Abstract
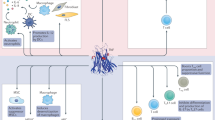
Resolution or persistence of the inflammatory response strictly reflects the dynamic balance between two major determinants: (1) the recruitment of circulating inflammatory cells together with the proliferation of resident cells and (2) the death, or apoptosis, of cells accumulated locally. The link between these two determinants seems to be represented by the incapacity of monocytes and macrophages to switch off activation of inflammation, thereby acting as a major promoter of the inappropriate recruitment, retention and survival of activated cells at inflamed tissue sites. Various pathways contribute to the persistent macrophage activation and, therefore, represent major rational targets for biologic approaches aimed at controlling the evolution of inflammation. These pathways include the continuous recruitment of Th1 cells into inflamed tissues, the subnormal production of anti-inflammatory IL-10 by regulatory T cells and macrophages, the reduced release of adenosine by endothelial cells and fibroblasts, the reduced production of soluble decoy receptors for TNF by macrophages and the reduced local availability of the anti-inflammatory cytokine IL-1 receptor antagonist. Moreover, the persistent activation and the survival of inflammatory cells strictly depends on the activity of the NF-κB system, which is responsible for inducing the synthesis of proinflammatory mediators in inflammatory cells such as monocytes, macrophages, fibroblasts and endothelial cells. It is of note that the activity of the NF-κB system can be inhibited by several drugs such as corticosteroids, leflunomide, cyclosporin A, tacrolimus, high concentrations of sulphasalazine and aspirin, and concentrations of oxaprozin achievable in vivo. Consequently, the possibility of controlling the NF-κB system pharmacologically raises opportunities for developing approaches to interfere with the transformation of transient to persistent inflammatory responses.
Similar content being viewed by others
REFERENCES
Arend, W. P. (2001). Cytokine imbalance in the pathogenesis of rheumatoid arthritis: the role of interleukin-1 receptor antagonist. Sem. Arthritis Rheum. 30, 1–6.
Baracchini, A., Minisola, G., Amicosante, G., et al. (2001). Oxaprozin: a NSAID able to inhibit the matrix metallo-proteinase activity, Inflammopharmacology 9, 143–146.
Bevilacqua, M. (2000). Pharmacology of oxaprozin: novel findings, in: Oxaprozin and the daily management of osteomuscolar impairment in arthritic patients, Highlights from the Satellite Symposium on Oxaprozin at the XIV EULAR Congress, pp. 3–6. Adis International, Milan, Italy.
Bevilacqua, M. (2002). Oxaprozin, a derivative of 2-arylpropionic acid, inhibits nuclear factor-kB at therapeuticallyrelevant concentrations, Ann. Rheum. Dis. 61 (Suppl. 1), p. 355, Abstract n. 18.
Choy, E. H. S. and Panayi, G. S. (2001). Cytokine pathways and joint inflammation in rheumatoid arthritis, New Engl. J. Med. 344, 907–916.
Coleman, J. W. (2001). Nitric oxide in immunity and inflammation, Int. Immunopharmacol. 1, 1397–1406.
Colville-Nash, P. R. and Gilroy, D. W. (2000). COX-2 and the cyclopentenone prostaglandins — a new chapter in the book of inflammation?, Prost. Lipid Mediators 62, 33–43.
Firestein, G. S. and Zvaifler, N. J. (2002). How important are T cells in chronic rheumatoid synovitis? Arthritis Rheum. 46, 298–308.
Gong J. H., Ratkay, L. G., Waterfield, D., et al. (1997). An antagonist of monocyte chemoattractant protein 1 (MCP-1) inhibits arthritis in the MRL-lpr mouse model, J. Exp. Med. 186, 131–137.
Israel, A. (2000). The IKK complex: an integrator of all signals that activate NF-kB, Trends Cell. Biol. 10, 129–133.
Kaiser, S. M. and Quinn, R. J. (1999). Adenosine receptors as potential therapeutic targets, Drug Discov. Today 4, 542–551.
Kinne, R. W., Brauer, R., Stuhlmuller, B., et al. (2000). Macrophages in rheumatoid arthritis, Arthritis Res. 2, 189–202.
Makarov, S. S. (2000). NF-·B as a therapeutic target in chronic inflammation: recent advances, Mol. Med. Today 6, 441–448.
McInnes, I. B. and Liew, F. Y. (1998). Interleukin 15: a proinflammatory role in rheumatoid arthritis synovitis, Immunol. Today 19, 75–79.
McInnes, I. B., Leung, B. P. and Liew, F. Y. (2000). Cell –cell interactions in synovitis. Interactions between T lymphocytes and synovial cells, Arthritis Res. 2, 374–378.
Mulherin, D., Fitzgerald, O. and Bresnihan, B. (1996). Synovial tissue macrophage populations and articular damage in rheumatoid arthritis, Arthritis Rheum. 39, 115–124.
Ottonello, L., Cutolo, M., Frumento, G., et al. (2002). Synovialfluid from patients with rheumatoid arthritis inhibits neutrophil apoptosis: role of adenosine and pro-inflammatory cytokines, Rheuma-tology (in press).
Pap, T., Muller-Ladner, U., Gay, R. E., et al. (2000). Role of synovial fibroblasts in the pathogenesis of rheumatoid arthritis, Arthritis Res. 2, 361–367.
Piomelli, D., Giuffrida, A., Calignano, A., et al. (2000). The cannabinoid system as a target for therapeutic drugs, Trends Pharmacol. Sci. 21, 218–224.
Ritchlin, C. (2000). Fibroblast biology. Effector signals released by synovial fibroblast in arthritis, Arthritis Res. 2, 356–360.
Tak, P. P. and Bresnihan, B. (2000). The pathogenesis and prevention of joint damage in rheumatoid arthritis, Arthritis Rheum. 43, 2619–2633.
Tak, P. P. and Firestein, G. S. (2001). NF-kB: a key role in in' ammatory diseases, J. Clin. Invest. 107, 7–11.
Taylor, P. C., Williams, R. O. and Maini, R. N. (2001). Immunotherapy for rheumatoid arthritis, Curr. Opin. Immunol. 13, 611–616.
Yamamoto, Y. and Gaynor, R. B. (2001). Therapeutic potential of inhibition of NF-kB pathway in the treatment of inflammation and cancer, J. Clin. Invest. 107, 135–141.
Rights and permissions
About this article
Cite this article
Dallegri, F., Ottonello, L. Pharmacological implications in the switch from acute to chronic inflammation. Inflammopharmacology 10, 159–171 (2002). https://doi.org/10.1163/156856002321168187
Issue Date:
DOI: https://doi.org/10.1163/156856002321168187