Abstract
In this study, we prepared paclitaxel/chitosan (PTX/CS) nanosuspensions (NSs) with different mass ratios of PTX and CS (1.5:2, 2:2, and 2.5:2), for controlled drug delivery purposes. For attachment and dispersion in water medium, a simple ultrasonic disruption technique was employed. The water-dispersed PTX/CS NSs exhibited a rod-shape morphology with an average diameter of 170–210 nm and average length of about 1–10 µm. Transmission electron microscopy, differential scanning calorimetry and X-ray diffraction indicated that the obtained PTX/CS NSs contain a nanocrystalline PTX phase. It was also inferred that presence of CS can promotes the crystalline nature of PTX up to 80%. In addition, efficiency of PTX loading reached over 85% in freeze-dried PTX/CS NSs, showing a slow rate of drug release in vitro for 8 days. The MTT and LDH assessments revealed that PTX/CS NSs significantly inhibit the growth of tumor cells (HeLa), while it is slightly toxic for the normal cells (NIH/3T3). Therefore, PTX/CS NSs is suggested as a potential nanodrug delivery system for cancer therapy.
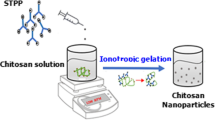
Graphic Abstract








Similar content being viewed by others
References
Merisko-Liversidge E, Liversidge GG, Cooper ER. Nanosizing: a formulation approach for poorly-water-soluble compounds. Eur J Pharm Sci. 2003;18:113–20.
Aungst BJ. Optimizing oral bioavailability in drug discovery: an overview of design and testing strategies and formulation options. J Pharm Sci. 2017;106:921–9.
Ting JM, Tale S, Purchel AA, Jones SD, Widanapathirana L, Tolstyka ZP, Guo L, Guillaudeu SJ, Bates FS, Reineke TM. High-throughput excipient discovery enables oral delivery of poorly soluble pharmaceuticals. ACS Cent Sci. 2016;2:748–55.
Siepmann J, Siepmann F, Florence AT. Factors influencing oral drug absorption and drug availability. In: Modern pharma, two volume set. 2016. p. 117.
Dening TJ, Rao S, Thomas N, Prestidge CA. Novel nanostructured solid materials for modulating oral drug delivery from solid-state lipid-based drug delivery systems. AAPS J. 2016;8:23–40.
Salunkhe SS, Bhatia NM, Mali SS, Thorat JD, Ahir AA, Hajare AA. Nanorobots: novel emerging technology in the development of pharmaceuticals for drug delivery applications. J Pharm Pharm Sci. 2014;6:4728–44.
Devadasu VR, Bhardwaj V, Kumar MR. Can controversial nanotechnology promise drug delivery? Chem Rev. 2013;113:1686–735.
Janousek S, Jirova D, Kejlova K, Dvorakova M. Nanoparticles in health and disease: an overview of nanomaterial hazard, benefit and impact on public health policy-current state and outlook. Front Clin Drug Res Hematol. 2015;2:176.
Wang L, Du J, Zhou Y, Wang Y. Safety of nanosuspensions in drug delivery. Nanomed Nanotechnol. 2017;13:455–69.
Charitidis CA, Georgiou P, Koklioti MA, Trompeta AF, Markakis V. Manufacturing nanomaterials: from research to industry. Manuf Rev. 2014;1:1–19.
Mane AN, Gilda SS, Ghadge AA, Bhosekar NR, Bhosale RR. Nanosuspension—a novel carrier for lipidic drug transfer. Sch Acad J Pharm. 2014;3:82–8.
Shah DA. To understand the thermodynamic and kinetic properties of nanocrystals using poorly soluble drugs. Long Island University. The Brooklyn Center. 2015.
Gadad AP, Kumar SV, Dandagi PM, Bolmol UB, Pallavi NP. Nanoparticles and their therapeutic applications in pharmacy. Int J Pharm Sci Nanotechnol. 2014;7:2515–6.
Chen L, Wang Y, Zhang J, Hao L, Guo H, Lou H, Zhang D. Bexarotene nanocrystal-oral and parenteral formulation development, characterization and pharmacokinetic evaluation. Eur J Pharm Biopharm. 2014;87:160–9.
Gao L, Liu G, Ma J, Wang X, Zhou L, Li X, Wang F. Application of drug nanocrystal technologies on oral drug delivery of poorly soluble drugs. Pharm Res. 2013;30:307–24.
Nedra Karunaratne D, Ariyarathna IR, Welideniya D, Siriwardhana A, Gunasekera D, Karunaratne V. Nanotechnological strategies to improve water solubility of commercially available drugs. Curr Nanomed. 2017;7:84–110.
Yadollahi R, Vasilev K, Simovic S. Nanosuspension technologies for delivery of poorly soluble drugs. J Nanomater. 2015;1:1–13.
Dening TJ, Rao S, Thomas N, Prestidge CA. Novel nanostructured solid materials for modulating oral drug delivery from solid-state lipid-based drug delivery systems. AAPS J. 2016;18:23–40.
Tuomela A, Saarinen J, Strachan CJ, Hirvonen J, Peltonen L. Production, applications and in vivo fate of drug nanocrystals. Drug Deliv Sci Technol. 2016;34:21–31.
Srivalli KMR, Mishra B. Drug nanocrystals: a way toward scale-up. Saudi Pharm J. 2016;24:386–404.
Parada-Bustamante A, Valencia C, Reuquén P, Díaz P, Rincion-Rodriguez R, A Orihuela P. Role of 2-methoxyestradiol, an endogenous estrogen metabolite, in health and disease. Mini Rev Med Chem. 2015;15:427–38.
