Abstract
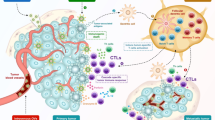
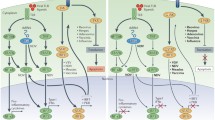
Preclinical studies demonstrate that a broad spectrum of human and animal malignant cells can be killed by oncolytic paramyxoviruses, which includes cells of ecto-, endo- and mesodermal origin. In clinical trials, significant reduction or even complete elimination of primary tumors and established metastases has been reported. Different routes of virus administration (intratumoral, intravenous, intradermal, intraperitoneal, or intrapleural) and single- vs. multiple-dose administration schemes have been explored. The reported side effects were grades 1 and 2, with the most common among them being mild fever. There are certain advantages in using paramyxoviruses as oncolytic agents compared to members of other virus families exist. Thanks to cytoplasmic replication, paramyxoviruses do not integrate the host genome or engage in recombination, which makes them safer and more attractive candidates for widely used therapeutic oncolysis than retroviruses or some DNA viruses. The list of oncolytic Paramyxoviridae members includes the attenuated measles virus, mumps virus, low pathogenic Newcastle disease, and Sendai viruses. Metastatic cancer cells frequently overexpress certain surface molecules that can serve as receptors for oncolytic paramyxoviruses. This promotes specific viral attachment to these malignant cells. Paramyxoviruses are capable of inducing efficient syncytium-mediated lysis of cancer cells and elicit strong immune stimulation, which dramatically enforces anticancer immune surveillance. In general, preclinical studies and phases I–III of clinical trials yield very encouraging results and warrant continued research of oncolytic paramyxoviruses as a particularly valuable addition to the existing panel of cancer-fighting approaches.
Similar content being viewed by others
Abbreviations
- PFU:
-
plaque-forming unit
- EID50 :
-
embryo infectious dose 50 (virus dilution that infects 50% of inoculated chicken embryos)
- CI:
-
confidence interval
References
Dock G. 1904. The influence of complicating diseases upon leukemia. Am. J. Med. Sci. 127, 563–592.
De Pace N. 1912. Sulla scomparsa di un enorme cancro vegetante del collo dell’utero senza cura chirurgica. Ginecologia. 9, 82–89.
Levaditi C., Nicolau S. 1923. Vaccine et neoplasmes Ann. Inst. Pasteur. 37, 443–447.
Farber S., Diamond L.K. 1948. Temporary remissions in acute leukemia in children produced by folic acid antagonist, 4-aminopteroyl-glutamic acid. N. Engl. J. Med. 238, 787–793.
Svejda J. 1950. Viruses and tumors. Lek. Listy. 5, 688–689.
Moore A.E. 1954. Effects of viruses on tumors. Annu. Rev. Microbiol. 8, 393–410.
Kelly E., Russell S.J. 2007. History of oncolytic viruses: Genesis to genetic engineering. Mol. Ther. 15, 651–659.
Netesov S.V., Kochneva G.V., Svyatchenko V.A., et al. 2011. Oncolytic viruses: Achievements and problems. Epidemiol. Sanit. (Moscow). 13, 10–17.
Kochneva G.V., Sivolobova G.F., Yudina K.V., et al. 2012. Oncolytic poxviruses. Mol. Genet. Microbiol. Virol. (Moscow). 27 (1), 7–15.
Loktev V.B., Ivankina T.Yu., Netesov S.V., Chumakov P.M. 2012. Oncolytic parvoviruses. New approaches to the treatment of cancer. Bull. Russ. Acad. Med. Sci. 67, 42–47.
Svyatchenko V.A., Tarasova M.V., Netesov S.V., Chumakov P.M. 2012. Oncolytic adenoviruses in anticancer therapy: Current status and prospects. Mol. Biol. (Moscow). 46, 496–507.
Breitbach C.J., Lichty B.D., Bell J.C. 2016. Oncolytic viruses: Therapeutics with an identity crisis. EBioMedicine. 9, 31–36.
