Abstract
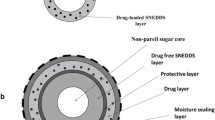
This proof-of-concept study explores the feasibility of using a drug-loaded hydrophilic polymeric layer sandwiched between two hydrophobic layers for improving film drug load while achieving sustained release of poorly water-soluble drug. Such films having total thickness in range ~ 146–250 μm were prepared by slurry-based casting using hydrophilic hydroxypropyl methylcellulose (HPMC) as matrix layer containing fenofibrate (FNB) as the model drug, encased between two very thin rate-limiting layers of 10 μm each of hydrophobic poly-ɛ-caprolactone (PCL). Film precursor slurry consisted of HPMC with plasticizer and water along with micronized FNB powders, which were dry-coated with hydrophilic silica. Characterization techniques demonstrated the presence of homogeneously dispersed crystalline FNB in films. The films are very thin and hence two-dimensional; hence, average drug load per unit area in range ~ 5 to ~ 9 mg/cm2 could be achieved by altering the thickness of the drug matrix layer. Drug amount and drug content uniformity were measured through assay of ten circular samples ~ 0.712 cm2 in area punched out using a circular-shaped punch tool. Drug release rate was investigated using USP IV flow-through cell and surface dissolution imaging system. Thinner films followed Fickian diffusion, and thicker films followed non-Fickian anomalous diffusion. Overall, the application of middle layer thickness could be used as a tool to manipulate drug load without the need for altering its formulation or precursor preparation by changing its thickness, hence achieving relatively high drug loading yet having sustained release of drug.







Similar content being viewed by others
References
Dixit RP, Puthli SP. Oral strip technology: overview and future potential. J Control Release. 2009;139(2):94–107.
Krull SM, Susarla R, Afolabi A, Li M, Ying Y, Iqbal Z, et al. Polymer strip films as a robust, surfactant-free platform for delivery of BCS class II drug nanoparticles. Int J Pharm. 2015;489(1–2):45–−57.
Borges AF, Silva C, Coelho JF, Simoes S. Oral films: current status and future perspectives: I—galenical development and quality attributes. J Control Release. 2015;206:1–19.
Sievens-Figueroa L, Bhakay A, Jerez-Rozo JI, Pandya N, Romañach RJ, Michniak-Kohn B, et al. Preparation and characterization of hydroxypropyl methyl cellulose films containing stable BCS class II drug nanoparticles for pharmaceutical applications. Int J Pharm. 2012;423(2):496–−508.
Beck C, Sievens-Figueroa L, Gärtner K, Jerez-Rozo JI, Romañach RJ, Bilgili E, et al. Effects of stabilizers on particle redispersion and dissolution from polymer strip films containing liquid antisolvent precipitated griseofulvin particles. Powder Technol. 2013;236:37–51.
Bhakay A, Vizzotti E, Li M, Davé R, Bilgili E. Incorporation of fenofibrate nanoparticles prepared by melt emulsification into polymeric films. J Pharm Innov. 2016;11(1):53–63.
Zhang L, Li Y, Abed M, Davé RN. Incorporation of surface-modified dry micronized poorly water-soluble drug powders into polymer strip films. Int J Pharm. 2018;535(1–2):462–72.
Krull SM, Patel HV, Li M, Bilgili E, Davé RN. Critical material attributes (CMAs) of strip films loaded with poorly water-soluble drug nanoparticles: I. Impact of plasticizer on film properties and dissolution. Eur J Pharm Sci. 2016;92:146–55.
Krull SM, Ammirata J, Bawa S, Li M, Bilgili E, Davé RN. Critical material attributes of strip films loaded with poorly water-soluble drug nanoparticles: II. Impact of polymer molecular weight. J Pharm Sci. 2017;106(2):619–28.
Kim S, Kim J-H, Jeon O, Kwon IC, Park K. Engineered polymers for advanced drug delivery. Eur J Pharm Biopharm. 2009;71(3):420–30.
Maderuelo C, Zarzuelo A, Lanao JM. Critical factors in the release of drugs from sustained release hydrophilic matrices. J Control Release. 2011;154(1):2–19.
Khaled SA, Burley JC, Alexander MR, Roberts CJ. Desktop 3D printing of controlled release pharmaceutical bilayer tablets. Int J Pharm. 2014;461(1):105–11.
Fukuda M, Peppas NA, McGinity JW. Properties of sustained release hot-melt extruded tablets containing chitosan and xanthan gum. Int J Pharm. 2006;310(1):90–100.
