Abstract
A significant interaction between kidneys and lungs has been shown in physiological and pathological conditions. The two organs can both be targets of the same systemic disease (eg., some vasculitides). Moreover, loss of normal function of either of them can induce direct and indirect dysregulation of the other one. Subjects suffering from COPD may have systemic inflammation, hypoxemia, endothelial dysfunction, increased sympathetic activation and increased aortic stiffness. As well as the exposure to nicotine, all the foresaid factors can induce a microvascular damage, albuminuria, and a worsening of renal function. Renal failure in COPD can be unrecognized since elderly and frail patients may have normal serum creatinine concentration. Lungs and kidneys participate in maintaining the acid-base balance. Compensatory role of the lungs rapidly expresses through an increase or reduction of ventilation. Renal compensation usually requires a few days as it is achieved through changes in bicarbonate reabsorption. Chronic kidney disease and end-stage renal diseases increase the risk of pneumonia. Vaccination against Streptococcus pneumonia and seasonal influenza is recommended for these patients. Vaccines against the last very virulent H1N1 influenza A strain are also available and effective. Acute lung injury and acute kidney injury are frequent complications in critical illnesses, associated with high morbidity and mortality. The concomitant failure of kidneys and lungs implies a multidisciplinary approach, both in terms of diagnostic processes and therapeutic management.
Similar content being viewed by others
Conditions in which lungs and kidneys are both targets of disease
Lungs and kidneys are different organs with their own body localization, structure, and function, but it is a shared concept that they are not completely independent from each other and can suffer damages concurrently in the course of systemic diseases (Table 1) [1]. Vasculitides and autoimmune disorders are the best-known examples. Goodpasture’s syndrome (also known as anti-glomerular basement antibody disease) is an autoimmune disease characterized by the production of antibodies which affect both lungs and kidneys. Antineutrophil cytoplasmic antibody (ANCA)-associated vasculitides are a small group of necrotizing vasculitides including Granulomatosis withpolyangiitis (GPA), Microscopic polyangiitis (MPA), and Eosinophilic granulomatosis with polyangiitis (EGPA) [2].
GPA, also known as Wegener’s granulomatosis, is a potentially fatal vasculitis affecting small- and medium-size vessels, often causing a granulomatous inflammation of the upper and lower respiratory tracts and a pauci-immune glomerulonephritis.
EGPA (or Churg–Strauss syndrome) is another vasculitis affecting mainly small vessels with almost constant respiratory involvement (chronic rhinosinusitis and asthma) and possible renal dysfunction. All the aforementioned diseases are acknowledged causes of pulmonary-renal syndrome, involving pulmonary vascular beds with diffuse alveolar hemorrhage and kidney damage, in particular glomerulonephritis.
Pulmonary-renal syndrome can be also induced by microscopic polyangiitis and immune-complex vasculitides like systemic lupus erythematosus, cryoglobulinemic vasculitis, and Schönlein-Henoch Purpura.
Several alterations in lung function have been described in patients with diabetes mellitus. Consequently, the term “diabetic lung” has been coined considering the similarity to the dysfunction that develops in other organs, including the kidneys, during the course of this chronic illness (e.g., diabetic foot, diabetic nephropathy, diabetic vasculopathy).
Some studies have proved that patients with both type 1 and 2 diabetes mellitus show impaired alveolar-capillary diffusion capacity for carbon monoxide (DLCO), as well as reduced lung volumes and flows, if compared to healthy subjects. The pathogenic mechanisms of these alterations are not entirely clear, but there has been speculation about microvascular damage of pulmonary capillary due to diabetic microangiopathy [3,4,5].
The extent of the lowering in DLCO seems to be linked to the degree of severity of other vascular complications, such as retinopathy and renal microangiopathy [6, 7]. Furthermore, at histopathologic level these functional modifications are supposed to correspond to a thickening of basal lamina of the pulmonary capillaries. This may contribute, in association with alveolar epithelium thickening, to a reduction in gas exchange capacity of the lungs [8].
Renal involvement in chronic obstructive pulmonary disease
Renal involvement in chronic respiratory diseases is commonly observed in clinical practice. Several studies have reported that prevalence of renal failure is higher in patients with diseases affecting mainly the lungs, especially in chronic obstructive pulmonary disease (COPD) [9,10,11]. This evidence is remarkable having considered that COPD is the seventh most frequent chronic disease in the world and it is expected to reach the fourth place in 2020 [12, 13]. COPD is considered the result of inflammatory processes of the airways and destructive changes of lung parenchyma, which lead to a progressive and irreversible airflow limitation. Inhalation of toxic gases and particles, in first place tobacco smoke, are the main factors capable of triggering these processes, but there is evidence that other elements and the genetic status may also play a role [14]. COPD is a complex and heterogeneous disease, frequently associated with several comorbidities [15]. It is estimated that in patients with COPD, concurrent diseases are often responsible for a higher morbidity and mortality than the respiratory disease itself [16]. The frequent association of a lot of other diseases with COPD has been for a long time considered consequence of their high prevalence in elderly people. However, increasing evidence supports the idea that COPD per se has a role in the development of extrapulmonary problems, to the extent that some authors consider COPD a systemic inflammatory disease [17, 18].
