Abstract
Background
Despite the overall major impact of long-lasting insecticide treated nets (LLINs) in eliciting individual and collective protection to malaria infections, some sub-Saharan countries, including Burkina Faso, still carry a disproportionately high share of the global malaria burden. This study aims to analyse the possible entomological bases of LLIN limited impact, focusing on a LLIN-protected village in the Plateau Central region of Burkina Faso.
Methods
Human landing catches (HLCs) were carried out in 2015 for 12 nights both indoors and outdoors at different time windows during the highest biting activity phase for Anopheles gambiae (s.l.). Collected specimens were morphologically and molecularly identified and processed for Plasmodium detection and L1014F insecticide-resistance allele genotyping.
Results
Almost 2000 unfed An. gambiae (s.l.) (54% Anopheles coluzzii and 44% Anopheles arabiensis) females landing on human volunteers were collected, corresponding to a median number of 23.5 females/person/hour. No significant differences were observed in median numbers of mosquitoes collected indoors and outdoors, nor between sporozoite rates in An. coluzzii (6.1%) and An. arabiensis (5.5%). The estimated median hourly entomological inoculation rate (EIR) on volunteers was 1.4 infective bites/person/hour. Results do not show evidence of the biting peak during night hours typical for An. gambiae (s.l.) in the absence of bednet protection. The frequency of the L1014F resistant allele (n = 285) was 66% in An. coluzzii and 38% in An. arabiensis.
Conclusions
The observed biting rate and sporozoite rates are in line with the literature data available for An. gambiae (s.l.) in the same geographical area before LLIN implementation and highlight high levels of malaria transmission in the study village. Homogeneous biting rate throughout the night and lack of preference for indoor-biting activity, suggest the capacity of both An. coluzzii and An. arabiensis to adjust their host-seeking behaviour to bite humans despite bednet protection, accounting for the maintenance of high rates of mosquito infectivity and malaria transmission. These results, despite being limited to a local situation in Burkina Faso, represent a paradigmatic example of how high densities and behavioural plasticity in the vector populations may contribute to explaining the limited impact of LLINs on malaria transmission in holo-endemic Sudanese savannah areas in West Africa.

Similar content being viewed by others
Background
Long-lasting insecticide treated nets (LLINs) are very effective in reducing malaria transmission by combining individual physical protection to people sleeping under the nets with collective protection provided by the insecticidal activity of pyrethroids restrained in the net fibres [1]. Published data show that this community effect is reached when net usage in the population exceeds 50% [2, 3]. Since 2005, massive campaigns of three-year periodical distributions of LLINs have been implemented in many malaria-endemic countries. In sub-Saharan African countries, about 254 million LLINs were supplied between 2008–2010 and a further 806 million between 2011–2016 [1, 4]. It has been estimated that 68% of the 663 million malaria cases prevented in the first 15 years of this century in Africa, are due to the usage of LLINs [5]. Despite this success, most of sub-Saharan Africa still carries a disproportionately high share of the global malaria deaths [6,7,8,9] and the WHO has registered a stalling of the progress in the fighting against malaria since 2015. Particularly, the effectiveness of LLINs seems to be heterogeneous in some sub-Saharan hyper-endemic countries where the annual incidence is still very high [10].
Among many causal factors for this scenario (e.g. bednet quality and usage, ecological context), a crucial role is played by insecticide resistance, which undermines LLINs collective protective effect by reducing mosquito exposure to lethal dose of pyrethroids within the nets. Indeed, multiple mechanisms of resistance to pyrethroid insecticides have been observed in African Anopheles populations [11,12,13]: increased metabolic detoxification of insecticide molecules by enhanced enzyme activity (e.g. P450 monooxygenase) [13], mutations in insecticide target site (e.g. mutations in the para-type sodium channel gene, kdr mutations [14]) and/or mosquito behavioural adaptations (e.g. increased exophily, opportunistic biting activity and/or shift in biting activity [15]). Moreover, according to Killeen et al. [16], vector species composition could be a limiting factor to reduce mosquito density to a level sufficient to obtain a relevant impact on malaria transmission through LLINs: massive abatement can be expected where major vector species feed mostly indoors on humans. On the other hand, where generalistic/opportunistic species are dominant, LLINs need to be combined with other interventions to obtain an effect on vector population and subsequently on malaria transmission.
This might be the case for Burkina Faso where the increase in LLIN coverage, from 20% to 70% between 2009–2014, did not significantly affect malaria annual incidence, with an increasing number of cases reported each year [5, 17,18,19,20,21,22,23]. In a previous study carried out in 2011 in the village of Goden (Burkina Faso) one year after LLINs introduction, we observed an unexpected high sporozoite rate (SR) in the major malaria vectors in the area (i.e. 7.6% in Anopheles coluzzii and 5.3% in Anopheles arabiensis) despite low human blood index (20.1% in An. coluzzii and 5.8% in An. arabiensis [24]). Similar infective rates were also confirmed in a subsequent entomological survey conducted in the same village in 2012 (SR = 6.6% in An. coluzzii [25]). These observations suggest that, despite LLINs having significantly reduced human/vector contact in holo-endemic areas such as Burkina Faso, they have not apparently led to a substantial reduction of mosquito infection rates.
Thanks to human landing catches carried out in the same village five years after mass LLIN introduction, we here provide evidence on how high densities and behavioural plasticity of An. coluzzii and An. arabiensis, in association with insecticide resistance mechanisms, undermine the community protective effect of LLIN and reduce the impact of LLINs on malaria transmission in the Ziniaré district of Burkina Faso.
Methods
Sampling area
Field collections were carried out in November 2015 (i.e. at the end of rainy season, just after the peak of malaria transmission) in a holo-endemic [26] Sudanese-savannah village in the Plateau Central region (12° 25′ N, 1° 21′ W; Zinaré health district), 41 km East of Ouagadougou, the capital city of Burkina Faso. The sampling occurred in Goden, a rural village with approximately 800 inhabitants mainly belonging to the Mossi ethnic group, mostly devoted to agriculture, and rearing a few animals and occasional settlements of Fulani ethnic group devoted to cattle. From 2010 LLINs were widely distributed in the Plateau Central region. Although specific data on the actual LLIN coverage, quality and usage in the study site are not available, more than 9 million LLIN have been distributed in the whole country during 2013 campaign [27], with 64% of population coverage estimated in the Plateau Central region [28], a level above the threshold needed to elicit a community protective effect [2, 3].
