Abstract
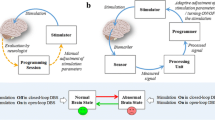
Traumatic brain injury (TBI) typically causes permanent brain tissue damage, which leads to permanent severe voiding dysfunction. Urinary retention is often refractory to standard therapies, and most patients require self-catheterization, which results in frequent urinary tract infections and reduces quality of life. Deep brain stimulation (DBS) might be a feasible alternative approach for treating bladder disorders in patients with TBI. In this study, we developed a DBS system with a closed-loop control strategy and determined the feasibility of this DBS system for improving bladder voiding function in a TBI animal model. A prototype of the DBS system was designed, fabricated and integrated with a closed-loop control algorithm based on the real-time external urethral sphincter-electromyogram feedback. A series of animal experiments was conducted to determine whether the feedback algorithm accurately detects the bladder status during cystometric measurements. Subsequent animal experiments were conducted to implement this DBS system and determine the performance of the closed-loop strategy for improving bladder functions in the TBI animal model. We successfully implemented a closed-loop algorithm for DBS control, and the accuracy of the bladder voiding phase detection was > 90%. Our system significantly improved the voiding efficiency in TBI rats from 22 to 74%. Although the prototype of the DBS feedback system was fabricated with surface-mounted device components and mounted on a 3D printed circuit board, the design principles and animal experience gathered from this research can serve as a basis for developing a new implantable bladder controller in the future.










Similar content being viewed by others
References
Faul, M., Xu, L., Wald, M. M., & Coronado, V. (2010). Traumatic brain injury in the United States. Atlanta, GA: National Center for injury Prevention and Control, Centers for disease Control and Prevention.
Prins, M., Greco, T., Alexander, D., & Giza, C. C. (2013). The pathophysiology of traumatic brain injury at a glance. Disease Models and Mechanisms, 6(6), 1307–1315.
Maas, A. I., Stocchetti, N., & Bullock, R. (2008). Moderate and severe traumatic brain injury in adults. The Lancet Neurology, 7(8), 728–741.
Burks, F. N., Bui, D. T., & Peters, K. M. (2010). Neuromodulation and the neurogenic bladder. Urologic Clinics of North America, 37(4), 559–565.
Masel, B. E., & DeWitt, D. S. (2010). Traumatic brain injury: A disease process, not an event. Journal of Neurotrauma, 27(8), 1529–1540.
Oostra, K., Everaert, K., & Van Laere, M. (1996). Urinary incontinence in brain injury. Brain Injury, 10(6), 459–464.
Moiyadi, A. V., Devi, B. I., & Nair, K. (2007). Urinary disturbances following traumatic brain injury: Clinical and urodynamic evaluation. NeuroRehabilitation, 22(2), 93–98.
Moody, B. J., Liberman, C., Zvara, P., Smith, P. P., Freeman, K., & Zvarova, K. (2014). Acute lower urinary tract dysfunction (LUTD) following traumatic brain injury (TBI) in rats. Neurourology and Urodynamics, 33(7), 1159–1164.
Aboseif, S., Tamaddon, K., Chalfin, S., Freedman, S., Mourad, M., Chang, J., et al. (2002). Sacral neuromodulation in functional urinary retention: An effective way to restore voiding. BJU International, 90(7), 662–665.
Lin, Y.-T., Lai, C.-H., Kuo, T.-S., Chen, C.-C., Chen, Y.-L., Young, S.-T., et al. (2014). Dual-channel neuromodulation of pudendal nerve with closed-loop control strategy to improve bladder functions. J Med Biol Eng, 34(34), 82–89.
Abd-Elfattah Foda, M. A., & Marmarou, A. (1994). A new model of diffuse brain injury in rats: Part II: Morphological characterization. Journal of Neurosurgery, 80(2), 301–313.
Marmarou, A., Foda, M. A. A.-E., Brink, W. V. D., Campbell, J., Kita, H., & Demetriadou, K. (1994). A new model of diffuse brain injury in rats: Part I: Pathophysiology and biomechanics. Journal of Neurosurgery, 80(2), 291–300.