There is evidence that some comorbidities of COPD are associated with increased frequency in specific phenotypes. For instance, osteoporosis and lung cancer appear to be preferentially associated with the emphysematous phenotype compared to bronchitis phenotype [19, 20]. Likewise, it has been suggested that a dysfunction of the kidney is linked in more cases with the emphysematous phenotype of COPD, and that this association is independent from known risk factors for renal failure like advanced age, diabetes mellitus, and hypertension [21].
Several components of tobacco smoke such as nicotine and heavy metals, are identified as risk factors for development of renal disease [22]. Among smokers, a higher incidence of microalbuminuria and progression to overt proteinuria has been shown [23]. The renal damage induced by cigarette smoking is due, at least in part, to increased blood pressure, mediated by nicotine activation of the sympathetic nervous system. Nicotine also considerably decreases the activity of superoxide dismutase and increases the activity of catalase in the kidney.
The course of nephropathies is accelerated by nicotine with an increased incidence of progression from microalbuminuria to proteinuria. Coronary heart disease, which is highly prevalent in patients with COPD, is associated with renal vascular disease [24].
Albuminuria reflects an increased permeability of glomerulus, usually due to microvascular damage. This may be due to direct podocyte injury, but other potential contributing factors have been identified in subjects with COPD: systemic inflammation, hypoxemia, endothelial dysfunction, increased sympathetic activation, and increased aortic stiffness (Fig. 1) [25,26,27,28,29].
These determinants explain why the coexistence of COPD and chronic renal failure is not a rare event. Chronic kidney disease (CKD) in older patients with COPD is likely to be underestimated [30]. It is noteworthy that many studies on COPD exclude patients with a serum creatinine greater than 2 mg/dL [31], or do not specify how the diagnosis of renal failure was made [32].
Many COPD patients are elderly and frail, and they may often have a hidden or unrecognized renal failure, where, nonetheless, the serum creatinine concentration is normal [33]. A certain degree of discrepancy exists in the estimation of glomerular filtrate provided by equations in elderly and fragile subjects, inducing misclassification and interfering with the proper management of CKD [34]. The prevalence of chronic renal failure increases with age and is frequently associated with chronic diseases such as congestive heart failure or diabetes mellitus. When present as a comorbidity, renal failure implies negative prognostic repercussions and affects therapeutic strategies [35].
Implications of renal dysfunction in patients with chronic pulmonary disease
The kidneys, as well as the lungs, participate to the maintenance of the acid-base balance and therefore blood pH (Fig. 2). Particularly, kidneys are the main organs involved when the acid–base balance is chronically impaired due to a respiratory cause [36].
In cases of “pump failure” with hypoventilation, e.g., due to emphysema or neuromuscular diseases, carbon dioxide (CO2) retention is frequently observed. A sudden worsening of alveolar ventilation can provoke an acute increase in blood CO2 levels, which rapidly reduces pH to values of acidosis (lower than 7.35).
If respiratory acidosis persists, kidneys respond by retaining bicarbonate ions (HCO3−).
This mostly occurs because the increase in CO2 at the level of renal tubular cells stimulates the secretion of H+ ions and the elimination of more acid urine, while HCO3− ions are reabsorbed.
In the case of renal impairment, acid–base balance is not efficiently restored, resulting in prolonged blood acidosis and suffering for the whole body.
It has been shown that in patients with COPD exacerbation and hypercapnia, the development of sufficient metabolic compensation and adequate renal function significantly decreases mortality [37]. Acidosis is an adverse prognostic indicator and is responsible for several deleterious effects on hemodynamics and metabolism [38, 39]. Acidosis causes myocardial depression, arrhythmias, a decrease in peripheral vascular resistances, and hypotension. In addition, hypercapnic acidosis is responsible for weakness of respiratory muscles, an increase of proinflammatory cytokines and apoptosis, and cachexia. Moreover, in hypercapnic COPD patients a reduction in renal blood flow, an activation of the renin-angiotensin system, and an increase in circulating values of antidiuretic hormone, atrial natriuretic peptide, and endothelin-1 have been reported [40]. It has been supposed that these hormonal abnormalities can play a role in the retention of salt and water and in the development of pulmonary hypertension, independently from the presence of myocardial dysfunction.
