Abstract
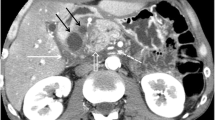
Isolated polycystic disease of the pancreas is a rare condition with few reported cases in the literature. It refers to multiple dysontogenetic, or congenital, cysts spanning the pancreas excluding those with inherited autosomal cystic diseases of abdominal organs, cystic fibrosis, and Von Hippen-Lindau disease with or without the involvement of cysts in other organs. These cystic lesions prove difficult to distinguish from those of neoplastic nature, including but not limited to intraductal papillary mucinous neoplasms, mucinous cystic neoplasms, and serous cystic neoplasms, potentially leading to unnecessary treatment. We report an incidental finding of the polycystic pancreas in a 73-year-old male upon CT for diverticulitis without any pancreas-related symptoms. A comprehensive collection of all reported cases of the isolated polycystic pancreas in the literature to date revealed that we report the oldest known patient to be diagnosed, as all other patients are between ages 13–62 with 64% being female. A thorough evaluation of the literature was completed and a diagnostic algorithm to diagnose IPDP was created to assist in the appropriate evaluation of these benign lesions to reduce the morbidity associated with unnecessary surgeries prompted by diagnostic uncertainty and the possibility of pre-malignant lesions.





Similar content being viewed by others
References
Mesutozturk M, Tumaybekci T, Muratdanaci M, Talatayyildiz T. Isolated polycystic pancreatic disease. Am J Diagn Imaging. 2018;4(1):24. https://doi.org/10.5455/ajdi.20180819103634.
Sonavane AD, Amarapurkar DN, Amarapurkar AD. Polycystic pancreas. ACG Case Rep J. 2016;3(1):199–201. https://doi.org/10.14309/crj.2016.49.
Kaestner KH. Of cilia and cysts: modeling pancreatic polycystic disease. Gastroenterology. 2006;130(3):926–8. https://doi.org/10.1053/j.gastro.2006.01.056.
Katsinelos P, Lazaraki G, Anastasiadis S. Isolated polycystic pancreatic disease: a very rare cause of pancreatic insufficiency. Clin Gastroenterol Hepatol. 2018;16(12):e121. https://doi.org/10.1016/j.cgh.2017.11.014.
Jain VK, Jain J, Singh R, Gupta S. Isolated polycystic disease of pancreas. Indian J Gastroenterol. 2016;35(3):250–1. https://doi.org/10.1007/s12664-016-0658-8.
Dhar DN, Suchi T, Sunny G, Dixit V. A rare isolated polycystic pancreatic disease. Radiation free diagnostic protocol in selected cases. Indian J Endocrinol Metab. 2012;16(6):1054. https://doi.org/10.4103/2230-8210.103044.
Lan C, Li X, Wang X, Hao J, Ren H. A new combined criterion to better predict malignant lesions in patients with pancreatic cystic neoplasms. Cancer Biol Med. 2018;15(1):70–8. https://doi.org/10.20892/j.issn.2095-3941.2017.0152.
Distler M, Aust D, Weitz J, Pilarsky C, Grützmann R. Precursor lesions for sporadic pancreatic cancer: PanIN, IPMN, and MCN. Biomed Res Int. 2014;2014:1–11. https://doi.org/10.1155/2014/474905.
Hocke M, Cui X, Domagk D, Ignee A, Dietrich C. Pancreatic cystic lesions: the value of contrast-enhanced endoscopic ultrasound to influence the clinical pathway. Endosc Ultrasound. 2014;3(2):123–30. https://doi.org/10.4103/2303-9027.131040.
Lariño-Noia J, Iglesias-Garcia J, De la Iglesia-Garcia D, Dominguez-Muñoz J. EUS-FNA in cystic pancreatic lesions: where are we now and where are we headed in the future? Endosc Ultrasound. 2018;7(2):102–9. https://doi.org/10.4103/eus.eus_93_17.
Kromrey M, Bülow R, Hübner J, Paperlein C, Lerch MM, Ittermann T, et al. Prospective study on the incidence, prevalence and 5-year pancreatic-related mortality of pancreatic cysts in a population-based study. Gut. 2017;67(1):138–45. https://doi.org/10.1136/gutjnl-2016-313127.