Fukuhara H., Ino Y., Todo T. 2016. Oncolytic virus therapy: A new era of cancer treatment at dawn. Cancer Sci. 107, 1373–1379.
Karapanagiotou E.M., Roulstone V., Twigger K., et al. 2012. Phase I/II trial of carboplatin and paclitaxel chemotherapy in combination with intravenous oncolytic reovirus in patients with advanced malignancies. Clin. Cancer Res. 18, 2080–2089.
Heo J., Reid T., Ruo L., et al. 2013. Randomized dosefinding clinical trial of oncolytic immunotherapeutic vaccinia JX-594 in liver cancer. Nat. Med. 19, 329–336.
Dolgin E. 2015. Oncolytic viruses get a boost with first FDA-approval recommendation. Nat. Rev. Drug Discov. 14, 369–371.
Donina S., Strele I., Proboka G., et al. 2015. Adapted ECHO-7 virus Rigvir immunotherapy (oncolytic virotherapy) prolongs survival in melanoma patients after surgical excision of the tumour in a retrospective study. Melanoma Res. 25, 421–426.
Takaoka A., Hayakawa S., Yanai H., et al. 2003. Integration of interferon-alpha/beta signalling to p53 responses in tumour suppression and antiviral defence. Nature. 424, 516–523.
Tanaka N., Ishihara M., Lamphier M.S., et al. 1996. Cooperation of the tumour suppressors IRF-1 and p53 in response to DNA damage. Nature. 382, 816–818.
Moiseeva O., Mallette F.A., Mukhopadhyay U.K., et al. 2006. DNA damage signaling and p53-dependent senescence after prolonged beta-interferon stimulation. Mol. Biol. Cell. 17, 1583–1592.
Haus O. 2000. The genes of interferons and interferonrelated factors: Localization and relationships with chromosome aberrations in cancer. Arch. Immunol. Ther. Exp. 48, 95–100.
Mansour M., Palese P., Zamarin D. 2011. Oncolytic specificity of Newcastle disease virus is mediated by selectivity for apoptosis-resistant cells. J. Virol. 85, 6015–6023.
Boisgerault N., Tangy F., Gregoire M. 2010. New perspectives in cancer virotherapy: Bringing the immune system into play. Immunotherapy. 2, 185–199.
Prestwich R.J., Errington F., Diaz R.M., et al. 2009. The case of oncolytic viruses versus the immune system: Waiting on the judgment of Solomon. Hum. Gene Ther. 20, 1119–1132.
Donnelly O.G., Errington-Mais F., Steele L., et al. 2011. Measles virus causes immunogenic cell death in human melanoma. Gene Ther. 20, 7–15.
Bartlett D.L., Liu Z., Sathaiah M., et al. 2013. Oncolytic viruses as therapeutic cancer vaccines. Mol. Cancer. 12, 103.
Yu Y.A., Shabahang S., Timiryasova T.M., et al. 2004. Visualization of tumors and metastases in live animals with bacteria and vaccinia virus encoding light-emitting proteins. Nat. Biotechnol. 22, 313–320.
Lemay C.G., Rintoul J.L., Kus A., et al. 2012. Harnessing oncolytic virus-mediated antitumor immunity in an infected cell vaccine. Mol. Ther. 20, 1791–1799.
Sze D.Y., Reid T.R., Rose S.C. 2013. Oncolytic virotherapy. J. Vasc. Interv. Radiol. 24, 1115–1122.
Tai L.H., Zhang J., Scott K.J., et al. 2013. Perioperative influenza vaccination reduces postoperative metastatic disease by reversing surgery-induced dysfunction in natural killer cells. Clin. Cancer Res. 19, 5104–5115.
Matveeva O.V., Guo Z.S., Shabalina S.A., Chumakov P.M. 2015. Oncolysis by paramyxoviruses: multiple mechanisms contribute to therapeutic efficiency. Mol. Ther. Oncolytics. 2, 15011.
Enders G. 1996. Paramyxoviruses. Galveston: Univ. Texas Med. Branch.
