Abstract
Background
This study aims to compare the graft uptake rate and hearing improvement of fat graft versus inlay butterfly tragal cartilage in the repair of perforations in chronic otitis media mucosal in adults.
In this retrospective study, twenty-eight patients were included with small dry anteroinferior tympanic membrane perforations (less than 1/3 of the tympanic membrane). The age range was 18 to 44 years old. Myringoplasty was done under general anesthesia for 8 patients with a fat graft (FG) and 20 patients with inlay butterfly cartilage graft (IBCG). Six months postoperatively, a follow-up evaluation was done for successful graft uptake and hearing outcomes.
Results
The success rate of graft uptake in the first group (fat graft) was 6/8 cases (75%) while in the second group (IBCG) was 19/20 (95%) with no statistically significant difference (P = 0.0148). Also, there was no statistical difference between the two groups as regards postoperative ABG, improvement changes in ABG, and number of patients with improved hearing.
Conclusions
Inlay butterfly cartilage graft is a useful graft in repairing small tympanic membrane perforations as regard graft take and hearing outcomes.
Similar content being viewed by others
Background
Myringoplasty is a procedure to repair tympanic membrane perforation [1]. Different autologous and heterologous materials were used to repair perforations with different techniques that require elevation of meatal flaps [2].
Ringenberg in 1962 was the first to report a transcranial approach without elevation of the tympano-meatal flap using fat plug myringoplasty [3], while the first reported cartilage usage in 1963 by Salen and Jansen [4, 5].
Various techniques of cartilage graft were applied which are palisade, cartilage shield, perichondrium-cartilage island flap, and inlay butterfly graft. In 1998, Eavey was the first to describe the inlay butterfly cartilage graft in type I tympanoplasty through a transcranial approach [6].
Our study compares the graft uptake and hearing improvement rate of fat graft versus inlay butterfly tragal cartilage (IBCG) in the repair of small size perforations in chronic otitis media mucosal in adults.
Fat graft myringoplasty is a safe procedure with limited postoperative care, less pain, and small invisible scar. Fat can be taken from the ear lobule with a comparable success rate with myringoplasty using temporalis fascia graft for management of small perforations without support in the middle ear [7]. Also, inlay butterfly cartilage has the same advantages as the fat graft, and it can be inserted in the tympanic membrane with tympanosclerosis. Moreover, IBCG is locked in the tympanic membrane as a grommet’s tube without the need for support in the middle ear or external canal [6, 8].
Methods
Study sample
This a retrospective study was done between the years 2017 and 2019 to compare patients who underwent myringoplasty with inlay butterfly cartilage graft versus fat graft in the repair of small size perforations in chronic otitis media mucosal in the last 3 years. The age was between 18 and 44 years old with 17 males and 11 females. Ethics committee approval was done. Informed written consent was taken from patients.
The patients were divided into two groups. Group 1 involves 8 patients who underwent transcanal myringoplasty using a fat plug harvested from the ear lobule. Group 2 composed of 20 patients underwent transcranial myringoplasty by inlay butterfly tragal cartilage. All procedures were done under general anesthesia.
The patients enrolled in the study were adults between 18 and 44 years old with unilateral tympanic membrane perforation due to chronic otitis media mucosal with no ossicular pathology. The perforation was central and less than 1/3 of the tympanic membrane surface (less than 5 mm) in the anteroinferior quadrant of the tympanic membrane. Moreover, there was no active infection and pus in the last 3 months.
Patients with other etiologies of tympanic membrane perforations were excluded: trauma, cholesteatoma, and previous ear surgeries. Other exclusion criteria were age under 18 years and above 44, bilateral tympanic membrane perforations, tympanosclerosis, bullous myringitis, nasopharyngeal pathology, and patients with diabetes mellitus and chronic diseases. Also, patients with congenital anomalies were excluded.
