Abstract
Purpose
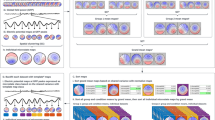
As depression has been a major contributor to the global disease burden, objective and effective computer-aided diagnosis has become an urgent problem. This study aims to assess the frontal asymmetry variation of alpha electroencephalography (EEG) in different severity depression patients and to find promising biomarkers for future depression recognition.
Methods
Three-channel EEG signals from 69 depression patients (divided into three groups according to illness severity) and 14 healthy subjects were collected. Except for cross-sample entropy (CSEn), two new asymmetry indexes (Asy_SEn and Asy_LZC) based on complexity measures were proposed to quantify the difference among the four groups. One-way ANOVA was used to test the difference among all four groups, followed by the group t-test to test the difference between each two groups.
Results
All indexes show significantly increased frontal alpha asymmetry in depressive groups compared with the healthy group, and the asymmetry keeps increasing as the depression deepens. The Asy_LZC value of the confirmed depression group (0.0015 ± 0.0008) is substantially higher than the other three groups (−0.0010 ± 0.0008, −0.0006 ± 0.0008, and −0.0007 ± 0.0006). And the Asy_SEn value of the healthy group (−0.0023 ± 0.0007) is significantly lower than the two depressive groups (0.0001 ± 0.0005 and 0.0007 ± 0.0007). All healthy CSEn between each two channels is considerably lower than depressive groups with p < 0.01.
Conclusion
This study confirms the increased frontal alpha asymmetry in depression patients and suggests that two new indexes could be promising biomarkers in future clinical depression detection.



Similar content being viewed by others
References
Organization, W.H. (2017). Depression and other common mental disorders, global health estimates. World Health Organization.
Organization, W.H. (2019). Depression. 2019. Retrieved May 30, 2020, from https://www.who.int/news-room/fact-sheets/detail/depression
Beeney, J. E., Levy, K. N., Gatzke-Kopp, L. M., & Hallquist, M. N. (2014). EEG asymmetry in borderline personality disorder and depression following rejection. Personal Disord, 5, 178–185. https://doi.org/10.1037/per0000032.
Debener, S., Beauducel, A., Nessler, D., Brocke, B., Heilemann, H., & Kayser, J. (2000). Is resting anterior EEG alpha asymmetry a trait marker for depression? Findings for healthy adults and clinically depressed patients. Neuropsychobiology, 41, 31–37. https://doi.org/10.1159/000026630.
Stewart, J. L., Bismark, A. W., Towers, D. N., Coan, J. A., & Allen, J. J. B. (2010). Resting frontal EEG asymmetry as an endophenotype for depression risk: Sex-specific patterns of frontal brain asymmetry. Journal of Abnormal Psychology, 119, 502–512. https://doi.org/10.1037/a0019196.
Smit, D. J., Posthuma, D., Boomsma, D. I., & De Geus, E. J. (2007). The relation between frontal EEG asymmetry and the risk for anxiety and depression. Biological Psychology, 74, 26–33. https://doi.org/10.1016/j.biopsycho.2006.06.002.
Bruder, G. E., Stewart, J. W., & McGrath, P. J. (2017). Right brain, left brain in depressive disorders: Clinical and theoretical implications of behavioral, electrophysiological and neuroimaging findings. Neuroscience and Biobehavioral Reviews, 78, 178–191. https://doi.org/10.1016/j.neubiorev.2017.04.021.
van der Vinne, N., Vollebregt, M. A., van Putten, M., & Arns, M. (2017). Frontal alpha asymmetry as a diagnostic marker in depression: Fact or fiction? A meta-analysis. Neuroimage Clinical, 16, 79–87. https://doi.org/10.1016/j.nicl.2017.07.006.
Gold, C., Fachner, J., & Erkkila, J. (2013). Validity and reliability of electroencephalographic frontal alpha asymmetry and frontal midline theta as biomarkers for depression. Scandinavian Journal of Psychology, 54, 118–126. https://doi.org/10.1111/sjop.12022.
