Abstract
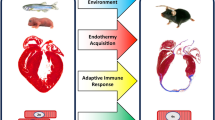
The review addresses the mechanisms of adaptation of the myocardium and cells of the cardiovascular system to hypoxia and ischemia as well as biochemical mechanisms of cardioprotection in animals of different phylogenetic levels. A special focus is placed on general adaptive strategies developed by evolutionarily distant animals in response to hypoxia and ischemia and on preconditioning and myocardial hibernation phenomena.
Similar content being viewed by others
References
Ferrari, R., Ceconi, C., Curello, S., Cargnoni, A., Alfieri, O., Pardini, A., Marzollo, P., and Visioli, O., Oxygen free radicals and myocardial damage: protective role ofthiol-containing agents, Am. J. Med., 1991, vol. 91, pp. S95–S105.
Dolzhenko, M.N., To the question of the expediency of metabolic cardioprotection in the era of evidence-based medicine, ML, 2012, nos. 2–3 (88–89), pp. 1–8.
Spath, N.B., Mills, N.L., and Cruden, N.L., Novel cardioprotective and regenerative therapies in acute myocardial infarction: a review of recent and ongoing clinical trials, Future Cardiol., 2016, vol. 12, pp. 655–672.
Agadzhanyan, N.A., Polunin, I.N., Stepanov, V.K., and Polyakov, V.N., Chelovek v usloviyakh gipokapnii i giperkapnii (A Man under Hypocapnic and Hypercapnic Conditions), Astrakhan, Moscow, 2001.
Gridin, L.A., Modern ideas about physiological and medioprophilactic effects of hypoxia and hypercapnia, Meditsina, 2016, no. 3, pp. 45–68.
Charniy, A.M., Patofiziologiya gipoksicheskikh sostoyaniy (Pathophysiology of Hypoxic States), Moscow, 1961.
Shik, L.L. and Kanaev, N.N., Rukovodstvo po klinicheskoi fiziologii dykhaniya (Handbook of Clinical Physiology of Respiration), Leningrad, 1980.
Barbashova, Z.I., Akklimatizatsiya k gipoksii i ee fiziologicheskie mekhanizmy (Acclimation to Hypoxia and its Physiological Mechanisms), Leningrad, 1960.
Nilsson, G.E., Vaage, J., and Stenslkken, K.O., Oxygen-and temperature-dependent expression of survival protein kinases in crucian carp (Carassius carassius) heart and brain, Am. J. Physiol. Regul. Integr. Comp. Physiol., 2015, vol. 308, pp. 50–61.
Ilyina, T.N., Ilyukha, V.A., Baishnikova, I.V., Belkin, V.V., Sergina, S.N., and Antonova, E.P., Antioxidant defense system in tissues of semiaquatic mammals, J. Evol. Biochem. Physiol., 2017, vol. 53, no. 4, pp. 282–288.
Silkin, Yu.A. and Silkina, E.N., Effect of hypoxia on physiological and biochemical blood parameters in some marine fish, Zh. Evol. Biokhim. Fiziol., 2005, vol. 41, no. 5, pp. 421–425.
Nayler, W.G. and Daily, M.D., Fiziologiya i pathofiziologiya serdtsa (Physiology and Pathophysiology of the Heart), Moscow, 1990, vol. l, pp. 556–578.
Allen, D.G. and Orchard, C.H., Measurements of intracellular calcium concentration in heart muscle: the effects of inotropic interventions and hypoxia, J. Mol. Cell Cardiol., 1984, vol. 16, pp. 117–128.
Potter, S. and Fothergill-Gilmore, L.A., Molecular evolution: The origin of glycolysis, Biochem. Educ., 1993, vol. 21, pp. 45–48.
Oslancová, A. and Janecek, S., Evolutionary relatedness between glycolytic enzymes most frequently occurring in genomes, Folia Microbiol. (Praha), 2004, vol. 49, pp. 247–258.
Meerson, F.Z., Adaptation medicine: mechanisms and protective effects of adaptation, Hypoxia Medical J., M., 1993, pp. 168–226.