Audiological evaluation
After a full history and complete ear, nose, and throat examination including flexible fiberoptic nasopharyngoscopy to exclude nasopharyngeal pathology, pure tone audiometry was performed for all subjects using a clinical audiometer and pre-operative ABG was calculated by taking the averages of bone conduction besides air conduction at the frequencies of 500,1000 and 2000 Hz.
The preoperative Eustachian tube (ET) function was measured using a modified pressure equilibration inflation-deflation test [9]. After confirmation of dryness of both the external and middle ear by otoscopy, a probe was fitted into the external auditory canal, and the pressure was varied over ± 300 daPa. Each patient was asked to swallow three times at intervals of 3–5 s with the nose and mouth closed. After each swallow, the applied pressure was normalized. The residual pressure after three swallows was recorded. ET function was evaluated and graded regarding residual pressure after each application of positive or negative pressure. This was done to all patients 3 days before surgery.
Surgical procedure
All surgeries were done under general anesthesia using a mask and not endotracheal tubes. The edges of perforation trimmed using a Plester sickle knife. The graft size should be slightly larger than the trimmed perforation.
Fat graft (FG)
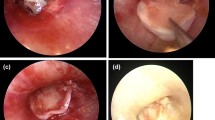
It was harvested from the ear lobule through a small incision at its inferior border. The fat plug was pushed through towards the middle ear. This caused inward inversion of the perforation edges. The graft was mobilized outwards to evert the perforation edges by a crocodile forceps or micro-sucker. The graft was supported by a silastic sheet disc in the external meatus; then, the meatus was filled with gel foam (Fig. 1).
Inlay butterfly cartilage graft (IBCG)
It was harvested through a 1-cm vertical incision on the upper edge of the tragus coinciding with the inner part of the end-aural incision. The IBCG was harvested with a size 3–4 mm larger than the perforation after trimming its edge. This is preferred over a horizontal incision to preserve the remaining tragal cartilage if needed for further procedure. The lateral perichondrium was removed preserving a medial one. Then, a circumferential fissure was created along the graft edge with a depth of about 1–1.5 mm (Fig. 2). Gently, the IBCG was applied obliquely by crocodile forceps in the same way of applying the grommet tubes. The split edge was placed to embrace the perforation edges; then, the position was adjusted using the fine tip of a sickle Plester knife. Finally, the graft was supported by a silastic disc and the external canal was filled with gel foam (Fig. 3).
Postoperative
All patients were discharged the same day of the surgery with oral antibiotics amoxicillin clavulonate and paracetamol as analgesics for 1 week. No suction was applied to the operated ears. Follow-up for 6 months postoperatively was done with an endoscopic and microscopic examination to all patients to evaluate complete closure of the perforation and ensure graft take success. Audiometry was done only for successful cases at 6 months postoperatively.
Statistical analysis
Fisher’s exact and chi-square tests were used to examine the relationship between categorical variables such as demographic data and graft uptake rates. A P value < 0.05 was considered significant.
Results
In our study, 28 patients aged between 18 and 44 years old were enrolled. All patients attended the follow-up for 6 months. They were 16 males and 12 females who underwent transcanal myringoplasty under general anesthesia. The patients divided into 2 groups: group 1 composed of 8 patients with homograft fat myringoplasty, and group 2 composed of 20 patients with homograft inlay cartilage butterfly (Table 1). No statistically significant difference in the preoperative air-bone gap (ABG) between the 2 groups as shown in Table 1.
Six months postoperatively, the success rate of the first group FG was 6/8 cases (75%) while in the second group IBCG, it was 19/20 (95%). There was no statistically significant difference between the two groups (P = 0.188) (Table 2). Audiometry was done on all 23 patients with successful graft uptake and complete closure of the perforation. Table 2 showed no statistical significance difference between the 2 groups as regards the postoperative air-bone gap, number of patients with improved hearing, and improvement change in ABG.