Kaiser, A. K., Doppelmayr, M., & Iglseder, B. (2016). Electroencephalogram alpha asymmetry in geriatric depression: Valid or vanished? Ztschrift Fur Gerontologie Und Geriatrie, 51, 1–6. https://doi.org/10.1007/s00391-016-1108-z.
Chang, J. S., Yoo, C. S., Yi, S. H., Her, J. Y., Choi, H. M., Ha, T. H., Park, T., & Ha, K. (2012). An integrative assessment of the psychophysiologic alterations in young women with recurrent major depressive disorder. Psychosomatic Medicine, 74, 495–500. https://doi.org/10.1097/PSY.0b013e31824d0da0.
Acharya, U. R., Sudarshan, V. K., Adeli, H., Santhosh, J., Koh, J. E., Puthankatti, S. D., & Adeli, A. (2015). A novel depression diagnosis index using nonlinear features in EEG signals. European Neurology, 74, 79–83. https://doi.org/10.1159/000438457.
Acharya, U. R., Sudarshan, V. K., Adeli, H., Santhosh, J., Koh, J. E., & Adeli, A. (2015). Computer-aided diagnosis of depression using EEG signals. European Neurology, 73, 329–336. https://doi.org/10.1159/000381950.
Faust, O., Ang, P. C. A., Puthankattil, S. D., & Joseph, P. K. (2014). Depression diagnosis support system based on EEG signal entropies. Journal of Mechanics in Medicine and Biology, 14, 1450035. https://doi.org/10.1142/s0219519414500353.
Richman, J. S., & Moorman, J. R. (2000). Physiological time-series analysis using approximate entropy and sample entropy. American Journal of Physiology. Heart and Circulatory Physiology, 278, 2039–2049. https://doi.org/10.1152/ajpheart.2000.278.6.H2039.
Bachmann, M., Paeske, L., Kalev, K., Aarma, K., Lehtmets, A., Oopik, P., Lass, J., & Hinrikus, H. (2018). Methods for classifying depression in single channel EEG using linear and nonlinear signal analysis. Computer Methods and Programs in Biomedicine, 155, 11–17. https://doi.org/10.1016/j.cmpb.2017.11.023.
Li, Y., Tong, S., Liu, D., Gai, Y., Wang, X., Wang, J., Qiu, Y., & Zhu, Y. (2008). Abnormal EEG complexity in patients with schizophrenia and depression. Clinical Neurophysiology, 119, 1232–1241. https://doi.org/10.1016/j.clinph.2008.01.104.
Zhang, Z. (2005). Emotion evaluation. In Behavioral medicine scale manual (p. 223). China: China Medical Electronic Audio and Video Publishing House.
Zhao, L., Yang, L., Su, Z., & Liu, C. (2019). Cardiorespiratory coupling analysis based on entropy and cross-entropy in distinguishing different depression stages. Frontiers in Physiology, 10, 359.351–359.314. https://doi.org/10.3389/fphys.2019.00359.
Cukic, M., Pokrajac, D., Stokic, M., Simic, S., Radivojevic, V., & Ljubisavljevic, M. (2018). EEG machine learning with Higuchi fractal dimension and sample entropy as features for successful detection of depression. Cognitive Neurodynamics, 14, 443–455. https://doi.org/10.1007/s11571-020-09581-x.
Zhao, L., Wei, S., Zhang, C., Zhang, Y., Jiang, X., Liu, F., & Liu, C. (2015). Determination of sample entropy and fuzzy measure entropy parameters for distinguishing congestive heart failure from normal sinus rhythm subjects. Entropy, 17, 6270–6288. https://doi.org/10.3390/e17096270.
Lempel, A., & Ziv, J. (1976). On the complexity of finite sequence.pdf. IEEE Transactions on Information Theory, 22, 75–81. https://doi.org/10.1109/tit.1976.1055501.
Zhao, L., Yang, L., Li, B., Su, Z., & Liu, C. (2020). Frontal alpha complexity of different severity depression patients. Journal of Healthcare Engineering, 2020, 8854725. https://doi.org/10.1155/2020/8854725.