Bossart K.N., Fusco D.L., Broder C.C. 2013. Paramyxovirus entry. Adv. Exp. Med. Biol. 790, 95–127.
Matrosovich M., Herrler G., Klenk H.D. 2013. Sialic acid receptors of viruses. Top. Curr. Chem. 7, 73.
Bull C., den Brok M.H., Adema G.J. 2014. Sweet escape: Sialic acids in tumor immune evasion. Biochim. Biophys. Acta. 1846, 238–246.
Bull C., Stoel M.A., den Brok M.H., Adema G.J. 2014. Sialic acids sweeten a tumor’s life. Cancer Res. 74, 3199–3204.
Kawaguchi Y., Miyamoto Y., Inoue T., Kaneda Y. 2009. Efficient eradication of hormone-resistant human prostate cancers by inactivated Sendai virus particle. Int. J. Cancer. 124, 2478–2487.
Villar E., Barroso I.M. 2006. Role of sialic acid-containing molecules in paramyxovirus entry into the host cell: a minireview. Glycoconj. J. 23, 5–17.
Anderson B.D., Nakamura T., Russell S.J., Peng K.W. 2004. High CD46 receptor density determines preferential killing of tumor cells by oncolytic measles virus. Cancer Res. 64, 4919–4926.
Surowiak P., Materna V., Maciejczyk A., et al. 2006. CD46 expression is indicative of shorter revival-free survival for ovarian cancer patients. Anticancer Res. 26, 4943–4948.
Maciejczyk A., Szelachowska J., Szynglarewicz B., et al. 2011. CD46 expression is an unfavorable prognostic factor in breast cancer cases. Appl. Immunohistochem. Mol. Morphol. 19, 540–546.
Noyce R.S., Bondre D.G., Ha M.N., et al. 2011. Tumor cell marker PVRL4 (nectin 4) is an epithelial cell receptor for measles virus. PLoS Pathog. 7, e1002240.
Noyce R.S., Richardson C.D. 2012. Nectin 4 is the epithelial cell receptor for measles virus. Trends Microbiol. 20, 429–439.
Fabre-Lafay S., Garrido-Urbani S., Reymond N., et al. 2005. Nectin-4, a new serological breast cancer marker, is a substrate for tumor necrosis factor-alphaconverting enzyme (TACE)/ADAM-17. J. Biol. Chem. 280, 19543–19550.
Derycke M.S., Pambuccian S.E., Gilks C.B., et al. 2010. Nectin 4 overexpression in ovarian cancer tissues and serum: Potential role as a serum biomarker. Am. J. Clin. Pathol. 134, 835–845.
Takano A., Ishikawa N., Nishino R., et al. 2009. Identification of nectin-4 oncoprotein as a diagnostic and therapeutic target for lung cancer. Cancer Res. 69, 6694–6703.
Myers R., Greiner S., Harvey M., et al. 2005. Oncolytic activities of approved mumps and measles vaccines for therapy of ovarian cancer. Cancer Gene Ther. 12, 593–599.
Fabre-Lafay S., Monville F., Garrido-Urbani S., et al. 2007. Nectin-4 is a new histological and serological tumor associated marker for breast cancer. BMC Cancer. 7, 73.
Kingsbury D.W. 1991. The Paramyxoviruses. New York: Plenum.
Cohen M., Elkabets M., Perlmutter M., et al. 2010. Sialylation of 3-methylcholanthrene-induced fibrosarcoma determines antitumor immune responses during immunoediting. J. Immunol. 185, 5869–5878.
Powell L.D., Whiteheart S.W., Hart G.W. 1987. Cell surface sialic acid influences tumor cell recognition in the mixed lymphocyte reaction. J. Immunol. 139, 262–270.
Galanis E. 2010. Therapeutic potential of oncolytic measles virus: Promises and challenges. Clin. Pharmacol. Ther. 88, 620–625.
Iwata S., Schmidt A.C., Titani K., et al. 1994. Assignment of disulfide bridges in the fusion glycoprotein of Sendai virus. J. Virol. 68, 3200–3206.