Czyzyk-Krzeska, M.F., Molecular aspects of oxygen sensing in physiological adaptation to hypoxia, Respir-Physiol., 1997, vol. 110, pp. 99–111.
Guo, H.C., Guo, F., Zhang, L.N., Zhang, R., Chen, Q., Li, J.X., Yin, J., and Wang, Y.L., Enhancement of Na/K pump activity by chronic intermittent hypobaric hypoxia protected against reperfusion injury, Am. J. Physiol. Heart Circ. Physiol., 2011, vol. 300, pp. H2280–H2287.
Seehase, M., Quentin, T., Wiludda, E., Hellige, G., Paul, T., and Schiffmann, H., Gene expression of the Na–Ca2+ exchanger, SERCA2a and calsequestrin after myocardial ischemia in the neonatal rabbit heart, Biol. Neonate, 2006, vol. 90, pp. 174–184.
Wang, W., Peng, Y., Wang, Y., Zhao, X., and Yuan, Z., Anti-apoptotic effect of heat shock protein 90 on hypoxia-mediated cardiomyocyte damage is mediated via the phosphatidylinositol 3-kinase/AKT pathway, Clin. Exp. Pharmacol. Physiol., 2009, vol. 36, pp. 899–903.
Viswanath, K., Bodiga, S., Balogun, V., Zhang, A., and Bodiga, V.L., Cardioprotective effect of zinc requires ErbB2 and Akt during hypoxia/reoxygenation, Biometals, 2011, vol. 24, pp. 171–180.
Silverman, H.S., Wei, S., Haigney, M.C., Ocampo, C.J., and Stern, M.D., Myocyte adaptation to chronic hypoxia and development of tolerance to subsequent acute severe hypoxia, Circ. Res., 1997, vol. 80, pp. 699–707.
Sun, Y. and MacRae, T.H., Small heat shock proteins: molecular structure and chaperone function, Cell Mol. Life Sci., 2005, vol. 62, pp. 2460–2476.
Paier, A., Agewall, S., and Kublickiene, K., Expression of heat shock proteins and nitrotyrosine in small arteries from patients with coronary heart disease, Heart Vessels, 2009, vol. 24, pp. 260–266.
Vilahur, G., Cubedo, J., Casani, L., Padro, T., Sabate-Tenas, M., Badimon, J.J., and Badimon, L., Reperfusion-triggered stress protein response in the myocardium is blocked by post-conditioning. Systems biology pathway analysis highlights the key role of the canonical aryl-hydrocarbon receptor pathway, Eur. Heart J., 2013, vol. 34, pp. 2082–2093.
Zhang, B., Zhou, H.S., Cheng, Q., Lei, L., and Hu, B., Overexpression of HSP27 in cultured human aortic smooth muscular cells reduces apoptosis induced by low-frequency and low-energy ultrasound by inhibition of an intrinsic pathway, Genet. Mol. Res., 2013, vol. 12, pp. 6588–6601.
Wu, J., Chen, P., Li, Y., Ardell, C., Der, T., Shohet, R., Chen, M., and Wright, G.L., HIF-1a in heart: protective mechanisms, Am. J. Physiol. Heart Circ. Physiol., 2013, vol. 305, pp. H821–H828.
Semenza, G.L., Hypoxia-inducible factor 1: oxygen homeostasis and disease pathophysiology, Trends Mol. Med., 2001, vol. 7, pp. 345–350.
Bekeredjian, R., Walton, C.B., MacCannell, K.A., Ecker, J., Kruse, F., Outten, J.T., Sutcliffe, D., Gerard, R.D., Bruick, R.K., and Shohet, R.V., Conditional HIF-1alpha expression produces a reversible cardiomyopathy, PLoS One, 2010, vol. 5, p. e11693.
Guimarães-Camboa, N., Stowe, J., Aneas, I., Sakabe, N., Cattaneo, P., Henderson, L., Kilberg, M.S., Johnson, R.S., Chen, J., McCulloch, A.D., Nobrega, M.A., Evans, S.M., and Zambon, A.C., HIF1a Represses cell stress pathways to allow proliferation of hypoxic fetal cardiomyocytes, Dev. Cell, 2015, vol. 33, pp. 507–521.
