Abstract
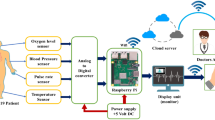
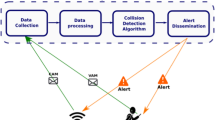
The advancement in telemedicine has been helpful in the development of smart healthcare in urban and rural areas. In India, however, this solution often falls short of connecting the remote villages with modern healthcare due to the difficulty in accessibility. In a developing country like India, consisting of geographically remote settlements, it is not feasible to provide infrastructure-based health support to all. To conquer this difficulty, an alternative solution is required in which the existing network infrastructure is not essential for the communication purposes. The main objective of this proposal is to provide an alternative approach for the transmission of health care related messages. It is also important to minimize the cost of this type of healthcare services by avoiding the establishment of communication network across the country. Here, we propose the framework of an IoT-based system to work as an aid for quicker diagnosis and health support for the remote villagers. We have used vehicular ad hoc network for cost-effective and fast data transportation, besides other advantages.










Similar content being viewed by others
References
2011. https://www.censusindia.gov.in/2011-prov-results/prov_results_paper1_india.html.
Gope P, Hwang T. BSN-care: a secure IoT-based modern healthcare system using body sensor network. IEEE Sens J. 2016;16:5. https://doi.org/10.1109/JSEN.2015.2502401.
Jansi R, Amutha R, Radha S. Remote monitoring of children with chronic illness using wearable vest, Telemedicine Technologies. In: book: Telemedicine Technologies, pp 121–137. 2019. https://doi.org/10.1016/B978-0-12-816948-3.00008-8.
Gopu G, Anitha T, Nagarajapandian M, Prabhakaran M. Investigation of telecardiology system to detect cardiac abnormalities. Telemed Technol. 2019;2019:43–55.
Wu T, Redouté J, Yuce M. An autonomous wireless body area network implementation towards IoT connected healthcare applications. IEEE Access. 2017;2017:5. https://doi.org/10.1109/ACCESS.2017.2716344.
Naranjo PGV, Shojafar M, Mostafaei H, Pooranian Z, Baccarelli E. P-SEP: a prolong stable election routing algorithm for energy-limited heterogeneous fog-supported wireless sensor networks. J Supercomput. 2017;73:733–55.
Saleh N, Kassem A, Haidar AM. Energy-efficient architecture for wireless sensor networks in healthcare applications. IEEE Access. 2018;6:6478–86.
Zhang H, Zhang H, Pirbhulal S, Wu W, Albuquerque VHCD. Active balancing mechanism for imbalanced medical data in deep learning-based classification models. ACM Trans Multimedia Comput Commun Appl. 2020;16:39–54.
Pirbhulal S, Samuel OW, Wu W, Sangaiah AK, Li G. A joint resource-aware and medical data security framework for wearable healthcare systems. Future Gener Comput Syst. 2019;95:382–91.
Am T, Dm W, Kb E, Ms M, Jc GGS. Telehealth: mapping the evidence for patient outcomes from systematic reviews. In: Technical Brief No. 26, AHRQ Publication No. 16-EHC034-EF, Rockville, MD: Agency for Healthcare Research and Quality; 2016.
McFarland S, Coufopolous A, Lycett D. The effect of telehealth versus usual care for home-care patients with long-term conditions: a systematic review, meta-analysis and qualitative synthesis. J Telemed Telecare. 2019. https://doi.org/10.1177/1357633X19862956.
Steventon A, Bardsley M, Billings J, Dixon J, Doll H, Hirani S. Effect of telehealth on use of secondary care and mortality: findings from the Whole System Demonstrator cluster randomized trial. BMJ. 2012;2012:344. https://doi.org/10.1136/bmj.e3874.
Versteeg H, Timmermans I, Widdershoven J, Kimman GJ, Prevot S, Rauwolf T. Effect of remote monitoring on patient- reported outcomes in european heart failure patients with an implantable cardioverter-defibrillator: primary results of the REMOTE-CIED randomized trial. Eurospace. 2019;21(9):1360–8. https://doi.org/10.1093/europace/euz140.
Guedon-Moreau L, Lacroix D, Sadout N, Clementy J, Kouakam C, Hermida JS. Costs of remote monitoring vs. ambulatory follow-ups of implanted cardioverter defibrillators in the randomized ECOST study. Europace. 2014;16(8):1181–8. https://doi.org/10.1093/europace/euu012.
