Abstract
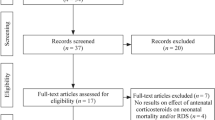
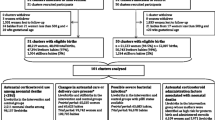
The objective of this study was to analyze the available evidence of systematic reviews that evaluated the efficacy of antenatal corticosteroids in order to contribute to a reduction in magnitude and transcendence of respiratory distress syndrome of the newborn (RDS). Thus, an overview was conducted including all systematic reviews of randomized controlled trials (RCTs) that evaluated women who received corticosteroid treatment during pregnancy to prevent RDS. Therefore, a search strategy was developed using the terms “respiratory distress syndrome, newborn,” “corticosteroids,” “perinatal death,” “neonatal death,” “neonate,” and “pregnancy.” The electronic databases searched were MEDLINE, EMBASE, Cochrane Library, LILACS, and Google Scholar, for studies published until June 2020. We identified 354 references, 38 of which were relevant after the initial screening. Ten systematic reviews met the inclusion criteria. For RDS, 1522 cases occurred in the control group composed of 8716 participants, while in the intervention group was 1088 in 8740 participants (RR = 0.67, 95% CI 0.60–0.75). For neonatal death, 343 cases occurred in 5248 participants of the control group, while in the intervention group, there were 227 cases in 5246 participants (RR = 0.66, 95% CI 0.56–0.78). For perinatal death, there were 344 cases in 3345 participants in the control group, while in the intervention group, the number of cases was 264 in 3384 participants (RR = 0.72, 95% CI 0.58–0.89). Thus, the use of corticosteroids during pregnancy in women at risk of preterm birth is effective for the prevention of RDS in neonates and reducing the number of neonatal and perinatal deaths in preterm. PROSPERO protocol no: CRD42017074604



Similar content being viewed by others
References
Goldenberg R, Culhane JF, Iams J, Romero R. Epidemiology and causes of preterm birth. Lancet. 2007;371:73–82.
Montenegro CAB, Rezende Filho J. (Org.). Rezende obstetrícia. 13. ed. Rio de Janeiro: Guanabara Koogan, 2017.
Iams JD, Berghella V. Care for women with prior preterm birth. Am J Obstet Gynecol. 2010;203(2):89–100.
Hamilton BE, Martin JA, Ventura SJ. Births: preliminary data for 2007. Natl Vital Stat Rep. 2009;12:1–23.
Hodek JM, von der Schulenburg JM, Mittendorf T. Measuring economic consequences of preterm birth-methodological recommendations for the evaluation of personal burden on children and their caregivers. Health economics reviews. 2011;1(1):6.
Nascimento Júnior FJM, da Silva JVF, Rodrigues APRA, Ferreira ALC. A síndrome do desconforto respiratório do recém-nascido: fisiopatologia e desafios assistenciais. Caderno de Graduação-Ciências Biológicas e da Saúde-UNIT-ALAGOAS. 2014;2(2):189–98.
Ramos JG, Urbanetz AA. Programa de Atualização em Ginecologia e Obstetrícia (PROAGO). Artmed/Panamericana: Porto Alegre; 2004.
Ballard PL, Ballard RA. Scientific basis and therapeutic regimens for use of antenatal glucocorticoids. Am J Obstet Gynecol. 1995;173:254–62.
Bornia RG, Costa Júnior IB, Amim Junior J. Protocolos assistenciais: Maternidade Escola da Universidade Federal do Rio de Janeiro: coletânea de artigos: anestesiologia, neonatologia, obstetrícia. Rio de Janeiro: Pod; 2013.
Roberts D, Dalziel S. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database Syst Rev. 2006 Jul;19(3):CD004454. https://doi.org/10.1002/14651858.CD004454.pub2.
Shea BJ, Grimshaw JM, Wells GA, Boers M, Andersson N, Hamel C, et al. Development of AMSTAR: a measurement tool to assess the methodological quality of systematic reviews. BMC Med Res Methodol. 2007;7(1):10.
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, et al. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 2008;336(7650):924–6.
Atkins D, Best D, Briss PA, Eccles M, Falck-Ytter Y, Flottorp S, et al. Grading quality of evidence and strength of recommendations. BMJ. 2004;328(7454):1490.
Iorio A, Spencer FA, Falavigna M, Alba C, Lang E, Burnand B, et al. Use of GRADE for assessment of evidence about prognosis: rating confidence in estimates of event rates in broad categories of patients. BMJ. 2015;350:870.
DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7(3):177–88.
Crowley P, Chalmers I, Keirse MJ. The effects of corticosteroid administration before preterm delivery: an overview of the evidence from controlled trials. BJOG Int J Obstet Gynaecol. 1990;97(1):11–25.
Crowley P. Corticosteroids after preterm premature rupture of membranes. Obstet Gynecol Clin N Am. 1992;19(2):317–26.
Harding JE, Pang JM, Knight DB, Liggins GC. Do antenatal corticosteroids help in the setting of preterm rupture of membranes? Am J Obstet Gynecol. 2001;184(2):131–9.
McLaughlin KJ, Crowther CA, Walker N, Harding JE. Effects of a single course of corticosteroids given more than 7 days before birth: a systematic review. Aust N Z J Obstet Gynaecol. 2003;43(2):101–6.
Mwansa-Kambafwile J, Cousens S, Hansen T, Lawn JE. Antenatal steroids in preterm labour for the prevention of neonatal deaths due to complications of preterm birth. Int J Epidemiol. 2010;39(1):122–33.
Roberge S, Lacasse Y, Tapp S, Tremblay Y, Kari A, Liu J, et al. Role of fetal sex in the outcome of antenatal glucocorticoid treatment to prevent respiratory distress syndrome: systematic review and meta-analysis. J Obstet Gynaecol Can. 2011 Mar;33(3):216–26.
Peltoniemi OM, Kari MA, Hallman M. Repeated antenatal corticosteroid treatment: a systematic review and meta-analysis. Acta Obstet Gynecol Scand. 2011;90(7):719–2. https://doi.org/10.1111/j.1600-0412.2011.01132.x.
Saccone G, Berghella V. Antenatal corticosteroids for maturity of term or near term fetuses: systematic review and meta-analysis of randomized controlled trials. BMJ. 2016;12:355–5044. https://doi.org/10.1136/bmj.i5044.
Roberts D, Brown J, Medley N, Dalziel SR. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database Syst Rev. 2017;3:Cd004454.
Sotiriadis A, Makrydimas G, Papatheodorou S, Ioannidis JP, McGoldrick E. Corticosteroids for preventing neonatal respiratory morbidity after elective caesarean section at term. Cochrane Database Syst Rev. 2018;8.
Drummond S, Souza TS, Lima FGD, Vieira AA. Correlação entre o uso de corticoterapia antenatal, a reanimação e a mortalidade de recém-nascidos prematuros de muito baixo peso. Rev Bras Ginecol Obstet. 2014;36(5):211–5.
Travers CP, Carlo WA, McDonald SA, Das A, Bell EF, Ambalavanan N, et al. Mortality and pulmonary outcomes of extremely preterm infants exposed to antenatal corticosteroids. Am J Obstet Gynecol. 2018;218(1):130–e1.
Meneguel JF, Guinsburg R, Miyoshi MH, Peres CDA, Russo RH, Kopelman BI, et al. Antenatal treatment with corticosteroids for preterm neonates: impact on the incidence of respiratory distress syndrome and intra-hospital mortality. Sao Paulo Med J. 2003;121(2):45–52.
Lassi ZS, Middleton PF, Crowther C, Bhutta ZA. Interventions to improve neonatal health and later survival: an overview of systematic reviews. EBioMedicine. 2015;2(8):985–1000.
Shahzad F, Umar N. Impact of antenatal corticosteroids on frequency and mortality due to respiratory distress syndrome in preterm neonates. Journal of Ayub Medical College Abbottabad. 2016;28(4):698–701.
Walfisch A, Hallak M, Mazor M. Multiple courses of antenatal steroids: risks and benefits. Obstet Gynecol. 2001;98(3):491–7.
Author information
Authors and Affiliations
Contributions
MLR Uggioni: Protocol/project development, data collection and management, data analysis, statistical analysis, and manuscript writing/editing. T Colonetti: Data collection or management, data analysis, and manuscript writing/editing. AJ Grande: Data collection or management, data analysis, and manuscript writing/editing. MVB Cruz: Manuscript writing/editing. MI Rosa: Protocol/project development, data collection or management, data analysis, statistical analysis, and manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Uggioni, M.L.R., Colonetti, T., Grande, A.J. et al. Corticosteroids in Pregnancy for Preventing RDS: Overview of Systematic Reviews. Reprod. Sci. 29, 54–68 (2022). https://doi.org/10.1007/s43032-020-00425-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43032-020-00425-x