Tashiro M., Yokogoshi Y., Tobita K., et al. 1992. Tryptase Clara, an activating protease for Sendai virus in rat lungs, is involved in pneumopathogenicity. J. Virol. 66, 7211–7216.
Sakai K., Kohri T., Tashiro M., et al. 1994. Sendai virus infection changes the subcellular localization of tryptase Clara in rat bronchiolar epithelial cells. Eur. Respir. J. 7, 686–692.
Sakai K., Kawaguchi Y., Kishino Y., Kido H. 1993. Electron immunohistochemical localization in rat bronchiolar epithelial cells of tryptase Clara, which determines the pneumotropism and pathogenicity of Sendai virus and influenza virus. J. Hostochem. Cytochem. 41 (1), 89–93.
Nagai Y. 1995. Virus activation by host proteinases. A pivotal role in the spread of infection, tissue tropism and pathogenicity. Microbiol. Immunol. 39, 1–9.
Kido H., Beppu Y., Sakai K., Towatari T. 1997. Molecular basis of proteolytic activation of Sendai virus infection and the defensive compounds for infection. Biol. Chem. 378, 255–263.
Choi S., Bertram S., Glowacka I., et al. 2009. Type II transmembrane serine proteases in cancer and viral infections. Trends Mol. Med. 15, 303–312.
Abe M., Tahara M., Sakai K., et al. 2013. TMPRSS2 Is an activating protease for respiratory parainfluenza viruses. J. Virol. 87, 11930–11935.
Bertram S., Glowacka I., Blazejewska P., et al. 2010. TMPRSS2 and TMPRSS4 facilitate trypsin-independent spread of influenza virus in Caco-2 cells. J. Virol. 84, 10016–10025.
Bateman A., Bullough F., Murphy S., et al. 2000. Fusogenic membrane glycoproteins as a novel class of genes for the local and immune-mediated control of tumor growth. Cancer Res. 60, 1492–1497.
Bateman A.R., Harrington K.J., Kottke T., et al. 2002. Viral fusogenic membrane glycoproteins kill solid tumor cells by nonapoptotic mechanisms that promote cross presentation of tumor antigens by dendritic cells. Cancer Res. 62, 6566–6578.
Lin E., Salon C., Brambilla E., et al. 2010. Fusogenic membrane glycoproteins induce syncytia formation and death in vitro and in vivo: A potential therapy agent for lung cancer. Cancer Gene Ther. 17, 256–265
Delpeut S., Rudd P.A., Labonte P., von Messling V. 2012. Membrane fusion-mediated autophagy induction enhances morbillivirus cell-to-cell spread. J. Virol. 86, 8527–8535.
Kurooka M., Kaneda Y. 2007. Inactivated Sendai virus particles eradicate tumors by inducing immune responses through blocking regulatory T cells. Cancer Res. 67, 227–236.
Fujihara A., Kurooka M., Miki T., Kaneda Y. 2008. Intratumoral injection of inactivated Sendai virus particles elicits strong antitumor activity by enhancing local CXCL10 expression and systemic NK cell activation. Cancer Immunol. Immunother. 57, 73–84.
Senin V., Senina A., Matveeva O. 2014. RF Patent No. 2519763.
Matveeva O.V., Guo Z.S., Senin V.M., et al. 2015. Oncolysis by paramyxoviruses: Preclinical and clinical studies. Mol. Ther. Oncolytics. 2, 15017.
Cassel W.A., Murray D.R. 1992. A ten-year follow-up on stage II malignant melanoma patients treated postsurgically with Newcastle disease virus oncolysate. Med. Oncol. Tumor Pharmacother. 9, 169–171.
Batliwalla F.M., Bateman B.A., Serrano D., et al. 1998. A 15-year follow-up of AJCC stage III malignant melanoma patients treated postsurgically with Newcastle disease virus (NDV) oncolysate and determination of alterations in the CD8 T cell repertoire. Mol. Med. 4, 783–794.