HAS, Remote monitoring systems for automatic implantable cardiac defibrillators. 2017. https://www.has-sante.far//jcms/c.2790581/fr/systems-de-telesurveillance-pour-defibrillateurs-cardiaques-automatiques-implantables.
Hindricks G, Taborsky M, Glikson M, Heinrich U, Schumacher B, Katz A, et al. Implant-based multiparameter telemonitoring of patient with heart failure (in time); a randomized controlled trial. Lancet. 2014;384(9943):583–90. https://doi.org/10.1016/S0140-6736(14)61176-4.
Crossley GH, Boyle A, Vitense H, Chang Y, Mead RH. The CONNECT (Clinical Evaluation of Remote Notification to Reduce Time to Clinical Decision) trial: the value of wireless remote monitoring with automatic clinical alerts. J Am Coll Cardiol. 2011;57(10):1181–9. https://doi.org/10.1016/j.jacc.2010.12.012.
Guedon-Moreau L, Lacroix D, Sadoul N, Clementy J, Kouakam C, Hermids JS, et al. A randomized study of remote follow-up of implantable cardioverter defibrillators: safety and efficacy report of the ECOST trial. Eur Heart J. 2013;34(8):605–14. https://doi.org/10.1093/eurheartj/ehs425.
Crossley GH, Chen J, Choucair W, Cohen TJ, Gohn DC, Johnson WB, et al. Clinical benefit of remote versus trans telephonic monitoring of implanted pacemakers. J Am Coll Cardiol. 2009;54(22):2012–9. https://doi.org/10.1016/j.jacc.2009.10.001.
Varma N, Epstein AE, Irimpen A, Schweikert R, Love C. Efficacy and safety of automatic remote monitoring for implantable cardioverter-defibrillator follow-up: the Lumos-T Safely Reduces, Routine Office Device Follow-up (TRUST) trial. Circulation. 2010;122(4):325–32. https://doi.org/10.1161/CIRCULATIONAHA.110.937409.
Mabo P, Victor F, Bazin P, Ahres S, Baduty D, Da Costa A, et al. A randomized trial of long-term remote monitoring of pacemaker recipients (The COMPAS trial). Eur Heart J. 2012;33(9):1105–11. https://doi.org/10.1093/eurheartj/ehr419.
Amara W, Montagnier C, Cheggour S, Boursier M, Gully C, Barnay C, et al. Early detection and treatment of atrial arrhythmias alleviates the arrhythmic burden in paced patients: the SETAM study. Pacing Clin Electrophysiol. 2017;40(5):527–36. https://doi.org/10.1111/pace.13062.
Boriani G, Da Costa A, Ricci RP, Quesada A, Favale S, Iacopino S, et al. The MOnitoring Resynchronization dEvices and CARdiacpatiEnts (MORE-CARE) randomized controlled trial: phase 1 results on dynamics of early intervention with remote monitoring. J Med Internet Res. 2013;15(8):e167. https://doi.org/10.2196/jmir.2608.
Slotwiner D, Varma N, Akar JG, Annas G, Beardsall M, Fogel Rl, et al. HRS Expert Consensus Statement on remote interrogation and monitoring for cardiovascular implantable electronic devices. Heart Rhythm. 2015;12(7):e69-100. https://doi.org/10.1016/j.hrthm.2015.05.008 (Epub 2015 May 14).
White G. Active queue management in DOCSIS® 31 networks. IEEE Commun Mag. 2015;2015:0163-6804/15.
Khan I, Qureshi I, Shah SB, Akhlaq M, Safi E, et al. Comparative analysis and route optimization of state-of-the-art routing protocols. EAI Endorsed Trans Mobile Commun Appl. 2018;3:13. https://doi.org/10.4108/eai.22-3-2018.154385.
Barua M, Liang X, Lu R, et al. RCare: extending secure health care to rural area using VANETs. Mobile Netw Appl. 2014;19:318–30. https://doi.org/10.1007/s11036-013-0446-y.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the topical collection “Applications of Software Engineering and Tool Support” guest edited by Nabendu Chaki, Agostino Cortesi and Anirban Sarkar”.
Rights and permissions
About this article
Cite this article
DasGupta, S., Choudhury, S. & Chaki, R. VADiRSYRem: VANET-Based Diagnosis and Response System for Remote Locality. SN COMPUT. SCI. 2, 41 (2021). https://doi.org/10.1007/s42979-020-00430-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s42979-020-00430-6