When renal failure occurs in COPD patients, the compensatory role of kidney in respiratory acidosis may be less effective, resulting in a reduced ammoniagenesis and titratable acidity production with consequent limited rise of serum bicarbonate and a more severe acidosis. Clinical reports have demonstrated that bicarbonate levels in these patients are inversely related to survival and that concomitant renal failure is predictive of death and risk of exacerbation [41,42,43].
Chronic acidosis, insulin resistance, hypercalcemia in addition to malnutrition and uremic toxins may contribute developing systemic skeletal muscle atrophy in uremic patients. The resulting muscle weakness and poor physical performance mirror a progressive general physical deconditioning. An impairment in lung function has also been found, due to reduced respiratory muscle strength and phrenic neuropathy. This condition could worsen the exercise tolerance in individuals suffering from pulmonary diseases. Maximal inspiratory pressure (MIP) and maximal expiratory pressure (MEP) are reduced in patients on hemodialysis or continuous ambulatory peritoneal dialysis, as well as in renal transplant recipients [44]. However, the lowest inspiratory muscle strength has been found in peritoneal dialysis subjects, suggesting that the presence of intra-abdominal dialysate might interfere with diaphragmatic contraction [45]. Muscles and cardiovascular limitations lead patients to reduce daily life activities and increase disability and mortality. Weakening of respiratory and lower-limb muscle seems to be progressive and partially reversible following exercise, but little is known whether training could lead to a better outcome [46, 47].
Exhaled breath gases in chronic kidney disease
The composition of exhaled breath in subjects with CKD changes according to the excretion of several volatile compounds that are retained due to decreased renal function. These gases can now be detected through various techniques (e.g., gas chromatography), although the collection of exhaled breath is difficult because the sample is easily contaminated by organic compounds produced in the mouth or by room air.
The most notable volatile substance detected in the breath of patients with CKD is ammonia, that is responsible for the typical uremic breath of these patients. The concentration of ammonia in healthy people is about 800 parts per billion by volume (ppbv) [48], with great variability, mostly derived from the abovementioned sampling problems. In people with undergoing hemodialysis, this concentration increases up to 2000 ppbv [49].
Several other metabolites are retained in CKD and excreted by the lung, such as the secondary and tertiary amines dimethylamine and trimethylamine [50], hydroxyacetone and 3-hydroxy-2 butanone. Other compounds such as 4-heptanal, 4-heptanone, and 2-heptanone, are detectable only in patients undergoing hemodialysis [51]. Finally, it is not clear whether isoprene in breath increases as a consequence of impaired renal function. While in a rat model of renal insufficiency it shows an early increase, in humans it only increases during hemodialysis: therefore, it is not clear whether the result in rats is a consequence of renal injury rather than an actual retention in the blood [52].
Implications of the respiratory impairment in patients with chronic renal failure
CO2 elimination through breathing is a powerful and rapid mechanism which regulates acid-base status of the blood and of the body as a whole. The lungs daily eliminate over 10,000 mEq of carbonic acid, compared to less than 100 mEq of fixed acid daily eliminated by the kidney. By regulating (increasing) the alveolar ventilation, it is possible to maintain a normal blood pH even when levels of HCO3− are relatively low as a consequence of renal dysfunction, as well as of other sources of HCO3− loss (e.g., enteric).
Generally, in a patient with low levels of bicarbonates, hyperventilation and hypocapnia are observed. This should be taken into account in the clinical evaluation of such a patient, since this status may raise the suspicion of a lung disease. Compensatory hyperventilation usually is associated with pO2 levels that move towards the upper limit of normal. Low levels of pO2 (hypoxemia) despite hyperventilation should lead to the hypothesis of a concomitant respiratory problem.
Patients with advanced cystic fibrosis, who often develop respiratory failure and hypercapnia, may have altered electrolyte transport and malnutrition. Such conditions may predispose to metabolic alkalosis and, therefore, may contribute to hypercapnia, especially during acute exacerbations [53].
Acid–base balance can be influenced by drugs frequently used in patients with chronic renal failure, such as diuretics. Loop and thiazide diuretics increase sodium delivery to the distal tubule, thus stimulating the aldosterone-sensitive sodium pump to intensify sodium reabsorption in exchange for potassium and hydrogen ions, which are consequently lost in the urine. This situation can cause metabolic alkalosis and in the same time electrolyte alterations, such as hypokalemia and hyponatremia [54].