Entomological collections and molecular analysis
Host-seeking mosquitoes were collected by human landing catch (HLC) in two houses, both indoors and outdoors, at three different time windows (21:00–22:00 h; 00:00–01:00 h; 03:00–04:00 h) for a total of 12 nights. This interval corresponds to the highest biting activity phase reported for An. gambiae (s.l.) [29]. During the sampling period, no other human host was present in the houses with the exception of the volunteer who performed the collection and no LLINs or IRS were used.
All mosquitoes were morphologically identified under stereomicroscope [30], separated by species and sex. Heads and thoraces of An. gambiae (s.l.) females were dissected from abdomens and stored individually in tubes containing desiccant. DNA was extracted from heads and thoraces according to DNAZOL protocol (Molecular Research Center, Cincinnati, Ohio) [31]. Species were molecularly identified by SINE-PCR [32]. DNA from heads and thoraces was used as templates for Plasmodium sporozoite DNA detection by real-time PCR [33]. Subsamples of An. arabiensis and An. coluzzii were further processed by real-time PCR for genotyping L1014 (kdr-w), the most ancient and common insecticide-resistance associated allele in the sodium-gated voltage-channel gene [14, 34, 35].
Statistical analysis
Differences in biting activity indoors vs outdoors and among different time windows of HLC collections were analysed by Mann-Whitney and Kruskal-Wallis tests (after assessment of non-normal distribution of data by Shapiro-Wilk test) for An. gambiae (s.l.), as well as for single species of the complex. Chi-square test was employed to investigate possible differences in sporozoite rate among species and between positions of sampling within each species. Chi-square test was also applied to assess prospective diversities in insecticide resistance level between species, between indoor vs outdoor collections within each species and between different infectivity states.
Generalized linear mixed effect models (GLMM) were built to verify variation in the abundance of vector species (Anopheles gambiae (s.l.), An. arabiensis, An. coluzzii) between trapping positions (indoors, outdoors), between houses (A and B) and among different HLC time windows (21:00–22:00 h; 00:00–01:00 h; 03:00–04:00 h). As the response variable of mosquito abundances is highly over-dispersed, a negative binomial distribution was chosen. For each species, two models were built, both including time windows, trapping locations and houses as covariates and the sampling days as a random effect. The two models differed in: (i) no interaction among variables; and (ii) interaction between trapping location and house. The best model was chosen by the Akaike information criterion (AIC) and likelihood ratio test. The tests were conducted using the R statistical software version 3.5.0 [36] with lme4 package [37].
Overall hourly entomological inoculation rate (EIR) was calculated multiplying the median number of human biting mosquitoes in an hour (obtained by HLC data) with the estimated sporozoite rate.
Results
During the 12 nights of sampling, 1996 unfed mosquito females were collected landing on human volunteers, corresponding to a median number of 23.5 females/hour/person. All of them were morphologically identified as An. gambiae (s.l.), of which 53.9% were An. coluzzii, 43.5% An. arabiensis and 0.5% An. gambiae (s.s). One An. coluzzii/An. gambiae (s.s) hybrid was found and 42 specimens (2.1%) were not successfully identified by PCR (Table 1).
No significant differences were observed in median numbers of mosquitoes collected indoors and outdoors (Mann-Whitney test: An. arabiensis, U = 0.51, P = 0.90; An. coluzzii, U = 0.52, P = 0.77; An. gambiae complex, U = 0.52, P = 0.74; Fig. 1). GLMM results indicated a higher abundance of An. arabiensis and An. coluzzii outdoors in one of the two houses sampled (see Additional file 1: Table S2). No significant differences were observed in median numbers of females collected during the three HLC-time windows (Kruskal-Wallis test; GLMM results: An. arabiensis, T = 1.16, P = 0.56; An. coluzzii, T = 2.84, P = 0.24; An. gambiae complex, T = 0.83, P = 0.66; Additional file 1: Table S2).
Overall, a 5.8% sporozoite rate (SR) was estimated: 114 An. gambiae (s.l.) females were found positive for P. falciparum, 1 for Plasmodium sp. (either P. vivax, P. ovale or P. malariae), and 1 for mixed infection (i.e. presence of both P. falciparum and P. vivax/P. ovale/P. malariae). No significant differences in SR were detected between An. coluzzii (6.1%) and An. arabiensis (5.5%) (χ2 = 0.2, P = 0.7), nor between samples collected indoors and outdoors (An. arabiensis: 6.6% indoors, 4.9% outdoors, χ2 = 1.5, P = 0.22; An. coluzzii 6.9% indoors, 5.2% outdoors, χ2 = 1.1, P = 0.24). The estimated median hourly entomological inoculation rate (EIR) was 1.4 infective bites/hour per human volunteer, corresponding to a cumulative EIR of 9.8 infective bites during the 7-hour sampling interval.
The observed frequency of kdr-w resistant allele was 66% in An. coluzzii (n = 163) and 38% in An. arabiensis (n = 122). The frequency of the homozygous resistant genotype was significantly higher in An. coluzzii (χ2 = 59.4, P < 0.0001) (Table 2). No differences in resistance genotypes were detected in indoors vs outdoors collected samples (An. coluzzii, χ2 = 0.3, P = 0.65; An. arabiensis, χ2 = 1.4, P = 0.49), nor in infective (n = 100) vs not infective (n = 188) specimens (χ2 = 2.3, P = 0.32). This, in agreement with Traoré et al. [38] and Doumbe-Belisse et al. [39], does not confirm previous reports of higher P. falciparum infective status/susceptibility in kdr-resistant mosquitoes [40,41,42].
Discussion
Our results show that at the end of rainy season, inhabitants of Goden are potentially exposed to at least ten infective bites/person/night, despite five years since the beginning of LLIN mass distribution campaign in Plateau Central region of Burkina Faso [28]. Indeed, the fraction of bednet-protected people (about two-thirds of the whole population [28]) are likely exposed to mosquito-bites in early evening and early morning, when not sleeping under the LLIN and receive much less infective bites than estimated in the present study. However, the high biting rates observed between 21:00 and 22:00 h (when most people are inside houses and possibly not yet protected by LLINs; CNRFP, unpublished data) suggest actual high levels of exposure of the Goden population. This levels of exposures are unusually high compared to EIRs reported (per night) before LLIN distribution in the same village (mean 7.4, min 2.5, max 17.0 [43]), as well as in the Plateau Central region of Burkina Faso (mean 2.3, min 0.2, max 8.3 [44, 45]), as well as those reported in other regions of Burkina Faso (2.4 [46]) and in other sub-Saharan African countries where LLINs are in use (ranging from 0.04 to 3.4 [47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63]).