Hsieh, T.-H., Huang, Y.-Z., Chen, J.-J. J., Rotenberg, A., Chiang, Y.-H., Chien, W.-S. C., et al. (2015). Novel use of theta burst cortical electrical stimulation for modulating motor plasticity in rats. Journal of Medical and Biological Engineering, 35(1), 62–68.
Blok, B. F., & Holstege, G. (1997). Ultrastructural evidence for a direct pathway from the pontine micturition center to the parasympathetic preganglionic motoneurons of the bladder of the cat. Neuroscience Letters, 222(3), 195–198.
Blok, B. F., & Holstege, G. (2000). The pontine micturition center in rat receives direct lumbosacral input. An ultrastructural study. Neuroscience Letters, 282(1), 29–32.
Nishijima, S., Sugaya, K., Miyazato, M., Shimabukuro, S., Morozumi, M., & Ogawa, Y. (2005). Activation of the rostral pontine reticular formation increases the spinal glycine level and inhibits bladder contraction in rats. The Journal of Urology, 173(5), 1812–1816.
Noto, H., Roppolo, J., Steers, W., & De Groat, W. (1989). Excitatory and inhibitory influences on bladder activity elicited by electrical stimulation in the pontine micturition center in the rat. Brain Research, 492(1), 99–115.
Kimura, Y., Ukai, Y., Kimura, K., Sugaya, K., & Nishizawa, O. (1995). Inhibitory influence from the nucleus reticularis pontis oralis on the micturition reflex induced by electrical stimulation of the pontine micturition center in cats. Neuroscience Letters, 195(3), 214–216.
Noto, H., Roppolo, J., Steers, W., & De Groat, W. (1991). Electrophysiological analysis of the ascending and descending components of the micturition reflex pathway in the rat. Brain Research, 549(1), 95–105.
Fan, W.-J., Li, Y.-T., Chen, J.-J. J., Chen, S.-C., Lin, Y. S., Kou, Y. R., et al. (2013). Sexually dimorphic urethral activity in response to pharmacological activation of 5-HT1A receptors in the rat. American Journal of Physiology-Renal Physiology, 305(9), F1332–F1342.
Hsieh, T.-H., Lin, Y.-T., Chen, S.-C., & Peng, C.-W. (2016). Chronic pudendal neuromodulation using an implantable microstimulator improves voiding function in diabetic rats. Journal of Neural Engineering, 13(4), 046001.
Opisso, E., Borau, A., & Rijkhoff, N. (2011). Urethral sphincter EMG-controlled dorsal penile/clitoral nerve stimulation to treat neurogenic detrusor overactivity. Journal of Neural Engineering, 8(3), 036001.
Bosch, J. R. (2006). Electrical neuromodulatory therapy in female voiding dysfunction. BJU International, 98(s1), 43–48.
Krasmik, D., Krebs, J., van Ophoven, A., & Pannek, J. (2014). Urodynamic results, clinical efficacy, and complication rates of sacral intradural deafferentation and sacral anterior root stimulation in patients with neurogenic lower urinary tract dysfunction resulting from complete spinal cord injury. Neurourology and Urodynamics, 33(8), 1202–1206.
Brindley, G. (1994). The first 500 patients with sacral anterior root stimulator implants: General description. Spinal Cord, 32(12), 795–805.
Gaunt, R. A., & Prochazka, A. (2006). Control of urinary bladder function with devices: Successes and failures. Progress in Brain Research, 152, 163–194.
Lozano, A. M., & Lipsman, N. (2013). Probing and regulating dysfunctional circuits using deep brain stimulation. Neuron, 77(3), 406–424.
Rosa, M., Giannicola, G., Marceglia, S., Fumagalli, M., Barbieri, S., & Priori, A. (2012). Neurophysiology of deep brain stimulation. International Review of Neurobiology, 107, 23–55.
Hescham, S., Lim, L. W., Jahanshahi, A., Steinbusch, H. W., Prickaerts, J., Blokland, A., et al. (2013). Deep brain stimulation of the forniceal area enhances memory functions in experimental dementia: The role of stimulation parameters. Brain Stimulation, 6(1), 72–77.