Kaspar, F., & Schuster, H. G. (1987). Easily calculable measure for the complexity of spatiotemporal patterns. Physical Review A: General Physics, 36, 842–848. https://doi.org/10.1103/physreva.36.842.
Berger, S., Boettger, M. K., Tancer, M., Guinjoan, S. M., Yeragani, V. K., & Bar, K. J. (2010). Reduced cardio-respiratory coupling indicates suppression of vagal activity in healthy relatives of patients with schizophrenia. Progress in Neuro-Psychopharmacology & Biological Psychiatry, 34, 406–411. https://doi.org/10.1016/j.pnpbp.2010.01.009.
Liu, C., Zhang, C., Zhang, L., Zhao, L., Liu, C., & Wang, H. (2015). Measuring synchronization in coupled simulation and coupled cardiovascular time series: A comparison of different cross entropy measures. Biomedical Signal Processing and Control, 21, 49–57. https://doi.org/10.1016/j.bspc.2015.05.005.
Ahern, G. L., Sollers, J. J., Lane, R. D., Labiner, D. M., Herring, A. M., Weinand, M. E., Hutzler, R., & Thayer, J. F. (2001). Heart rate and heart rate variability changes in the intracarotid sodium amobarbital test. Epilepsia, 42, 912–921. https://doi.org/10.1046/j.1528-1157.2001.042007912.x.
Hilz, M. J., Matthias Dütsch, M. D., Perrine, K., Nelson, P. K., & Orrin Devinsky, M. D. (2001). Hemispheric influence on autonomic modulation and baroreflex sensitivity. Annals of Neurology, 49, 575–584. https://doi.org/10.1002/ana.1006.
Paniccia, M., Paniccia, D., Thomas, S., Taha, T., & Reed, N. (2017). Clinical and non-clinical depression and anxiety in young people: A scoping review on heart rate variability. Autonomic Neuroscience, 208, 1–14. https://doi.org/10.1016/j.autneu.2017.08.008.
Chen, X., Yang, R., Kuang, D., Zhang, L., Lv, R., Huang, X., Wu, F., Lao, G., & Ou, S. (2017). Heart rate variability in patients with major depression disorder during a clinical autonomic test. Psychiatry Research, 256, 207–211. https://doi.org/10.1016/j.psychres.2017.06.041.
Acknowledgements
The authors appreciate the psychiatrists and nurses from the Second Affiliated Hospital of Jining Medical College, for their long time help in patients’ data collection. We also thank the support from the Southeast–Lenovo Wearable Heart-Sleep-Emotion Intelligent Monitoring Lab.
Funding
This research was funded by the Shandong Province Natural Science Foundation (ZR2018FM027), the Key Research and Development Project of Shandong Province (2016GSF120009), the National Key Research and Development Program of China (2019YFE0113800), the Distinguished Young Scholars of Jiangsu Province (BK20190014) and the National Natural Science Foundation of China (81871444).
Author information
Authors and Affiliations
Contributions
Conceptualization, LY and CL; Data curation, LZ, BL and ZS; Formal analysis, LZ; Funding acquisition, LY and CL; Investigation, LZ and CL; Methodology, LZ; Project administration, CL; Resources, LY and CL; Software, LZ; Supervision, LY and CL; Validation, LZ, LY, and BL; Writing—original draft, LZ; Writing—review & editing, LY and CL.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare no conflict of interest.
Ethical Approval
The protocol of this study was approved by the Ethics Committee of the Second Affiliated Hospital of Jining Medical College.
Informed Consent
Written informed consent was given by all participants in accordance with the Declaration of Helsinki.
Rights and permissions
About this article
Cite this article
Zhao, L., Yang, L., Li, B. et al. Frontal Alpha EEG Asymmetry Variation of Depression Patients Assessed by Entropy Measures and Lemple–Ziv Complexity. J. Med. Biol. Eng. 41, 146–154 (2021). https://doi.org/10.1007/s40846-020-00594-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40846-020-00594-9