Ford JL, Rubinstein MH, McCaul F, Hogan JE, Edgar PJ. Importance of drug type, tablet shape and added diluents on drug release kinetics from hydroxypropylmethylcellulose matrix tablets. Int J Pharm. 1987;40(3):223–34.
Siepmann J, Kranz H, Peppas NA, Bodmeier R. Calculation of the required size and shape of hydroxypropyl methylcellulose matrices to achieve desired drug release profiles. Int J Pharm. 2000;201(2):151–64.
Kim H, Fassihi R. Application of binary polymer system in drug release rate modulation. 2. Influence of formulation variables and hydrodynamic conditions on release kinetics. J Pharm Sci. 1997;86(3):323–8.
Zhang L, Alfano JE, Race D, Dave R. Zero-order release of poorly water-soluble drug from polymeric films made via aqueous slurry casting. Eur J Pharm Sci. 2018;117:245–54.
Krull SM, Ma Z, Li M, Dave RN, Bilgili E. Preparation and characterization of fast dissolving pullulan films containing BCS class II drug nanoparticles for bioavailability enhancement. Drug Dev Ind Pharm. 2016;42(7):1073–85.
Woertz C, Kleinebudde P. Development of orodispersible polymer films containing poorly water soluble active pharmaceutical ingredients with focus on different drug loadings and storage stability. Int J Pharm. 2015;493(1):134–45.
Colombo P. Swelling-controlled release in hydrogel matrices for oral route. Adv Drug Deliv Rev. 1993;11(1):37–57.
Siepmann J, Peppas NA. Modeling of drug release from delivery systems based on hydroxypropyl methylcellulose (HPMC). Adv Drug Deliv Rev. 2001;48(2):139–57.
Tiwari SB, Rajabi-Siahboomi AR. Extended-release oral drug delivery technologies: monolithic matrix systems. In: Jain KK, editor. Drug delivery systems. Methods in molecular biology™. Totowa: Humana Press; 2008.
Ishikawa T, Watanabe Y, Takayama K, Endo H, Matsumoto M. Effect of hydroxypropylmethylcellulose (HPMC) on the release profiles and bioavailability of a poorly water-soluble drug from tablets prepared using macrogol and HPMC. Int J Pharm. 2000;202(1–2):173–8.
Perugini P, Genta I, Conti B, Modena T, Pavanetto F. Periodontal delivery of ipriflavone: new chitosan/PLGA film delivery system for a lipophilic drug. Int J Pharm. 2003;252(1–2):1–9.
Preis M, Woertz C, Schneider K, Kukawka J, Broscheit J, Roewer N, et al. Design and evaluation of bilayered buccal film preparations for local administration of lidocaine hydrochloride. Eur J Pharm Biopharm. 2014;86(3):552–61.
Visser CJ, Weggemans OAF, Boosman RJ, Loos KU, Frijlink HW, Woerdenbag HJ. Increased drug load and polymer compatibility of bilayered orodispersible films. Eur J Pharm Sci. 2017;107:183–90.
Sun S, Li J, Li X, Lan B, Zhou S, Meng Y, et al. Episcleral drug film for better-targeted ocular drug delivery and controlled release using multilayered poly-ε-caprolactone (PCL). Acta Biomater. 2016;37:143–54.
Remuñán-López C, Portero A, Vila-Jato JL, MaJ A. Design and evaluation of chitosan/ethylcellulose mucoadhesive bilayered devices for buccal drug delivery. J Control Release. 1998;55(2):143–52.
Han X, Ghoroi C, To D, Chen Y, Dave R. Simultaneous micronization and surface modification for improvement of flow and dissolution of drug particles. Int J Pharm. 2011;415(1–2):185–95.
Wei X, Gong C, Gou M, Fu S, Guo Q, Shi S, et al. Biodegradable poly(ɛ-caprolactone)–poly(ethylene glycol) copolymers as drug delivery system. Int J Pharm. 2009;381(1):1–18.
Tziomalos K, Athyros VG. Fenofibrate: a novel formulation (Triglide™) in the treatment of lipid disorders: a review. Int J Nanomedicine. 2006;1(2):129–47.
Susarla R, Sievens-Figueroa L, Bhakay A, Shen Y, Jerez-Rozo JI, Engen W, et al. Fast drying of biocompatible polymer films loaded with poorly water-soluble drug nano-particles via low temperature forced convection. Int J Pharm. 2013;455(1–2):93–103.
Higuchi T. Mechanism of sustained-action medication. Theoretical analysis of rate of release of solid drugs dispersed in solid matrices. J Pharm Sci. 1963;52(12):1145–9.
Hixson AW, Crowell JH. Dependence of reaction velocity upon surface and agitation. Ind Eng Chem. 1931;23(10):1160–8.