The estimated EIR value is due to both high malaria vector densities (HBR = 23.5 females/hour/person) and very high levels of infectivity in the vector population (SR = 5.8%). Both biting rate and infectivity rate are in line with the few literature data available for An. gambiae (s.l.) in Goden (1.8 < SR < 12.1 [43]) and in the same geographical area before LLIN implementation (0.5 < HBR < 26.3 [64, 65]; 3 < SR < 10 [64,65,66] in 6 villages in a radius of 40 km from Ouagadougou) and comparable to SR in Goden in 2011 (6.9% [24]) and 2012 (6.6% [25]). Notably, even though SRs were assessed by different approaches in different studies, results by recently developed rDNA-based TaqMan assays [33, 67] do not significantly differ to those obtained by traditionally used CSP-ELISA [67].
Data also shed some light on other entomological factors, which could have reduced LLIN-effectiveness after 5-year implementation (i.e. endophagy vs exophagy, time of biting and genetic resistance to insecticides) in the two main malaria vector species in the village, i.e. An. coluzzii and An. arabiensis.
First, our results do not suggest endophagic preferences in either vector species, in agreement with what observed in An. coluzzii in other settings characterized by massive LLIN coverage (North-West Burkina Faso [46], Benin [68] and Bioko Island [69]). Although most studies focusing on resting mosquitoes indirectly suggest high endophagy for An. coluzzii/An. gambiae, the few studies carried out by HLC both indoors and outdoors show lack of preference for the biting location even before LLIN implementation [70,71,72,73,74,75,76,77]. Overall, this highlights that anthropophily is the main driver of the endophagic behaviour in An. coluzzii/An. gambiae. Consequently, the supposed higher exophagy of An. arabiensis is a consequence of its generalistic host preference [78, 79]. Thus, in cases of reduced human-host availability indoors due to LLIN, both An. coluzzii and An. arabiensis do not require a secondary adaptation to bite outdoors, as they are already adapted to do it. Notably, mathematical models suggest that even relatively modest changes in outdoor biting can have a substantial public health impact (e.g. a 10% increased outdoor biting activity could result in 10.6 million additional malaria cases in whole Africa, even assuming a 100% LLINs coverage) [29].
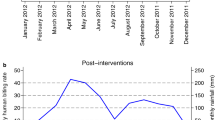
Secondly, no differences in biting rates were observed between 21:00 and 4:00 h in vector species. Indeed, a peak of activity during night hours is typical for An. gambiae (s.l.) in the absence of bednet protection [71, 72, 74, 75, 80,81,82,83,84,85]. To our knowledge, a lack of peak of activity was observed in An. coluzzii only in Burkina Faso [46] and in Bioko Island [69] where, two years after the introduction of LLINs, the proportion of host-seeking events changed towards a lack of significant differences throughout the night. On the other hand, a wide range of peak biting times (i.e. early, late or “central” night activity) has been reported in An. arabiensis after control interventions [52, 86,87,88,89]. According to theoretical predictions, lack of biting time peak is indicative of a situation in which the selective pressure exerted by LLIN has altered the typical biting pattern, but has not been yet sufficient to trigger a strong shift towards earlier and later biting times (Fig. 2; [90]) Expanding the duration of HLC before dusk and after dawn would allow to analyse more in detail a possible peak of biting activities to earliest and latest hours to access hosts unprotected by LLINs, as reported by Russell et al. [91]. In particular, measuring the numbers of host-seeking mosquitoes at times when people are still engaged in working activities outdoors would give a better estimate of actual risk of malaria transmission in the area.
Predictive model describing the biting time profile of mosquitoes for different proportion of inhabitants using bednets: absence of coverage (a); intermediate coverage (b); full coverage (c). In b the model curve is overlapped with the human biting activity observed in sampling time windows in Goden, Burkina Faso (21:00–22:00 h; 00:00–01:00 h; 03:00–04:00 h). Differently from the theoretical model proposed by Ferreira et al. [90], in this study the curve of the biting activity is shrinked to three time windows, from which 100% of mosquitoes are counted. This results in a higher relative proportion of mosquitoes in this time window compared to the model curve (x-axis, hours; y-axis, percentage of biting mosquitoes). Modified from Ferreira et al. (2017) Modelling the impact of the long-term use of insecticide-treated bed nets on Anopheles mosquito biting time. Malar J. 16:373 [90] (Creative commons license http://creativecommons.org/licenses/by/4.0)
Thirdly, while we did not carry out insecticide resistance bioassays, we genotyped a subsample of collected specimens for the locus L1014 of the sodium-gated voltage-channel gene, known to be one of the markers associated to pyrethroid resistance, to speculate on the possible role of insecticide resistance in contributing to high levels of transmission in the village by increasing survival of endophagic vectors entering in contact with the bednet. We found frequencies of the L1014F allele of 67% and 38% in An. coluzzii and An. arabiensis, respectively (without significant differences between indoor and outdoor collections), suggesting that pyrethroids are selecting target site resistance in the study site. Notably, the deterrent effect of LLINs on partially resistant (either behaviourally or genetically) mosquitoes is known to diverge biting activity to unprotected hosts both indoors and outdoors [92,93,94,95].