Discussion
In our study, successful graft take is 95% in group 2 with IBCG with no statistically significant difference when compared to group 1 with fat graft uptake of 75%. Our success rate in IBCG is in line with the success rate of other studies and literature which showed a rate between 71 and 100% [8]. In 2005, Couloigner et al. showed graft healing rates were 71% for the butterfly technique using Eavey’s procedure as modified by Lubianca [10], while Riss et al. in 2016 showed a higher graft success rate 85.7% in pediatric patients [8]. In 2006, Ghanem et al. expanded IBCG to repair larger perforation of the tympanic membrane with a 92% success rate in patients aged 2 to 20 years old [11]. This may be explained by the fact that IBCG can be stabilized much better in its place, needs minimal blood supply for healing, and resist more the effect of mild infection.
Fat is an hourglass plug technique that does not need middle ear support and does not show collapse [12]. Unfortunately, the success rate of fat graft in this study is 75%. It is a low success rate when compared to other studies. Ringenberg [3], Chalishazar [13], and Mitchel et al. [14] reported success rates of 87% and 92%, respectively. This may be due to inappropriate randomization of patients and a small sample of patients in whom we used fat as a graft.
Hearing improvement is the other outcome measured in our study. Audiometry was done 6 months postoperatively, with the calculation of ABG, to the patients with a successful graft taken and complete closure of the perforation. Postoperative ABGs were improved in 20 patients (4 in group 1 and 16 in group 2). There was no statistical difference between the 2 groups as regards postoperative ABG, the number of patients with improved hearing, and improvement changes in ABG (Table 2).
In group 1 with a fat graft, four patients out of six had improved hearing (66.6%). Previous literature showed wide variations of postoperative hearing improvements. While Hagemann and Housler [15] in 2003 had 21 patients with hearing improvement of their 44 patients (47.72%), Liew et al. [16] recorded an improvement in 11 of their 15 patients (73.3%).
In group 2 with IBCG 16 patients had hearing improvement (80%). Eavey [6] stated that all his pediatric patients had a normal postoperative hearing with an average hearing of 12 dB. Ghanem et al. [11] reported acceptable hearing results for large perforations after IBCG despite the need for mastoidectomy in many patients. In his study hearing in the 0–10 dB range following surgery were doubled from 16 to 32 ears with a statistically significant difference. Other studies like Mauri et al. [17] and Wang and Lin [18] showed a significant improvement in hearing results for patients with IBCG, but the difference between these 2 groups (IBCT and underlay cartilage graft) was not statistically significant.
The average time of performing that type of repair in our study was 35 min. Both types are easy, simple, and quick techniques for the repair of small tympanic membrane perforation without iatrogenic trauma to the middle ear. Surgery performed under general anesthesia using mask without need postauricular incisions or elevation of tympanomeatal flap [14].
Our study sample is small, and we recommend other prospective randomized large sample studies to get more precise results especially since these two types of grafts are underused. Although the sample size is small, a higher study power may be able to show a statistically significant difference in the outcome.