Respiratory infections in hemodialysis
Chronic kidney disease and end-stage renal disease (ESRD) increase the risk of bacterial infections, particularly urinary tract infections, pneumonia, and sepsis [55, 56]. This risk is partially due to dialysis access devices, but patients requiring renal replacement therapy are also susceptible to non-access-related infections. Many of these patients also have diabetes, take immunosuppressant agents and chronically retain uremic toxins. It follows that particular attention should be paid to the diagnosis and treatment of these infections. Choosing appropriate antibiotics class and dosage is crucial and nephrotoxic drugs should be avoided, if possible, in patients with residual renal function.
Pneumonia are the second more common cause of severe infections among subjects undergoing hemodialysis [57]. They are most frequently community-acquired pneumonia, mainly caused by Streptococcus pneumoniae and seasonal influenza. Treatment of pneumonia in hemodialysis patients does not differ from the one for the general population, but the death rates are 14–16 times higher [58]. A polysaccharide vaccine against Streptococcus pneumonia is available with a satisfactory early serological response in these particular subjects. However, studies with over 6 months of observation showed a more rapid decline in antibody titer compared to the general population [59]. Vaccination of all patients with ESRD and re-vaccination after 5 years is usually recommended.
Influenza affects 10–20% of the general population, reaching 50% in case of a pandemic outbreak. Even though hemodialysis patients may have a reduced immune response to the vaccine against influenza, it is believed to provide sufficient protection and should be annually performed. A second dose of seasonal influenza vaccine showed no benefit to hemodialysis patients [60].
ESRD patients also are at high risk for infection by the last very virulent H1N1 influenza A strain. Suspected cases should start treatment within 48 h, even before the definitive identification of H1N1 influenza A strain. The neuroaminidase inhibitor oseltamivir at a dose of 30 mg after every hemodialysis session is the treatment of choice. However, its use should be limited to subjects with high diagnostic suspicion, to avoid the development of resistance, which occurred with former antiviral agents like amantadine. Vaccines against H1N1 influenza A strain with or without the immune adjuvant MF59 are available and effective.
Tuberculosis (TB) is another respiratory infection which assumes peculiar features in ESRD patients. The latter have an increased risk of active TB, which may also occur as a fever of unknown origin or with extrapulmonary localization. As a consequence, the Centers for Disease Control (CDC) recommend that all hemodialysis patients should be tested with tuberculin skin test (TST). A quite high percentage of anergy (30–40%) due to a defective cellular immunity has been described in this population, with resulting reduction of hypersensitivity skin reactions and TST sensitivity [61]. Therefore, in hemodialysis patients, TST is considered positive if the skin induration is larger than 5 mm in diameter. In the case of TST positivity, preventive treatment with isoniazid alone or in combination with rifampicin is recommended. In many countries, this policy is limited to renal transplant recipient candidates because of the increased risk of activation after transplantation. Other methods for diagnosing latent TB like INF-γ release assay (IGRA) or even serologic tests have been proposed [62].
The occurrence of lung diseases after kidney transplantation
Pulmonary complications are among the major causes of morbidity and mortality after renal transplantation. Their occurrence heavily affects the prognosis of kidney transplant patients and is associated with a 20% incidence of graft failure [63].
Studies show a variable incidence of lung diseases after kidney transplantation, ranging from 3.1 to 37%, with mortality rates of 22.5–32% [64,65,66].
The most common complication is pneumonia, followed by cardiogenic pulmonary edema and acute lung injury (ALI) or acute respiratory distress syndrome (ARDS) resulting from extrapulmonary bacterial sepsis. Noninfectious complications after renal transplantation include atelectasis, pulmonary thromboembolism, and post-transplant malignancy [67].
An early and accurate diagnosis of pneumonia is crucial both because of its high morbidity and mortality and also because of the frequent complications associated with the drugs needed to treat the infection.
Most infections during the first month after kidney transplantation are caused by hospital bacteria. Between the second and sixth month after transplantation, when immunosuppression reaches its maximum levels, the patient is highly susceptible to opportunistic pulmonary infections [68].
Pathogens that most frequently cause pneumonia during this time period include bacteria, fungi (especially Pneumocystis jirovecii), and viruses (especially Cytomegalovirus). The risk for opportunistic infections is particularly high in patients treated for chronic rejection or recurrent episodes of acute rejection [69]. The level of immunosuppression is usually reduced beyond 6 months, when the infections are mainly due to common community-acquired pathogens.
It should be noticed that several immunosuppressive drugs have been clearly shown to be toxic for lungs. Azathioprine and mammalian target of rapamycin inhibitors (mTOR, e.g., Sirolimus and Everolimus) are those at greater risk for pulmonary complications. A few reports suggest that Tacrolimus and Mycophenolate mofetil may also lead to lung injury [70,71,72].
A relationship between interstitial lung disease and specific drug concentration has been found [73]. Formulas to calculate more precisely immunosuppressants drugs dosage have been suggested in order to lower the probability of lung toxicity in clinical practice [74].
