Abstract
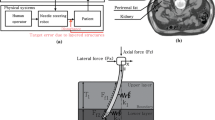
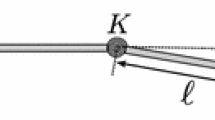
Accurate estimation of needle deflection is necessary to successfully steer the needle to targets located deep inside the body. In particular, the deflection that occurs until the tissue surface is breached differs according to the tissue shape and stiffness. This topic has not been a focus of previous work. In the present paper, we propose a model with which to estimate the needle deflection that occurs until breaching of the tissue surface with consideration of the tissue shape and stiffness. This model comprises a cantilever beam supported by virtual springs that represent the interaction forces between the needle tip and tissue surface. The effects of different insertion angles and tissue stiffness on needle deflection are represented by changing the spring constants. The model was used in experiments involving four different insertion angles (0º, 15º, 30º, and 45º) and three different polyvinyl chloride (PVC) phantoms with different stiffness (100, 75, and 50%). We verified the proposed model with the 80% PVC phantom and showed a maximum error of 0.04 mm.
















Similar content being viewed by others
References
Moreira, P., & Misra, S. (2014). Biomechanics-based curvature estimation for ultrasound-guided flexible needle steering in biological tissues. Annals of Biomedical Engineering. https://doi.org/10.1007/s10439-014-1203-5.
Majewicz, A., Marra, S., van Vledder, M., Lin, M., Choti, M., Song, D., et al. (2012). Behavior of tip-steerable needles in ex vivo and in vivo tissue. IEEE Transactions on Biomedical Engineering, 59, 2705–2715.
Abayazid, M., Roesthuis, R. J., Reilink, R., & Misra, S. (2013). Integrating deflection models and image feedback for real-time flexible needle steering. IEEE Transactions on Robotics, 29, 542–553.
Vrooijink, G., & Abayazid, M. (2014). Needle path planning and steering in a three-dimensional non-static environment using two-dimensional ultrasound images. International Journal of Robotics Research, 33, 1361–1374.
Abolhassani, N., Patel, R., & Moallem, M. (2007). Needle insertion into soft tissue: A survey. Medical Engineering and Physics, 29, 413–431.
Okamura, A. M., Simone, C., & O’Leary, M. D. (2004). Force modeling for needle insertion into soft tissue. IEEE Transactions on Biomedical Engineering, 51, 1707–1716.
Asadian, A., Patel, R. V., & Kermani, M. R. (2014). Dynamics of translational friction in needle-tissue interaction during needle insertion. Annal of Biomedical Engineering, 42, 73–85.
Khadem, M., Rossa, C., Sloboda, R. S., Usmani, N., & Tavakoli, M. (2016). Mechanics of tissue cutting during needle insertion in biological tissue. IEEE Robotics and Automation Letter, 1, 800–807.
Barbé, L., Bayle, B., De Mathelin, M., & Gangi, A. (2007). Needle insertions modelling: Identifiability and limitations. Biomedical Signal Processing and Control, 2, 191–198.
van Gerwen, D. J., Dankelman, J., & van den Dobbelsteen, J. J. (2012). Needle–tissue interaction forces: A survey of experimental data. Medical Engineering and Physics, 34, 665–680.
Webster, R. J., III, Cowan, N. J., Chirikjian, G. S., & Okamura, M. (2006). Nonholonomic modelling of needle steering. International Journal of Robotics Research, 25, 509–525.
Yan, K., Ng, W., Ling, K., Yu, Y., Podder, T., Liu, T., & Cheng C. (2006). Needle steering modeling and analysis using unconstrained modal analysis. Proceedings of First IEEE/RAS-EMBS International Conference Biomedical Robotics and Biomechatronics (BioRob). https://doi.org/10.1109/BIOROB.2006.1639065
Khadem, M., Fallahi, B., Rossa, C., Sloboda, R., Usmani, N., & Tavakoli, M. (2015). A mechanics-based model for simulation and control of flexible needle insertion in soft tissue. Proceedings of IEEE International Conference on Robotics and Automation (pp. 2264–2269). https://doi.org/10.1109/ICRA.2015.7139499
Misra, S., Reed, K. B., Schafer, B. W., Ramesh, K. T., & Okamura, M. (2010). Mechanics of flexible needles robotically steered through soft tissue. International Journal of Robotics Research, 29, 1640–1660.