Marden, J.H., Fescemyer, H.W., Schilder, R.J., Doerfler, W.R., Vera, J.C., and Wheat, C.W., Genetic variation in HIF signaling underlies quantitative variation in physiological and life-history traits within lowland butterfly populations, Evolution, 2013, vol. 67, pp. 1105–1115.
Zeng, L., Wang, Y.H., Ai, C.X., Zheng, J.L., Wu, C.W., and Cai, R., Effects of β-glucan on ROS production and energy metabolism in yellow croaker (Pseudosciaena crocea) under acute hypoxic stress, Fish Physiol. Biochem., 2016, vol. 42, pp. 1395–1405.
Yin, H.L., Luo, C.W., Dai, Z.K., Shaw, K.P., Chai, C.Y., and Wu, C.C., Hypoxia-inducible factor-1a, vascular endothelial growth factor, inducible nitric oxide synthase, and endothelin-1 expression correlates with angiogenesis in congenital heart disease, Kaohsiung J. Med. Sci., 2016, vol. 32, pp. 348–355.
Yue, X., Lin, X., Yang, T., Yang, X., Yi, X., Jiang, X., Li, X., Li, T., Guo, J., Dai, Y., Shi, J., Wei, L., Youker, K.A., Torre-Amione, G., Yu, Y., Andrade, K.C., and Chang, J., Rnd3/RhoE modulates hypoxia-inducible factor 1a/vascular endothelial growth factor signaling by stabilizing hypoxia-inducible factor 1a and regulates responsive cardiac angiogenesis, Hypertension, 2016, vol. 67, pp. 597–605.
Hansen, A.H., Nielsen, J.J., Saltin, B., and Helsten, Y., Exercise training normalizes skeletal muscle vascular endothelial growth factor levels in patients with essential hypertension, J. Hypertens., 2010, vol. 28, pp. 1176–1185.
Ferrara, N. and Davis-Smyth, T., The biology of vascular endothelial growth factor, Endocr. Rev., 1997, vol. 18, pp. 4–25.
Eklund, L., Kangas, J., and Saharinen, P., Angiopoietin-Tie signalling in the cardiovascular and lymphatic systems, Clin. Sci. (Lond.), 2017, vol. 131, pp. 87–103.
Mrochek, A.G., Basalay, M.V., Barsukevich, V.Ch., and Gurin, A.V., Endogenous cardioprotective phenomena and their mechanisms, Kardiol. Belarus., 2014, vol. 34, no. 3, pp. 88–109.
Gubareva, L.I., Adaptation systems of the organism during pre-and postnatal periods of ontogenesis under the effect of anthropogenic factors of the environment, Doctorate Sci. Diss., Stavropol, 1999.
Kozlovskii, V.I., Humoral mechanisms of endothelium-dependent regulation of coronary blood flow, Doctorate Sci. Diss., Minsk, 2015.
Moncada, S., Palmer, R.M.J., and Higgs, E.A., Nitric oxide: physiology, pathophysiology, and pharmacology, Pharmacol. Rev., 1991, vol. 43, pp. 109–141.
Malyshev, I.Yu. and Manukhina, E.B., Stress, adaptation, and nitric oxide, Biokhim., 1998, vol. 6, no. 7, pp. 992–1006.
Torreilles, J., Nitric oxide: one of the more conserved and widespread signaling molecules, Front. Biosci., 2001, vol. 6, pp. D1161–D1172.
Silva, B.R., Paula, T.D., Paulo, M., and Bendhack, L.M., Nitric oxide signaling and the cross talk with prostanoids pathways in vascular system, Med. Chem., 2016, PubMed PMID: 28031017.
Moncada, S., Gryglewski, R., Bunting, S., and Vane, J.R., An enzyme isolated from arteries transforms prostaglandin endoperoxides to an unstable substance that inhibits platelet aggregation, Nature, 1976, vol. 263, pp. 663–665.