Csatary L.K., Eckhardt S., Bukosza I., Czegledi F., Fenyvesi C., Gergely P., Bodey B., Csatary C.M. 1993. Attenuated veterinary virus vaccine for the treatment of cancer. Cancer Detect. Prev. 17, 619–627.
Csatary L.K., Gosztonyi G., Szeberenyi J., Fabian Z., Liszka V., Bodey B., Csatary C.M. 2004. MTH-68/H oncolytic viral treatment in human high-grade gliomas. J. Neurooncol. 67, 83–93.
Freeman A.I., Zakay-Rones Z., Gomori J.M., et al. 2006. Phase I/II trial of intravenous NDV-HUJ oncolytic virus in recurrent glioblastoma multiforme. Mol. Ther. 13, 221–228.
Pecora A.L., Rizvi N., Cohen G.I., et al. 2002. Phase I trial of intravenous administration of PV701, an oncolytic virus, in patients with advanced solid cancers. J. Clin. Oncol. 20, 2251–2266.
Laurie S.A., Bell J.C., Atkins H.L., et al. 2006. A phase 1 clinical study of intravenous administration of PV701, an oncolytic virus, using two-step desensitization. Clin. Cancer Res. 12, 2555–2562.
Lorence R.M., Roberts M.S., O’Neil J.D., et al. 2007. Phase 1 clinical experience using intravenous administration of PV701, an oncolytic Newcastle disease virus. Curr. Cancer Drug Targets. 7, 157–167.
Hotte S.J., Lorence R.M., Hirte H.W., et al. 2007. An optimized clinical regimen for the oncolytic virus PV701. Clin. Cancer Res. 13, 977–985.
Steiner H.H., Bonsanto M.M., Beckhove P., et al. 2004. Antitumor vaccination of patients with glioblastoma multiforme: A pilot study to assess feasibility, safety, and clinical benefit. J. Clin. Oncol. 22, 4272–4281.
Karcher J., Dyckhoff G., Beckhove P., et al. 2004. Antitumor vaccination in patients with head and neck squamous cell carcinomas with autologous virusmodified tumor cells. Cancer Res. 64, 8057–8061.
Herold-Mende C., Karcher J., Dyckhoff G., Schirrmacher V. 2005. Antitumor immunization of head and neck squamous cell carcinoma patients with a virusmodified autologous tumor cell vaccine. Adv. Otorhinolaryngol. 62, 173–183.
Schulze T., Kemmner W., Weitz J., et al. 2009. Efficiency of adjuvant active specific immunization with Newcastle disease virus modified tumor cells in colorectal cancer patients following resection of liver metastases: Results of a prospective randomized trial. Cancer Immunol. Immunother. 58, 61–69.
Keshelava V.B. 2007. Newcastle disease oncolytic virus and autologous tumor cells in complex cancer therapy. Epidemiol. Vaktsinoprofilakt. 3, 23–28.
Keshelava V.V., Dobrovolskaya N.Y., Podolskaya M.V., Gardarnik T.V. 2009. Organ-preserving treatment of breast cancer with the use of oncolytic Newcastle disease virus. Vestn. Ross. Nauch. Tsentra Rentgenoradiol. 9, 6.
Keshelava V.V., Dobrovolskaya N.Y., Stavitsky R.V., Podolskaya M.V. 2010. Efficacy of the integrated treatment of cervical cancer using the Newcastle disease virus. Radiology–Practice. 15, 38–45.
Heinzerling L., Kunzi V., Oberholzer P.A., et al. 2005. Oncolytic measles virus in cutaneous T-cell lymphomas mounts antitumor immune responses in vivo and targets interferon-resistant tumor cells. Blood. 106, 2287–2294.
Galanis E., Hartmann L.C., Cliby W.A., et al. 2010. Phase I trial of intraperitoneal administration of an oncolytic measles virus strain engineered to express carcinoembryonic antigen for recurrent ovarian cancer. Cancer Res. 70, 875–882.
Russell S.J., Federspiel M.J., Peng K.W., et al. 2014. Remission of disseminated cancer after systemic oncolytic virotherapy. Mayo Clin. Proc. 89, 926–933.
