Abstract
Background: In severe acute coronary syndromes (ACS) elevation of markers of inflammation and acute phase reaction (APR) like C-reactive protein (CRP) as well as a release of troponin have been reported.
Using a high sensitivity troponin T (TnT) test we investigated whether an APR occurs in ACS only in the presence of ischemic myocardial damage.
Methods: In 85 patients with ACS C-reactive protein (CRP), serum amyloid A (SAA), fibrinogen, thrombin antithrombin III complexes (TAT) and kallikrein were determined vs. high sensitive TnT (≥0.02 ng/ml) initially and 2 d later vs. 45 patients with stable angina pectoris and 42 controls.
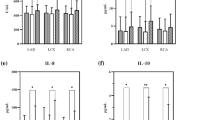
Results: In stable angina pectoris, markers of inflammation and coagulation were slightly elevated (p < 0.05). Initially in ACS elevations of CRP to 1.2 ± 0.3 mg/dl, SAA to 4.8 ± 2.6 mg/dl and fibrinogen to 448 ± 21 mg/dl (all p < 0.01 vs. controls) were found followed by a significant APR (p < 0.01).
In the subgroup of TnT positive ACS patients, an APR with increased CRP (4.1 ± 1.3 mg/dl), SAA (20.4 ± 8.3 mg/dl), and fibrinogen (641 ± 45 mg/dl) was detectable (all p < 0.05 vs. TnT negative patients). In contrast, patients without TnT release showed APR markers comparable to patients with stable angina pectoris.
Conclusion: Our findings demonstrate an association between myocardial injury in ACS and acute phase reaction as evidenced by several molecular markers. A highly sensitive TnT-test identified myocardial inury in about all patients with APR while a standard TnT cut-off (0.1 ng/ml) missed 32% of these patients. Thus, the APR in patients with ACS is strongly associated with at least minor ischemic myocardial damage and prior findings of an APR independent from myocardial injury are probably based on less sensitive troponin tests.
Similar content being viewed by others
References
Falk E, Shah PK, Fuster V. Coronary plaque disruption. Circulation 1995;92:657-671.
Ross R. Atherosclerosis–an inflammatory disease. N Engl J Med 1999;340:115-126.
Gotoh K, Minamino T, Katoh O, et al. The role of intracoronary thrombus in unstable angina: angiographic assessment and thrombolytic therapy during ongoing anginal attacks. Circulation 1988;77:526-534.
Zalewski A, Shi Y, Nardone D, et al. Evidence for reduced fibrinolytic activity in unstable angina at rest. Circulation 1991;83:1685-1691.
Hoffmeister HM, Jur M, Wendel HP, et al. Alterations of the coagulation, the fibrinolytic and the kallikrein-kinin system in the acute and post-acute phase in patients with unstable angina pectoris. Circulation 1995;91:2520-2527.
Merlini PA, Bauer KA, Oltrona L, et al. Persistent activation of coagulation mechanism in unstable angina and myocardial infarction. Circulation 1994;90:61-68.
Giannitsis E, Müller Bardorff M, Schweikart S, et al. Relationship of cardiac troponin T and procoagulant activity in unstable angina. Thromb Haemost 2000;83:224-228.
Liuzzo G, Biasucci LM, Gallimore JR, et al. The prognostic value of C-reactive protein and serum amyloid A protein in severe unstable angina. N Engl J Med 1994;331:417-424.
Liuzzo G, Biasucci LM, Rebuzzi AG, et al. A Plasma protein acute-phase response in unstable angina is not induced by ischemic injury. Circulation 1996;94:2373-2380.
Biasucci LM, Liuzzo G, Caligiuri G, et al. Temporal relation between ischemic episodes and activation of the coagulation system in unstable angina. Circulation 1996;93:2121- 2127.
Otrona L, Merlini PA, Savonitto S, et al. Lack of correlation between activation of hemostatic mechanism and inflammation in unstable angina pectoris. Thromb & Thrombolysis 1998; 5: 169-173.
Fyfe AI, Rothenberg LS, DeBeer FC, et al. Association between serum amyolid A proteins and coronary artery disease. Circulation 1997;96:2914-2919.
Ridker PM, Cushman M, Stampfer MJ, et al. CH Inflammation, aspirin, and the risk of cardiovascular disease in apparently healthy men. N Engl J Med 1997;336:973-979.
Haverkate F, Thompson SG, Pyke SDM, et al. Production of C-reactive protein and risk of coronary events in stable and unstable angina. Lancet 1997;349:462-466.
Toss H, Lindahl B, Siegbahn A, Wallentin L. Prognostic influence of increased fibrinogen and C-reactive protein levels in unstable coronary artery disease. Circulation 1997;96:4204-4210.
Morrow DA, Rifai N, Antman EM, et al. C-reactive protein is a potent predictor of mortality independently of and in combination with troponin T in acute coronary syndromes: a TIMI 11A substudy. J Am Coll Cardiol 1998;31:1460-1465.
Théroux P, Latour JG, Léger-Gauthier C, et al. FibrinopeptideAand platelet factor levels in unstable angina pectoris. Circulation 1987;75:156-162.
Eisenberg PR, Kenzora JL, Sobel BE, et al. Relation between ST segment shifts during ischemia and thrombin activity in patients with unstable angina pectoris. J Am Coll Cardiol 1991;8:898-903.