Badran A-MK, Fotiadou AK, Kays SK. Polycystic pancreatic disease associated with pineal cyst in an adolescent: a case report and literature overview. Clin Case Rep. 2017;5(10):1689–91. https://doi.org/10.1002/ccr3.1167.
Nygaard KK, Walters W. Polycystic disease of the pancreas (dysontogenetic cysts). Ann Surg. 1937;106(1):49–53. https://doi.org/10.1097/00000658-193707000-00006.
Klassen MG, Vetto JT, Reber HA. Congenital polycystic pancreas. Int J Pancreatol. 1990;7:405–8. https://doi.org/10.1007/BF02924466.
Casadei R, Campione O, Greco VM, Marrano D. Congenital true pancreatic cysts in young adults. Pancreas. 1996;12(4):419–21. https://doi.org/10.1097/00006676-199605000-00018.
Rodrigues-Pinto E, Pereira P, Macedo G. Dysontogenetic pancreatic cysts in a patient with a Wallenberg syndrome. Am J Gastroenterol. 2016;108:S246. https://doi.org/10.14309/00000434-201310001-00820.
Chowdhury MM, Ullah AA, Karim R, Sobhan SA, Mohammed S, Farmidi AA, et al. A rare case of polycystic disease of the pancreas. Mymensingh Med J. 2017;26(4):934–8.
Ufuk F, Tekinhatun M, Alver KH. Polycystic pancreas disease. J Pediatr Gastroenterol Nutr. 2017;1:1. https://doi.org/10.1097/00005176-900000000-96923.
Ghabi EM, El Asmar AR, Akl BJ, Saber TE, Abou-Malhab CA, El Rassi ZS. Polycystic disease of the pancreas. Am Surg. 2020:000313482095630. https://doi.org/10.1177/0003134820956303.
Elta GH, Enestvedt BK, Sauer BG, Lennon AM. ACG clinical guideline: diagnosis and management of pancreatic cysts. Am J Gastroenterol. 2018;113(4):464–79. https://doi.org/10.1038/ajg.2018.14.
Ngamruengphong S, Lennon AM. Analysis of pancreatic cyst fluid. Surg Pathol Clin. 2016;9(4):677–84. https://doi.org/10.1016/j.path.2016.05.010.
Sahani DV, Kambadakone A, Macari M, Takahashi N, Chari S, Castillo CF-D. Diagnosis and management of cystic pancreatic lesions. Am J Roentgenol. 2013;200(2):343–54. https://doi.org/10.2214/ajr.12.8862.
de Pretis N, Mukewar S, Aryal-Khanal A, Bi Y, Takahashi N, Chari S. Pancreatic cysts: diagnostic accuracy and risk of inappropriate resections. Pancreatology. 2017;17:267–72. https://doi.org/10.1016/j.pan.2017.01.002.
Jenssen C, Kahl S. Management of incidental pancreatic cystic lesions. Visc Med. 2015;31(1):14–24. https://doi.org/10.1159/000375282.
Chittiboina P, Lonser RR. Von Hippel–Lindau disease. Neurocutaneous syndromes handbook of clinical neurology; 2015. p. 139-156. https://doi.org/10.1016/b978-0-444-62702-5.00010-x
Cnossen WR, Morsche RH, Hoischen A, Gilissen C, Venselaar H, Mehdi S, et al. LRP5 variants may contribute to ADPKD. Eur J Hum Genet. 2015;24(2):237–42. https://doi.org/10.1038/ejhg.2015.86.
Farrell JJ. Prevalence, Diagnosis and management of pancreatic cystic neoplasms: current status and future directions. Gut Liver. 2015;9(5):571–89. https://doi.org/10.5009/gnl15063.
Gupta R, Singh AK, Verma P, Mistry K, Pokharia P. Polycystic disease of the pancreas: a case report. J Gastrointest Digest Syst. 2018;08(01). https://doi.org/10.4172/2161-069x.1000552.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Patient approval was obtained by universal consent and this retrospective study was approved by the Prisma Health Institutional Review Board and documented on Health Sciences South Carolina (Pro00103421)
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Surgery
Rights and permissions
About this article
Cite this article
Little, M., Desai, S., Schammel, C. et al. Polycystic Disease of the Pancreas: a Case Report and Comprehensive Review of the Literature. SN Compr. Clin. Med. 3, 1053–1061 (2021). https://doi.org/10.1007/s42399-021-00791-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42399-021-00791-w