Effects of acute lung injury and mechanical ventilation on renal function
ALI and acute kidney injury (AKI) are frequent complications in critical illnesses, associated with high morbidity and mortality [75]. ALI is defined by several clinical criteria, including acute onset of bilateral pulmonary infiltrates with hypoxemia and PaO2/FIO2 ratio of less than 300 mm Hg, without evidence of hydrostatic pulmonary edema [76]. The same clinical features but PaO2/FIO2 ratio lower than 200 mmHg, define the acute respiratory distress syndrome (ARDS). The AKI, also known as acute renal failure (ARF), is an abrupt loss of kidney function, with retention of nitrogenous waste products such as urea, and alteration of fluid and electrolyte homeostasis [77].
Both forms of end-organ injury commonly occur in similar settings of systemic inflammatory response syndrome, shock, and evolving multiple organ dysfunction. The complex interplay between injured organs in patients with multiple organ dysfunction syndrome has been called “the slippery slope of critical illness” [78].
Respiratory complications are common in patients with AKI and include pulmonary edema, respiratory failure needing mechanical ventilation, prolonged duration of mechanical ventilation and difficult weaning from it. Data from patients and animal models support the notion that cardiogenic pulmonary edema (from volume overload) and non-cardiogenic pulmonary edema (from endothelial injury due to inflammation and apoptosis) can occur in AKI.
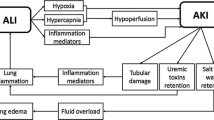
Recent data show that kidneys play an important role in the production and elimination of inflammation mediators of ALI. On the other hand, exposure to the inflammatory setting of ALI and mechanical ventilation-induced injury may precipitate the onset of AKI. The term ventilator-induced kidney injury (VIKI) has been suggested to describe this phenomenon.
It is believed that hemodynamic and neurohormonal factors are able to reduce renal perfusion and function during positive-pressure mechanical ventilation (PPV) [79]. Hemodynamic effects of PPV arise from the increased intrathoracic pressure, which in turn lowers the venous return to the heart (preload) and may result in decreased cardiac output. This may lead to hypotension and fluid-responsive shock, which is common in the initial postintubation period when PPV is initiated. Growth of intrathoracic pressure has been shown to be correlated with a diminution in renal plasma flow, glomerular filtration rate (GFR) and urine output during PPV.
Neurohormonal effects of PPV include the production of vasoactive substances, rennin-angiotensin axis activation, increased nonosmotic vasopressin (ADH) secretion, suppression of atrial natriuretic peptide (ANP) release, downstream stimulation of aldosterone production. Each of these neurohormonal pathways may result in a reduction of renal blood flow and GFR, fluid retention (salt and water), and oliguria.
Permissive hypercapnia is a commonly accepted mechanical ventilation practice, in which tidal volumes and alveolar ventilation are reduced in order to diminish ventilator-induced lung injury (VALI) while treating ALI. Through a variety of mechanisms, permissive hypercapnia may favorably influence the course of ALI, associated VALI, and harmful organ cross-talk between damaged lungs and other organs, leading to a protective effect against the development of VIKI.
Change history
16 September 2019
Given names of all the authors have been interchanged with family names.
16 September 2019
Given names of all the authors have been interchanged with family names.
References
Visconti L, Santoro D, Cernaro V et al (2016) Kidney–lung connections in acute and chronic diseases: current perspectives. J Nephrol 29:341
Binda V, Moroni G, Messa P (2018) ANCA-associated vasculitis with renal involvement. J Nephrol 31:197
Strojek K, Ziora D, Sroczynski J, Oklek K (1992) Pulmonary complications of type 1 (insulin-dependent) diabetic patients. Diabetologia 35:1173–1176
Innocenti F, Fabbri A, Anichini R et al (1994) Indications of reduced pulmonary function in type 1 (insulindependent) diabetes mellitus. Diabetes Res Clin Pract 25:161–168
Mori H, Okubo M, Okamura M et al (1992) Abnormalities of pulmonary function in patients with non-insulindependent diabetes mellitus. Intern Med 31:189–193