ACC/AHA guidelines for the management of patients with unstable angina and non-ST segment elevation myocardial Minor Myocardial Damage and Inflammation 39 infarction: executive summary and recommendations. Circulation 2000;102:1193-1209.
Ohman E, Armstrong P, Christenson R. Cardiac troponin T levels for risk stratification in acute myocardial ischemia. N Engl J Med 1996;335:1333-1341.
Hamm C, Ravkilde J, Gerhardt W. The prognostic value of serum troponin T in unstable angina. N Engl J Med 1992;327:146-150.
Heeschen C, Hamm CW, Bruemmer J, et al. Predictive value of C-reactive protein and troponin T in patients with unstable angina: a comparative analysis. J Am Coll Cardiol 2000;35:1535-1542.
Lindahl B, Toss H, Siegbahn A, et al. Markers of myocardial damage and inflammation in relation to long-term mortality in unstable coronary artery disease. N Engl J Med 2000;343:1139-1147.
Braunwald E. Unstable angina: a classification. Circulation 1989;80:410-414.
Hocke G, Ebel H, Bittner K, et al. A rapid laser immunonephelometric assay for serum amyloid A (SAA) and its application to the diagnosis of kidney allograft rejection. Klin Wochenschr 1989;67:447-451.
Katus HA, Loser S, Hallermayer K, et al. Development and in vitro characterization of a new immunoassay of cardiac troponin T. Clin Chem 1992;38:386-393.
Torzewski J, Torzewski M, Bowyer DE, et al. C-reactive protein frequently colocalizes with the terminal complement complex in the intima of early atherosclerotic lesions of human coronary arteries. Arterioscler Thromb Vasc Biol 1998;18:1386-1392.
Cermak J, Key NS, Bach RR, et al. C-reactive protein induces human peripheral blood monocytes to synthesize tissue factor. Blood 1993;82:513-520.
Badolato R, Wang JM, Murphy WJ, et al. Serum amyloid A is a chemoattractant: induction of migration, adhesion, and tissue infiltration of monocytes and polymorphonuclear leukocytes. J Exp Med 1994;180:203-209.
Meek RL, Urieli-Shoval S, Benditt EP. Expression of apolipoprotein serum amyolid A mRNA in human atherosclerotic lesions and cultured vascular cells: implications for serum amyloid A. Proc Natl Acad Sci USA 1994;91:3186-3190.
Chooi CC, Gallus AS. Acute phase reaction, fibrinogen level and thrombus size. Thromb Res 1989;53:493-501.
Biasucci LM, Liuzzo G, Caligiuri G, et al. Episodic activation of the coagulation system in unstable angina does not elicit an acute phase reaction. Am J Cardiol 1996;77:85-87.
Biasucci LM, Vitelli A, Liuzzo G, et al. Elevated levels of interleukin-6 in unstable angina. Circulation 1996;94:874-877.
Takihara KY, Ihara Y, Ogata A, et al. Hypoxic stress induces cardiac myocyte-derived interleukin-6. Circulation 1995;91:1520-1524.
Kukielka GL, Smith CM, Manning AM, et al. Induction of interleukin-6 synthesis in the myocardium: potential role in postreperfusion inflammatory injury. Circulation 1995;92:1866-1875.
Le J, Vilcek J. Biology of disease: interleukin 6: amultifunctional cytokine regulating immune reactions and acute phase response. Lab Invest 1989;61:588-602.
Schieffer B, Schieffer E, Hilfiker-Kleiner D, et al. Expression of angiotensin II and interleukin 6 in human coronary atherosclerotic plaques. Circulation 2000;101:1372-1378.
Bauer J, Gantr U, Geiger T, et al. Regulation of interleukin-s6 expression in cultured human blood monocytes and monocyte-derived macrophages. Blood 1988;72:1134- 1140.
Neumann FJ, Marx N, Gawaz M, et al. Induction of cytokine expression in leukocytes by binding of thrombinstimulated platelets. Circulation 1997;95:2387-2394.
Hoffmeister HM, Büttcher E, Ehlers R, et al. Increased leukocyte-platelet adhesion parallels platelet activation in acute coronary syndromes. Circulation 1998;98(Suppl):I–171.
Liuzzo G, Buffon A, Biasucci LM, et al. Enhanced inflammatory response to coronary angioplasty in patients with severe unstable angina. Circulation 1998;98:2370-2376.
Liuzzo G, Biasucci LM, Gallimore R, et al. Enhanced in-flammatory response in patients with preinfarction unstable angina. J Am Coll Cardiol 1999;34:1696-1703.
Heeschen C, Dimmeler S, Hamm CW, et al. Soluble CD40 ligand in acute coronary syndromes. N Engl J Med 2003;348:1104-1111.
Hamm CW, Goldmann BU, Heeschen C, et al. Emergency room triage of patients with acute chest pain by means of rapid testing for cardiac troponin T or troponin I. N Engl J Med 1997;327:1648-1653.
Hoffmeister HM, Jur M, Helber U, et al. Correlation between coronary morphology and molecular markers of fibrinolysis in unstable angina pectoris. Atherosclerosis 1999;144:151-157.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Hoffmeister, H.M., Ehlers, R., Büttcher, E. et al. Relationship Between Minor Myocardial Damage and Inflammatory Acute-Phase Reaction in Acute Coronary Syndromes. J Thromb Thrombolysis 15, 33–39 (2003). https://doi.org/10.1023/A:1026140317777
Issue Date:
DOI: https://doi.org/10.1023/A:1026140317777