DiMaio, S. P., & Salcudean, S. E. (2005). Interactive simulation of needle insertion models. IEEE Transactions on Biomedical Engineering, 52, 1167–1179.
Goksel, O., Dehghan, E., & Salcudean, S. E. (2009). Modeling and simulation of flexible needles. Medical Engineering and Physics, 31, 1069–1078.
Alterovitz, R., Goldberg, K., & Okamura, A. (2005). Planning for steerable bevel-tip needle insertion through 2D soft tissue with obstacles. Proceedings of IEEE International Conference on Robotics and Automation (pp. 1640–1645). https://doi.org/10.1109/ROBOT.2005.1570348
Yamaguchi, S., Tsutsui, K., Satake, K., Morikawa, S., Shirai, Y., & Tanaka, H. (2014). Dynamic analysis of a needle insertion for soft materials: Arbitrary Lagrangian–Eulerian-based three-dimensional finite element analysis. Computers in Biology and Medicine, 53, 42–47.
Rossa, C., Khadem, M., Sloboda, R., Usmani, N., & Tavakoli, M. (2016). Adaptive quasi-static modelling of needle deflection during steering in soft tissue. IEEE Robotics and Automation Letter, 1, 916–923.
Assaad, W., Jahya, A., Moreira, P., & Misra, S. (2015). Finite-element modeling of a bevel-tipped needle interacting with gel. Journal of Mechanics in Medicine and Biology, 15, 1550079-1–1550079-15.
Barnett, A. C., Lee, Y.-S., & Moore, J. Z. (2015). Fracture mechanics model of needle cutting tissue. Journal of Manufacturing Science and Engineering, 138, 011005-1–011005-8.
Misra, S., Macura, K. J., Ramesh, K. T., & Okamura, A. M. (2009). The importance of organ geometry and boundary constraints for planning of medical interventions. Medical Engineering and Physics, 31, 195–206.
Jahya, A., Schouten, M. G., Fütterer, J. J., & Misra, S. (2012). On the importance of modelling organ geometry and boundary conditions for predicting three-dimensional prostate deformation. Computer Methods in Biomechanics and Biomedical Engineering. https://doi.org/10.1080/10255842.2012.694876.
Roesthuis, R. J., van Veen, Y. R. J., Jahya, A., & Misra, S. (2011). Mechanics of needle-tissue interaction. Proceedings of IEEE/RSJ International Conference Intelligent Robots and Systems (pp. 2557–2563). https://doi.org/10.1109/IROS.2011.6048612
Lee, H., & Kim, J. (2014). Estimation of flexible needle deflection in layered soft tissues with different elastic moduli. Medical and Biological Engineering and Computing, 52, 729–740. https://doi.org/10.1007/s11517-014-1173-7.
Mahvash, M., & Dupont, P. E. (2009). Fast needle insertion to minimize tissue deformation and damage. Proceedings of IEEE International Conference on Robotics and Automation (pp. 3097–3102). https://doi.org/10.1109/ROBOT.2009.5152617
Elgezua, I., Kobayashi, Y., & Fujie, M. G. (2014). Estimation of needle tissue interaction based on non-linear elastic modulus and friction force patterns. Proceedings of IEEE/RSJ International Conference on Intelligent Robots and Systems (pp. 4315–4320). https://doi.org/10.1109/IROS.2014.6943172
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tsumura, R., Miyashita, T. & Iwata, H. Mechanical-Based Model for Extra-Fine Needle Tip Deflection Until Breaching of Tissue Surface. J. Med. Biol. Eng. 38, 697–706 (2018). https://doi.org/10.1007/s40846-017-0359-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40846-017-0359-5