Galanis E., Atherton P.J., Maurer M.J., et al. 2015. Oncolytic measles virus expressing the sodium iodide symporter to treat drug-resistant ovarian cancer. Cancer Res. 75, 22–30.
Asada T. 1974. Treatment of human cancer with mumps virus. Cancer. 34, 1907–1928.
Okuno Y., Asada T., Yamanishi K., et al. 1978. Studies on the use of mumps virus for treatment of human cancer. Biken J. 21, 37–49.
Shimizu Y., Hasumi K., Okudaira Y., et al. 1988. Immunotherapy of advanced gynecologic cancer patients utilizing mumps virus. Cancer Detect. Prev. 12, 487–495.
Emmerson P.T. 1999. Newcastle disease virus (Paramyxoviridae). In: Encyclopedia of Virology. Oxford: Elsevier, pp. 1020–1026.
Swayne D.E., King D.J. 2003. Avian influenza and Newcastle disease. J. Am. Vet. Med. Assoc. 222, 1534–1540.
Flanagan A.D., Love R., Tesar W. 1955. Propagation of Newcastle disease virus in Ehrlich ascites cells in vitro and in vivo. Proc. Soc. Exp. Biol. Med. 90, 82–86.
Lech P.J., Russell S.J. 2010. Use of attenuated paramyxoviruses for cancer therapy. Expert Rev. Vaccines. 9, 1275–1302.
Fournier P., Bian H., Szeberenyi J., Schirrmacher V. 2012. Analysis of three properties of Newcastle disease virus for fighting cancer: Tumor-selective replication, antitumor cytotoxicity, and immunostimulation. Meth. Mol. Biol. 797, 177–204.
Zamarin D., Palese P. 2012. Oncolytic Newcastle disease virus for cancer therapy: Old challenges and new directions. Future Microbiol. 7, 347–367.
Lam H.Y., Yeap S.K., Rasoli M., et al. 2011. Safety and clinical usage of newcastle disease virus in cancer therapy. J. Biomed. Biotechnol. 718710, 26.
Reichard K.W., Lorence R.M., Cascino C.J., et al. 1992. Newcastle disease virus selectively kills human tumor cells. J. Surg. Res. 52, 448–453.
Fiola C., Peeters B., Fournier P., et al. 2006. Tumor selective replication of Newcastle disease virus: Association with defects of tumor cells in antiviral defence. Int. J. Cancer. 119, 328–338.
Fabian Z., Csatary C.M., Szeberenyi J., Csatary L.K. 2007. p53-independent endoplasmic reticulum stressmediated cytotoxicity of a Newcastle disease virus strain in tumor cell lines. J. Virol. 81, 2817–2830.
Schirrmacher V., Haas C., Bonifer R., et al. 1999. Human tumor cell modification by virus infection: An efficient and safe way to produce cancer vaccine with pleiotropic immune stimulatory properties when using Newcastle disease virus. Gene Ther. 6, 63–73.
Zamarin D., Martinez-Sobrido L., Kelly K., et al. 2009. Enhancement of oncolytic properties of recombinant newcastle disease virus through antagonism of cellular innate immune responses. Mol. Ther. 17, 697–706.
Fabian Z., Torocsik B., Kiss K., et al. 2001. Induction of apoptosis by a Newcastle disease virus vaccine (MTH-68/H) in PC12 rat phaeochromocytoma cells. Anticancer Res. 21, 125–135.
Szeberenyi J., Fabian Z., Torocsik B., et al. 2003. Newcastle disease virus-induced apoptosis in PC12 pheochromocytoma cells. Am. J. Ther. 10, 282–288.
Tzadok-David Y., Metzkin-Eizenberg M., Zakay-Rones Z. 1995. The effect of a mesogenic and a lentogenic Newcastle disease virus strain on Burkitt lymphoma Daudi cells. J. Cancer Res. Clin. Oncol. 121, 169–174.
