Abstract
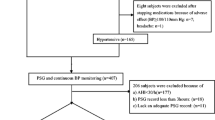
Obstructive sleep apnea syndrome (OSAS) is closely associated with hypertension. Activity of angiotensin II (Ang II) and non-dipping nocturnal blood pressure (BP) variability are implicated in hypertension-related target organ damage. We examined the correlation between OSAS with serum Ang II levels and evaluated the risk of non-dipping BP variability in 180 patients with essential hypertension (EHT). Eligible patients were divided into three subgroups based on their apnea-hypopnea index (AHI) evaluated by polysomnography. EHT alone, EHT with mild OSAS, and EHT with moderate/severe OSAS. Ambulatory BP monitoring was used to calculate mean BP over 24 h, as well as diurnal and nocturnal BP variability. Serum Ang II was determined with enzyme-linked immun-osorbent assay. EHT patients with OSAS had significantly higher systolic BP calculated either over 24 h, or by diurnal or nocturnal monitoring (P < 0.05). More EHT patients with OSAS showed non-dipping BP profiles than did EHT patients alone (P < 0.05). The number of patients with non-dipping BP increased with increasing OSAS severity. Surgical treatment alleviated OSAS and reduced AHI (P < 0.05). Preoperative serum Ang II in EHT patients with OSAS was significantly higher than that in those without OSAS (P < 0.05), and showed a rising trend with OSAS severity (P < 0.05). Postoperative serum Ang II, BP and the incidence of non-dipping BP were reduced by surgery to levels lower than preoperative values in patients with OSAS. We therefore conclude that OSAS leads to increased serum Ang II and increased risk of non-dipping BP in patients with EHT.
Similar content being viewed by others
References
Goodfriend TL. Obesity, sleep apnea, aldosterone, and hypertension. Curr. Hypertens. Rep. 2008; 10: 222–6.
Lopez-Jimenez F, Sert Kuniyoshi FH, Gami A, Somers VK. Obstructive sleep apnea: implications for cardiac and vascular disease. Chest 2008; 133: 793–804.
Chobanian AV, Bakris GL, Black HR et al. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA 2003; 289: 2560–72
Haentjens P, Van Meerhaeghe A, Moscariello A et al. The impact of continuous positive airway pressure on blood pressure in patients with obstructive sleep apnea syndrome: evidence from a meta-analysis of placebo-controlled randomized trials. Arch. Intern. Med. 2007; 167: 757–64.
Dernaika TA, Kinasewitz GT, Tawk MM. Effects of nocturnal continuous positive airway pressure therapy in patients with resistant hypertension and obstructive sleep apnea. J. Clin. Sleep Med. 2009; 5: 103–7.
Campos-Rodriguez F, Grilo-Reina A, Perez-Ronchel J et al. Effect of continuous positive airway pressure on ambulatory BP in patients with sleep apnea and hypertension: a placebo-controlled trial. Chest 2006; 129: 1459–67.
Barbe F, Duran-Cantolla J, Capote F et al. Long-term effect of continuous positive airway pressure in hypertensive patients with sleep apnea. Am. J. Respir. Crit. Care Med. 2010; 181: 718–26.
Hui DS, To KW, Ko FW et al. Nasal CPAP reduces systemic blood pressure in patients with obstructive sleep apnoea and mild sleepiness. Thorax 2006; 61: 1083–90.
Johansson ME, Bernberg E, Andersson IJ et al. High-salt diet combined with elevated angiotensin II accelerates atherosclerosis in apolipoprotein E-deficient mice. J. Hypertens. 2009; 27: 41–7.
Hassler C, Burnier M. Circadian variations in blood pressure: implications for chronotherapeutics. Am. J. Cardio-vasc. Drugs 2005; 5: 7–15.
Hermida RC, Ayala DE, Calvo C et al. Effects of time of day of treatment on ambulatory blood pressure pattern of patients with resistant hypertension. Hypertension 2005; 46: 1053–9.
Qiu YG, Zhu JH, Tao QM et al. Captopril administered at night restores the diurnal blood pressure rhythm in adequately controlled, nondipping hypertensives. Car-diovasc. Drugs Ther. 2005; 19: 189–95.