Korsmeyer RW, Gurny R, Doelker E, Buri P, Peppas NA. Mechanisms of solute release from porous hydrophilic polymers. Int J Pharm. 1983;15(1):25–35.
Costa P, Sousa Lobo JM. Modeling and comparison of dissolution profiles. Eur J Pharm Sci. 2001;13(2):123–33.
Gordon S, Naelapaa K, Rantanen J, Selen A, Mullertz A, Ostergaard J. Real-time dissolution behavior of furosemide in biorelevant media as determined by UV imaging. Pharm Dev Technol. 2013;18(6):1407–16.
Ostergaard J, Meng-Lund E, Larsen SW, Larsen C, Petersson K, Lenke J, et al. Real-time UV imaging of nicotine release from transdermal patch. Pharm Res. 2010;27(12):2614–23.
Yang J, Sliva A, Banerjee A, Dave RN, Pfeffer R. Dry particle coating for improving the flowability of cohesive powders. Powder Technol. 2005;158(1–3):21–33.
Vogt M, Kunath K, Dressman JB. Dissolution enhancement of fenofibrate by micronization, cogrinding and spray-drying: comparison with commercial preparations. Eur J Pharm Biopharm. 2008;68(2):283–8.
Elzubair A, Elias CN, Suarez JCM, Lopes HP, Vieira MVB. The physical characterization of a thermoplastic polymer for endodontic obturation. J Dent. 2006;34(10):784–9.
Cha KH, Cho KJ, Kim MS, Kim JS, Park HJ, Park J, et al. Enhancement of the dissolution rate and bioavailability of fenofibrate by a melt-adsorption method using supercritical carbon dioxide. Int J Nanomedicine. 2012;7:5565–75.
Kothapally S, Bada PK, Harish G. Formulation and evaluation of fenofibrate tablets prepared by employing bioavailability enhancement technique. Ind J Res Pharm Biotechnol. 2013;1(5):602.
Cristescu R, Doraiswamy A, Socol G, Grigorescu S, Axente E, Mihaiescu D, et al. Polycaprolactone biopolymer thin films obtained by matrix assisted pulsed laser evaporation. Appl Surf Sci. 2007;253(15):6476–9.
Takala PN, Salmieri S, Boumail A, Khan RA, Vu KD, Chauve G, et al. Antimicrobial effect and physicochemical properties of bioactive trilayer polycaprolactone/methylcellulose-based films on the growth of foodborne pathogens and total microbiota in fresh broccoli. J Food Eng. 2013;116(3):648–55.
Dong Y, Zhang Z, Feng S-S. d-α-Tocopheryl polyethylene glycol 1000 succinate (TPGS) modified poly(l-lactide) (PLLA) films for localized delivery of paclitaxel. Int J Pharm. 2008;350(1–2):166–71.
Karuppuswamy P, Reddy Venugopal J, Navaneethan B, Luwang Laiva A, Ramakrishna S. Polycaprolactone nanofibers for the controlled release of tetracycline hydrochloride. Mater Lett. 2015;141:180–6.
Wu C, McGinity JW. Influence of relative humidity on the mechanical and drug release properties of theophylline pellets coated with an acrylic polymer containing methylparaben as a non-traditional plasticizer. Eur J Pharm Biopharm. 2000;50(2):277–84.
Lei L, Liu X, Guo S, Tang M, Cheng L, Tian L. 5-Fluorouracil-loaded multilayered films for drug controlled releasing stent application: drug release, microstructure, and ex vivo permeation behaviors. J Control Release. 2010;146(1):45–53.
Dave R, Zhang L, Guluzar G, Li M. Compositions and methods for preparing polymeric films loaded with uniformly distributed drug particles. US Patent # 62/567,517. 2017.
Acknowledgments
The authors appreciate useful discussions and comments from Prof. Ecevit Bilgili and Dr. Scott Krull on earlier versions of this paper and also thanks to Mr. Benchafia Mostafa for his assistance with ATR-FTIR spectroscopy analysis.
Funding
The study was supported by financial grant from the National Science Foundation (NSF) through grant nos. EEC-0540855 and IIP-1312125.
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
ESM 1
(DOCX 4173 kb)
Rights and permissions
About this article
Cite this article
Kevadiya, B.D., Zhang, L. & Davé, R.N. Sustained Release of Poorly Water-Soluble Drug from Hydrophilic Polymeric Film Sandwiched Between Hydrophobic Layers. AAPS PharmSciTech 19, 2572–2584 (2018). https://doi.org/10.1208/s12249-018-1089-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1208/s12249-018-1089-x