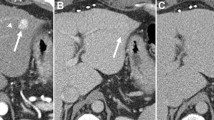
Abstract
Distinguishing benign tumors and pseudotumors of the liver from malignant tumors is a common clinical problem. Regenerative nodular hyperplasia (RNH) represents one of the more challenging pseudotumors to diagnose, because they can appear clinically indistinguishable from either a primary or a secondary liver malignancy. Even after comprehensive radiologic evaluation and image-guided percutaneous biopsy, the diagnosis of RNH can remain elusive. We reviewed the pathophysiology of RNH and present five cases illustrating the limitations of percutaneous biopsy and the utility of laparoscopic wedge biopsy in establishing the diagnosis. All patients underwent a complete workup that included percutaneous biopsy. Patients with a nondiagnostic percutaneous biopsy underwent a laparoscopic wedge biopsy or anatomical resection. H&E, vimentin, trichrome, and reticulin staining as well as CD34 immunostaining were performed. Five patients were diagnosed with RNH between May 2002 and April 2004. Three had focal nodular disease, whereas the other two had a diffuse multinodular presentation. Percutaneous biopsy definitively made the diagnosis in only one out of the five cases. Laparoscopic wedge biopsy was necessary to accurately make the diagnosis in three cases, whereas the fifth diagnosis was established after an anatomical resection. RNH is a unique pseudotumor of the liver that can present either as a solitary nodule or as a multinodular process. Percutaneous biopsy is associated with limitations in diagnosing RNH, and a more definitive surgical biopsy may be required. When RNH is considered, laparoscopic wedge biopsy is a safe and efficient way to obtain enough tissue to preserve the hepatic architecture required for diagnosis, while avoiding the morbidity of an unnecessary open resection.
Similar content being viewed by others
References
Nakanuma Y. Nodular regenerative hyperplasia of the liver: Retrospective survey at autopsy series. J Clin Gastroenterol 1990;12:460–465.
Wanless IR. Micronodular transformation (nodular regenerative hyperplasia) of the liver: A report of 64 cases among 2500 autopsies and a new classification of benign hepatocellular nodules. Hepatology 1990;11:787–797.
Ranstrom S. Milear hepatocellular adenomatosis. Acta Pathol Microbiol Scand 1953;33:225–229.
Steiner PE. Nodular regenerative hyperplasia of the liver. Am J Pathol 1959;35:943–952.
Wanless IR, Goodwin TA, Aen F, Feder A. Nodular regenerative hyperplasia of the liver in hematological disorders: A possible response to obliterative portal venopathy. A morphometric study of nine cases with a hypothesis of pathogenesis. Medicine 1980;59:367–379.
Wanless IR, Letz JS, Roberts EA. Partial nodular transformation of the liver in an adult with persistent ductus venosus. Arch Pathol Lab Med 1985;109:427–432.
Kondo F. Benign nodular hepatocellular lesions caused by abnormal hepatic circulation: Etiological analysis and of a new concept. J Gastroenterol Hepatol 2001;16:1319–1328.
Morales JM, Prieto C, Colina F, et al. Nodular regenerative hyperplasia of the liver in renal transplantation. Transplant Proc 1987;19:3694–3696.
Snover DC, Weisdorf S. Bloomer, et al. Nodular regenerative hyperplasia of the liver following bone marrow transplantation. Hepatology 1989;9:443–9448.
Solis-Herruzo JA, Vidal JV, Colina F. Nodular regenerative hyperplasia of the liver associated with toxic oil syndrome. Report of five cases. Hepatology 1986;6:687–693.
Thung SN, Gerber MA, Bodenheimer HC Jr. Nodular regenerative hyperplasia of the liver in a patient with diabetes mellitus. Cancer 1982;49:543–546.
Shimamatsu K, Wanless IR. Role of ischemia in causing apoptosis, atrophy and nodular regenerative hyperplasia in human liver. Hepatology 1996;26:343–350.
Gibbs JF, Litwin A, Kallenberg MS. Contemporary management of benign liver tumors. Surg Clin North Am 2004;84:463–480.
Connolly CE, O’Brien MJ. Nodular transformation of the liver. Report of a case. Human Pathol 1977;8:350.
Rougier P, Degott C, Rueff B, Benhamou JP. Nodular regenerative hyperplasia of the liver. Report of six cases and review of the literature. Gastroenterology 1978;75:169–175.
Stroymeyer WF, Ishak KG. Nodular transformation (nodular regenerative hyperplasia) of the liver. Human Pathol 1981;12:60–71.
Dachman AH, Ros PR, Goodman ZD, Olmsted WW, Ishak KG. Nodular regenerative hyperplasia of the liver: Clinical and radiologic observations. AJR Am J Roentgenol 1987;148:712–722.
Arvanitaki M, Adler M. Nodular regenerative hyperplasia of the liver. A review of 14 Cases. Hepatogastroenterology 2001;48:1425–1429.
Nzeako UC, Goodman ZD, Ishak KG. Hepatocellular carcinoma and nodular regenerative hyperplasia possible pathogenetic relationship. Am J Gastroenterol 1996;91:879–884.
Kim T, Baron RL, Nalesnik MA. Infarcted regenerative nodules in cirrhosis: Ct and MR imaging findings with pathologic correlation. AJR Am J Roentgenol 2000;174:1121–1125.
Clouet M, Boulay I, Boudiaf M, et al. Imaging features of nodular regenerative hyperplasia of the liver mimicking hepatic metastasis. Abdom Imaging 1999;24:258–261.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Foster, J.M., Litwin, A., Gibbs, J.F. et al. Diagnosing regenerative nodular hyperplasia, the “great masquerader” of liver tumors. J Gastrointest Surg 10, 727–733 (2006). https://doi.org/10.1016/j.gassur.2005.10.010
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.gassur.2005.10.010