Malakhova, Z.L., Vasina, E.Yu., Vorobyov, E.A., Nesterovich, I.I., and Vlasov, T.D., A noninvasive method to study the endothelial hyperpolarizing factor in clinic, Region. Krovoobr. Mikrotsirkul., 2013, vol. 12, no. 4, pp. 70–74.
Rahimtoola, S., The hibernating myocardium, Am. Heart J., 1989, vol. 117, pp. 211–221.
Rahimtoola, S.H., Concept and evaluation of hibernating myocardium, Annu. Rev. Med., 1999, vol. 50, pp. 75–86.
Opie, L.H., Cardiac metabolism in ischemic heart disease, Arch. Mal. Coeur. Vaiss., 1999, vol. 92, pp. 1755–1760.
Brauwald, E. and Rutherford, J.D., Reversible ischemic left ventricular dysfunction: evidence for the “hibernating myocardium”, J. Am. Coll. Cardiol., 1986, vol. 8, pp. 1467–1470.
Pantely, G.A., Arai, A.E., Grauer, S.E., and Bristow, J.D., Metabolic aspects of hibernating myocardium, Z. Kardiol., 1995, vol. 84, pp. 101–105.
Tarasov, R.S., Vereshchagin, E.I., and Ganyukov, V.I., Methods of cardioprotection in myocardial infarction. A status quo, Kompl. Probl. Serd.-Sosud. Zabol., 2016, no. 4, pp. 44–50.
Hochachka, P.W., Metabolic arrest, Intensive Care Med., 1986, vol. 12, pp. 127–133.
Yan, L., Kudej, R.K., Vatner, D.E., and Vatner, S.F., Myocardial ischemic protection in natural mammalian hibernation, Basic. Res. Cardiol., 2015, vol. 110, p.9.
Heyndrickx, G.R., Early reperfusion phenomena, Semin. Cardiothorac. Vasc. Anesth., 2006, vol. 10, pp. 236–241.
McFalls, E.O., Hou, M., Bache, R.J., Best, A., Marx, D., Sikora, J., and Ward, H.B., Activation of p38 MAPK and increased glucose transport in chronic hibernating swine myocardium, Am. J. Physiol. Heart Circ. Physiol., 2004, vol. 287, pp. H1328–H1334.
Chereshnev, V.A., Klinicheskaya patofiziologiya (Clinical Pathophysiology), St. Petersburg, 2012.
Depre, C., Kim, S.J., John, A.S., Huang, Y., Rimoldi, O.E., Pepper, J.R., Dreyfus, G.D., Gaussin, V., Pennell, D.J., Vatner, D.E., Camici, P.G., and Vatner, S.F., Program of cell survival underlying human and experimental hibernating myocardium, Circ. Res., 2004, vol. 95, pp. 433–440.
Blagonravov, M.L., Apoptosis in cardiomyocytes as a typical reaction of the altered heart, Doctorate Sci. Diss., Moscow, 2011.
Masri, C. and Chandrashekhar, Y., Apoptosis: a potentially reversible, meta-stable state of the heart, Heart Fail. Rev., 2008, vol. 13, pp. 175–179.
Kremastinos, D.T., The phenomenon of preconditioning today, Hell. J. Cardiol., 2005, vol. 46, pp. 1–4.
Murry, C.E., Jennings, R.B., and Reimer, K.A., Preconditioning with ischemia: A delay of lethal cell injury in ischemic myocardium, Circulation, 1986, vol. 74, pp. 1124–1136.
Xu, Q., Li, Q.G., Fan, G.R., Liu, Q.H., Mi, F.L., and Liu, B., Protective effects of fentanyl preconditioning on cardiomyocyte apoptosis induced by ischemia-reperfusion in rats, Braz. J. Med. Biol. Res., 2017, vol. 50, p. e5286.
Shizukuda, Y., Mallet, R.T., Lee, S.C., and Downey, H.F., Hypoxic preconditioning of ischaemic canine myocardium, Cardiovasc. Res., 1992, vol. 26, pp. 534–542.