Effectiveness of ITN/LLINs relies on anthropophilic and therefore endophagic behaviour of vector populations and susceptibility to insecticides used to impregnate the bednets. A limited number of studies showed that changes in vector biting behaviour, as well as shift in species dominance, following LLIN implementation can undermine the efficacy of such control measures (Additional file 1: Table S3). A species shift was repeatedly shown in East Africa where, after LLIN introduction, the former most abundant highly anthropophilic vector, An. gambiae, has been outnumbered by the more generalist An. arabiensis, leading to an overall decrease in sporozoite rates [51,52,53, 88, 96,97,98,99,100]. To our knowledge, shifts in vector dominance after LLIN introduction has never been investigated in West and Central Africa (where An. coluzzii is also present), with the exception of Bioko Island, where a progressive replacement of An. gambiae by An. coluzzii was observed as indoor control measures were applied [69]. Our results do not show a shift in species composition following 5-year LLIN implementation in the study area in Burkina Faso where, even before bednet introduction, An. coluzzii and An. arabiensis were the main circulating vectors and An. gambiae was uncommon [101]. Nevertheless, our results suggest that LLINs have elicited a “behavioural resilience” (sensu Govella et al. [102]) in An. coluzzii, leading to the biting rhythms observed in the present study [72, 75, 84], as well as to a higher zoophagy, as detected in 2011 [24]. Indeed, An. coluzzii is known to be characterized by high ecological plasticity in the exploitation of different habitats [103,104,105,106,107,108,109], as well as by an opportunistic host-seeking behaviour [16, 69, 110]. Overall, the ecological plasticity of the two main vectors maximises their capacity to reach the human host when not protected by bednets, consistent with the high biting and sporozoite rates observed in the study site.
Conclusions
Our results, despite being limited to a local situation in Burkina Faso, represent a paradigmatic example of how behavioural plasticity in the vector population may contribute to explain the limited impact of LLINs on malaria transmission in malaria holo-endemic Sudanese savannah areas in West Africa. Data suggest that the capacity of the two main vectors in the study site (An. coluzzii and An. arabiensis) to adjust their host-seeking behaviour to bite humans despite bednet protection, coupled with high densities and insecticide resistance, can undermine LLIN community protective effect, allowing the maintenance of high rates of mosquito infectivity and malaria transmission. The behavioural plasticity of An. coluzzii here highlighted suggests that this species is capable to react to indoor control interventions as shown in the case of An. arabiensis in East Africa. This should not be neglected when modelling the efficacy or planning malaria control measures at the local/regional level.
Availability of data and materials
Data supporting the conclusions of this article are included within the article and its additional files. The datasets used and analyzed during the present study are available from the corresponding author upon reasonable request.
Abbreviations
- CNRFP:
-
Centre National de Recherche et de Formation sur le Paludisme
- EIR:
-
entomological inoculation rate
- HLC:
-
human landing catch
- LLIN:
-
long-lasting insecticide treated net
- SR:
-
sporozoite rate
References
WHO. World malaria report 2011. Geneva: World Health Organization; 2012.
Killeen GF, Smith TA. Exploring the contributions of bed nets, cattle, insecticides and excitorepellency to malaria control: a deterministic model of mosquito host-seeking behaviour and mortality. Trans R Soc Trop Med Hyg. 2007;101:867–80.
Hawley WA, Phillips-Howard PA, Nahlen BL, Alaii JA, Ter Kuile FO, Gimnig JE, et al. Community-wide effects of permethrin-treated bed nets on child mortality and malaria morbidity in western Kenya. Am J Trop Med Hyg. 2003;68:121–7.
WHO. World malaria report 2017. Geneva: World Health Organization; 2018.
Bhatt S, Weiss DJ, Cameron E, Bisanzio D, Mappin B, Dalrymple U, et al. The effect of malaria control on Plasmodium falciparum in Africa between 2000 and 2015. Nature. 2015;526:207–11.
Jagannathan P, Muhindo MK, Kakuru A, Arinaitwe E, Greenhouse B, Tappero J, et al. Increasing incidence of malaria in children despite insecticide-treated bed nets and prompt anti-malarial therapy in Tororo, Uganda. Malar J. 2012;11:435.
Roca-Feltrer A, Kwizombe CJ, Sanjoaquin MA, Sesay SSS, Faragher B, Harrison J, et al. Lack of decline in childhood malaria, Malawi, 2001–2010. Emerg Infect Dis. 2012;18:272–8.
Mwesigwa J, Okebe J, Affara M, Di Tanna GL, Nwakanma D, Janha O, et al. On-going malaria transmission in The Gambia despite high coverage of control interventions: a nationwide cross-sectional survey. Malar J. 2015;14:314.
CPS/SSDSPF I. Enquête Démographique et de Santé du Mali EDSM-V Rapport Préliminaire 2012–2013. Ministère de la Santé et des Affaires Sociales du Mali; 2014.
WHO. World malaria peport 2018. Geneva: World Health Organization; 2019.
Ranson H, N’Guessan R, Lines J, Moiroux N, Nkuni Z, Corbel V. Pyrethroid resistance in African anopheline mosquitoes: what are the implications for malaria control? Trends Parasitol. 2011;27:91–8.
Sokhna C, Ndiath MO, Rogier C. The changes in mosquito vector behaviour and the emerging resistance to insecticides will challenge the decline of malaria. Clin Microbiol Infect. 2013;19:902–7.
Namountougou M, Simard F, Baldet T, Diabaté A, Ouédraogo JB. Multiple insecticide resistance in Anopheles gambiae sl populations from Burkina Faso, West Africa. PLoS ONE. 2012;7:48412.
Silva APB, Santos JMM, Martins AJ. Mutations in the voltage-gated sodium channel gene of anophelines and their association with resistance to pyrethroids - a review. Parasit Vectors. 2014;7:450.
Killeen GF. Characterizing, controlling and eliminating residual malaria transmission. Malar J. 2014;13:330.
Killeen GF, Kiware SS, Okumu FO, Sinka ME, Moyes CL, Claire Massey N, et al. Going beyond personal protection against mosquito bites to eliminate malaria transmission: population suppression of malaria vectors that exploit both human and animal blood. BMJ Glob Health. 2017;2:e000198.
WHO. World malaria report 2015. Geneva: World Health Organization; 2015.
MoH - Burkina Faso. Annuaire Statistique Santé 2012. Ouagadougou: Conseil National de la Statistique, Burkina Faso; 2013. http://www.cns.bf/IMG/pdf/annuaire_ms_2012.pdf.
MoH - Burkina Faso. Annuaire serie longue de la santé, 1960–2009. Ouagadougou: Conseil National de la Statistique, Burkina Faso; 2011. http://www.cns.bf/IMG/pdf/dgiss_annuaire_serie_longue.pdf.
MoH - Burkina Faso. Annuaire Statistique Santé 2014. Ouagadougou: Conseil National de la Statistique, Burkina Faso; 2015. http://www.cns.bf/IMG/pdf/annuaire_2014_du_ms.pdf.