Ruehland WR, Rochford PD, O’Donoghue FJ, Pierce RJ, Singh P, Thornton AT. The new AASM criteria for scoring hypopneas: impact on the apnea hypopnea index. Sleep 2009; 32: 150–7.
Williams GH, Cain JP, Dluhy RG, Underwood RH. Studies of the control of plasma aldosterone concentration in normal man. I. Response to posture, acute and chronic volume depletion, and sodium loading. J. Clin. Invest. 1972; 51 (7): 173–142.
Verdecchia P, Clement D, Fagard R, Palatini P, Blood PG. Pressure Monitoring. Task force III: Target-organ damage, morbidity and mortality. Blood Press. Monit. 1999; 4: 303–17.
Gurley SB, Allred A, Le TH et al. Altered blood pressure responses and normal cardiac phenotype in ACE2-null mice. J. Clin. Invest. 2006; 116: 2218–25.
Foster GE, Hanly PJ, Ahmed SB, Beaudin AE, Pialoux V, Poulin MJ. Intermittent hypoxia increases arterial blood pressure inhumans through a Renin-Angiotensin system-dependent mechanism. Hypertension 2010; 56 (3): 369–77.
Pépin JL, Tamisier R, Barone-Rochette G, Launois SH, Lévy P, Baguet JP. Comparison of continuous positive airway pressure and valsartan in hypertensive patients with sleep apnea. Am. J. Respir. Crit. Care Med. 2010; 182 (7): 954–60.
Izzedine H, Launay-Vacher V, Deray G. Abnormal blood pressure circadian rhythm: a target organ damage? Int. J. Cardiol. 2006; 107: 343–9.
Zoccali C, Benedetto FA, Mallamaci F et al. Left ventricular hypertrophy and nocturnal hypoxemia in hemodialy-sis patients. J. Hypertens. 2001; 19: 287–93.
Routledge F, McFetridge-Durdle J. Nondipping blood pressure patterns among individuals with essential hypertension: a review of the literature. Eur. J. Cardiovasc. Nurs. 2007; 6: 9–26.
Madin K, Iqbal P. Twenty four hour ambulatory blood pressure monitoring: a new tool for determining cardiovascular prognosis. Postgrad. Med. J. 2006; 82: 548–51.
Imadojemu VA, Mawji Z, Kunselman A, Gray KS, Hogeman CS, Leuenberger UA. Sympathetic chemore-flex responses in obstructive sleep apnea and effects of continuous positive airway pressure therapy. Chest 2007; 131: 1406–13.
Moller DS, Lind P, Strunge B, Pedersen EB. Abnormal vasoactive hormones and 24-hour blood pressure in obstructive sleep apnea. Am. J. Hypertens. 2003; 16: 274–80.
Carneiro G, Togeiro SM, Hayashi LF et al. Effect of continuous positive airway pressure therapy on hypothalamic-pituitary-adrenal axis function and 24-h blood pressure profile in obese men with obstructive sleep apnea syndrome. Am. J. Physiol. Endocrinol. Metab. 2008; 295: E380–384.
Somers VK, White DP, Amin R et al. Sleep apnea and cardiovascular disease: an American Heart Association/ American College Of Cardiology Foundation Scientific Statement from the American Heart Association Council for High Blood Pressure Research Professional Education Committee, Council on Clinical Cardiology, Stroke Council, and Council On Cardiovascular Nursing. In collaboration with the National Heart, Lung, and Blood Institute National Center on Sleep Disorders Research (National Institutes of Health). Circulation 2008; 118: 1080–111.
Butt M, Dwivedi G, Khair O, Lip GY. Obstructive sleep apnea and cardiovascular disease. Int. J. Cardiol. 2010; 139: 7–16.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, H., Zhang, Y., Chen, Y. et al. Factors associated with severity of daytime sleepiness and indications for initiating treatment in patients with periodic limb movements during sleep. Sleep Biol. Rhythms 10, 195–201 (2012). https://doi.org/10.1111/j.1479-8425.2012.00561.x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1111/j.1479-8425.2012.00561.x