Jennings, R.B., Sebbag, L., Schwartz, L.M., Crago, M.S., and Reimer, K.A., Metabolism of preconditioned myocardium: effect of loss and reinstatement of cardioprotection, J. Mol. Cell Cardiol., 2001, vol. 33, pp. 1571–1588.
Murry, C.E., Richard, V.J., Reimer, K.A., and Jennings, R.B., Ischemic preconditioning slows energy metabolism and delays ultrastructural damage during a sustained ischemic episode, Circ. Res., 1990, vol. 66, pp. 913–931.
Downey, J.M., Davis, A.M., and Cohen, M.V., Signaling pathways in ischemic preconditioning, Heart Fail. Rev., 2007, vol. 12, pp. 181–188.
Likhvantsev, V.V., Moroz, V.V., Grebenchikov, O.A., Gorokhovatsky, Yu.I., Zarzhetsky, Yu.V., Timoshin, S.S., Levikov, D.I., and Shaibakova, V.L., Ischemic and pharmacological preconditioning, Obshch. Reanimat., 2011, vol. 7, no. 6, pp. 59–65.
Garlid, K.D., Dos Santos, P., Xie, Z.J., Costa, A.D., and Paucek, P., Mitochondrial potassium transport: the role of the mitochondrial ATPsensitive K+-channel in cardiac function and cardioprotection, Biochim. Biophys. Acta, 2003, vol. 1606, pp. 1–21.
Budas, G., Costa, H.M., Ferreira, J.C., Teixeira da Silva Ferreira, A., Perales, J., Krieger, J.E., Mochly-Rosen, D., and Schechtman, D., Identification of εPKC targets during cardiac ischemic injury, Circ. J., 2012, vol. 76, pp. 1476–1485.
Ping, P., Zhang, J., Zheng, Y.T., Li, R.C., Dawn, B., Tang, X.L., Takano, H., Balafanova, Z., and Bolli, R., Demonstration of selective protein kinase C-dependent activation of Src and Lck tyrosine kinases during ischemic preconditioning in conscious rabbits, Circ. Res., 1999, vol. 85, pp. 542–550.
Ma, L.L., Ge, H.W., Kong, F.J., Qian, L.B., Hu, B.C., Li, Q., Xu, L., Liu, J.Q., Xu, Y.X., and Sun, R.H., Ventricular hypertrophy abrogates intralipid-induced cardioprotection by alteration of reperfusion injury salvage kinase/glycogen synthase kinase 3β signal, Shock, 2014, vol. 41, pp. 435–442.
Juhaszova, M., Zorov, D.B., Kim, S.H., Pepe, S., Fu, Q., Fishbein, K.W., Ziman, B.D., Wang, S., Ytrehus, K., Antos, C.L., Olson, E.N., and Sollott, S.J., Glycogen synthase kinase-3beta mediates convergence of protection signaling to inhibit the mitochondrial permeability transition pore, J. Clin. Invest., 2004, vol. 113, pp. 1535–1549.
Zorov, D.B., Juhaszova, M., Yaniv, Y., Nuss, H.B., Wang, S., and Sollott, S.J., Regulation and pharmacology of the mitochondrial permeability transition pore, Cardiovasc. Res., 2009, vol. 83, pp. 213–225.
Kroemer, G., Dallaporta, B., and Resche-Rigon, M., The mitochondrial death/life regulator in apoptosis and necrosis, Annu Rev. Physiol., 1998, vol. 60, pp. 619–642.
Karch, J. and Molkentin, J.D., Regulated necrotic cell death: the passive aggressive side of Bax and Bak, Circ Res., 2015, vol. 116, pp. 1800–1809.
Kowaltowski, A.J., Castilho, R.F., and Vercesi, A.E., Mitochondrial permeability transition and oxidative stress, FEBS Lett., 2001, vol. 495, pp. 12–15.
Grachev, D.E., The role of the peripheral benzodiazepine receptor at early stages of apoptosis and induction of the mitochondrial nonspecific pore, Candidate Sci. Diss., Pushchino, 2009.
