Abstract
Background
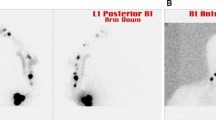
Interval sentinel nodes (SNs) are lymph nodes receiving direct lymphatic drainage from a primary site and lying between the tumor and a recognized node field. It is not clear what further nodal surgery should be performed when interval nodes are found to contain micrometastatic disease. In this study, the incidence, location, and treatment of interval SNs in melanoma patients were analyzed to develop recommendations regarding the treatment of patients with interval SNs.
Methods
A retrospective review was undertaken of all patients with primary cutaneous melanoma who underwent lymphoscintigraphy at a single institution between 1992 and 2007. Data concerning the primary melanoma, location of SNs, treatment and survival were analyzed.
Results
Of 4895 patients who had a lymphoscintigram during the study period, 442 (9.0%) had an interval SN identified on lymphoscintigraphy. Interval SNs occurred significantly more often in patients with melanomas on the posterior trunk than in those with melanomas at other sites (P < 0.001). A total of 197 patients (44.6%) with an identified interval SN underwent excision biopsy of the node. Of the 16 patients found to have metastatic melanoma in their interval SN, four also had negative SNs in a recognized lymph node field, and no other positive nodes were found on completion lymphadenectomy.
Conclusions
Interval SNs are present in approximately 1 in 10 melanoma patients but are about half as likely to contain metastases as SNs in recognized node fields. If a positive interval SN is found, completion lymphadenectomy of the recognized lymph node field is only recommended if a SN in this field is also positive.



Similar content being viewed by others
References
Uren RF, Howman-Giles R, Thompson JF, et al. Lymphoscintigraphy to identify sentinel nodes in patients with melanoma. Melanoma Res. 1994;4:395–9.
Uren RF, Howman-Giles R, Thompson JF, et al. Interval nodes: the forgotten sentinel nodes in patients with melanoma. Arch Surg. 2000;135:1168–72.
McMasters KM, Chao C, Wong SL, et al. Sunbelt Melanoma Trial Group. Interval sentinel lymph nodes in melanoma. Arch Surg. 2002;137:543–7.
Roozendaal GK, de Vries JD, van Poll D, et al. Sentinel nodes outside lymph node basins in patients with melanoma. Br J Surg. 2001;88:305–8.
Scolyer RA, Murali R, McCarthy SW, Thompson JF. Pathologic examination of sentinel lymph nodes from melanoma patients. Semin Diagn Pathol. 2008;25:100–11.
Morton DL, Thompson JF, Cochran AJ, et al. Sentinel-node biopsy or nodal observation in melanoma. N Engl J Med. 2006;355:1307–17.
Thompson JF, Morton DL, Kroon, B. Textbook of melanoma. 4th ed. London: Martin Dunitz; 2004.
van Akkooi AC, Nowecki ZI, Voit C, et al. Sentinel node tumor burden according to the Rotterdam criteria is the most important prognostic factor for survival in melanoma patients: a multicenter study in 388 patients with positive sentinel nodes. Ann Surg. 2008;248:949–55.
Carling T, Pan D, Ariyan S, et al. Diagnosis and treatment of interval sentinel lymph nodes in patients with cutaneous melanoma. Plast Reconstr Surg. 2007;119:907–13.
Sumner WE III, Ross MI, Mansfield PF, et al. Implications of lymphatic drainage to unusual sentinel lymph node sites in patients with primary cutaneous melanoma. Cancer. 2002;95:354–60.
Alazraki NP, Eshima D, Eshima LA, et al. Lymphoscintigraphy, the sentinel node concept, and the intraoperative gamma probe in melanoma, breast cancer, and other potential cancers. Semin Nucl Med. 1997;27:55–67.
Nathanson SD, Nelson L, Karvelis KC. Rates of flow of technetium 99m-labeled human serum albumin from peripheral injection sites to sentinel lymph nodes. Ann Surg Oncol. 1996;3:329–35.
Tonakie A, Sondak V, Yahanda A, Wahl RL. Reproducibility of lymphoscintigraphic drainage patterns in sequential 99mTc human serum albumin and 99mTc sulfur colloid studies: implications for sentinel node identification in melanoma. Surgery. 1999;126:955–62.
Hunt JA, Thompson JF, Uren RF, et al. Epitrochlear lymph nodes as a site of melanoma metastasis. Ann Surg Oncol. 1998;5:248–52.
Thompson JF, Hunt JA, Culjak G, et al. Popliteal lymph node metastasis from primary cutaneous melanoma. Eur J Surg Oncol. 2000;26:172–6.
Balch CM, Buzaid AC, Soong SJ, et al. Final version of the American Joint Committee on Cancer staging system for cutaneous melanoma. J Clin Oncol. 2001;19:3635–48.
Gershenwald JE, Thompson W, Mansfield PF, et al. Multi-institutional melanoma lymphatic mapping experience: the prognostic value of sentinel lymph node status in 612 stage I or II melanoma patients. J Clin Oncol. 1999;17:976–83.
Vidal-Sicart S, Pons F, Fuertes S, et al. Is the identification of in-transit sentinel lymph nodes in malignant melanoma patients really necessary? Eur J Nucl Med Mol Imaging. 2004;31:945–9.
Matter M, Nicod Lalonde M, Allaoua M, et al. The role of interval nodes in sentinel lymph node mapping and dissection for melanoma patients. J Nucl Med. 2007;48:1607–13.
Ortín-Pérez J, Vidal-Sicart S, Doménech B, et al. In-transit sentinel lymph nodes in malignant melanoma. What is their importance? Rev Esp Med Nucl. 2008;27:424–9.
Chakera AH, Hansen LB, Lock-Andersen J, et al. In-transit sentinel nodes must be found: implication from a 10-year follow-up study in melanoma. Melanoma Res. 2008;18:359–64.
Acknowledgment
N.V. was a MIA and ErasmusMC doctoral student supported by an ErasmusMC student fund and Stichting A. A. van Beek-Fonds. We thank Kaye Oakley, Maria Mancone, Sandie Grierson, and Elizabeth Paton for their assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Verwer, N., Scolyer, R.A., Uren, R.F. et al. Treatment and Prognostic Significance of Positive Interval Sentinel Nodes in Patients with Primary Cutaneous Melanoma. Ann Surg Oncol 18, 3292–3299 (2011). https://doi.org/10.1245/s10434-011-1988-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-011-1988-5