MoH - Burkina Faso. Annuaire Statistique Santé 2010. Ouagadougou: Conseil National de la Statistique, Burkina Faso; 2011. http://www.cns.bf/IMG/pdf/dgiss_annuaire_statistique_sante_2010.pdf.
MoH - Burkina Faso. Annuaire Statistique Santé 2013. Ouagadougou: Conseil National de la Statistique, Burkina Faso; 2014. http://www.cns.bf/IMG/pdf/annuaire_sante_2013.pdf.
MOH- Burkina Faso. Annuaire Statistique Santé 2011. Ouagadougou: Conseil National de la Statistique, Burkina Faso; 2012. http://www.cns.bf/IMG/pdf/dgiss_annuaire_ms_2011.pdf.
Pombi M, Calzetta M, Guelbeogo WM, Manica M, Perugini E, Pichler V, et al. Unexpectedly high Plasmodium sporozoite rate associated with low human blood index in Anopheles coluzzii from a LLIN-protected village in Burkina Faso. Sci Rep. 2018;8:12806.
Calzetta M, Perugini E, Seixas G, Sousa CA, Guelbeogo WM, Sagnon N, et al. A novel nested polymerase chain reaction assay targeting Plasmodium mitochondrial DNA in field-collected Anopheles mosquitoes. Med Vet Entomol. 2018;32:372–7.
Ouédraogo A, Tiono AB, Diarra A, Sanon S, Yaro JB, Ouedraogo E, et al. Malaria morbidity in high and seasonal malaria transmission area of Burkina Faso. PLoS ONE. 2013;8:e50036.
U.S. President’s Malaria Initiative. President’s Malaria Initiative Burkina Faso Malaria Operational Plan FY 2019. Arlington, USA: U.S. Agency for International Development; 2019. https://www.pmi.gov/docs/default-source/default-document-library/malaria-operational-plans/fy19/fy-2019-burkina-faso-malaria-operational-plan.pdf?sfvrsn=3.
Institut National de la Statistique et de la Démographie Ouagadougou BF, Programme National de Lutte contre le Paludisme Ouagadougou BF, ICF International Rockville, Maryland U. Enquête sur les Indicateurs du Paludisme (EIPBF) 2014. Ouagadougou: Institut National de la Statistique et de la Démographie; 2015. https://dhsprogram.com/pubs/pdf/MIS19/MIS19.pdf.
Sherrard-Smith E, Skarp JE, Beale AD, Fornadel C, Norris LC, Moore SJ, et al. Mosquito feeding behavior and how it influences residual malaria transmission across Africa. Proc Natl Acad Sci USA. 2019;116:15086–96.
Gillies MT, Coetzee M. A supplement to the Anophelinae of Africa south of the Sahara. Johannesburg: South African Institute of Medical Research; 1987.
Rider MA, Byrd BD, Keating J, Wesson DM, Caillouet KA. PCR detection of malaria parasites in desiccated Anopheles mosquitoes is uninhibited by storage time and temperature. Malar J. 2012;11:193.
Santolamazza F, Mancini E, Simard F, Qi Y, Tu Z, Della Torre A. Insertion polymorphisms of SINE200 retrotransposons within speciation islands of Anopheles gambiae molecular forms. Malar J. 2008;7:163.
Bass C, Nikou D, Blagborough AM, Vontas J, Sinden RE, Williamson MS, et al. PCR-based detection of Plasmodium in Anopheles mosquitoes: a comparison of a new high-throughput assay with existing methods. Malar J. 2008;7:177.
Bass C, Nikou D, Donnelly MJ, Williamson MS, Ranson H, Ball A, et al. Detection of knockdown resistance (kdr) mutations in Anopheles gambiae: a comparison of two new high-throughput assays with existing methods. Malar J. 2007;6:111.
Dabiré RK, Namountougou M, Diabaté A, Soma DD, Bado J, Toé HK, et al. Distribution and frequency of kdr mutations within Anopheles gambiae s.l. populations and first report of the Ace1.G119S mutation in Anopheles arabiensis from Burkina Faso (West Africa). PLoS ONE. 2014;9:e101484.
R Development Core Team. R: A language and enviroment for statistical computing. Vienna: R Foundation for Statistical Computing; 2018. https://www.R-project.org/.
Bates D, Maechler M, Bolker B, Walker S. lme4: linear mixed-effects models using S4 classes. R package version 1.1-6. R. 2014. https://www.jstatsoft.org/article/view/v067i01.
Traoré A, Badolo A, Guelbeogo MW, Sanou A, Viana M, Nelli L, et al. Anopheline species composition and the 1014F-genotype in different ecological settings of Burkina Faso in relation to malaria transmission. Malar J. 2019;18:165.
Doumbe-Belisse P, Ngadjeu CS, Sonhafouo-Chiana N, Talipouo A, Djamouko-Djonkam L, Kopya E, et al. High malaria transmission sustained by Anopheles gambiae s.l. occurring both indoors and outdoors in the city of Yaoundé, Cameroon. Wellcome Open Res. 2018;3:164.
Alout H, Ndam NT, Sandeu MM, Djégbe I, Chandre F, Dabiré RK, et al. Insecticide resistance alleles affect vector competence of Anopheles gambiae s.s. for Plasmodium falciparum field isolates. PLoS ONE. 2013;8:e63849.
Ndiath MO, Cailleau A, Diedhiou SM, Gaye A, Boudin C, Richard V, et al. Effects of the kdr resistance mutation on the susceptibility of wild Anopheles gambiae populations to Plasmodium falciparum: a hindrance for vector control. Malar J. 2014;13:340.
Kabula B, Tungu P, Rippon EJ, Steen K, Kisinza W, Magesa S, et al. A significant association between deltamethrin resistance, Plasmodium falciparum infection and the Vgsc-1014S resistance mutation in Anopheles gambiae highlights the epidemiological importance of resistance markers. Malar J. 2016;15:289.
Costantini C, Badolo A, Ilboudo-Sanogo E. Field evaluation of the efficacy and persistence of insect repellents DEET, IR3535, and KBR 3023 against Anopheles gambiae complex and other Afrotropical vector mosquitoes. Trans R Soc Trop Med Hyg. 2004;98:644–52.
