Abstract
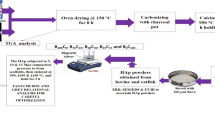
The aim of the present study was to prepare and evaluate a sustained-release mangiferin scaffold for improving alveolar bone defect repair in diabetes. Mangiferin-loaded poly(D,L-lactide-co-glycolide) (PLGA) scaffolds were prepared using a freeze-drying technique with ice particles as the porogen material. The produced scaffolds were examined using a scanning electron microscope (SEM). Drug content and drug release were detected using a spectrophotometer. Degradation behaviors were monitored as a measure of weight loss and examined using SEM. Then, the scaffolds were incubated with rat bone marrow stromal cells under the diabetic condition in vitro, and cell viability was assessed using an 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay. Afterward, the scaffolds were implanted into alveolar bone defects of diabetic rats, and bone repair was examined using hematoxylin and eosin staining. The fabricated scaffolds showed porous structures, with average pore size range from 111.35 to 169.45 μm. A higher PLGA concentration led to decreased average pore size. A lower PLGA concentration or a higher mangiferin concentration resulted in increased drug content. The prepared scaffolds released mangiferin in a sustained manner with relatively low initial burst during 10 weeks. Their degradation ratios gradually increased as degradation proceeded. The mangiferin-loaded scaffolds attenuated cell viability decrease under the diabetic condition in vitro. Moreover, they increased histological scorings of bone regeneration and improved delayed alveolar bone defect healing in diabetic rats. These results suggest that the produced mangiferin-loaded scaffolds may provide a potential approach in the treatment of impaired alveolar bone healing in diabetes.








Similar content being viewed by others
References
Cramer C, Freisinger E, Jones R, Slakey D, Dupin C, Newsome E, et al. Persistent high glucose concentrations alter the regenerative potential of mesenchymal stem cells. Stem Cells Dev. 2010;19:1875–84.
Jiao H, Xiao E, Graves D. Diabetes and its effect on bone and fracture healing. Curr Osteoporos Rep. 2015;13:327–35.
He H, Liu R, Desta T, Leone C, Gerstenfeld L, Graves D. Diabetes causes decreased osteoclastogenesis, reduced bone formation, and enhanced apoptosis of osteoblastic cells in bacteria stimulated bone loss. Endocrinology. 2004;145:447–52.
Wang Q, Li H, Xiao Y, Li S, Li B, Zhao X, et al. Locally controlled delivery of TNFα antibody from a novel glucose-sensitive scaffold enhances alveolar bone healing in diabetic conditions. J Control Release. 2015;206:232–42.
Rivera D, Hernández I, Merino N, Luque Y, Álvarez A, Martín Y, et al. Mangifera indica L. extract (Vimang) and mangiferin reduce the airway inflammation and Th2 cytokines in murine model of allergic asthma. J Pharm Pharmacol. 2011;63:1336–45.
Márquez L, García-Bueno B, Madrigal J, Leza J. Mangiferin decreases inflammation and oxidative damage in rat brain after stress. Eur J Nutr. 2012;51:729–39.
Pal P, Sinha K, Sil P. Mangiferin attenuates diabetic nephropathy by inhibiting oxidative stress mediated signaling cascade, TNFα related and mitochondrial dependent apoptotic pathways in streptozotocin-induced diabetic rats. PLoS One. 2014;9:e107220.
Kokotkiewicz A, Luczkiewicz M, Pawlowska J, Luczkiewicz P, Sowinski P, Witkowski J, et al. Isolation of xanthone and benzophenone derivatives from Cyclopia genistoides (L.) Vent. (honeybush) and their pro-apoptotic activity on synoviocytes from patients with rheumatoid arthritis. Fitoterapia. 2013;90:199–208.
Luo Y, Fu C, Wang Z, Zhang Z, Wang H, Liu Y. Mangiferin attenuates contusive spinal cord injury in rats through the regulation of oxidative stress, inflammation and the Bcl-2 and Bax pathway. Mol Med Rep. 2015;12:7132–8.
Huh J, Koh P, Seo B, Park Y, Baek Y, Lee J, et al. Mangiferin reduces the inhibition of chondrogenic differentiation by IL-1β in mesenchymal stem cells from subchondral bone and targets multiple aspects of the Smad and SOX9 pathways. Int J Mol Sci. 2014;15:16025–42.
Carvalho R, Pellizzon C, Justulin LJ, Felisbino S, Vilegas W, Bruni F, et al. Effect of mangiferin on the development of periodontal disease: involvement of lipoxin A4, anti-chemotaxic action in leukocyte rolling. Chem Biol Interact. 2009;179:344–50.
