCRH.
Conclusions
The outcome for localized patients treated with extraosseous ESFT was similar to that reported for all ESFT patients treated on protocols at SJCRH. Patients with subcutaneous ESFT had a favorable prognosis when compared to their counterparts.




Similar content being viewed by others
References
Grier HE. The Ewing family of tumors. Ewing’s sarcoma and primitive neuroectodermal tumors. Pediatr Clin North Am. 1997;44:991–1004.
Cavazzana AO, Miser JS, Jefferson J, Triche TJ. Experimental evidence for a neural origin of Ewing’s sarcoma of bone. Am J Pathol. 1987;127:507–18.
Cotterill SJ, Ahrens S, Paulussen M, Jurgens HF, Voute PA, Gadner H, et al. Prognostic factors in Ewing’s tumor of bone: analysis of 975 patients from the European Intergroup Cooperative Ewing’s Sarcoma Study Group. J Clin Oncol. 2000;18:3108–14.
Krasin MJ, Davidoff AM, Rodriguez-Galindo C, Billups CA, Fuller CE, Neel MD, et al. Definitive surgery and multiagent systemic therapy for patients with localized Ewing sarcoma family of tumors: local outcome and prognostic factors. Cancer. 2005;104:367–73.
Marina NM, Pappo AS, Parham DM, Cain AM, Rao BN, Poquette CA, et al. Chemotherapy dose-intensification for pediatric patients with Ewing’s family of tumors and desmoplastic small round-cell tumors: a feasibility study at St. Jude Children’s Research Hospital. J Clin Oncol. 1999;17:180–90.
Rodriguez-Galindo C, Spunt SL, Pappo AS. Treatment of Ewing sarcoma family of tumors: current status and outlook for the future. Med Pediatr Oncol. 2003;40:276–87.
Rodriguez-Galindo C, Liu T, Krasin MJ, Wu J, Billups CA, Daw NC, et al. Analysis of prognostic factors in ewing sarcoma family of tumors: review of St. Jude Children’s Research Hospital studies. Cancer. 2007;110:375–84.
Raney RB, Asmar L, Newton WA Jr, Bagwell C, Breneman JC, Crist W, et al. Ewing’s sarcoma of soft tissues in childhood: a report from the intergroup rhabdomyosarcoma study, 1972 to 1991. J Clin Oncol. 1997;15:574–82.
Applebaum MA, Worch J, Matthay KK, Goldsby R, Neuhaus J, West DC, et al. Clinical features and outcomes in patients with extraskeletal Ewing sarcoma. Cancer. 2011;117:3027–32.
Ayadi L, Chaari C, Kallel R, Ayadi K, Khabir A, Jlidi R, et al. [Ewing sarcoma osseous and extraosseous: a clinicopathologic study of 29 cases]. Tunis Med. 2010;88:301–5.
Chow E, Merchant TE, Pappo A, Jenkins JJ, Shah AB, Kun LE. Cutaneous and subcutaneous Ewing’s sarcoma: an indolent disease. Int J Radiat Oncol Biol Phys. 2000;46:433–8.
dos Santos REJ, Harhangi BS, Kros JM, Vincent AJ, Dirven CM. A primary extraosseous Ewing sarcoma in the cerebellopontine angle of a child: review of relevant literature and case report. Neurosurgery. 2010;67:E1852–6.
El Weshi A, Allam A, Ajarim D, Al Dayel F, Pant R, Bazarbashi S, et al. Extraskeletal Ewing’s sarcoma family of tumours in adults: analysis of 57 patients from a single institution. Clin Oncol (R Coll Radiol). 2010;22:374–81.
Moodley M, Jordaan A. Ewing’s sarcoma of the vulva—a case report. Int J Gynecol Cancer. 2005;15:1177–8.
van den Berg H, Heinen RC, van der Pal HJ, Merks JH. Extra-osseous Ewing sarcoma. Pediatr Hematol Oncol. 2009;26:175–85.
Peto R, Pike MC, Armitage P, Breslow NE, Cox DR, Howard SV, et al. Design and analysis of randomized clinical trials requiring prolonged observation of each patient. II. analysis and examples. Br J Cancer. 1977;35:1–39.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shannon Orr, W., Denbo, J.W., Billups, C.A. et al. Analysis of Prognostic Factors in Extraosseous Ewing Sarcoma Family of Tumors: Review of St. Jude Children’s Research Hospital Experience. Ann Surg Oncol 19, 3816–3822 (2012). https://doi.org/10.1245/s10434-012-2458-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-012-2458-4