Cuzin-Ouattara N, Van Den Broek AHA, Habluetzel A, Diabaté A, Sanogo-Ilboudo E, Diallo DA, et al. Wide-scale installation of insecticide-treated curtains confers high levels of protection against malaria transmission in a hyperendemic area of Burkina Faso. Trans R Soc Trop Med Hyg. 1999;93:473–9.
Ouédraogo AL, de Vlas SJ, Nébié I, Ilboudo-Sanogo E, Bousema JT, Ouattara AS, et al. Seasonal patterns of Plasmodium falciparum gametocyte prevalence and density in a rural population of Burkina Faso. Acta Trop. 2008;105:28–34.
Epopa PS, Collins CM, North A, Millogo AA, Benedict MQ, Tripet F, et al. Seasonal malaria vector and transmission dynamics in western Burkina Faso. Malar J. 2019;18:113.
Asante KP, Zandoh C, Dery DB, Brown C, Adjei G, Antwi-Dadzie Y, et al. Malaria epidemiology in the Ahafo area of Ghana. Malar J. 2011;10:211.
Ossè R, Aikpon R, Padonou GG, Oussou O, Yadouléton A, Akogbéto M. Evaluation of the efficacy of bendiocarb in indoor residual spraying against pyrethroid resistant malaria vectors in Benin: results of the third campaign. Parasit Vectors. 2012;5:163.
Atangana J, Bigoga JD, Patchoké S, Ndjemaï MNH, Tabue RN, Nem TE, et al. Anopheline fauna and malaria transmission in four ecologically distinct zones in Cameroon. Acta Trop. 2010;115:131–6.
Helinski M, Nuwa A, Protopopoff N, Feldman M, Ojuka P, Oguttu D, et al. Entomological surveillance following a long-lasting insecticidal net universal coverage campaign in midwestern Uganda. Parasit Vectors. 2015;8:458.
Mutuku FM, King CH, Mungai P, Mbogo C, Mwangangi J, Muchiri EM, et al. Impact of insecticide-treated bed nets on malaria transmission indices on the south coast of Kenya. Malar J. 2011;10:356.
Bayoh MN, Walker ED, Kosgei J, Ombok M, Olang GB, Githeko AK, et al. Persistently high estimates of late night, indoor exposure to malaria vectors despite high coverage of insecticide treated nets. Parasit Vectors. 2014;7:380.
Russell TL, Lwetoijera DW, Maliti D, Chipwaza B, Kihonda J, Charlwood JD, et al. Impact of promoting longer-lasting insecticide treatment of bed nets upon malaria transmission in a rural Tanzanian setting with pre-existing high coverage of untreated nets. Malar J. 2010;9:187.
Abraham M, Massebo F, Lindtjørn B. High entomological inoculation rate of malaria vectors in area of high coverage of interventions in southwest Ethiopia: implication for residual malaria transmission. Parasite Epidemiol Control. 2017;2:61–9.
Getawen SK, Ashine T, Massebo F, Woldeyes D, Lindtjørn B. Exploring the impact of house screening intervention on entomological indices and incidence of malaria in Arba Minch town, southwest Ethiopia: a randomized control trial. Acta Trop. 2018;181:84–94.
Owusu-Agyei S, Asante KP, Adjuik M, Adjei G, Awini E, Adams M, et al. Epidemiology of malaria in the forest-savannah transitional zone of Ghana. Malar J. 2009;8:220.
Tchouassi DP, Quakyi IA, Addison EA, Bosompem KM, Wilson MD, Appawu MA, et al. Characterization of malaria transmission by vector populations for improved interventions during the dry season in the Kpone-on-Sea area of coastal Ghana. Parasit Vectors. 2012;5:212.
Govoetchan R, Gnanguenon V, Azondékon R, Agossa RF, Sovi A, Oké-Agbo F, et al. Evidence for perennial malaria in rural and urban areas under the Sudanian climate of Kandi, northeastern Benin. Parasit Vectors. 2014;7:79.
Sovi A, Azondékon R, Aïkpon RY, Govoétchan R, Tokponnon F, Agossa F, et al. Impact of operational effectiveness of long-lasting insecticidal nets (LLINs) on malaria transmission in pyrethroid-resistant areas. Parasit Vectors. 2013;6:319.
Orlandi-Pradines E, Rogier C, Koffi B, Jarjaval F, Bell M, MacHault V, et al. Major variations in malaria exposure of travellers in rural areas: an entomological cohort study in western Côte d’Ivoire. Malar J. 2009;8:171.
Ouattara AF, Dagnogo M, Constant EA, Koné M, Raso G, Tanner M, et al. Transmission of malaria in relation to distribution and coverage of long-lasting insecticidal nets in central Côte d’Ivoire. Malar J. 2014;13:109.
Akono PN, Tonga C, Mbida JAM, Hondt OEN, Ambene PA, Ndo C, et al. Anopheles gambiae, major malaria vector in Logbessou, zone peri-urban area of Douala (Cameroon). Bull Soc Pathol Exot. 2015;108:360–8.
Tabue RN, Awono-Ambene P, Etang J, Atangana J, Antonio-Nkondjio C, Toto JC, et al. Role of Anopheles (Cellia) rufipes (Gough, 1910) and other local anophelines in human malaria transmission in the northern savannah of Cameroon: a cross-sectional survey. Parasit Vectors. 2017;10:22.
Merzagora L. Variazioni ecologiche ed epidemiologia della malaria in una zona di savana sudanese presso Ouagadougou, Burkina Faso. PhD Thesis, Università ‘La Sapienza’, Rome; 1993.
Costantini C. Behavioural studies on West African malaria vectors in the field. PhD Thesis, University of London, London; 1996.
Badolo A, Traore A, Jones CM, Sanou A, Flood L, Guelbeogo WM, et al. Three years of insecticide resistance monitoring in Anopheles gambiae in Burkina Faso: resistance on the rise? Malar J. 2012;11:232.
Sandeu MM, Moussiliou A, Moiroux N, Padonou GG, Massougbodji A, Corbel V, et al. Optimized pan-species and speciation duplex real-time PCR assays for Plasmodium parasites detection in malaria vectors. PLoS ONE. 2012;7:e52719.
