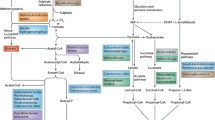
Abstract
Study of the interactions between the gut microbiota and brain-gut axis represents a very appealing approach to increasing our knowledge about the mechanisms leading to obesity and obesity-related diseases. The aim of this review is to focus on the effects of short-chain fatty acids (SCFAs), which are the main products of gut microbial fermentation from non-digestible carbohydrates in the colon, on the gut-brain axis. Evidence is accumulating regarding the role of SCFAs in the fine-tuning of the gut-brain axis, a feedback system which is vital not only for the proper maintenance of gastrointestinal and metabolic functions, but also for the regulation of food intake and energy expenditure. SCFAs are thought to play a key role in increasing the host capacity to harvest excess energy from the diet. SCFAs, however, can exert their effects on the host metabolism via multiple complementary pathways. Metabolic, inflammatory, and neural pathways can be regulated by SCFAs, which can act by sensing nutritional status, thereby maintaining body energy homeostasis. SCFA production from prebiotic consumption is the rationale for targeting intestinal mechanisms to increase energy expenditure and thereby reduce obesity risk.

Similar content being viewed by others
References
Eckburg PB, Bik EM, Bernstein CN et al (2005) Diversity of the human intestinal microbial flora. Science 308:1635–1638
Patterson E, Ryan PM, Cryan JF et al (2016) Gut microbiota, obesity and diabetes. Postgrad Med J 92:286–300
Backhed F, Ding H, Wang T et al (2004) The gut microbiota as an environmental factor that regulates fat storage. Proc Natl Acad Sci U S A 101:15718–15723
Turnbaugh PJ, Ley RE, Mahowald MA et al (2006) An obesity-associated gut microbiome with increased capacity for energy harvest. Nature 444:1027–1031
Muscogiuri G, Balercia G, Barrea L et al (2018) Gut: a key player in the pathogenesis of type 2 diabetes? Crit Rev Food Sci Nutr 58:1294–1309
Bohan R, Tianyu X, Tiantian Z et al (2018) Gut microbiota: a potential manipulator for host adipose tissue and energy metabolism. J Nutr Biochem 64:206–217
Gibson GR, Roberfroid MB (1995) Dietary modulation of the human colonic microbiota: introducing the concept of prebiotics. J Nutr 125:1401–1412
Wolever TM, Brighenti F, Royall D et al (1989) Effect of rectal infusion of short chain fatty acids in human subjects. Am J Gastroenterol 84:1027–1033
Rios-Covian D, Ruas-Madiedo P, Margolles A et al (2016) Intestinal short chain fatty acids and their link with diet and human health. Front Microbiol 7:185
Cani PD, Knauf C (2016) How gut microbes talk to organs: the role of endocrine and nervous routes. Mol Metab 5:743–752
Kasubuchi M, Hasegawa S, Hiramatsu T et al (2015) Dietary gut microbial metabolites, short-chain fatty acids, and host metabolic regulation. Nutrients 7:2839–2849
Cox LM, Yamanishi S, Sohn J et al (2014) Altering the intestinal microbiota during a critical developmental window has lasting metabolic consequences. Cell 158:705–721
Gao Z, Yin J, Zhang J et al (2009) Butyrate improves insulin sensitivity and increases energy expenditure in mice. Diabetes 58:1509–1517
Frost G, Sleeth ML, Sahuri-Arisoylu M et al (2014) The short-chain fatty acid acetate reduces appetite via a central homeostatic mechanism. Nat Commun 5:3611
Inoue D, Kimura I, Wakabayashi M et al (2012) Short-chain fatty acid receptor GPR41-mediated activation of sympathetic neurons involves synapsin 2b phosphorylation. FEBS Lett 586:1547–1554
De Vadder F, Kovatcheva-Datchary P, Goncalves D et al (2014) Microbiota-generated metabolites promote metabolic benefits via gut-brain neural circuits. Cell 156:84–96
Kimura I, Ozawa K, Inoue D et al (2013) The gut microbiota suppresses insulin-mediated fat accumulation via the short-chain fatty acid receptor GPR43. Nat Commun 4:1829