Bar-Eli N., Giloh H., Schlesinger M., Zakay-Rones Z. 1996. Preferential cytotoxic effect of Newcastle disease virus on lymphoma cells. J. Cancer Res. Clin. Oncol. 122, 409–415.
Song K.Y., Wong J., Gonzalez L., et al. 2010. Antitumor efficacy of viral therapy using genetically engineered Newcastle disease virus [NDV(F3aa)-GFP] for peritoneally disseminated gastric cancer. J. Mol. Med. 88, 589–596.
Lorence R.M., Reichard K.W., Katubig B.B., et al. 1994. Complete regression of human neuroblastoma xenografts in athymic mice after local Newcastle disease virus therapy. J. Natl. Cancer Inst. 86, 1228–1233.
Lorence R.M., Katubig B.B., Reichard K.W., et al. 1994. Complete regression of human fibrosarcoma xenografts after local Newcastle disease virus therapy. Cancer Res. 54, 6017–6021.
Phuangsab A., Lorence R.M., Reichard K.W., et al. 2001. Newcastle disease virus therapy of human tumor xenografts: Antitumor effects of local or systemic administration. Cancer Lett. 172, 27–36.
Vigil A., Park M.S., Martinez O., et al. 2007. Use of reverse genetics to enhance the oncolytic properties of Newcastle disease virus. Cancer Res. 67, 8285–8292.
Altomonte J., Marozin S., Schmid R.M., Ebert O. 2010. Engineered newcastle disease virus as an improved oncolytic agent against hepatocellular carcinoma. Mol. Ther. 18, 275–284.
Schirrmacher V., Fournier P. 2009. Newcastle disease virus: A promising vector for viral therapy, immune therapy, and gene therapy of cancer. Meth. Mol. Biol. 542, 565–605.
Schirrmacher V., Griesbach A., Ahlert T. 2001. Antitumor effects of Newcastle disease virus in vivo: Local versus systemic effects. Int. J. Oncol. 18, 945–952.
Lorence R.M., Pecora A.L., Major P.P., et al. 2003. Overview of phase I studies of intravenous administration of PV701, an oncolytic virus. Curr. Opin. Mol. Ther. 5, 618–624.
Keshelava V.B. 2014. Cancer: Realities and possibilities of application of the Newcastle disease virus. In: Virotherapy: Rationale, Criteria, Indications of Use, Effectiveness. Saarbrücken, Germany: Palmarum Acad.
Keshelava V.B. 2010. Results of a study of the oncolytic Newcastle disease virus in neoadjuvant therapy for breast cancer over a 3-year follow-up period. Vestn. Ross. Nauch. Tsentra Rentgenoradiol. 10, Article ID 04210000150421000022.
Nakamura T., Russell S.J. 2004. Oncolytic measles viruses for cancer therapy. Expert Opin. Biol. Ther. 4, 1685–1692.
Blechacz B., Russell S.J. 2008. Measles virus as an oncolytic vector platform. Curr. Gene Ther. 8, 162–175.
Allen C., Opyrchal M., Aderca I., et al. 2012. Oncolytic measles virus strains have significant antitumor activity against glioma stem cells. Gene Ther. 20, 444–449.
Enders J.F., Katz S.L., Milovanovic M.V., Holloway A. 1960. Studies on an attenuated measles-virus vaccine: 1. Development and preparations of the vaccine: Technics for assay of effects of vaccination. N. Engl. J. Med. 263, 153–159.
Grote D., Russell S.J., Cornu T.I., et al. 2001. Live attenuated measles virus induces regression of human lymphoma xenografts in immunodeficient mice. Blood. 97, 3746–3754.
Dingli D., Peng K.W., Harvey M.E., et al. 2004. Image-guided radiovirotherapy for multiple myeloma using a recombinant measles virus expressing the thyroidal sodium iodide symporter. Blood. 103, 1641–1646.
Studebaker A.W., Kreofsky C.R., Pierson C.R., et al. 2010. Treatment of medulloblastoma with a modified measles virus. Neuro Oncol. 12, 1034–1042.