Jubic S, Metelko Z, Car N et al (1998) Reduction of diffusion capacity for carbon monoxide in diabetic patients. Chest 114:1033–1035
Arvisi M, Bartolini L, del Borrello P et al (2001) Pulmonary function in non-insulin—dependent diabetes mellitus. Respiration 68:268–272
Sandler M (1990) Is the lung a ‘target organ’ in diabetes mellitus? Arch Intern Med 150:1385–1388
Gjerde B, Bakke PS, Ueland T, Hardie JA, Eagan TM (2012) The prevalence of undiagnosed renal failure in a cohort of COPD patients in western Norway. Respir Med 106:361–366
van Gestel YR, Chonchol M, Hoeks SE et al (2009) Association between chronic obstructive pulmonary disease and chronic kidney disease in vascular surgery patients. Nephrol Dial Transplant 24:2763–2767
Incalzi RA, Corsonello A, Pedone C, Battaglia S, Paglino G, Bellia V (2010) Extrapulmonary consequences of COPD in the elderly study investigators. Chronic renal failure: a neglected comorbidity of COPD. Chest 137:831–837
Rabe KF, Hurd S, Anzueto A et al (2007) Global initiative for chronic obstructive lung disease. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: gold executive summary. Am J Respir Crit Care Med 176:532–555
Mannino DM, Braman S (2007) The epidemiology and economics of chronic obstructive pulmonary disease. Proc Am Thorac Soc 4:502e6
Sorheim IC, DeMeo DL, Washko G, Litonjua A, Sparrow D, Bowler R et al (2010) Polymorphisms in the superoxide dismutase-3 gene are associated with emphysema in COPD. COPD 7:262e8
Fabbri LM, Luppi F, Beghé B, Rabe KF (2008) Complex chronic comorbidities of COPD. Eur Respir J 31(1):204–212
Huiart L, Ernst P, Suissa S (2005) Cardiovascular morbidity and mortality in COPD. Chest 128:2640–2646
Fabbri LM, Rabe KF (2007) From COPD to chronic systemic inflammatory syndrome? Lancet 1(9589):797–799 370(
Barnes PJ (2013) COPD: Inflammatory mechanisms and systemic consequences. Eur Respir Monograph 59:(13–27)
Bon JM, Zhang Y, Duncan SR et al (2010) Plasma infl ammatory mediators associated with bone metabolism in COPD. COPD 7:186–191
McAllister DA, Maclay JD, Mills NL et al (2007) Arterial stiffness is independently associated with emphysema severity in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 176(12):1208–1214
Elmahallawy II, Qora MA (2013) Prevalence of chronic renal failure in COPD patients. Egypt J Chest Dis Tuberc 62:221–227
Cooper RG (2006) Effect of tobacco smoking on renal function. Indian J Med Res 124:261–268
Hansen HP, Rossing K, Jacobsen P, Jensen BR, Parving HH (1996) The acute effect of smoking on systemic haemodynamics, kidney and endothelial functions in insulin-dependent diabetic patients with microalbuminuria. Scand J Clin Lab Invest 56:393–399
Soriano JB, Visick GT, Muellerova H, Payvandi N, Hansell AL (2005) Patterns of comorbidities in newly diagnosed COPD and asthma in primary care. Chest 128:2099–2107
Gan WQ, Man SF, Senthilselvan A, Sin DD (2004) Association between chronic obstructive pulmonary disease and systemic inflammation: a systematic review and a meta-analysis. Thorax 59:574–580
Eickhoff P, Valipour A, Kiss D, Schreder M, Cekici L, Geyer K, Kohansal R, Burghuber OC (2008) Determinants of systemic vascular function in patients with stable chronic obstructive pulmonary disease. Am J Respir Crit Care Med 178:1211–1218
Andreas S, Anker SD, Scanlon PD, Somers VK (2005) Neurohumoral activation as a link to systemic manifestations of chronic lung disease. Chest 128:3618–3624
Hansen JM, Olsen NV, Feldt-Rasmussen B, Kanstrup IL, Dechaux M, Dubray C, Richalet JP (1994) Albuminuria and overall capillary permeability of albumin in acute altitude hypoxia. J Appl Physiol 76:1922–1927
John M, Hussain S, Prayle A, Simms R, Cockcroft JR, Bolton CE (2013) Target renal damage: the microvascular associations of increased aortic stiffness in patients with COPD. Respir Res 14:31
Corsonello A, Aucella F, Pedone C, Antonelli-Incalzi R (2017) Chronic kidney disease: A likely underestimated component of multimorbidity in older patients with chronic obstructive pulmonary disease. Geriatr Gerontol Int 17:1770–1788
Bellia V, Pistelli R, Catalano F et al (2000) Quality control of spirometry in the elderly. The SA.R.A. study. SAlute Respiration nell’Anziano = respiratory health in the elderly. Am J Respir Crit Care Med 161:1094–1100
Almagro P, Calbo E, Ochoa de Echagüen A et al (2002) Mortality after hospitalization for COPD. Chest 121(5):1441–1448