Maslowski KM, Vieira AT, Ng A et al (2009) Regulation of inflammatory responses by gut microbiota and chemoattractant receptor GPR43. Nature 461:1282–1286
Ge H, Li X, Weiszmann J et al (2008) Activation of G protein-coupled receptor 43 in adipocytes leads to inhibition of lipolysis and suppression of plasma free fatty acids. Endocrinology 149:4519–4526
Ferrarese R, Ceresola ER, Preti A et al (2018) Probiotics, prebiotics and synbiotics for weight loss and metabolic syndrome in the microbiome era. Eur Rev Med Pharmacol Sci 22:7588–7605
Ropert A, Cherbut C, Roze C et al (1996) Colonic fermentation and proximal gastric tone in humans. Gastroenterology 111:289–296
Kellow NJ, Coughlan MT, Reid CM (2014) Metabolic benefits of dietary prebiotics in human subjects: a systematic review of randomised controlled trials. Br J Nutr 111:1147–1161
Nohr MK, Pedersen MH, Gille A et al (2013) GPR41/FFAR3 and GPR43/FFAR2 as cosensors for short-chain fatty acids in enteroendocrine cells vs FFAR3 in enteric neurons and FFAR2 in enteric leukocytes. Endocrinology 154:3552–3564
Verbeke KA, Boobis AR, Chiodini A et al (2015) Towards microbial fermentation metabolites as markers for health benefits of prebiotics. Nutr Res Rev 28:42–66
Zhu X, Han Y, Du J et al (2017) Microbiota-gut-brain axis and the central nervous system. Oncotarget 8:53829–53838
Sam AH, Troke RC, Tan TM et al (2012) The role of the gut/brain axis in modulating food intake. Neuropharmacology 63:46–56
Ahlman H, Nilsson (2001) The gut as the largest endocrine organ in the body. Ann Oncol 12(Suppl 2):S63–S68
Dahiya DK, Renuka PM et al (2017) Gut microbiota modulation and its relationship with obesity using prebiotic fibers and probiotics: a review. Front Microbiol 8:563
Cani PD, Dewever C, Delzenne NM (2004) Inulin-type fructans modulate gastrointestinal peptides involved in appetite regulation (glucagon-like peptide-1 and ghrelin) in rats. Br J Nutr 92:521–526
Engelstoft MS, Park WM, Sakata I et al (2013) Seven transmembrane G protein-coupled receptor repertoire of gastric ghrelin cells. Mol Metab 2:376–392
Barazzoni R (2014) Ghrelin and insulin secretion in humans: not a tale of two hormones? Diabetes 63:2213–2215
Tolhurst G, Heffron H, Lam YS et al (2012) Short-chain fatty acids stimulate glucagon-like peptide-1 secretion via the G-protein-coupled receptor FFAR2. Diabetes 61:364–371
Cani PD, Hoste S, Guiot Y et al (2007) Dietary non-digestible carbohydrates promote L-cell differentiation in the proximal colon of rats. Br J Nutr 98:32–37
Brooks L, Viardot A, Tsakmaki A et al (2017) Fermentable carbohydrate stimulates FFAR2-dependent colonic PYY cell expansion to increase satiety. Mol Metab 6:48–60
Anastasovska J, Arora T, Sanchez Canon GJ et al (2012) Fermentable carbohydrate alters hypothalamic neuronal activity and protects against the obesogenic environment. Obesity (Silver Spring, Md) 20:1016–1023
O'Malley D (2018) Endocrine regulation of gut function - a role for glucagon-like peptide-1 in the pathophysiology of irritable bowel syndrome. Exp Physiol
Li ZY, Zhang N, Wen S et al (2017) Decreased glucagon-like peptide-1 correlates with abdominal pain in patients with constipation-predominant irritable bowel syndrome. Clin Res Hepatol Gastroenterol 41:459–465
Hustoft TN, Hausken T, Ystad SO et al (2017) Effects of varying dietary content of fermentable short-chain carbohydrates on symptoms, fecal microenvironment, and cytokine profiles in patients with irritable bowel syndrome. Neurogastroenterol Motil 29
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Barrea, L., Muscogiuri, G., Annunziata, G. et al. From gut microbiota dysfunction to obesity: could short-chain fatty acids stop this dangerous course?. Hormones 18, 245–250 (2019). https://doi.org/10.1007/s42000-019-00100-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42000-019-00100-0