Dranitsaris G, Yu B, Wang L, Sun W, Zhou Y, King J, Kaura S, Zhang A, Yuan P. Abraxane® versus Taxol® for patients with advanced breast cancer: a prospective time and motion analysis from a Chinese health care perspective. J Oncol Pharm Pract. 2016;22:205–11.
Wang Y, Song J, Chow SF, Chow AH, Zheng Y. Particle size tailoring of ursolic acid nanosuspensions for improved anticancer activity by controlled antisolvent precipitation. Int J Pharm. 2015;494:479–89.
Peltonen L, Tuomela A, Hirvonen J, Polymeric stabilizers for drug nanocrystals. In: Handbook of polymers for pharmaceutical technologies: bioactive and compatible synthetic/hybrid polymers, vol. 4. 2015. p. 67–87.
Loh ZH, Samanta AK, Heng PWS. Overview of milling techniques for improving the solubility of poorly water-soluble drugs. Asian J Pharm Sci. 2015;10:255–74.
Xia D, Gan Y, Cui F. Application of precipitation methods for the production of water-insoluble drug nanocrystals: production techniques and stability of nanocrystals. Curr Pharm Des. 2014;20:408–35.
Chaturvedi S, Dave PN. Design process for nanomaterials. J Mater Sci. 2013;48:3605–22.
Mohyeldin SM, Mehanna MM, Elgindy NA. The relevancy of controlled nanocrystallization on rifampicin characteristics and cytotoxicity. Int J Nanomed. 2016;11:2209.
Arunkumar N, Deecaraman M, Rani C. Nanosuspension technology and its applications in drug delivery. Asian J Pharm Sci. 2009;3:168.
Ruecroft G, Hipkiss D, Ly T, Maxted N, Cains PW. Sonocrystallization: the use of ultrasound for improved industrial crystallization. Org Process Res Dev. 2005;9:923–32.
Li H, Li H, Guo Z, Liu Y. The application of power ultrasound to reaction crystallization. Ultrason Sonochem. 2006;13:359–63.
Singh S, Dash AK. Paclitaxel in cancer treatment: perspectives and prospects of its delivery challenges. Crit Rev Ther Drug. 2009;26:333–72.
Crown J, O’leary M. The taxanes: an update. Lancet. 2000;355:1176–8.
Wang YS, Jiang Q, Li RS, Liu LL, Zhang QQ, Wang YM, Zhao J. Self-assembled nanoparticles of cholesterol-modified O-carboxymethyl chitosan as a novel carrier for paclitaxel. Nanotechnology. 2008;19:1–13.
Green MR, Manikhas GM, Orlov S, Afanasyev B, Makhson AM, Bhar P, Hawkins MJ. Abraxane®, a novel Cremophor®-free, albumin-bound particle form of paclitaxel for the treatment of advanced non-small-cell lung cancer. Ann Oncol. 2006;17:1263–8.
Henderson IC, Bhatia V. Nab-paclitaxel for breast cancer: a new formulation with an improved safety profile and greater efficacy. Expert Rev Anticancer Ther. 2007;2007(7):919–43.
Singla AK, Garg A, Aggarwal D. Paclitaxel and its formulations. Int J Pharm. 2002;235:179–92.
Ikada Y, Tsuji H. Biodegradable polyesters for medical and ecological applications. Macromol Rapid Commun. 2000;21:117–32.
Takeuchi H, Matsui Y, Sugihara H, Yamamoto H, Kawashima Y. Effectiveness of submicron-sized, chitosan-coated liposomes in oral administration of peptide drugs. Int J Pharm. 2005;303:160–70.
Wang F, Yang S, Hua D, Yuan J, Huang C, Gao Q. A novel preparation method of paclitaxcel-loaded folate-modified chitosan microparticles and in vitro evaluation. J Biomater Sci Polym E. 2016;27:276–89.
Lee E, Lee J, Lee IH, Yu M, Kim H, Chae SY, Jon S. Conjugated chitosan as a novel platform for oral delivery of paclitaxel. J Med Chem. 2008;51:6442–9.
Li F, Li J, Wen X, Li J, Wen X, Zhou S, Tong X, Su P, Li H, Shi D. Anti-tumor activity of paclitaxel-loaded chitosan nanoparticles: an in vitro study. Mater Sci Eng C. 2009;29:2392–7.
Liu Y, Wang R, Hou J, Sun B, Zhu B, Qiao Z, Su Y, Zhu X. Paclitaxel/chitosan nanosupensions provide enhanced intravesical bladder cancer therapy with sustained and prolonged delivery of paclitaxel. ACS Appl Bio Mater. 2018;1:1992–2001.
Tang J, Liu Y, Zhu B, Su Y, Zhu X. Preparation of paclitaxel/chitosan co-assembled core-shell nanofibers for drug-eluting stent. Appl Surf Sci. 2017;393:299–308.
Acknowledgements
This work is financially supported by National Natural Science Foundation of China (Grant No: 51373099) State Key Laboratory of open funds of China from Donghua University (LK1411).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflicts of interest to this work.
Rights and permissions
About this article
Cite this article
Liu, Y., Wu, F., Ding, Y. et al. Preparation and Characterization of Paclitaxel/Chitosan Nanosuspensions for Drug Delivery System and Cytotoxicity Evaluation In Vitro. Adv. Fiber Mater. 1, 152–162 (2019). https://doi.org/10.1007/s42765-019-00012-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42765-019-00012-z