Middleton RJ, Foley RN, Hegarty J et al (2006) The unrecognized prevalence of chronic kidney disease in diabetes. Nephrol Dial Transplant 21:88–92
Corsonello A, Pedone C, Bandinelli S, Ferrucci L, Antonelli Incalzi R (2017) Agreement between chronic kidney disease epidemiological collaboration and Berlin initiative study equations for estimating glomerular filtration rate in older people: the Invecchiare in Chianti (aging in Chianti region) study. Geriatr Gerontol Int 17(10):1559–1567
McAlister FA, Ezekowitz J, Tonelli M, Armstrong PW (2004) Renal insufficiency and heart failure: prognostic and therapeutic implications from a prospective cohort study. Circulation 109 (8):1004–1009
Bruno CM, Valenti MJ (2012) Acid–base disorders in patients with chronic obstructive pulmonary disease: a pathophysiological review. Biomed Biotechnol 2012:915150. Epub 2012 Feb 1
Ucgun I, Oztuna F, Dagli CE, Yildirim H, Bal C (2008) Relationship of metabolic alkalosis, azotemia and morbidity in patients with chronic obstructive pulmonary disease and hypercapnia. Respiration 76(3):270–274.(Epub 2008 May 8)
Handy JM, Soni N (2008) Physiological effects of hyperchloraemia and acidosis. Br J Anaesth 101(2):141–150
Kraut JA, Madias NE (2010) Metabolic acidosis: pathophysiology, diagnosis and management. Nat Rev Nephrol 6(5):274–285
Anand IS, Chandrashekhar Y, Ferrari R et al (1992) Pathogenesis of congestive state in chronic obstructive pulmonary disease: studies of body water and sodium, renal function, hemodynamics, and plasma hormones during edema and after recovery. Circulation 86(1):12–21
Ucgun I, Oztuna F, Dagli CE, Yildirim H, Bal C (2008) Relationship of metabolic alkalosis, azotemia and morbidity in patients with chronic obstructive pulmonary disease and hypercapnia. Respiration 76(3):270–274
Khilnani GC, Banga A, Sharma SK (2004) Predictors of mortality of patients with acute respiratory failure secondary to chronic obstructive pulmonary disease admitted to an intensive care unit: a one year study. BMC Pulm Med 4:12
Banga A, Khilnani GC (2006) A comparative study of characteristics and outcome of patients with acute respiratory failure and acute on chronic respiratory failure requiring mechanical ventilation. Indian J Crit Care Med 10(2):80–87
Karacan O, Tutal E, Colak T et al (2006) Pulmonary function in renal transplant recipients and endstage renal disease patients undergoing maintenance dialysis. Transpl Proc 38:396–400
Gómez-Fernández P, Sánchez Agudo L, Calatrava JM et al (1984) Respiratory muscle weakness in uremic patients under continuous ambulatory peritoneal dialysis. Nephron 36:219–223
Manfredini F, Lamberti N, Malagoni AM et al (2015) The role of deconditioning in the end-stage renal disease myopathy: physical exercise improves altered resting muscle oxygen consumption. Am J Nephrol 41:329–336
Pomidori L, Lamberti N, Malagoni AM et al (2016) Respiratory muscle impairment in dialysis patients: can minimal dose of exercise limit the damage? A Preliminary study in a sample of patients enrolled in the EXCITE trial. J Nephrol 29:863–869
Turner C, Spanel P, Smith D (2006) A longitudinal study of ammonia, acetone and propanol in the exhaled breath of 30 subjects using selected ion flow tube mass spectrometry, SIFT-MS. Physiol Meas 27(4):321–337
Narasimhan LR, Goodman W, Patel CK (2001) Correlation of breath ammonia with blood urea nitrogen and creatinine during hemodialysis. Proc Natl Acad Sci USA 98(8): 4617–4621
Simenhoff ML, Burke JF, Saukkonen JJ et al (1977) Biochemical profile of uremic breath. N Engl J Med 297(3):132–135
Davies SJ, Španěl P, Smith D (2014) Breath analysis of ammonia, volatile organic compounds and deuterated water vapor in chronic kidney disease and during dialysis. Bioanalysis 6(6):843–857
Jankowski J, Westhof T, Vaziri ND et al (2014) Gases as uremic toxins: is there something in the air? Semin Nephrol 34(2):135–150
Holland AE, Wilson JW, Kotsimbos TC, Naughton MT. (2003). Metabolic alkalosis contributes to acute hypercapnic respiratory failure in adult cystic fibrosis. Chest 124(2):490–493
Sbardella E, Isidori AM, Arnaldi G et al (2018 Jan) Approach to hyponatremia according to the clinical setting: consensus statement from the Italian Society of Endocrinology (SIE), Italian Society of Nephrology (SIN), and Italian Association of Medical Oncology (AIOM). J Endocrinol Invest 41(1):3–19