Akogbéto MC, Salako AS, Dagnon F, Aïkpon R, Kouletio M, Sovi A, et al. Blood feeding behaviour comparison and contribution of Anopheles coluzzii and Anopheles gambiae, two sibling species living in sympatry, to malaria transmission in Alibori and Donga region, northern Benin, West Africa. Malar J. 2018;17:307.
Reddy MR, Overgaard HJ, Abaga S, Reddy VP, Caccone A, Kiszewski AE, et al. Outdoor host seeking behaviour of Anopheles gambiae mosquitoes following initiation of malaria vector control on Bioko Island, Equatorial Guinea. Malar J. 2011;10:184.
Hamon J, Choumara R, Adam D, Bailly H. Le paludisme dans la zone pilote de Bobo-Dioulasso, Haute-Volta. 3e partie. Cah. I’ORSTOM. 1959;1:63–98.
Molineaux L, Gramiccia G. Le projet Garki. Geneva: World Health Organization; 1980. https://apps.who.int/iris/bitstream/handle/10665/40347/9242560618.pdf?sequence=1&isAllowed=y.
Lemasson JJ, Fontenille D, Lochouarn L, Dia I, Simard F, Ba K, et al. Comparison of behavior and vector efficiency of Anopheles gambiae and Anopheles arabiensis (Diptera: Culicidae) in Barkedji, a Sahelian area of Senegal. J Med Entomol. 1997;34:396–403.
Quiñones ML, Lines JD, Thomson MC, Jawara M, Morris J, Greenwood BM. Anopheles gambiae gonotrophic cycle duration, biting and exiting behaviour unaffected by permethrin-impregnated bednets in The Gambia. Med Vet Entomol. 1997;11:71–8.
Carnevale P, Robert V, Manguin S, Corbel V, Fontenille D, Garros C, Rogier C. Les anophèles: biologie, transmission du Plasmodium et lutte antivectorielle. Marseille: IRD Editions; 2009.
Wanji S, Tanke T, Atanga SN, Ajonina C, Nicholas T, Fontenille D. Anopheles species of the Mount Cameroon region: biting habits, feeding behaviour and entomological inoculation rates. Trop Med Int Health. 2003;8:643–9.
Dabiré KR, Diabaté A, Paré-Toé L, Rouamba J, Ouari A, Fontenille D, et al. Year to year and seasonal variations in vector bionomics and malaria transmission in a humid savannah village in west Burkina Faso. J Vector Ecol. 2008;33:70–5.
Sinka ME, Bangs MJ, Manguin S, Coetzee M, Mbogo CM, Hemingway J, et al. The dominant Anopheles vectors of human malaria in Africa, Europe and the Middle East: occurrence data, distribution maps and bionomic précis. Parasit Vectors. 2010;3:117.
Tirados I, Costantini C, Gibson G, Torr SJ. Blood-feeding behaviour of the malarial mosquito Anopheles arabiensis: implications for vector control. Med Vet Entomol. 2006;20:425–37.
Torr SJ, Della Torre A, Calzetta M, Costantini C, Vale GA. Towards a fuller understanding of mosquito behaviour: use of electrocuting grids to compare the odour-orientated responses of Anopheles arabiensis and An quadriannulatus in the field. Med Vet Entomol. 2008;22:93–108.
Mendis C, Jacobsen JL, Gamage-Mendis A, Bule E, Dgedge M, Thompson R, et al. Anopheles arabiensis and Anopheles funestus are equally important vectors of malaria in Matola coastal suburb of Maputo, southern Mozambique. Med Vet Entomol. 2000;14:171–80.
Hamon J. Les moustiques anthropophiles de la région de Bobo-Dioulasso (République de Haute-Volta): cycles d’agressivité et variations saisonnières. Ann Soc Entomol Fr. 1963;132:85–144.
Gillies MT. Age-groups and the biting cycle in Anopheles gambiae. A preliminary investigation. Bull Entomol Res. 1957;48:553–9.
Dukeen MYH, Omer SM. Ecology of the malaria vector Anopheles arabiensis Patton (Diptera: Culicidae) by the Nile in northern Sudan. Bull Entomol Res. 1986;76:451–67.
Antonio-Nkondjio C, Awono-Ambene P, Toto JC, Meunier JY, Zebaze-Kemleu S, Nyambam R, et al. High malaria transmission intensity in a village close to Yaounde, the capital city of Cameroon. J Med Entomol. 2002;39:350–5.
Mattingly PF. Studies on West African forest mosquitos Part I The seasonal distribution, biting cycle and vertical distribution of four of the principal species. Bull Entomol Res. 1949;40:149–68.
Milali MP, Sikulu-Lord MT, Govella NJ. Bites before and after bedtime can carry a high risk of human malaria infection. Malar J. 2017;16:91.
Kenea O, Balkew M, Tekie H, Gebreichael T, Deressa W, Loha E, et al. Human-biting activities of Anopheles species in south-central Ethiopia. Parasit Vectors. 2016;9:527.
Hakizimana E, Karema C, Munyakanage D, Githure J, Mazarati JB, Tongren JE, et al. Spatio-temporal distribution of mosquitoes and risk of malaria infection in Rwanda. Acta Trop. 2018;182:149–57.
Mwesigwa J, Achan J, Di Tanna GL, Affara M, Jawara M, Worwui A, et al. Residual malaria transmission dynamics varies across The Gambia despite high coverage of control interventions. PLoS One. 2017;12:e0187059.
Ferreira CP, Lyra SP, Azevedo F, Greenhalgh D, Massad E. Modelling the impact of the long-term use of insecticide-treated bed nets on Anopheles mosquito biting time. Malar J. 2017;16:373.
Russell TL, Govella NJ, Azizi S, Drakeley CJ, Kachur SP, Killeen GF. Increased proportions of outdoor feeding among residual malaria vector populations following increased use of insecticide-treated nets in rural Tanzania. Malar J. 2011;10:80.
Doannio JMC, Dossou-Yovo J, Diarrassouba S, Chauvancy G, Darriet F, Chandre F, et al. Efficacité des moustiquaires pré-imprégnées de perméthrine Olyset Net en zone de résistance des vecteurs aux pyréthrinoïdes: 1. Evaluation entomologique. Med Trop. 1999;59:349–54.
Gu W, Novak RJ. Predicting the impact of insecticide-treated bed nets on malaria transmission: the devil is in the detail. Malar J. 2009;8:256.