Jagetia G, Baliga M. Radioprotection by mangiferin in DBAxC57BL mice: a preliminary study. Phytomedicine. 2005;12:209–15.
Hou S, Wang F, Li Y, Li Y, Wang M, Sun D, et al. Pharmacokinetic study of mangiferin in human plasma after oral administration. Food Chem. 2012;132:289–94.
Xiao W, Hou J, Ma J, Yu B, Ren J, Jin W, et al. Mangiferin loaded magnetic PCEC microspheres: preparation, characterization and antitumor activity studies in vitro. Arch Pharm Res. 2014.
Chang N, Lam C, Lin C, Chen W, Li C, Lin Y, et al. Transplantation of autologous endothelial progenitor cells in porous PLGA scaffolds create a microenvironment for the regeneration of hyaline cartilage in rabbits. Osteoarthr Cartil. 2013;21:1613–22.
Yoon S, Park K, Kim M, Rhee J, Khang G, Lee H. Repair of diaphyseal bone defects with calcitriol-loaded PLGA scaffolds and marrow stromal cells. Tissue Eng. 2007;13:1125–33.
Lee H, Seo S, Chang H, Bang J, Joung Y, Son T, et al. Fabrication and characteristics of anti-inflammatory magnesium hydroxide incorporated PLGA scaffolds formed with various porogen materials. Macromol Res. 2014;22:210–8.
Jeon O, Song S, Kang S, Putnam A, Kim B. Enhancement of ectopic bone formation by bone morphogenetic protein-2 released from a heparin-conjugated poly(L-lactic-co-glycolic acid) scaffold. Biomaterials. 2007;28:2763–71.
Song J, Xie J, Li C, Lu J, Meng Q, Yang Z, et al. Near infrared spectroscopic (NIRS) analysis of drug-loading rate and particle size of risperidone microspheres by improved chemometric model. Int J Pharm. 2014;472:296–303.
Hedberg E, Shih C, Lemoine J, Timmer M, Liebschner M, Jansen J, et al. In vitro degradation of porous poly(propylene fumarate)/poly(DL-lactic-co-glycolic acid) composite scaffolds. Biomaterials. 2005;26:3215–25.
Souza J, Carvalho J, Trevisan M, Paula R, Ricardo N, Feitosa J. Chitosan-coated pectin beads: characterization and in vitro release of mangiferin. food hydrocoll. 2009;23:2278–86.
Kretlow J, Klouda L, Mikos A. Injectable matrices and scaffolds for drug delivery in tissue engineering. Adv Drug Deliv Rev. 2007;59:263–73.
Sharma A, Bharti S, Kumar R, Krishnamurthy B, Bhatia J, Kumari S, et al. Syzygium cumini ameliorates insulin resistance and β-cell dysfunction via modulation of PPAR, dyslipidemia, oxidative stress, and TNF-α in type 2 diabetic rats. J Pharmacol Sci. 2012;119:205–13.
Ravi N, Gupta G, Milbrandt T, Puleo D. Porous PLGA scaffolds for controlled release of naked and polyethyleneimine-complexed DNA. Biomed Mater. 2012;7:055007.
Liu M, Dai L, Shi H, Xiong S, Zhou C. In vitro evaluation of alginate/halloysite nanotube composite scaffolds for tissue engineering. Mater Sci Eng C Mater Biol Appl. 2015;49:700–12.
Hu Y, Ma S, Yang Z, Zhou W, Du Z, Huang J, et al. Facile fabrication of poly(L-lactic acid) microsphere-incorporated calcium alginate/hydroxyapatite porous scaffolds based on Pickering emulsion templates. Colloids Surf B: Biointerfaces. 2016;140:382–91.
Kim K, Dean D, Wallace J, Breithaupt R, Mikos A, Fisher J. The influence of stereolithographic scaffold architecture and composition on osteogenic signal expression with rat bone marrow stromal cells. Biomaterials. 2011;32:3750–63.
Watanabe K, Petro B, Shlimon A, Unterman T. Effect of periodontitis on insulin resistance and the onset of type 2 diabetes mellitus in Zucker diabetic fatty rats. J Periodontol. 2008;79:1208–16.
Li H, Wang Q, Xiao Y, Bao C, Li W. 25-Hydroxyvitamin D(3)-loaded PLA microspheres: in vitro characterization and application in diabetic periodontitis models. AAPS PharmSciTech. 2013;14:880–9.
Lane J, Sandhu H. Current approaches to experimental bone grafting. Orthop Clin North Am. 1987;18:213–25.