Phuong L.K., Allen C., Peng K.W., et al. 2003. Use of a vaccine strain of measles virus genetically engineered to produce carcinoembryonic antigen as a novel therapeutic agent against glioblastoma multiforme. Cancer Res. 63, 2462–2469.
Blechacz B., Splinter P.L., Greiner S., et al. 2006. Engineered measles virus as a novel oncolytic viral therapy system for hepatocellular carcinoma. Hepatology. 44, 1465–1477.
Msaouel P., Iankov I.D., Allen C., et al. 2009. Noninvasive imaging and radiovirotherapy of prostate cancer using an oncolytic measles virus expressing the sodium iodide symporter. Mol. Ther. 17, 2041–2048.
McDonald C.J., Erlichman C., Ingle J.N., et al. 2006. A measles virus vaccine strain derivative as a novel oncolytic agent against breast cancer. Breast Cancer Res. Treat. 99, 177–184.
Iankov I.D., Msaouel P., Allen C., et al. 2010. Demonstration of anti-tumor activity of oncolytic measles virus strains in a malignant pleural effusion breast cancer model. Breast Cancer Res. Treat. 122, 745–754.
Peng K.W., Hadac E.M., Anderson B.D., et al. 2006. Pharmacokinetics of oncolytic measles virotherapy: Eventual equilibrium between virus and tumor in an ovarian cancer xenograft model. Cancer Gene Ther. 13, 732–738.
Guillerme G., Tangy M., Fonteneau F. 2013. Antitumor virotherapy by attenuated measles virus. Biology. 2, 587–602.
Msaouel P., Dispenzieri A., Galanis E. 2009. Clinical testing of engineered oncolytic measles virus strains in the treatment of cancer: an overview. Curr. Opin. Mol. Ther. 11, 43–53.
Institute of Laboratory Animal Resources, U.S. Committee on Infectious Diseases of Mice and Rats. 1991. Infectious Diseases of Mice and Rats. Washington, DC: Natl. Acad. Press.
Inoue M., Tokusumi Y., Ban H., et al. 2003. A new Sendai virus vector deficient in the matrix gene does not form virus particles and shows extensive cell-tocell spreading. J. Virol. 77, 6419–6429.
Yonemitsu Y., Ueda Y., Kinoh H., Hasegawa M. 2008. Immunostimulatory virotherapy using recombinant Sendai virus as a new cancer therapeutic regimen. Front. Biosci. 13, 1892–1898.
Iwadate Y., Inoue M., Saegusa T., et al. 2005. Recombinant Sendai virus vector induces complete remission of established brain tumors through efficient interleukin-2 gene transfer in vaccinated rats. Clin. Cancer Res. 11, 3821–3827.
Matveeva O.V., Kochneva G.V., Netesov S.V. et al. 2015. Mechanisms of oncolysis by paramyxovirus Sendai. Acta Naturae 7 (2), 6–17.
Tanemura A., Kiyohara E., Katayama I., Kaneda Y. 2013. Recent advances and developments in the antitumor effect of the HVJ envelope vector on malignant melanoma: from the bench to clinical application. Cancer Gene Ther. 20, 599–605.
Slobod K.S., Shenep J.L., Lujan-Zilbermann J., et al. 2004. Safety and immunogenicity of intranasal murine parainfluenza virus type 1 (Sendai virus) in healthy human adults. Vaccine. 22, 3182–3186.
Author information
Authors and Affiliations
Corresponding author
Additional information
Original Russian Text © O.V. Matveeva, G.V. Kochneva, S.S. Zainutdinov, G.V. Ilyinskaya, P.M. Chumakov, 2018, published in Molekulyarnaya Biologiya, 2018, Vol. 52, No. 3, pp. 360–379.
Rights and permissions
About this article
Cite this article
Matveeva, O.V., Kochneva, G.V., Zainutdinov, S.S. et al. Oncolytic Paramyxoviruses: Mechanism of Action, Preclinical and Clinical Studies. Mol Biol 52, 306–322 (2018). https://doi.org/10.1134/S002689331803010X
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S002689331803010X