Conclusions
Inlay butterfly cartilage graft is a useful graft in repairing small tympanic membrane perforations as regards graft take and hearing outcomes.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- IBCG:
-
Inlay butterfly cartilage graft
- ABG:
-
Air bone gap
- ET:
-
Eustachian tube
- FG:
-
Fat graft
References
Rizer FM (1997) Overlay versus underlay tympanoplasty. Part I: a historical review and a comparison of techniques. Laryngoscope. 107:1–25. https://doi.org/10.1097/00005537-199712001-00001
Gross CW, Bassila M, Lazar RH et al (1989) Adipose tissue plug myringoplasty: an alternative to formal myringoplasty techniques in children. Otolaryngol Head Neck Surg 101:617–620. https://doi.org/10.1177/019459988910100601
Ringenberg J (1962) Fat graft tympanoplasty. Laryngoscope. 72:188–192. https://doi.org/10.1288/00005537-196202000-00005
Salen B (1963) Myringoplasty using septum cartilage. Acta Otolaryngol 188:82–91
Jansen C (1963) Cartilage-tympanoplasty. Laryngoscope. 73:1288–1302. https://doi.org/10.1288/00005537-196310000-00006
Eavey RD (1998) Inlay tympanoplasty: cartilage butterfly technique. Laryngoscope 108:657–661. https://doi.org/10.1097/00005537-199805000-00006
Ozgursoy OB, Yorulmaz I (2005) Fat graft myringoplasty: a cost-effective but underused procedure. J Laryngol Otol 119:277–279. https://doi.org/10.1258/0022215054020377
Riss JC, Roman S, Morredu E et al (2016) Butterfly-cartilage tympanoplasty in children: a 28-case series and literature review. Eur Ann Otorhinolaryngol Head Neck Dis 133:179–182. https://doi.org/10.1016/j.anorl.2016.02.004
Yuceturk AV, Unlu HH, Okumus M et al (1997) The evaluation of eustachian tube function in patients with chronic otitis media. Clin Otolaryngol Allied Sci 22(5):449–452. https://doi.org/10.1046/j.1365-2273.1997.00029.x
Couloigner V, Baculard F, El Bakkouri W et al (2005) Inlay butterfly cartilage tympanoplasty in children. Otol Neurotol 26:247–251. https://doi.org/10.1097/00129492-200503000-00020
Ghanem MA, Monroy A, Alizade FS et al (2006) Butterfly cartilage graft inlay tympanoplasty for large perforations. Laryngoscope 116:1813–1816. https://doi.org/10.1097/01.mlg.0000231742.11048.ed
Hegazy HM (2013) Fat graft myringoplasty – a prospective clinical study. Egyptian J Ear, Nose, Throat Allied Sci 14:91–95. https://doi.org/10.1016/j.ejenta.2012.11.006
Chalishazar U (2005) Fat plug myringoplasty. Indian J Otolaryngol Head Neck Surg 57:43–44. https://doi.org/10.1007/BF02907626
Mitchell RP, Periera KD, Lazer RH (1997) Fat graft myringoplasty in children: a safe and successful day-stay procedure. J Laryngol Otol 111:106–108. https://doi.org/10.1017/s002221510013659x
Hagemann M, Housler R (2003) Tympanoplasty with adipose tissue. Laryngorhinootologie. 82(6):393–396. https://doi.org/10.1055/s-2003-40537
Liew L, Daudia A, Narula AA (2002) Synchronous fat plug myringoplasty and tympanostomy tube removal in the management of refractory otorrhoea in younger patients. Int J Pediatr Otorhinolaryngol 66(3):291–296. https://doi.org/10.1016/s0165-5876(02)00257-4
Mauri M, LubiancaNeto JF, Fuchs SC (2001) Evaluation of inlay butterfly cartilage tympanoplasty: a randomized clinical trial. Laryngoscope 111(8):1479–1485. https://doi.org/10.1097/00005537-200108000-00027
Wang WH, Lin YC (2008) Minimally invasive inlay and underlay tympanoplasty. Am J Otolaryngol 29(6):363–366. https://doi.org/10.1016/j.amjoto.2007.11.002
Acknowledgements
Not applicable.
Funding
There is no funding.
Author information
Authors and Affiliations
Contributions
AK, MAE, and MME contributed to the following: idea, protocol, patient selection, surgery, follow-up, data analysis, and writing the manuscript. PA contributed to the idea, protocol, preoperative and postoperative hearing tests, and writing the manuscript. The authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was approved by the ethics committee of the Magrabi Hospital. The reference number is ENT-12-0009Q. Informed written consent was taken from all patients to participate in the study.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Khafagy, A.G., El-Begermy, M., El-Begermy, M.M. et al. Comparative study between fat plug and inlay butterfly cartilage grafts for myringoplasty in adults. Egypt J Otolaryngol 37, 13 (2021). https://doi.org/10.1186/s43163-021-00076-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43163-021-00076-y