Zhu X, Cheng Y, Du L, Li Y, Zhang F, Guo H, et al. Mangiferin attenuates renal fibrosis through down-regulation of osteopontin in diabetic rats. Phytother Res. 2015;29:295–302.
Mandal B, Kundu S. Calcium alginate beads embedded in silk fibroin as 3D dual drug releasing scaffolds. Biomaterials. 2009;30:5170–7.
Wang J, Yang W, Xie H, Song Y, Li Y, Wang L. Ischemic stroke and repair: current trends in research and tissue engineering treatments. Regen Med Res. 2014;2:3.
Wang Y, Liu X, Zhao J, Kong X, Shi R, Zhao X, et al. Degradable PLGA scaffolds with basic fibroblast growth factor: experimental studies in myocardial revascularization. Tex Heart Inst J. 2009;36:89–97.
Liu B, Cai S, Ma K, Xu Z, Dai X, Yang L, et al. Fabrication of a PLGA-collagen peripheral nerve scaffold and investigation of its sustained release property in vitro. J Mater Sci Mater Med. 2008;19:1127–32.
Oh S, Kang S, Lee J. Degradation behavior of hydrophilized PLGA scaffolds prepared by melt-molding particulate-leaching method: comparison with control hydrophobic one. J Mater Sci Mater Med. 2006;17:131–7.
Khaled K, Sarhan H, Ibrahim M, Ali A, Naguib Y. Prednisolone-loaded PLGA microspheres. In vitro characterization and in vivo application in adjuvant-induced arthritis in mice. AAPS PharmSciTech. 2010;11:859–69.
Lee D, Kwon T, Kim K, Kwon S, Cho D, Jang S, et al. Anti-inflammatory drug releasing absorbable surgical sutures using poly(lactic-co-glycolic acid) particle carriers. Polym Bull. 2014;71:1933–46.
Brochhausen C, Zehbe R, Watzer B, Halstenberg S, Gabler F, Schubert H, et al. Immobilization and controlled release of prostaglandin E2 from poly-L-lactide-co-glycolide microspheres. J Biomed Mater Res A. 2009;91:454–62.
Brownfield L, Weltman R. Ridge preservation with or without an osteoinductive allograft: a clinical, radiographic, micro-computed tomography, and histologic study evaluating dimensional changes and new bone formation of the alveolar ridge. J Periodontol. 2012;85:581–9.
Jonnalagadda J, Rivero I, Dertien J. In vitro chondrocyte behavior on porous biodegradable poly(e-caprolactone)/polyglycolic acid scaffolds for articular chondrocyte adhesion and proliferation. J Biomater Sci Polym Ed. 2015;26:401–19.
Song J, Li J, Hou F, Wang X, Liu B. Mangiferin inhibits endoplasmic reticulum stress-associated thioredoxin-interacting protein/NLRP3 inflammasome activation with regulation of AMPK in endothelial cells. Metabolism. 2015;64:428–37.
Lee C, Lee Y. Preparation of porous biodegradable poly(lactide-co-glycolide)/hyaluronic acid blend scaffolds: characterization, in vitro cells culture and degradation behaviors. J Mater Sci Mater Med. 2006;17:1411–20.
Chang P, Chung M, Wang Y, Chien L, Lim J, Liang K, et al. Patterns of diabetic periodontal wound repair: a study using micro-computed tomography and immunohistochemistry. J Periodontol. 2012;83:644–52.
Graves D, Alblowi J, Paglia D, O’Connor J, Lin S. Impact of diabetes on fracture healing. J Exp Clin Med. 2011;3:3–8.
Stolzing A, Sellers D, Llewelyn O, Scutt A. Diabetes induced changes in rat mesenchymal stem cells. Cells Tissues Organs. 2010;191:453–65.
Das A, Fishero B, Christophel J, Li C, Kohli N, Lin Y, et al. Poly(lactic-co-glycolide) polymer constructs cross-linked with human BMP-6 and VEGF protein significantly enhance rat mandible defect repair. Cell Tissue Res. 2015.
Acknowledgments
This work was supported by the National Natural Science Foundation of China (No. 81200794), Guangxi Natural Science Foundation (No. 2015GXNSFBA139140), Guangxi Scientific and Technologic Research Project of Colleges and Universities (No. KY2015YB060), and Youth Science Foundation of Guangxi Medical University (No. GXMUYSF2014017).
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Li, H., Liao, H., Bao, C. et al. Preparation and Evaluations of Mangiferin-Loaded PLGA Scaffolds for Alveolar Bone Repair Treatment Under the Diabetic Condition. AAPS PharmSciTech 18, 529–538 (2017). https://doi.org/10.1208/s12249-016-0536-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1208/s12249-016-0536-9