Naqvi SB, Collins AJ (2006) Infectious complications in chronic kidney disease. Adv Chronic Kidney Dis 13(3):199
Dalrymple LS, Katz R, Kestenbaum B, de Boer IH, Fried L, Sarnak MJ, Shlipak MG (2012) The risk of infection-related hospitalization with decreased kidney function. Am J Kidney Dis 59(3):356
Eleftheriadis T, Liakopoulos V, Leivaditis K et al. (2011) Infections in hemodialysis: a concise review—part 1: bacteremia and respiratory infections. Hippokratia 15(1): 12–17
Sarnak MJ, Jaber BL (2001) Pulmonary infectious mortality among patients with end-stage renal disease. Chest 120:1883–1887
Robinson J (2004) Efficacy of pneumococcal immunization in patients with renal disease—what is the data? Am J Nephrol 24:402–409
Tanzi E, Amendola A, Pariani E, Zappa A, Colzani D, Logias F et al (2007) Lack of effect of a booster dose of influenza vaccine in hemodialysis patients. J Med Virol 79:1176–1179
Poduval RD, Hammes MD (2003) Tuberculosis screening in dialysis patients—is the tuberculin test effective? Clin Nephrol 59:436–440
Winthrop KL, Nyendak M, Calvet H, Oh P, Lo M, Swarbrick G et al (2008) Interferon-gamma release assays for diagnosing mycobacterium tuberculosis infection in renal dialysis patients. Clin J Am Soc Nephrol 3:1357–1363
Pencheva VP, Petrova DS, Genov DK et al (2015) Risk factors for lung diseases after renal transplantation. J Res Med Sci 20(12):1127–1132
Canet E, Osman D, Lambert J et al (2011) Acute respiratory failure in kidney transplant recipients: a multicenter study. Crit Care 15(2):R91
Pencheva V, Petrova D, Genov D et al (2014) Pulmonary complications as a cause of death after renal transplantation. Open J Intern Med 4:41–46
Zeyneloglu P (2015) Respiratory complications after solid-organ transplantation. Exp Clin Transpl 13(2):115–125
Kupeli E, Ulubay G, Colak T et al (2011) Pulmonary complications in renal recipients after transplantation. Transpl Proc 43(2):551–553
Splendiani G, Cipriani S, Tisone G et al (2005) Infectious complications in renal transplant recipients. Transpl Proc 37(6):2497–2499
Fishman JA (2007) Infection in solid-organ transplant recipients. N Engl J Med 357:2601–2614
Sasaki T, Nakamura W, Inokuma S et al (2016) Characteristic features of tacrolimus-induced lung disease in rheumatoid arthritis patients. Clin Rheumatol 35(2):541–545
Boddana P, Webb LH, Unsworth J et al (2011) Hypogammaglobulinemia and bronchiectasis in mycophenolate mofetil-treated renal transplant recipients: an emerging clinical phenomenon? Clin Transpl 25(3):417–419
Gorgan M, Bockorny B, Lawlor M et al (2013) Pulmonary hemorrhage with capillaritis secondary to mycophenolate mofetil in a heart-transplant patient. Arch Pathol Lab Med 137(11):1684–1687
Tomei P, Masola V, Granata S et al (2016) Everolimus-induced epithelial to mesenchymal transition (EMT) in bronchial/pulmonary cells: when the dosage does matter in transplantation. J Nephrol 29:881
Solazzo A, Botta C, Nava F et al. (2016) Interstitial lung disease after kidney transplantation and the role of Everolimus. Transpl Proc 48(2):349–351
Faubel S, Edelstein CL (2016 Jan) Mechanisms and mediators of lung injury after acute kidney injury. Nat Rev Nephrol 12(1):48–60
Dushianthan A, Grocott MP, Postle AD, Cusack R (2011) Acute respiratory distress syndrome and acute lung injury. Postgrad Med J 87(1031):612–622
Srisawat N, Kellum JA (2011) Acute kidney injury: definition, epidemiology, and outcome. Curr Opin Crit Care 17(6):548–555
Koyner JL, Murray PT (2010) Mechanical ventilation and the kidney. Blood Purif 29:52–68
Pannu N et al (2004) Effect of mechanical ventilation on the kidney. Best Pract Res Clin Anaesthesiol 18:189–203
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors disclose all relationships or interests that could have direct or potential influence or impart bias on the work.
Research involving human participants and/or animals
The research does not involve human participants and/or animals.
Informed consent
No informed consent was required.
Additional information
The original article has been revised: Due to authors family name and sur name interchange.
Rights and permissions
About this article
Cite this article
Sorino, C., Scichilone, N., Pedone, C. et al. When kidneys and lungs suffer together. J Nephrol 32, 699–707 (2019). https://doi.org/10.1007/s40620-018-00563-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-018-00563-1