Takken W. Do insecticide-treated bednets have an effect on malaria vectors? Trop Med Int Health. 2002;7:1022–30.
Killeen GF, Chitnis N, Moore SJ, Okumu FO. Target product profile choices for intra-domiciliary malaria vector control pesticide products: repel or kill? Malar J. 2011;10:207.
Mwangangi JM, Mbogo CM, Orindi BO, Muturi EJ, Midega JT, Nzovu J, et al. Shifts in malaria vector species composition and transmission dynamics along the Kenyan coast over the past 20 years. Malar J. 2013;12:13.
Kapesa A, Kweka EJ, Atieli H, Kamugisha E, Zhou G, Githeko AK, et al. Why some sites are responding better to anti-malarial interventions? A case study from western Kenya. Malar J. 2017;16:498.
Gatton ML, Chitnis N, Churcher T, Donnelly MJ, Ghani AC, Godfray HCJ, et al. The importance of mosquito behavioural adaptations to malaria control in Africa. Evolution. 2013;67:1218–30.
Derua YA, Alifrangis M, Hosea KM, Meyrowitsch DW, Magesa SM, Pedersen EM, et al. Change in composition of the Anopheles gambiae complex and its possible implications for the transmission of malaria and lymphatic filariasis in north-eastern Tanzania. Malar J. 2012;11:188.
Bayoh MN, Mathias DK, Odiere MR, Mutuku FM, Kamau L, Gimnig JE, et al. Anopheles gambiae: historical population decline associated with regional distribution of insecticide-treated bed nets in western Nyanza Province, Kenya. Malar J. 2010;9:62.
Costantini C, Ayala D, Guelbeogo WM, Pombi M, Some CY, Bassole IH, et al. Living at the edge: biogeographic patterns of habitat segregation conform to speciation by niche expansion in Anopheles gambiae. BMC Ecol. 2009;9:16.
Govella NJ, Chaki PP, Killeen GF. Entomological surveillance of behavioural resilience and resistance in residual malaria vector populations. Malar J. 2013;12:124.
Kamdem C, Tene Fossog B, Simard F, Etouna J, Ndo C, Kengne P, et al. Anthropogenic habitat disturbance and ecological divergence between incipient species of the malaria mosquito Anopheles gambiae. PLoS ONE. 2012;7:e39453.
Lehmann T, Diabate A. The molecular forms of Anopheles gambiae: a phenotypic perspective. Infect Genet Evol. 2008;8:737–46.
Gimonneau G, Pombi M, Choisy M, Morand S, Dabiré RK, Simard F. Larval habitat segregation between the molecular forms of the mosquito Anopheles gambiae in a rice field area of Burkina Faso, West Africa. Med Vet Entomol. 2012;26:9–17.
Gimonneau G, Pombi M, Dabiré RK, Diabaté A, Morand S, Simard F. Behavioural responses of Anopheles gambiae sensu stricto M and S molecular form larvae to an aquatic predator in Burkina Faso. Parasit Vectors. 2012;5:65.
Pombi M, Kengne P, Gimonneau G, Tene-Fossog B, Ayala D, Kamdem C, et al. Dissecting functional components of reproductive isolation among closely related sympatric species of the Anopheles gambiae complex. Evol Appl. 2017;10:1102–20.
Simard F, Ayala D, Kamdem GC, Pombi M, Etouna J, Ose K, et al. Ecological niche partitioning between Anopheles gambiae molecular forms in Cameroon: the ecological side of speciation. BMC Ecol. 2009;9:17.
Tene Fossog B, Ayala D, Acevedo P, Kengne P, Mebuy I, Makanga B, et al. Habitat segregation and ecological character displacement in cryptic African malaria mosquitoes. Evol Appl. 2015;8:326–45.
Lefèvre T, Gouagna LC, Dabiré KR, Elguero E, Fontenille D, Renaud F, et al. Beyond nature and nurture: phenotypic plasticity in blood-feeding behavior of Anopheles gambiae ss when humans are not readily accessible. Am J Trop Med Hyg. 2009;81:1023–9.
Acknowledgements
We thank the inhabitants of Goden village for their collaboration during the whole course of this study.
Funding
The study was supported by the EC FP7 Project grant no. 265660 “AvecNet” and by Sapienza University of Rome, projects “Avvio alla Ricerca 2019” No. AR11916B4CC76BF1 and “Progetti di Ricerca Medi” No. RM11916B7AFEA99E.
Author information
Authors and Affiliations
Contributions
WMG, HR, NS, AdT and MP conceived the study. WMG organized and supervised field collections. EP, MC, SM and VP carried out molecular analyses. EP, CV, BC and MP analysed the data. EP, HR, AdT and MP drafted the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The study has been conducted upon the ethical approval of the committee “Comité d’ethique pour la recherché en santé”, in agreement with Ministry of Health and Ministry of Research (approval n. 2013-7-057, issued on 11 July 2013). Volunteers chosen for mosquito samplings were local collaborators trained by CNRFP from several years in performing landing collections in the village. After the study, medical follow-up has been conducted on the volunteers for two weeks. None of them showed any malaria symptoms. In order to ensure empty houses during HLC, the inhabitants of those houses were moved to another safe place and rewarded for their time.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1.
: Table S1. Generalized linear mixed models built to evaluate the role of sampling conditions in explaining distributions of species abundance in study. In all models a negative binomial distribution has been chosen for the response variable, including time window, position and house as fixed effect and date as random effect. AIC: Akaike Information Criterion; d.f.: degrees of freedom; χ2: chi-square test value. Table S2. Summary of GLMM chosen for each species tested. Figure S1. Boxplots showing differences in abundances of Anopheles gambiae (s.l.), Anopheles arabiensis and Anopheles coluzzii according to the house and sampling position. Table S3. Changes in biting behaviour (time, exophagy and zoophagy), species dominance and sporozoite rate of mosquitoes of the A. gambiae species complex after LLIN/ITN introduction in sub-Saharan countries.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Perugini, E., Guelbeogo, W.M., Calzetta, M. et al. Behavioural plasticity of Anopheles coluzzii and Anopheles arabiensis undermines LLIN community protective effect in a Sudanese-savannah village in Burkina Faso. Parasites Vectors 13, 277 (2020). https://doi.org/10.1186/s13071-020-04142-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13071-020-04142-x