Blok, B. F., De Weerd, H., & Holstege, G. (1995). Ultrastructural evidence for a paucity of projections from the lumbosacral cord to the pontine micturition center or M-region in the cat: A new concept for the organization of the micturition reflex with the periaqueductal gray as central relay. Journal of Comparative Neurology, 359(2), 300–309.
Stone, E., Coote, J., & Lovick, T. (2015). Effect of electrical vs. chemical deep brain stimulation at midbrain sites on micturition in anaesthetized rats. Acta Physiologica, 214(1), 135–145.
Wang, J., Hou, C., Zheng, X., Zhang, W., Chen, A., & Xu, Z. (2009). Design and evaluation of a new bladder volume monitor. Archives of Physical Medicine and Rehabilitation, 90(11), 1944–1947.
Schlebusch, T., Nienke, S., Leonhardt, S., & Walter, M. (2014). Bladder volume estimation from electrical impedance tomography. Physiological Measurement, 35(9), 1813.
Seif, C., Herberger, B., Cherwon, E., Martinez Portillo, F., Molitor, M., Stieglitz, T., et al. (2004). Urinary bladder volumetry by means of a single retrosymphysically implantable ultrasound unit. Neurourology and Urodynamics, 23(7), 680–684.
Mendez, A., Sawan, M., Minagawa, T., & Wyndaele, J.-J. (2013). Estimation of bladder volume from afferent neural activity. IEEE Transactions on Neural Systems and Rehabilitation Engineering, 21(5), 704–715.
Beaumont, A., Marmarou, A., Czigner, A., Yamamoto, M., Demetriadou, K., Shirotani, T., et al. (1999). The impact-acceleration model of head injury: Injury severity predicts motor and cognitive performance after trauma. Neurological Research, 21(8), 742–754.
Beaumont, A., Marmarou, C., & Marmarou, A. (2000). The effects of human corticotrophin releasing factor on motor and cognitive deficits after impact acceleration injury. Neurological Research, 22(7), 665–673.
Hylin, M. J., Orsi, S. A., Zhao, J., Bockhorst, K., Perez, A., Moore, A. N., et al. (2013). Behavioral and histopathological alterations resulting from mild fluid percussion injury. Journal of Neurotrauma, 30(9), 702–715.
Ekmark-Lewén, S., Flygt, J., Kiwanuka, O., Meyerson, B. J., Lewén, A., Hillered, L., et al. (2013). Traumatic axonal injury in the mouse is accompanied by a dynamic inflammatory response, astroglial reactivity and complex behavioral changes. Journal of Neuroinflammation, 10(1), 44.
Jiang, H.-H., Kokiko-Cochran, O. N., Li, K., Balog, B., Lin, C.-Y., Damaser, M. S., et al. (2013). Bladder dysfunction changes from underactive to overactive after experimental traumatic brain injury. Experimental Neurology, 240, 57–63.
Perkes, I., Baguley, I. J., Nott, M. T., & Menon, D. K. (2010). A review of paroxysmal sympathetic hyperactivity after acquired brain injury. Annals of Neurology, 68(2), 126–135.
Rabinstein, A. A., & Benarroch, E. E. (2008). Treatment of paroxysmal sympathetic hyperactivity. Current Treatment Options in Neurology, 10(2), 151–157.
Walter, J. S., Fitzgerald, M. P., Wheeler, J. S., & Orris, B. (2005). Bladder-wall and pelvic-plexus stimulation with model microstimulators: Preliminary observations. Journal of Rehabilitation Research and Development, 42(2), 251.
Acknowledgements
This study was supported by grants from the Ministry of Science and Technology (MOST106-2221-E-038-010-MY3, MOST103-2221-E-038-007-MY3, and NSC 102-2320-B-002-040 -MY2) and by the R&D Foundation of Urological Medicine, Taiwan. The authors also thank Professors Te-Son Kuo and Shuenn-Tsong Young for their outstanding technical support.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jen, E., Lin, CW., Hsieh, TH. et al. Prototype Deep Brain Stimulation System with Closed-Loop Control Feedback for Modulating Bladder Functions in Traumatic Brain Injured Animals. J. Med. Biol. Eng. 38, 337–349 (2018). https://doi.org/10.1007/s40846-017-0326-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40846-017-0326-1