Korotkov, S.M., Konovalova, S.A., Brailovskaya, I.V., and Saris, N.E., To involvement the conformation of the adenine nucleotide translocase in opening the Tl+-induced permeability transition pore in Ca2+-loaded rat liver mitochondria, Toxicol. In Vitro, 2016, vol. 32, pp. 320–332.
Calmettes, G., Ribalet, B., John, S., Korge, P., Ping, P., and Weiss, J.N., Hexokinases and cardioprotection, J. Mol. Cell Cardiol., 2015, vol. 78, pp. 107–115.
Datler, C., Pazarentzos, E., Mahul-Mellier, A.L., Chaisaklert, W., Hwang, M.S., Osborne, F., and Grimm, S., CKMT1 regulates the mitochondrial permeability transition pore in a process that provides evidence for alternative forms of the complex, J. Cell Sci., 2014, vol. 127, pp. 1816–1828.
Halestrap, A.P. and Brenner, C., The adenine nucleotide translocase: a central component of the mitochondrial permeability transition pore and key player in cell death, Curr. Med. Chem., 2003, vol. 10, pp. 1507–1525.
Crompton, M., The mitochondrial permeability transition pore and its role in cell death, Biochem. J., 1999, vol. 341, pp. 233–249.
Baines, C.P., The molecular composition of the mitochondrial permeability transition pore, J. Mol. Cell. Cardiol., 2009, vol. 46, pp. 850–857.
Azarashvili, T., Odinokova, I., Bakunts, A., Ternovsky, V., Krestinina, O., Tyynel, J., and Saris, N.E., Potential role of subunit c of F0F1-ATPase and subunit c of storage body in the mitochondrial permeability transition. Effect of the phosphorylation status of subunit c on pore opening, Cell Calcium, 2014, vol. 55, pp. 69–77.
Lebuffe, G., Schumacker, P.T., Shao, Z.H., Anderson, T., Iwase, H., and Vanden Hoek, T.L., ROS and NO trigger early preconditioning: relationship to mitochondrial KATP channel, Am. J. Physiol. Heart Circ. Physiol., 2003, vol. 284, pp. H299–H308.
Tang, X.L., Takano, H., Rizvi, A., Turrens, J.F., Qiu, Y., Wu, W.J., Zhang, Q., and Bolli, R., Oxidant species trigger late preconditioning against myocardial stunning in conscious rabbits, Am. J. Physiol. Heart Circ. Physiol., 2002, vol. 282, pp. H281–H291.
Green, D.R. and Reed, J.C., Mitochondria and apoptosis, Science, 1998, vol. 281, pp. 1309–1312.
Borisov, L.Yu., Pharmacological myocardial preconditioning in surgeries with artificial blood circulation, Candidate Sci. Diss., Moscow, 2013.
Shemarova, I.V. and Nesterov, V.P., Role of Ca2+ and neurotransmitters of the sympathetic nervous system in transmission of stress signal in cardiomyocytes, Zh. Evol. Biokhim. Fiziol., 2006, vol. 42, no. 2, pp. 97–104.
Karpova, E.S., Ischemic preconditioning and its cardioprotective effect in cardiorehabilitation programs for patients with ischemic heart disease after transcutaneous coronary interventions, Ross. Kardiol. Zh., 2012, no. 4, pp. 104–108.
Hausenloy, D.J., Ong, S.B., and Yellon, D.M., The mitochondrial permeability transition pore as a target for preconditioning and postconditioning, Basic Res. Cardiol., 2009, vol. 104, pp. 189–202.
Author information
Authors and Affiliations
Corresponding author
Additional information
Original Russian Text © I.V. Shemarova, V.P. Nesterov, S.M. Korotkov, Yu.A. Sylkin, 2018, published in Zhurnal Evolyutsionnoi Biokhimii i Fiziologii, 2018, Vol. 54, No. 1, pp. 9—19.
Rights and permissions
About this article
Cite this article
Shemarova, I.V., Nesterov, V.P., Korotkov, S.M. et al. Evolutionary Aspects of Cardioprotection. J Evol Biochem Phys 54, 8–21 (2018). https://doi.org/10.1134/S0022093018010027
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S0022093018010027